Comparison of Healing Following Tooth Extraction With Ridge Preservation Using Anorganic Bovine Bone Mineral Particulate and Self-Expanding Composite Graft
Farah Masood, DDS, MS; Jason Nicholson, DDS, MS; Joy Beckerley, DDS, Med, MS; Hui Liang, DDS, PhD; and Lida Radfar, DDS, MS
Abstract
Objectives: To study the radiographic mean grey values after bone grafting and to clinically evaluate the intraoral alveolar ridge dimensional stability with anorganic bovine bone mineral (ABBM) particulate and a patented self-expanding composite graft (SECG) after 6 months of healing. Methods: A total of 20 single-rooted tooth-extraction sites grafted with either ABBM or SECG were evaluated radiographically and clinically after 6 months of healing, prior to dental implant placement. A multivariable mixed regression model was used. Results: Mean grey values at the coronal, midroot, and apex levels within the socket were compared. A significant difference was shown in the midroot and apex maxillary regions. For both of these regions, the estimated mean grey value of ABBM was significantly lower than that of SECG. No significant difference was noted in the ridge-width change patterns between the two materials. Conclusion: This study supports that suggestion that newer SECG is as efficacious in terms of mean grey value and alveolar ridge stability as the previously available ABBM.
Bone grafting is performed to preserve or reestablish the bony architecture and buccolingual and vertical dimensions of the alveolar ridge. After a tooth extraction, the alveolar bone remodels, with the greatest changes occurring within the first 3 months.1 It was reported that 25% of total bone width and 4 mm of ridge height are lost in the first year after extraction.2
Bone-grafting materials are derived from a variety of sources: same patient (autografts), same species (allografts), different species (xenografts), and synthetic materials (alloplasts). Autografts are thought to be the gold standard because they are osteoinductive, osteoconductive, and osteogenic. Autografts are harvested from the maxillary tuberosity, mandibular ramus, mandibular symphysis, tibia, and hip.3 These areas are corticated and may be used for both particulate (smaller pieces) and block graft (larger pieces) harvesting. However, autografts are associated with risks, including simple bruising and nerve damage. Therefore, allografts may be preferred for ridge preservation.
Primary implant stability can be decreased in low-quality bone.4 Digital grey-value analysis of bone may predict bone density and was found to be accurate for assessing bone-mineral density.5
Anorganic bovine bone mineral (ABBM) and self-expanding composite graft (SECG) (ACE Surgical Supply Co., acesurgical.com) are commercially available bone-grafting materials. ABBM is a xenograft made of deproteinized bovine bone (cancellous granules). Clinically, it is packed into the socket using an instrument. SECG is a xenograft that is a preshaped self-expanding composite material. It consists of cancellous bone granules and purified type I bovine collagen, which are compressed and preformed. The material expands to a predetermined size and shape when placed in a bleeding site. It is placed in the socket with a syringe, which possibly simplifies the technique.
Limited research has been performed that compared these two materials. The objectives of this study were to compare the radiographic mean grey values of ABBM and SECG bone-grafting material after 6 months of healing and study the dimensional stability of the grafted alveolar ridges by comparing clinically the buccolingual ridge measurements with ABBM and SECG after 6 months of healing.
Methods
Patients referred to the Graduate Periodontics Program at the College of Dentistry for possible implant placement after extraction of a nonrestorable tooth were candidates for this study. The Institutional Review Board approved the study protocol. At the initial appointment, patients were evaluated medically and dentally according to selection criteria. Patients were given verbal and written information regarding the protocol and signed the written consent forms. Both female and male patients aged ≥18 willing to receive bone grafting were included. Exclusion criteria included medical disorders known to adversely affect implant success such as recent myocardial diseases and cerebrovascular accident, bleeding disorders, active cancer treatment, immunosuppression, uncontrolled diabetes, osteoporosis, drug abuse, psychiatric illness, intravenous bisphosphonate, history of radiation treatment to the head and neck, smoking ≥10 cigarettes per day, or use of other tobacco products.6,7
The patients were divided into two groups for bone grafting: ABBM and SECG. Initial coin toss determined the assignment for the first graft. Subsequent group assignment was done by alternating the two bone-grafting materials. For the ABBM group, particulate graft was hydrated in sterile saline and placed into the socket using a dental instrument. For the SECG group, a preformed shape was carried in a syringe and inserted into the socket.
