Lithium Disilicate: The Restorative Material of Multiple Options
Lee Culp, CDT and Edward A. McLaren, DDS, MDC
Abstract
As dentistry continues to evolve, new technologies and materials are continually being offered to the dental profession. Throughout the years restorative trends and techniques have come and gone. Some material developments have transformed the face of esthetic dentistry, while other initial concepts have already phased out and disappeared. Today, all-ceramic restorations continue to grow in the area of restorative dentistry, from pressed-ceramic techniques and materials to the growing use of zirconia, and new materials that can be created from CAD/CAM technology. This article will explore new uses for the all-ceramic material known as lithium disilicate, and the use of a digital format to design and process this material in new and exciting ways. An overview of the material as well as unique clinical procedures will be presented.
Embracing proven alternative solutions and transforming traditional methods can be challenging to dental restorative teams facing increasing patient demands while being tasked to deliver high-strength restorative options without compromising esthetic outcomes. Traditionally, dental professionals have used a high-strength core material made of either a cast-metal framework or an oxide-based ceramic (such as zirconia or alumina). This approach has two disadvantages.
Compared with glass-ceramic materials, the substructure material has high value and increased opacity but may not be esthetically pleasing.1 This is especially an issue in conservative tooth preparation when the core material will be close to the restoration's exterior surface.
The other problem is that although the high-strength material has great mechanical properties, the layering ceramic with which it is veneered exhibits a much lower flexural strength and fracture toughness.2,3 The zirconia core (with a 900 MPa to 1000 MPa flexural strength) is less than half of the cross-sectional width of a restoration; it must be completed with a veneering material with a flexural strength in the range of 80 MPa to 110 MPa range (depending on delivery method).4 The veneering material tends to chip or fracture during function. Also, such restorations depend significantly on the ability to create a strong bond interface between the dissimilar materials of oxide-ceramic and silica-based glass-ceramic, a bond that is not difficult to create.5 However, the quality of the bond interface can vary substantially because of cleanliness of the bond surface, furnace calibration, user experience, and other issues.
In today's industry, monolithic glass-ceramic structures can provide exceptional esthetics without requiring a veneering ceramic. Greater structural integrity can be achieved by eliminating the veneered ceramic and its requisite bond interface.6 The relative strength of the available glass-ceramic material has traditionally been the disadvantage of these restorations. Because of their flexural strength of 130 MPa to 160 MPa, they are limited to single-tooth restorations and adhesive bonding techniques are needed for load sharing with the underlying tooth.6 This has been resolved through the development of highly esthetic lithium-disilicate glass-ceramic materials.
The 70% crystal phase of this unique glass-ceramic material refracts light very naturally while also providing improved flexural strength (360 MPa to 400 MPa).7 This gives more indications for use and the ability to place restorations using traditional cementation techniques while also having strength and esthetics.
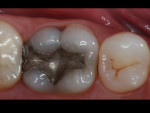
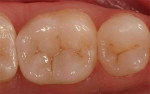
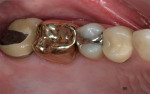
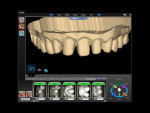
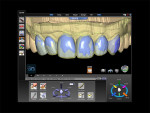
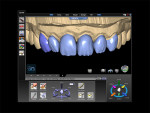
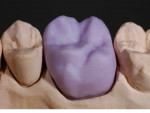
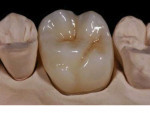
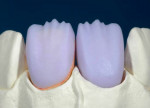
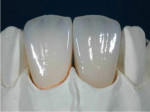
With a monolithic technique (Figure 1 and Figure 2), most restorations built from lithium-disilicate materials can be completely fabricated. This approach provides high strength and esthetics but requires surface colorants for the final shade. When in-depth color effects are needed, a partial layering technique may be employed. Although no longer a purely monolithic structure (Figure 3 and Figure 4) because the restoration maintains a large volume of the core material, the resulting restoration should reasonably maintain its high strength. However, no evidence supports this.
