Endodontic Diagnostic Dilemmas: Thorough Examination May Preclude Inappropriate Treatment
Abstract:
In situations where suspicious lesions of undetermined origins are encountered, it is important for clinicians to consider non-endodontic and perhaps non-odontogenic sources to properly diagnose the condition in order to provide appropriate treatment. Differential diagnoses may include cysts, anatomic variations, and neoplastic lesions. Diagnostic dilemmas and misperceptions can be prevented and ineffective treatment avoided by thoroughly reviewing the patient’s medical and dental histories and employing a detailed clinical and radiographic examination. This article presents three cases that were referred to the authors’ clinic for endodontic treatment but were ultimately diagnosed as non-endodontic in origin.
In the course of practice, clinicians may encounter suspicious lesions of undetermined origins. In these situations, it is important to consider non-endodontic and perhaps non-odontogenic sources to properly diagnose the condition in order to provide appropriate treatment. Because of their wide range of treatments and prognoses, differential diagnoses of periapical lesions should include, but not be limited to, cysts, anatomic variations, and neoplastic lesions.1,2 By executing a thorough review of the patient’s medical and dental histories and employing a detailed clinical and radiographic examination, the clinician can prevent diagnostic dilemmas and confusion and avoid ineffective treatment.3-6
The following three cases were referred to the authors’ clinic for endodontic treatment. Each case was ultimately diagnosed as being non-endodontic in origin.
Case Report No. 1
A 45-year-old female patient with a non-contributory medical history was referred by her periodontist for endodontic treatment on her maxillary left lateral and central incisors, teeth Nos. 9 and 10. She revealed a recent history of swelling on the buccal and lingual soft tissues adjacent to these teeth. She denied a history of trauma, and no caries or restorations were present. Periodontal probing depths between 1.5 mm and 2 mm around both teeth were considered to be within normal limits. Repeated thermal pulp testing with an ice pencil also produced normal results; the cold was felt, but dissipated immediately upon removal of the ice pencil.
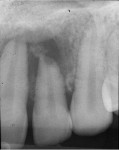
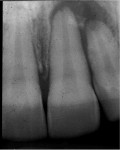
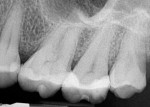
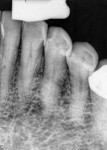
Radiographic examination revealed the presence of a large periapical radiolucency with some opacities within it that, combined with a vital pulp response, was inconsistent with an endodontic problem (Figure 1 and Figure 2). Differential diagnosis included lateral periodontal cyst, keratocyst, odontogenic tumor, traumatic bone cyst, periapical cyst, and nasopalatine duct cyst.
A follow-up visit 1 week later—after the patient had received antibiotic treatment (V-Cillin K 500 mg) from her periodontist—again produced a vital response to ice, and the swelling had subsided. Further discussion with the patient on a third visit revealed a history of pain and palatal bleeding following chewing on homemade venison sausage. Further review of the radiographs indicated the possible presence of a foreign body.
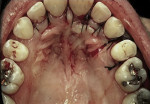
Surgical intervention on the anterior palate revealed a piece of deer bone that was sitting in a resorptive defect. While the patient was advised that endodontic treatment may be necessary, the foreign object was carefully excised without subsequent damage to the apical blood supply of either the central or lateral incisor (Figure 3). No endodontic therapy was required.
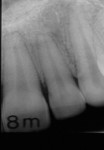
Healing occurred uneventfully, and an 8-month follow-up radiograph showed complete resolution of the periradicular radiolucency (Figure 4). Teeth Nos. 9 and 10 continued to respond normally to pulp tests when evaluated with cold.
Case Report No. 2
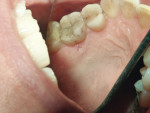
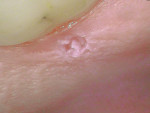
A 55-year-old female patient was referred to the authors’ clinic for endodontic examination and assessment of the maxillary left first molar (tooth No. 14), where there was a 3-mm x 3-mm ulcerated lesion with raised borders (Figure 5). Her medical history revealed psoriatic arthritis, which was managed with methotrexate and Enbrel.
Upon presentation, she reported that the lesion had been present for approximately 6 months and had not changed in size, shape, or character. The lesion was asymptomatic, as was the tooth adjacent to it (No. 14) (Figure 6 and Figure 7). There was no sensitivity to percussion, apical palpation tenderness, or mobility associated with tooth No. 14, and there were no signs of bone loss or radiolucencies/radiopacities on the radiographs. Pulp testing with an ice pencil revealed responses within normal limits on teeth Nos. 13 through 15. After the patient consented to a punch biopsy, a 6-mm x 6-mm excision was performed, including the 3-mm x 3-mm lesion, with the patient under local anesthesia using 2% lidocaine with 1:100,000 epinephrine. The underlying bone was intact without any evidence of resorption. The biopsy was stored in 10% formalin and transported to the pathology department.
