Ceramic Restorations Flourishing With State-of-the-Art Materials, Methods
Nathaniel C. Lawson, DMD, PhD; Hernán Lázaro Villa, MDC; and Augusto Robles, DMD, MS
Arecent survey of general dentists in the United States reported that the most common material choice for a single-unit anterior fixed restoration is lithium disilicate, followed by layered zirconia and leucite-reinforced glass-ceramic.1 While this information reflects a basic trend in material prescription, the combinations of materials and methods of fabrication within these categories can be altered in the dental laboratory. This article discusses the most current materials available for ceramic restorations, with the intention of providing clinicians insight into the methods of crown fabrication prevalent in dental laboratories.
New Types of Glass-Ceramics
Lithium disilicate is a crystalline structure that can be used to reinforce a glass-ceramic material. Only one commercial product has this formulation (IPS e.max®, Ivoclar Vivadent, ivoclarvivadent.com), and it may be fabricated by milling a hardened block of uncrystallized material into a desired shape (IPS e.max CAD), or the crown shape can be printed in wax, invested, burnt out, and pressed into with the molten material (IPS e.max Press). The differences in mechanical properties between the two forms of fabrication seem to be negligible.2 Some dentists prefer pressed restorations due to perceived advantages in marginal detail; however, several studies have reported no difference in marginal fit between fabrication methods.3,4
Newer classes of glass-ceramic material with lithium-containing crystalline reinforcement have been introduced. Materials containing lithium-metasilicate and lithium-orthophosphate crystals include Suprinity® (VITA, vita-zahnfabrik.com), Celtra® Duo, and Celtra® Press (Dentsply Sirona, dentsplysirona.com). This class of material has also been called zirconia-reinforced lithium silicate, as it has 10% dissolved zirconia in its glass phase, though the zirconia does not truly act as a reinforcing phase.5 The lithium-metasilicate (and lithium-orthophosphate) crystals in these materials are smaller than lithium-disilicate crystals, making the materials slightly more translucent.6 Other lithium crystal-containing materials include Obsidian® (Glidewell Laboratories, glidewelldental.com), which is described as a lithium-silicate block, and n!ce® (Straumann, straumann.com), which is considered a fully crystallized lithium disilicate/lithium aluminosilicate.
Different Types of Zirconia
A common belief among many dentists is that all zirconia is the same. This is somewhat true in that zirconia crowns are milled from green-state pucks with the consistency of sidewalk chalk, and many pucks are composed of commonly manufactured powders. However, zirconia pucks may differ in the way that the powders are pressed into the puck (uniaxial versus isostatic) and in the additives that are mixed with the powders to achieve color and translucency.
Aside from relatively minor differences among brands of zirconia, there are three generations of zirconia with significant variations.7 The first generation of zirconia was used as a framework material that needed to be veneered with feldspathic zirconia. The second generation was modified by reducing the amount of alumina stabilizer from 0.25% to 0.05 wt%, which increased translucency to enable the material's use for monolithic posterior restorations (eg, BruxZir®, Glidewell Laboratories; Lava™ Plus, 3M ESPE, 3m.com). Lastly, the third generation has an increased concentration of yttria (5 mol%), which stabilizes the cubic phase of zirconia (eg, Katana™ Zirconia UTML, Kuraray, kuraraydental.com). Inclusion of the cubic phase makes this generation of zirconia more translucent though weaker. The third generation of zirconia has sufficient translucency to allow monolithic anterior restorations.
Adding Color to Restorations
The final appearance of a ceramic restoration can be attained through either selecting the internal shade of the ceramic, painting an external stain on the ceramic, or applying a layer of veneering porcelain.
Internal shade of ceramic-The internal shade and translucency of a glass-ceramic material, such as lithium disilicate, is based on the block or ingot from which the restoration is fabricated. The blocks and ingots come in a variety of VITA classic shades and as multilayer blocks and ingots that transition in chroma and value from cervical to incisal. Options are also available for translucency. For example, IPS e.max is available in high opacity (HO), medium opacity (MO), low translucency (LT), medium translucency (MT), and high translucency (HT). The HO and MO materials are useful for frameworks, the LT and MT for monolithic crowns, and the HT for inlays and onlays.
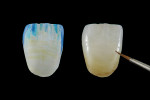
For zirconia, the internal shade and translucency is based on the puck from which the restoration is milled and any dipping stains used with the material. Zirconia pucks are available in unshaded, shaded, and multilayered versions. Unshaded zirconia may be modified by applying dipping stains to the zirconia while it is in the green (pre-sintered) state and allowing these stains to "soak" into the zirconia. The color will then appear in the zirconia when it is sintered in the furnace. The entire crown may be dipped in the stain, or the dipping stain may be selectively applied to the crown (eg, yellow/orange at cervical, blue/violet near incisal) (Figure 1, left).
Use of unshaded zirconia pucks allows the laboratory to achieve different shade restorations, lessening the need to stock multiple shaded pucks. Multilayered pucks vary in chroma and value from the top to the bottom of the puck. These pucks reduce the amount of external staining needed to be done by the lab to achieve a natural crown appearance. Additionally, some pucks vary in translucency.
