Minimally Invasive Single-Implant Treatment in the Esthetic Zone
David E. Azar, DDS, FICOI
Abstract:
Clinicians face significant challenges when placing single-tooth, implant-supported restorations in the esthetic zone. Understanding myriad factors, such as smile design, patient expectations, and hard- and soft-tissue responses, plays a vital role in achieving a predicable outcome. This article presents a case report demonstrating a minimally invasive approach, which combined immediate implant placement, hard- and soft-tissue augmentation, and immediate provisionalization in 1 visit.
Single-tooth, implant-supported replacements in the esthetic zone present a significant challenge in modern restorative dentistry. A broad understanding of multiple factors is required if success is to be achieved. In addition to esthetic factors such as smile design, tooth morphology, restorative materials, and patient expectations, the clinician must have an awareness of ideal implant positioning, prosthetic/implant interfaces, hard- and soft-tissue behavior, and the interrelationship of all of these.
Being successful in implant dentistry requires starting from the restoration desired and working backward. This is referred to as the restorative-driven approach and is best when used in combination with a biologic technique.
At least 2 publications have organized the criteria for success into easily understood paradigms to assist clinicians in assessing the risks in such cases. In 2001 Kois1 enumerated the 5 diagnostic keys that would assist a clinician in evaluating an esthetic single-tooth case to determine the predictability of the result. In 2009, the International Team for Implantology2 developed the straightfoward, advanced, and complex (SAC) classification in implant dentistry. This paradigm was designed to help evaluate the associated risks in specific esthetic case types and make recommendations on the skill sets required by a clinician wishing to undertake such a case.
Based on SAC classification, 4 criteria must be evaluated to divide cases into 1 of 3 groups: straightforward, advanced, or complex. The criteria are: smile line, tooth shape/midfacial contour, contact to crest, and gingival biotype (Table 1).
Kois’ criteria include these but added osseous crest position, which he categorized as high, normal, or low. These designations refer to the height of the facial bone crest to the existing free gingival margin, with high being closest and low as furthest. This plays a critical role in assessing predictability of the resultant free gingival margin, as the facial crest height and the soft-tissue margin are highly dependent and limited by the biologic width. The lower the osseous crest position, the less likely it will be to achieve a favorable result without some staged augmentation.
Case Report
In September 2013, a 25-year-old woman was referred to the author by a member of his implant study club for replacement of the maxillary left central incisor with an implant-supported restoration. Consultation with the patient revealed she was in good medical health. The patient’s chief complaints were that the tooth had recently become symptomatic and she was concerned about esthetics. The patient reported the tooth had been traumatically avulsed and re-implanted when she was aged 10 years.
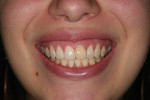
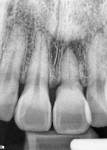
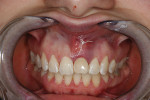
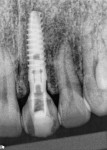
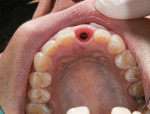
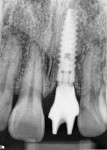
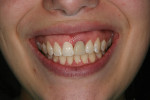
Clinical evaluation revealed a healthy periodontium, a thin biotype, and several Miller Class 1 recession defects. The tooth was rotated distobuccally and highly discolored (Figure 1). The tooth form was tapered, and the central papilla length was approximately 50% of the overall tooth length. Findings from the radiographic evaluation (Figure 2) revealed periapical radiolucency, a fully calcified pulp chamber, a highly constricted root canal, and a short root with areas of resorption. An unusual finding was the existence of a radiopaque buildup on the root surface just apical to the cementoenamel junction. The author did not think it was calculus deposits as the rest of the patient’s teeth did not exhibit significant buildup and probing depths and bleeding on probing were negligible. It was surmised that it was either residual composite from a splint that may have been applied at the time of re-implantation, which seemed improbable based on the position, or a cementum callus related to posttraumatic hypercementotic repair of the torn cementum surface.3 The latter was more likely.