Microscopic examination revealed keratinized squamous epithelium forming a lip bordering a depressed verruciform surface. The depressed lesional surface exhibited suprabasal acantholysis and formation of subjacent, elongated “test tube” rete ridges exhibiting epithelial atypia and extending into the superficial lamina propia.
The diagnosis made was warty dyskeratoma (WD), which is a benign condition, so no further treatment was advised. Also known as an isolated dyskeratosis follicularis,7 warty dyskeratoma is a benign8 epidermal proliferation with distinctive histologic findings that may mimic invasive squamous cell carcinoma9 and commonly manifests as an umbilicated (having a central mark or depression resembling a navel) lesion with a keratotic plug.10 WD has some histopathologic similarities to viral warts but is not caused by human papillomavirus (HPV), and the majority of these lesions display overall histopathologic features consistent with a follicular adnexal neoplasm.11 They are usually limited to the head, neck,12 scalp,13 or face and vulva.12
The patient was seen 2 weeks post-biopsy, at which time healing was deemed to be uneventful.
Case Report No. 3
A 79-year-old Caucasian woman was referred by her general dentist to the authors’ endodontics practice for root canal treatment of her lower left canine, tooth No. 22. The patient’s dental and medical histories were unremarkable. She appeared to be in good health; she was not taking any medications nor was she being treated for any systemic diseases.
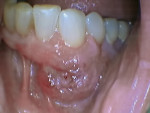
Her extraoral examination was noncontributory, revealing neither swelling nor lymphadenopathy. However, the intraoral examination revealed a large, round lesion on the mucobuccal gingiva adjacent to tooth No. 22. The lesion measured 1.5 cm x 1 cm high, was red, ulcerated, and painless (Figure 8). The patient denied receiving trauma to the area and was unaware of the lesion’s presence until her referring dentist found it incidentally. Tooth No. 22 and its adjacent teeth were unrestored, had no periodontal defects or fractures, and were not sensitive to percussion or to biting. There was no apparent radiographic evidence of pathology since all periodontal ligament (PDL) spaces appeared to be intact and the patient’s bone pattern was normal. Vitality testing of teeth Nos. 20 through 24 with tetrafluoroethane (the clinician’s choice in this case rather than using an ice stick) concluded that all teeth were vital and normal (Figure 9).
It was apparent that this lesion was not associated with a non-vital tooth requiring endodontic treatment. A differential diagnosis was made that included the following conditions: peripheral giant cell granuloma, squamous cell carcinoma, and granulomatous ulcer. The patient was then referred to a pathologist, who conducted an incisional biopsy of the lesion. Cryostat sections were taken for immunohistochemical diagnosis, which revealed the presence of a high-grade B-cell non-Hodgkin’s lymphoma (NHL). After the preliminary diagnosis, the patient underwent a computerized axial tomography (CAT) scan, followed by a full-body magnetic resonance imaging (MRI), which revealed an absence of malignancy elsewhere in the body. It was determined that the oral lesion was, in fact, a primary lesion and the patient was diagnosed with stage one NHL. After surgical removal of the oral lesion, the patient decided not to undergo radiation or chemotherapy, as the risks of treatment and its effect on a person her age outweighed the benefits.
Non-Hodgkin’s lymphoma occurs within the lymphatic system and can also arise extranodally. When NHL appears extranodally in the oral cavity, it is usually indicative of widely disseminated disease. However, on rare occasions, it can appear orally as a primary lesion. Oral NHL can spread via the lymphatic system and blood, giving rise to distant metastases, or by contiguous spread to adjacent tissues.14 The survival time is greatly dependent on the extent of disease dissemination and its aggressiveness. The literature places the 5-year survival rate of head and neck NHL at 65% to 73%.15-21
The prevalence of NHL appears to be on the rise among people afflicted with autoimmune disorders and those who are immunocompromised due to organ transplantation. Oral NHL has also been recognized as a first sign of acquired immunodeficiency syndrome (AIDS).
Conclusions
When an unusual lesion appears in the oral cavity that is unexplained by an endodontic or even an odontogenic source, it is important to suspect possible systemic pathology or other non-endodontic or non-odontogenic origins. A complete history and careful examination of the head and neck, along with radiographic examination and dental vitality testing, will help in determining the origin of these lesions. When a source of the lesion is not found, other pathology should be considered. Early diagnosis of any lesion significantly improves the outcome of treatment, and in cases of NHL, it significantly improves the patient’s prognosis.15
References
1. Faitaroni LA, Bueno MR, De Carvalhosa AA, et al. Ameloblastoma suggesting large apical periodontitis. J Endod. 2008;34(2):216-219.