Esthetic Options
If covering or masking underlying tooth structure is part of the treatment plan, the restorative team can imagine doing so in an esthetic way. The ceramist can make that vision a reality with IPS e.max® (Ivoclar Vivadent, https://www.ivoclarvivadent.com) by using a very high-opacity ingot. Ingot opacities available for IPS e.max include high opacity (HO), medium opacity (MO), low translucency (LT), and high translucency (HT).7 The MO ingot can be used as an anatomic framework material if restorations must be fully layered. The LT ingot can be employed with stain and glaze methods or hybrid-layer techniques, which have been used for years with IPS Empress® Esthetic (Ivoclar Vivadent). The HT ingot is meant for staining and glazing techniques.
Choosing which of these four different esthetic options depends on the preparation and the technique to be used in order to match the adjacent dentition or restorations. In addition, the laboratory can select the processing choice that is appropriate for the selected restoration. IPS e.max includes press and computer-aided design/computer-aided manufacturing (CAD/CAM) options because lithium disilicate can be pressed from an ingot form or milled from a block form. If the CAD/CAM option is used, the technician will digitally design the restoration rather than perform a full wax-up and invest/press.
Preparation Options
If LT or HT ingots will be needed, then dentists can have flexibility with their preparations because of the translucent margins. This is the situation with partial preparations (eg, inlays, onlays, veneers)—the margins can be placed wherever clinically proper. IPS e.max's translucency enables dentists to place the margins virtually anywhere on the restoration, blending seamlessly with the natural dentition.
Dentists can use a traditional preparation of 1-mm to 1.5-mm reduction (eg, a full-crown preparation) if they need more opaque materials (eg, HO, MO). Because the resulting restoration will have a slight opacity, the margins will be equigingival or slightly subgingival. In either case, the material will be fully layered to create the final restoration. IPS e.max provides the choice of using traditional or creative preparation designs.
Cementation Options
Because lithium disilicate can be fully light-cure bonded or cemented using a self-etching primer with conventional resin-cement techniques, IPS e.max also provides options for cementation. Conventional self-etching primer cement is ideal for full crowns. For partial and veneer preparations in which an adhesive protocol will be used, full light-cure bonding is preferred.
Case Report
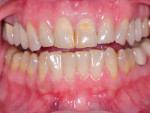
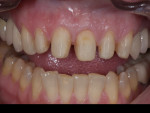
A 42-year-old woman presented with discolored teeth that had been repaired with various composite restorations placed throughout the years (Figure 5). A lingual amalgam restoration in tooth No. 10 and composite restorations in teeth Nos. 6, 8, 9, and 11 showed recurrent decay that was diagnosed with digital X-rays. She had a negative medical history and exhibited good oral hygiene with resultant periodontal health and asymptomatic teeth. Treatment options of zirconia or porcelain-fused-to-metal crowns or CAD/CAM all-ceramic restorations were discussed with the patient.
Ultimately, CAD/CAM all-ceramic restorations were tested. When proper preparation and occlusal design considerations are followed, properly placed CAD/CAM designed and milled restorations have been extremely successful. The patient made a preparation appointment. The existing restorations were removed, and teeth Nos. 6 to 11 were prepared for all-ceramic veneer restorations, following accepted CAD/CAM glass-ceramic preparation guidelines (Figure 6): Adequate clearance, rounded internal aspects, and equigingival butt-joint margins were ensured. Once the preparations were completed, conventional impressions were taken and poured in high-quality, laser-reflective dental stone.
Laboratory Communication
The dentist is to the dental technician what the architect is to the builder. Each has a primary role in indirect restorative dentistry, which is to perfectly imitate natural function and esthetics and translate that into a restorative solution. The communication paths between the clinician and technician require a thorough transfer of information—which includes functional components, occlusal parameters, phonetics, and esthetics—and continues throughout the restorative process, from the initial consultation through treatment planning, provisionalization, and final placement. The primary and conventional communication tools between the dentist and technician are:
- photography
- written documentation
- impressions of the patient's existing dentition
- the clinical preparation
- the opposing dentition
This information is used to create models, which are mounted on an articulator to simulate the mandibular jaw movements.
Traditional Indirect Restorative Process
The indirect restorative process involves the following steps: The clinician prepares the case according to the appropriate preparation guidelines, takes the impressions, sends these and other critical communication aspects to the laboratory, and the laboratory receives all the materials from the dentist. Then, the impressions are poured, the models are mounted, and the dies are trimmed. Appropriate restorations—layered, pressed, milled, cast, or combinations—are made. However, as restorative dentistry shifts further into the digital era, clinicians must change their perceptions and definitions of the dental laboratory. Traditionally, a laboratory is the site that receives and processes patient impressions and returns the completed restorations to the clinician, who adjusts and delivers them to the patient. Similar to how the Internet has transformed the communication landscape, the possibility to use CAD/CAM restoration files electronically has spurred evolutions in the way dental restorative teams perceive and structure the dentist—laboratory relationship.