The current case presented with challenging parameters: high esthetics desire, high smile line, tapered tooth form, thin gingival biotype, long crest to contact, and, as was discovered on bone sounding, no buccal plate. The patient was advised about the high degree of esthetic unpredictability of an implant approach and the possible need for multiple surgeries and/or a compromised result. In light of the highly unfavorable esthetic risk for implant treatment, the author recommended attempting to save the tooth by performing root-canal therapy, which, if successful, would be followed by a ceramic restoration to improve tooth esthetics. The patient was further advised if root-canal therapy was unsuccessful, extraction and restoration with a 3-unit fixed dental prosthesis may be the treatment of choice. The patient agreed to attempt root-canal treatment first.
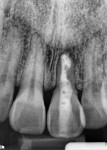
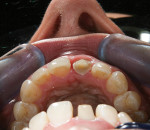
Root-canal treatment was performed, and on condensation of the gutta-percha filling material, extensive resorption defects were discovered (Figure 3). After several weeks, symptoms persisted along with inflammation of the buccal mucosa. It was decided that extraction and an implant-supported restoration would be the next step.
It is widely accepted today that when treatment approaches are kept as minimally invasive as possible, treatment outcomes are more likely to be favorable as treatment modalities are less traumatic and will lead to less post treatment complications, such as hard-tissue resorption and soft-tissue recession.4 To that end, the author chose to employ a minimally invasive approach introduced to him by a Brazilian colleague,5,6 Dr. Robert Carvalho daSilva, whose periodontics group, ImpalntePerio in Sao Paulo, Brazil, had been using the technique for almost a decade with highly predictable outcomes.
The technique is a variation on immediate dentoalveolar restoration by da Rosa et al,7 substituting guided bone regeneration for a cortical bone graft harvested from the tuberosity, along with a simultaneous connective tissue graft. They had found high esthetic success at up to 58 months in 18 patients. Noelken et al,8 using a similar approach, reported statistically significant improvement in the pink esthetic scores in 16 cases at 13 to 36 months.
This technique involves extraction, flapless immediate-implant placement, hard-tissue augmentation of the vertical buccal defect, and soft-tissue augmentation through a buccal pouch, along with immediate provisionalization. In other words, the process is combined into 1 minimally invasive procedure—steps that may otherwise have taken 3 or 4 visits throughout several months.
This protocol is based on several well-understood biologic and clinical principles. First among these is a thorough understanding of extraction socket healing and the potency for regeneration in the healing extraction socket.9 Rupture of the periodontal ligament initiates a cascade of bone repair and regeneration that is unique compared with other forms of osseous healing. Placing an implant at the time of extraction takes advantage of this high healing potential. It has been shown that bone will form into the gaps surrounding the titanium surface and the walls of the extraction socket.10
This also comes into play for regenerating the missing buccal plate. The extraction-socket healing cascade boosts an already effective method of simultaneous implant placement and simultaneous guided bone regeneration of buccal dehiscences,11 known as the “sandwich” graft. As long as the buccal surface of the implant is within the confines of the bony housing, simultaneous guided bone regeneration will regenerate the missing buccal bone. This procedure utilizes a layer of autogenous bone particles covered by another layer of anorganic bovine bone mineral and a resorbable collagen barrier membrane.
In addition, studies have shown, due to the unavoidable reduction in buccal bone volume after tooth extraction, it is advisable to augment the buccal soft-tissue volume with an interpositional connective tissue graft.12 The width and thickness of the keratinized mucosa surrounding the implant/restorative interface minimizes the potential for facial soft-tissue recession, which could result in an unfavorable esthetic outcome.13
Finally, immediate provisionalization with an appropriately contoured screw-retained crown provides support for soft-tissue healing and development of a favorable emergence profile.14 Failure to provide this support will result in a collapse of the gingival collar and necessitate additional treatment and possible additional surgery to correct.
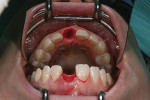
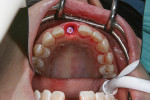
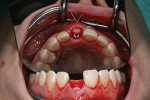
After the area was anesthetized, bone sounding was performed, and it was discovered that the buccal aspect of the root lacked bone. The tooth was extracted atraumatically, and the socket was debrided thoroughly (Figure 4). The buccal bone defect was found to be 4 mm wide and 6 mm high. A full-thickness pouch was created with sharp and blunt reflection that extended at least 3 mm around the defect in all directions. No vertical releasing incisions were made. A subepithelial connective tissue harvest was taken from the left palate. The implant osteotomy was prepared according to 3D immediate implant placement protocol, in the palatal aspect of the socket, leaving a gap of approximately 2 mm from the buccal wall (Figure 5), 3 mm from the desired free gingival margin, less than a 20° angulation, and several millimeters beyond the root fundus to achieve primary stability. The osteotomy was prepared 1 drill size smaller than the manufacturer’s recommendation to ensure adequate insertion torque (ie, more than 35 Ncm) and primary stability for immediate provisionalization.