2. Sirotheau Corrêa Pontes F, Paiva Fonseca F, Souza de Jesus A, et al. Nonendodontic lesions misdiagnosed as apical periodontitis lesions: series of case reports and review of literature. J Endod. 2014;40(1):16-27.
3. Rosenberg PA, Frisbie J, Lee J, et al. Evaluation of pathologists (histopathology) and radiologists (cone beam computed tomography) differentiating radicular cysts from granulomas. J Endod. 2010;36(3):423-428.
4. Faitaroni LA, Bueno MR, Carvalhosa AA, et al. Differential diagnosis of apical periodontitis and nasopalatine duct cyst. J Endod. 2011;37(3):403-410.
5. de Moraes Ramos-Perez FM, Soares UN, Silva-Sousa YT, da Cruz Perez DE. Ossifying fibroma misdiagnosed as chronic apical periodontitis. J Endod. 2010;36(3):546-548.
6. Rodrigues CD, Estrela C. Traumatic bone cyst suggestive of large apical periodontitis. J Endod. 2008;34(4):484-489.
7. Freedberg IM, Goldsmith LA, Katz S, et al. Fitzpatrick’s Dermatology in General Medicine. 6th ed. New York, NY: McGraw-Hill; 2003.
8. Diallo M, Cribier B, Scrivener Y. Warty dyskeratoma: infundibular histogenesis. Anatomoclinical study of 43 cases [article in French]. Ann Dermatol Venereol. 2007;134(8-9):633-636.
9. Chau MN, Radden BG. Oral warty dyskeratoma. J Oral Pathol. 1984;13(5):546-556.
10. Kaugars GE, Lieb RJ, Abbey LM. Focal oral warty dyskeratoma. Int J Dermatol. 1984;23(2):123-130.
11. Kaddu S, Dong H, Mayer G, et al. Warty dyskeratoma–“follicular dyskeratoma”: analysis of clinicopathologic features of a distinctive follicular adnexal neoplasm. J Am Acad Dermatol. 2002;47(3):423-428.
12. Duray PH, Merino MJ, Axiotis C. Warty dyskeratoma of the vulva. Int J Gynecol Pathol. 1983;2(3):286-293.
13. Griffiths TW, Hashimoto K, Sharata HH, Ellis CN. Multiple warty dyskeratomas of the scalp. Clin Exp Dermatol. 1997;22(4):189-191.
14. Parrington SJ, Punnia-Moorthy A. Primary non-Hodgkin’s lymphoma of the mandible presenting following tooth extraction. Br Dent J. 1999;187(9):468-470.
15. Kell T, Glassman G. Primary non-Hodgkin’s lymphoma presentation on the gingival mucosa: a case report. Oral Health Dental Journal. May 2008.
16. Eisenbud L, Sciubba J, Mir R, Sachs SA. Oral presentations in non-Hodgkin’s lymphoma: a review of thirty-one cases. Part I. Data analysis. Oral Surg Oral Med Oral Pathol. 1983;56(2):151-156.
17. Howell ER, Handlers PJ, Abrams MA, Melrose JR. Extranodal oral lymphoma. Part II. Relationships between clinical features and the Lukes-Collins classification of 34 cases. Oral Surg Oral Med Oral Pathol. 1987;64(5):597-602.
18. Non-Hodgkin Lymphoma. National Cancer Institute Web site. https://www.cancer.gov/cancertopics/types/non-hodgkin. Accessed March 7, 2014.
19. Wolvius EB, Schulten EA, van der Waal I. Non-Hodgkin’s lymphoma of the oral cavity as the first manifestation of AIDS. Br Dent J. 1997;182(3):107-118.
20. Rowley H, McRae RD, Cook JA, et al. Lymphoma presenting to a head and neck clinic. Clin Otolaryngol Allied Sci. 1995;20(2):137-144.
21. Economopoulos T, Asprou N, Stathakis N, et al. Primary extranodal non-Hodgkin’s lymphoma of the head and neck. Oncology. 1992;49(6):484-488.
About the Authors
Gary Glassman, DDS, FRCD(C)
Graduate Department of Endodontics, Faculty of Dentistry, University of Toronto, Toronto, Ontario, Canada;
Adjunct Professor of Dentistry, Director of Endodontic Programming, School of Oral Health Sciences, University of Technology, Jamaica, Kingston, Jamaica;
Private Practice limited to Endodontics, Toronto, Canada
Yair Lenga, DDS, MSc, FRCD(C), Dip. Perio
Private Practice, Toronto, Ajax, and Oshawa, Canada
Joseph D. Maggio, DDS
Private Practice limited to Endodontics, Lisle, Illinois