External stain-As glass-ceramic materials have become stronger and zirconia materials have improved in translucency, esthetic monolithic ceramic restorations are now possible. To achieve the final color and characterization on a monolithic restoration, external stains are painted on its surface (Figure 1, right). The external stains are applied along with the glaze layer or below a layer of glaze. These surface stains can be used to impart characterization in the crown to match features such as staining, white spots, or cracks and mimic translucency through the addition of violet, blue, and grey hues. One concern is that in patients with high exposure to gastric or dietary acids, stains that are only applied to the surface may erode over time.
Layer of veneering porcelain-Perhaps the most esthetic option available for a ceramic crown is a ceramic coping layered with feldspathic porcelain. Both zirconia and lithium-disilicate materials can be used as a core over which porcelain is layered. Layering porcelain allows color and translucency characterization within a depth of the crown that can only be mimicked with surface painting alone. In other words, feldspathic porcelain can be placed in layers so that certain stains and tints may be placed on top of other stains.
Several methods can be used to apply the veneering porcelain onto the ceramic coping. A traditional method of applying porcelain is to have a dental ceramist hand-layer powder slurries of porcelain onto the surface of the crown (Figure 2). The ceramist may apply several different shades and translucencies of porcelain powders onto the coping at a time and then bake them onto the coping. Hand-layering porcelain requires artistic skill and can take time.
Less technique-sensitive methods of applying porcelain to a ceramic coping involve pressing a layer of porcelain or bonding a milled layer of porcelain onto the coping. In both of these techniques, a single shade and translucency of porcelain is applied onto the ceramic. This layer of porcelain imparts an enamel-like translucency to the restoration but does not provide the detailed characterization that can be achieved with hand-layered porcelain.
Porcelain may be applied to all surfaces of a layered crown or just the facial surface or facial incisal area. Application of veneering porcelain to the lingual surface of anterior maxillary crowns is not recommended as veneering porcelain causes considerably more wear to opposing tooth structure than lithium disilicate or zirconia.8 Layering porcelain only to the incisal facial aspect of the crown is referred to as cut-back layering or micro-layering. It requires less tooth reduction at the cervical section of the crown. Additionally, if the cut-back does not reach the lingual surface of the coping, the coping material can protect the weaker veneering porcelain in excursive movements.
Indirect dental restorations continue to evolve and improve-for the betterment of dentistry and, most importantly, dental patients. Aided by state-of-the-art materials and innovative crown fabrication methods, ceramic restorations provide robust, cosmetic solutions.
About the Authors
Nathaniel C. Lawson, DMD, PhD
Assistant Professor and Division Director of Biomaterials, Department of Clinical and Community Sciences, University of Alabama at Birmingham School of Dentistry, Birmingham, Alabama
Hernán Lázaro Villa, MDC
Director, Master Dental Ceramist Program, Department of Clinical and Community Sciences, University of Alabama at Birmingham School of Dentistry, Birmingham, Alabama
Augusto Robles, DMD, MS
Associate Professor, Division of General Dentistry, Department of Restorative Sciences, University of Alabama at Birmingham School of Dentistry, Birmingham, Alabama
References
1. Makhija SK, Lawson NC, Gilbert GH, et al. Dentist material selection for single-unit crowns: findings from the National Dental Practice-Based Research Network. J Dent. 2016;55:40-47.
2. Fabian Fonzar R, Carrabba M, Sedda M, et al. Flexural resistance of heat-pressed and CAD-CAM lithium disilicate with different translucencies. Dent Mater. 2017;33(1):63-70.
3. Al Hamad KQ, Al Rashdan BA, Al Omari WM, Baba NZ. Comparison of the fit of lithium disilicate crowns made from conventional, digital, or conventional/digital techniques. J Prosthodont. 2018. doi: 10.1111/jopr.12961. [Epub ahead of print]
4. Dolev E, Bitterman Y, Meirowitz A. Comparison of marginal fit between CAD-CAM and hot-press lithium disilicate crowns. J Prosthet Dent. 2018. doi: 10.1016/j.prosdent.2018.03.035. [Epub ahead of print]
5. Belli R, Wendler M, de Ligny D, et al. Chairside CAD/CAM materials. Part 1: measurement of elastic constants and microstructural characterization. Dent Mater. 2017;33(1):84-98.
6. Awad D, Stawarczyk B, Liebermann A, Ilie N. Translucency of esthetic dental restorative CAD/CAM materials and composite resins with respect to thickness and surface roughness. J Prosthet Dent. 2015;113(6):534-540.
7. Zhang Y, Lawn BR. Novel zirconia materials in dentistry. J Dent Res. 2018;97(2):140-147.
8. Lawson NC, Janyavula S, Syklawer S, et al. Wear of enamel opposing zirconia and lithium disilicate after adjustment, polishing and glazing. J Dent. 2014;42(12):1586-1591.