The Digital Process
When the E4D LabWorks system (D4D Technologies, https://www.e4dsky.com) was introduced in 2008 (Figure 7), it was the first computerization model to accurately present a real 3-D virtual model and automatically account for the occlusal effect of the opposing and adjacent dentition. It could enable the user to design 16 individual full-contour, anatomically correct teeth simultaneously. The device condenses the information from a complex occlusal case and displays it in a user-friendly format that allows clinicians with basic knowledge of dental anatomy and occlusion to modify the design. Once this is completed, the information is sent to the automated milling unit.
The innovation of digitally designed restorations meant some of the more mechanical and labor-intensive procedures (eg, waxing, investing, burnout, casting, pressing) involved in the conventional fabrication of a restoration were essentially automated. The dentist and technician had a consistent, precise method to construct functional dental restorations.
A file is created within the design software for each patient. The operator can input the patient's name or record number and selects the appropriate tooth number(s) to be treated. Each tooth's planned restoration is checked (eg, full-crown, veneer, inlay, onlay). Lastly, additional preferences include material choices and preferred shade. System defaults that can be set ahead of time or changed for each patient are preferred contact tightness, occlusal contact intensity, and virtual die spacer, which determines the internal fit of the final restoration to the die/preparation. All of this information can be entered prior to treatment or changed at any time if the actual treatment differs from what was planned.
When the images of the preparation, provisional restorations, and opposing dentition are captured, the computer has all of the required information for preparing the working models, preparation, and opposing model. The real 3-D virtual model is then shown on the screen and can be rotated and viewed from any perspective (Figure 8). In designing the restoration, the first step must be to digitally define the final restoration's parameters. This is achieved by employing the opposing and adjacent teeth for occlusal interproximal contact areas and, finally, the gingival margins of the preparation.
Using input and neighboring anatomic detail as a basis, the software will place the restorations in an appropriate position—but not necessarily the clinically ideal location. Instead, the operator relies on his or her knowledge of form and function and experience to reposition and contour the restoration as needed. As the crown's position and rotation are fine-tuned, the software's automatic occlusion application will readjust each triangular ridge and cusp tip—and the restoration's contours, contacts, and marginal ridges—employing the preferences and bite registration information. The virtual restoration adapts all of the parameters in relation to the new position. Instantaneously, the position and intensity of each contact point is illustrated graphically and color-mapped, where it can easily be modified based on the operator's and clinician's preferences. Through a variety of virtual carving and waxing tools, customization and artistry are also possible. These tools can be used to adjust occlusal anatomy, preferences, and contours, reflecting actual laboratory methods. Each step in the process is updated on the screen, therefore the effect of any changes is immediately apparent.
For this case, three files were loaded into the computer software for restoration design. Scans of the preparations, provisional restorations, and opposing dentition were joined to form a composite file that accurately represented the patient's oral situation (Figure 9). When the final virtual restorations were completely designed (Figure 10), the milling chamber with the predetermined shade, opacity, and size of the IPS e.max block was loaded, an onscreen button was pressed and, in a short time, an exact replica of the design was produced in ceramic.
Glass-ceramics are categorized according to their chemical composition and/or application. The IPS e.max lithium disilicate is composed of quartz, lithium dioxide, phosphor oxide, alumina, potassium oxide, and other components.7 These powders are combined to produce a glass melt, which is poured into a steel mold where it cools until it reaches a specific temperature at which no deformation occurs. This method results in minimal defects and improved quality control (due to the translucency of the glass). The blocks or ingots are generated in one batch, based on the shade and size of the materials. Because of the low thermal expansion that results during manufacture, a highly thermal shock-resistant glass-ceramic is produced.
Next, the glass ingots or blocks are processed using CAD/CAM milling procedures or lost-wax hot-pressing techniques (IPS e.max Press) (Figure 11). The IPS e.max CAD "blue block" is based on two-stage crystallization: a controlled double nucleation process, in which the first step includes the precipitation of lithium meta-silicate crystals. Depending on the quantity of colorant added, the resulting glass-ceramic demonstrates a blue color. This ceramic has superior processing properties for milling. After the milling process, a second heat-treating process is performed in a porcelain furnace at approximately 850°C; the meta-silicate is dissolved and the lithium disilicate crystallizes. This results in a fine-grain glass-ceramic with 70% crystal volume incorporated into a glass matrix.