A drilling protocol was followed that allowed harvesting of autogenous bone chips from the osteotomy.15 The 2-mm pilot drill was used at 1500 rpm with saline irrigation; all other twist drills were used at 50 rpm without irrigation, and the bone chips were collected from the drill flutes after each pass. A 16-mm-long, standard-diameter implant was inserted with 45 Ncm of torque.
To create the initial, screw-retained provisional restoration, the extracted tooth was sectioned 3 mm apical to the cementoenamel junction and prepared to fit over a temporary titanium abutment. The internal aspect of the tooth was etched and conditioned with a light-cured bonding agent. Flowable composite was used to lute the tooth to the temporary abutment. The assembly was unscrewed from the implant and finished extraorally, developing an undercontoured, transmucosal neck (Figure 6). This transmucosal undercontour is intended to reduce ischemia on the connective tissue graft and to promote the development of a thick band of tissue around the abutment neck. The finished provisional was set aside, and a healing abutment was placed to prevent bone-graft particles from entering the internal screw access.
A very stiff resorbable collagen membrane was trimmed to shape and placed into the buccal pouch. The autogenous bone chips were mixed with an equal amount of anorganic bovine bone mineral and condensed into the gap between the implant surface and membrane (Figure 7). Using a purse-string suture, the connective tissue graft was drawn into the pouch between the membrane and soft tissue (Figure 8). The provisional restoration was placed with finger torque, and the access hole was sealed (Figure 9 and Figure 10).
Postoperative visits were scheduled at 2 weeks, 4 weeks, and 2 months. Healing proceeded uneventfully, with the patient reporting no pain. No swelling, inflammation, or mobility was noted at any time. At 4 months, the provisional restoration was removed (Figure 11), a polyvinylsolixane transfer impression was taken, and a soft-tissue model was fabricated. This model was utilized to create a modified provisional. This alteration involves adding material to bulk up the buccal margin approximately 0.5 mm to reposition the free gingival margin apically. To prevent ischemia and reduce the risk for uncontrolled recession, 3 such modifications at 1-month intervals were performed. The final provisional remained in place for 6 weeks prior to impression-taking to allow for adequate tissue maturation. At the patient’s request, minor adjustments were made to the incisal edge of the adjacent central and mimicked in the provisional.
A custom, zirconia abutment was fabricated using a technique to duplicate the developed transmucosal and emergence profile of the final provisional.16 An acrylic pattern and transfer model were sent to the laboratory for scanning and milling. The abutment was fabricated with a zirconia body luted to a titanium sleeve, which has been shown to demonstrate long-term durability when compared to an all zirconia design.17
The final abutment was inserted with 35 Ncm torque (Figure 12). The access opening was sealed with an opaque composite with the same shade as the zirconia. The existing provisional was reamed out and relined to create a cement-retained restoration (Figure 13). A vinyl polysiloxane (VPS) impression was made along with counter model and bite registration and sent to the laboratory for fabrication of a pressed lithium-disilicate crown. The patient made 3 visits to the laboratory for custom shade matching and characterization.
At the final insertion visit, the soft-tissue volume was found to be stable (Figure 14). On achieving satisfactory fit and appearance for the author and patient, the crown was cemented with a dual-cure resin cement. Unlike natural teeth, implants lack a fibrous connection at the base of a sulcus. As such, the flow of excess cement beyond the gingival margin is possible and can be extremely difficult to detect and remove. This problem has been reported to be a major cause of peri-implantitis.18 To avoid this issue, a cementing protocol19 (Figure 15) was utilized to reduce cement thickness to a minimum and thus eliminate almost any overflow. A fast-setting VPS material was injected into the intaglio of the crown to create a die. This was used as a plunger to exude the excess cement and develop a thin film layer within the intaglio of the crown. Insertion with this technique resulted in minimal excess cement directly at the crown-gingival interface, which was easily and thoroughly removed at the cement’s gel phase (Figure 16). The patient was dismissed and scheduled for a 2-month follow-up to observe soft-tissue response.