First visit included obtaining history, consent form, head and neck and hard- and soft-tissue examinations, and preoperative digital x-ray images of the sites using an XCP instrument (DENTSPLY Rinn, rinncorp.com). Teeth were extracted under local anesthesia using 2% lidocaine with 1:100,000 epinephrine. A full-thickness flap was reflected. An examiner measured baseline buccolingual-ridge dimensions with a periodontal probe (11 Colorvue®, Hu-Friedy, hu-friedy.com) at the most crestal and convex point of the extraction site. Bone grafts were placed according to the assigned group and were covered with ConFORM™ absorbable collagen membrane (ACE Surgical Supply Co.) and sutured with Vicryl® absorbable suture (Ethicon US, LLC, ethicon.com). Every effort was made to achieve primary closure, but it was not always possible over every extraction site. Postoperative instructions, antibiotics, and pain medication prescriptions were given.
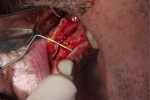
At 1-, 4-, and 12-week postoperative visits, photographs of the surgical sites were taken and wound healing was evaluated. The 6-month postoperative visit included reviews of medical history, oral examination, and digital periapical radiography. After local anesthesia, a full-thickness flap was reflected. The buccolingual bony dimensions of the ridge were measured again using a periodontal probe by the same examiner (Figure 1). Later, a dental implant would be placed.
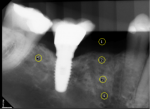
Regarding image acquisition and analysis, a reference aluminum step wedge (Margraf Dental Mfg. Inc., margrafdental.com) was fixed on the digital sensor (RVG 6100, Carestream Dental, carestreamdental.com), avoiding the superimposition over the region of interest. A handheld x-ray unit (NOMAD Pro™, Aribex Inc., aribex.com) was used for exposures. Density variations produced by the exposures were addressed and digitally similar step-wedge densities on radiographic images were provided.8 Images were exported in TIFF format and saved in a desktop folder, and were later imported into ImageJ software (National Institutes of Health) to study the mean grey values. On the images, three small circles similar in size were created in the center of the previous extraction socket at the crest, midroot, and apex (Figure 2 [circles 2 through 4]). Two independent calibrated examiners recorded the grey-value measurements at these sites.
Statistical Analysis
For ridge width pre- and post-grafting measurement, a mixed model with random intercept was used to account for the variability between subjects at baseline. An interaction term was tested to evaluate the overall change pattern between the two groups. A multivariate mixed regression model with random patients and examiners was used to account for the variability within material and location. Stratified analysis was applied once the interaction term was significant. Standard deviation and coefficient of variance of the difference between two measurements and Bland-Altman plots were provided to evaluate the reliability of the repeated measurements between examiners and within examiner. A two-sided 0.05 alpha level was used to define statistical significance.
Results
The study was conducted over an 18-month period. The age range of the patients was 27 to 65 years with a mean age of 49 years. Female to male ratio was 11:5.
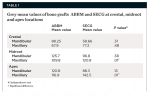
A total of 20 bone graft sites were analyzed radiographically with ImageJ software to obtain the grey values at three locations (apex, midroot, and crest) within the grafted socket area after 6 months of healing. The estimated mean grey values of the crestal, midroot, and apex areas of the mandible and crestal area of the maxilla were not significantly different between the two materials (P = .31, .38, .13, and .48, respectively). For the maxillary arch, the estimated mean grey values of the midroot and apex with ABBM were significantly lower than the estimated mean grey value of the SECG material (P = .01) (Table 1).
Buccolingual-ridge dimensions were also compared. Mean response profile between the two study materials showed that the SECG was dimensionally more stable than the ABBM. The change patterns from pre- and post-procedures between the two materials did not differ significantly (Figure 3).
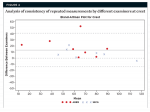
An analysis of internal consistency of repeated measurements by different examiners was accomplished by using the Bland-Altman plot, which is a visual representation of the differences between the two examiners. The intra-examiner measurements were more consistent than the interexaminer measurements. Crestal measurements by examiner 1 were typically higher than those of examiner 2 (Figure 4 through Figure 6).
Discussion
Prior to implant placement, ridge preservation is important in preventing deficiencies in the alveolar ridge. Deficient alveolar ridges may require bone augmentation procedures later, which may increase total treatment time and expense.
The authors found that the estimated mean grey value with ABBM was significantly lower than SECG for both midroot and apex maxillary regions. Other measured areas did not show any significant differences.
Although the authors found that bone dimension was more stable buccolingually with SECG, they found no statistically significant difference in buccolingual dimensions over time between the two groups. The evaluation of grey values using ImageJ software may aid in treatment planning. From a clinical standpoint, a higher mean grey value would seem to indicate a more mature and developed site for implant placement. Lower mean grey values on digital intraoral x-ray images may indicate that the bone is not ready for implant placement and/or more time may be needed for bone maturation. The denser the bone, the easier it is for the clinician to achieve primary stability of the dental implant, which will aid in implant success.