With two crystal types and two microstructures during processing, the IPS e.max CAD material demonstrates distinctive properties during each phase. The intermediate lithium meta-silicate crystal structure promotes easy milling, without excessive bur wear, while maintaining high tolerances and marginal integrity. In the "blue" stage, the glass-ceramic contains approximately 40% volume lithium meta-silicate crystals that are approximately 0.5 μm. The final-stage microstructure of lithium disilicate gives the restoration its superior mechanical and esthetic qualities. In this stage, the glass-ceramic contains approximately 70% volume lithium-disilicate crystals that are approximately 1.5 μm (Figure 12, Figure 13, Figure 14 and Figure 15).
The Laboratory Process
Once designed and milled, the IPS e.max ceramic restorations were then prepared for final esthetic adjustments. After the "milling sprue" was removed, the technician defined surface texture and occlusal anatomy using diamond and carbide burs, carefully avoiding any alteration to the perfected occlusal and interproximal contacts. Afterward, the restorations were rinsed to remove surface debris and dried. Then, the milled "blue" restorations were placed in a conventional ceramic furnace for the crystallization process. These restorations were digitally designed with an incisal "cut back" design that would allow a minimal application of translucent ceramics to artistically mimic the incisal effects found in nature. Contoured to final anatomic shape, the restorations were further esthetically improved by the subtle coloring and glaze.
Restoration Placement
Next, 5% hydrofluoric acid (IPS Ceramic Etch, Ivoclar Vivadent) was applied for 20 seconds onto the internal surfaces of the glazed restorations, and then rinsed and dried. This was followed by a silane coupling agent (Monobond Plus, Ivoclar Vivadent), which was also placed for 1 minute onto the internal surfaces, and then air-dried. For the final cementation, Variolink® Veneer (Ivoclar Vivadent) was used. After excess cement was removed, final light-curing was accomplished. The occlusal contacts were then reviewed and excursive pathway freedom was confirmed. Because of the correct capture and alignment of the bite registration information, few adjustments were required.
Conclusion
IPS e.max is about restorative options. Dentists and technicians now have a material with which they can do anterior or posterior restorations. With four different opacities or translucencies available, a variety of creative esthetic options can be accomplished in a restoration. Dentists and their laboratory ceramists now have the opportunity to be more creative for their patients (Figure 16, Figure 17 and Figure 18).
Disclosure
The primary author is a current consultant for Ivoclar Vivadent and D4D Technologies.
References
1. Kelly JR. Dental ceramics: current thinking and trends. Dent Clin North Am. 2004;48(2):513-530.
2. Vult von Steyern P, Carlson P, Nilner K. All-ceramic fixed partial dentures designed according to the DC-Zirkon technique. A 2-year clinical study. J Oral Rehabil. 2005;32:180-187.
3. Sailer I, Fehér A, Filser F, et al. Prospective clinical study of zirconia posterior fixed partial dentures: 3-year follow-up. Quintessence. 2006;37:685-693.
4. Sailer I, Fehér A, Filser F, et al. Five-year clinical results of zirconia frameworks for posterior fixed partial dentures. Int J Prosth. 2007;20:383-388.
5. Aboushelib MN, de Jager N, Kleverlaan CJ, Feilzer AJ. Microtensile bond strength of different components of core veneered all-ceramic restorations. Part II: Zirconia veneering ceramics. Dent Mater. 2006;22:857-863.
6. Tysowsky G. The science behind lithium disilicate: today's surprisingly versatile, esthetic and durable metal-free alternative. Oral Health J. 2009;March:93-97.
7. Ivoclar Vivadent. IPS e.max Lithium Disilicate: The Future of All-Ceramic Dentistry—Material Science, Practical Applications, Keys to Success. Amherst, NY: Ivoclar Vivadent; 2009:1-15.
About the Authors
Lee Culp, CDT
Chief Technology Officer
Microdental Laboratory
Dublin, California
Edward A. McLaren, DDS, MDC
Professor, Founder, and Director
UCLA Post Graduate Esthetics
Director
UCLA Center for Esthetic Dentistry
Los Angeles, California