At the 2-month follow-up visit, the soft tissue was stable and exhibited no inflammation. The patient was extremely satisfied with the outcome and expressed no dissatisfaction with the procedures or time involved. The patient was advised to return for once-yearly follow-up to monitor hard- and soft-tissue response.
Conclusion
The current paper described the treatment of a challenging esthetic case. A minimally invasive approach, which combined immediate implant placement, hard- and soft-tissue augmentation, and immediate provisionalization in 1 visit, was utilized to develop a highly acceptable outcome. Esthetic single-tooth implant-supported restorations present a trial for today’s practitioners. Utilizing a well-developed, evidence-based, minimally invasive approach can help in achieving long-term outcomes that are satisfactory to both the doctor and patient.
About the Author
David E. Azar, DDS, FICOI Director, gIDE NYC Implant Study Club; Private Practice, New York City, New York
References
1. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11):895-896,898, 900.
2. Dawson A, Chen S, Buser D, et al. The SAC Classification in Implant Dentistry. Berlin, Germany: Quintessence Publications; 2009.
3. Aisenberg MS. Adaptability of the periodontal membrane. J Dent Res. 1947;26(6):421-425.
4. Becker W, Goldstein M, Becker BE, Sennerby L. Minimally invasive flapless implant surgery: a prospective multicenter study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S21-S27.
5. Carvalho da Silva R. Lecture to the postgraduate periodontal & implantology students at NYUCD, Jan. 27, 2014.
6. Silva RC, Joly JC, Carvalho PFM. Abordagens alveolares: implantes imediatos x reconstrução alveolar. In: Perio-Implantodontia Estética. São Paulo, Brazil: Quintessence; 2015:504-753.
7. Rosa JC, Rosa AC, Francischone CE, Sotto-Maior BS. Esthetic outcomes and tissue stability of implant placement in compromised sockets following immediate dentoalveolar restoration: results of a prospective case series at 58 months follow-up. Int J Periodontics Restorative Dent. 2013;34(2):199-208.
8. Noelken R, Kunkel M, Wagner W. Immediate implant placement and provisionalization after long-axis root fracture and complete loss of the facial bony lamella. Int J Periodontics Restorative Dent. 2011;31(2):175-183.
9. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32(2):212-218.
10. Akimoto K, Becker W, Persson R, et al. Evaluation of titanium implants placed into simulated extraction sockets: a study in dogs. Int J Oral Maxillofac Implants. 1999;14(3):351-360.
11. Park SH, Lee KW, Oh TJ, et al. Effect of absorbable membranes on sandwich bone augmentation. Clin Oral Implants Res. 2008;19(1):32-41.
12. Rungcharassaeng K, Kan JY, Yoshino S, et al. Immediate implant placement and provisionalization with and without a connective tissue graft: an analysis of facial gingival tissue thickness. Int J Periodontics Restorative Dent. 2012;32(6):657-663.
13. Kan JY, Rungcharassaeng K, Lozada JL, Zimmerman G. Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2-to 8-year follow-up. Int J Oral Maxillofac Implants. 2011;26(1):179-187.
14. Rompen E, Raepsaet N, Domken O, et al. Soft tissue stability at the facial aspect of gingivally converging abutments in the esthetic zone: a pilot clinical study. J Prost Dent. 2007;97(6):119-125.
15. Anitua E, Carda C, Andia I. A novel drilling procedure and subsequent bone autograft preparation: a technical note. Int J Oral Maxillofac Implants. 2007;22(1):138-145.
16. Marchack CB, Vidjak MA, Futatsuki V. A simplified technique to fabricate a custom milled abutment. J Prost Dent. 2007;98(5):416-417.
17. Carvalho MA, Sotto-Maior BS, Del Bel Cury AA, Pessanha Henriques GE. Effect of platform connection and abutment material on stress distribution in single anterior implant-supported restorations: a nonlinear 3-dimensional finite element analysis. J Prosthet Dent. 2014;112(5):1096-1102.
18. Michalakis KX, Hirayama H, Garefis PD. Cement-retained versus screw-retained implant restorations: a critical review. Int J Oral Maxillofac Implants. 2003;18(5):719-728.
19. Wadhwani C, Piñeyro A. Technique for controlling the cement for an implant crown. J Prosthet Dent. 2009;102(1):57-58.