The mean grey values from ImageJ software for all sites’ regions of interest were evaluated within the maxillary and mandibular arches to account for the density variability between the two arches. Bone mineral density has been reported highest in the mandibular anterior region and lowest in the maxillary anterior and premolar regions.8 Therefore, a consideration was made for the variability in density between the two arches.
Ridge preservation techniques in the past have involved the use of particulate bone-grafting material. Packing particulate bone can be time-consuming for the clinician. At the beginning of the present study, it was thought that a possible drawback of using the SECG product (material in carrier) was the inability of the product to penetrate to the apex of the extracted socket. However, this study showed that both the midroot and the apex in the maxillary arch, in fact, exhibited greater osseous fill using SECG.
Bone graft may improve ridge height and width dimension. In a study by Iasella et al, the treatment group lost 1.2 mm of buccolingual dimension and the untreated group lost 2.6 mm.8 In the present study, a mean ridge width loss of 1.2 mm was seen in the ABBM group, which is similar to the study findings by Iasella et al, while in the SECG group a mean loss of only 0.25 mm in ridge width was reported, which possibly indicates that SECG performed slightly better.
ABBM needs to be hydrated before placement, which can be time-consuming. Use of the SECG required no hydration or additional delivery system for insertion, and use of the carrier made the placement simpler during the ridge preservation process.
Both of the grafts received a resorbable collagen membrane. This was done do ensure that ABBM particles were not lost from the alveolar socket. However, the SECG product may not require this additional measure because of the preformed expandable shape; a suture may be placed over the top of the socket to confine the preformed SECG in the socket until epithelium develops over the coronal portion of the socket. This may be a small but added benefit.
The authors found that the predetermined size and shape of SECG was sufficient to fill the entire extracted socket and yielded results at least similar to those of an already proven material such as ABBM. Additionally, the use of the preformed SECG product can decrease chairtime, which could benefit both the dentist and patient.
Conclusion
The authors recommend more research with a larger sample size and further evaluation of ridge dimensional stability over a longer period of time to draw stronger conclusions. In this study, similar results were found with both the ABBM and SECG products, and SECG offered an easier delivery method and shorter chairside time.
Disclosure
Funding for this project was provided in part by ACE Surgical Supply Co. The authors have no affiliation with the company.
About the Authors
Farah Masood, DDS, MS
Professor and Director of Radiology
Department of Oral Diagnosis and Radiology
University of Oklahoma College of Dentistry
Oklahoma City, Oklahoma
Diplomate
American Board of Oral and Maxillofacial Radiology
Jason Nicholson, DDS, MS
Private Practice
Provo, Utah
Joy Beckerley, DDS, Med, MS
Diplomate
American Board of Periodontology
Retired Clinical Associate Professor
Department of Graduate Periodontics
University of Oklahoma College of Dentistry
Oklahoma City, Oklahoma
Hui Liang, DDS, PhD
Associate Professor
Texas A&M Health Science Center
Dallas, Texas
Lida Radfar, DDS, MS
Clinical Professor
Department of Oral Diagnosis and Radiology
University of Oklahoma College of Dentistry
Oklahoma City, Oklahoma
Diplomate
American Board of Oral Medicine
References
1. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
2. Tallgren A. The continuing reduction of the residual alveolar ridges in complete denture wearers: a mixed-longitudinal study covering 25 years. J Prosthet Dent. 1972;27(2):120-132.
3. Hunt DR, Jovanovic SA. Autogenous bone harvesting: a chin graft technique for particulate and monocortical bone blocks. Int J Periodontics Restorative Dent. 1999;19(2):165-173.
4. Beer A, Gahleitner A, Holm A, et al. Correlation of insertion torques with bone mineral density from dental quantitative CT in the mandible. Clinical Oral Implants Res. 2003;14(5):616-620.
5. Vaccaro C, Busetto R, Bernardini D, et al. Accuracy and precision of computer-assisted analysis of bone density via conventional and digital radiography in relation to dual-energy x-ray absorptiometry. Am J Vet Res. 2012;73(3):381-384.
6. Hwang D, Wang HL. Medical contraindications to implant therapy: part I: absolute contraindications. Implant Dent. 2006;15(4):353-360.
7. Hwang D, Wang HL. Medical contraindications to implant therapy: part II: relative contraindications. Implant Dent. 2007;16(1):13-23.
8. Iasella JM, Greenwell H, Miller RL, et al. Ridge preservation with freeze-dried bone allograft and a collagen membrane compared to extraction alone for implant site development: a clinical and histologic study in humans. J Periodontol. 2003;74(7):990-999.