Restoration of Unusually Shaped Canals With Post Endodontic Treatment: A Review of Progressive Approaches
Patrick L. Roetzer, DDS; Shika Gupta, DDS; and Karen A. Schulze DDS, PhD
Abstract
Various economic, time-efficient options in endodontic therapy are available for treating wide, flared, and/or unusual canals and re-treating flared canals. Conservation of tooth structure, minimal use of cement, and the strengthening of the core and/or remaining tooth structure when possible are critical treatment objectives. This article discusses new, progressive treatment modalities that minimize the amount of cement and composite resin needed, resulting in the conserving of remaining dentin. These modalities include the anatomic post-core, oval fiber post, individually formed fiber "bundle" post, fiber-augmented post, and accessory post techniques.
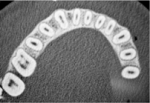
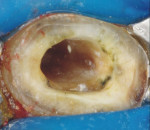
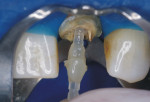
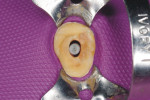
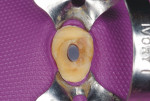
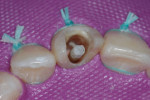
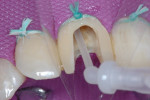
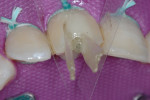
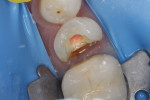
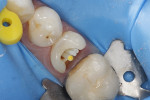
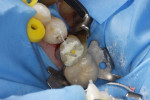
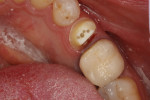
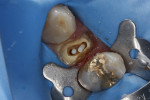
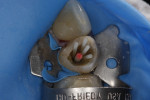
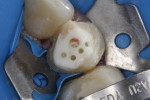
In the midst of the many advances made in restorative dentistry and implantology, a demand for endodontic treatments continues to persist. Some teeth requiring endodontic therapy present naturallywith oval-shaped, kidney bean-shaped (c-shaped), or ribbon-shaped canals (Figure 1).1Many such teeth bear these shapes after experiencing necessary endodontic access or coronal alteration (Figure 2). Some of these teeth also will be severely compromised due to the small amount of remaining tooth structure (dentinal walls), which may indicate the need for placement of a post to retain the subsequent core restoration, crown/bridge, or large Class II restoration.
Prefabricated metallic posts have been popular since the 1950s, as they provide an alternative to custom cast posts. Regardless of metallic composition, each of these two clinical techniques has its own drawbacks. The custom cast post traditionally offered a good "hand in glove" fit, often with a thin and uniform film thickness of cement, which was frequently achieved by removing additional dentin to prevent undercutting. However, this requires at least two appointments and a substantial laboratory fee while posing potentially catastrophic challenges to the remaining tooth structure by way of a mismatch in the elastic modulus. The modulus of dentin is ~18 GPa, that of dental gold is ~77, and that of base casting metal is over 100 GPa.
Prefabricated posts are available in both metal alloys and fiber-reinforced composites. Both types are produced with either a parallel shaft or a parallel coronal half and tapered apical half. In vitro studies in the 1980s suggested results that favored parallel posts over tapered. These studies were later countered with the advent of low-modulus fiber posts in the late 1980s.
This evolution has led to a trend toward fiber posts, where available.2 Pointed and tapered or double-tapered post shapes are becoming increasingly popular as opposed to parallel posts. Clinical trials of quartz and some glass-fiber posts reported good results with decementation rates equal to or better than metal posts, and there have been no reports of root fractures attributable to the posts themselves; they also showed better failure modes and statistics than metal posts.3-5
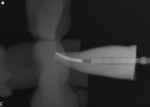
Circular parallel post systems are round from end to end and are effective only in the most apical portion of the post space. This is because most prepared post spaces demonstrate considerable flare in the coronal half. When the root canal is elliptical, a parallel-sided post will not be effective unless the canal is considerably enlarged (Figure 3).6
Treatment Options
The scope of this article is the consideration of options to treat wide, flared, and unusual canals and the re-treatment of flared canals in a practical, economical, and time-efficient manner. Emphasis is on the conservation of precious tooth structure, the use of minimal cement, and, where possible, the strengthening of the core and/or remaining tooth structure.
Dental cement has poor mechanical properties when thick; it is meant to serve in less than 50 µm thickness.7,8 Composite core restoratives have more filler than cements and generally higher mechanical properties, 9,10 but they possess approximately half the composite strength of fiber-reinforced, factory-produced composite posts.11 Therefore, for the purpose of maximizing the potential for a stronger post/core restoration (inside and outside the root) that, according to some research, 12-14 can reinforce/re-strengthen remaining tooth structure, the authors will evaluate several clinical approaches that minimize the amount of cement and composite resin and/or result in conserving remaining dentin.
Because resin restoratives still shrink somewhat when polymerized, it is important to consider what is known as the C-factor. No clinical restorative situation involves a higher C-factor index than post cementation, which involves five bonding walls. The goal in these situations is to displace as much of any material that is capable of shrinking with longitudinal fiber material that will not shrink, with the ultimate goal being crown retention.
In 2011 an international academic group co-authored an article that, taking into account these more progressive treatment modalities, sought to recommend newer methods for categorizing the optimal treatment approach, based on the size of the post endodontic treatment coronal opening versus the area or volume of fiber post available.15 The five techniques are the anatomic post-core, oval fiber post, individually formed fiber "bundle" post, fiber-augmented post, and accessory post.
Anatomic Post
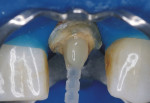
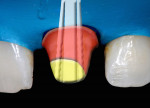
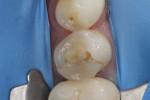
The anatomic post, sometimes called the "relined" post, is an indirect technique using a hybrid composite resin that is "pre-formed" to the surface of a prefabricated fiber post (Figure 4). When the root canal treatment is finished and the undercuts have been removed, a separating medium such as glycerin is used to lubricate the post space. The post, with composite applied to it (Figure 5), is inserted gently into the space and takes the shape of the irregular post space. It can be"spot-cured" for a couple of seconds and then removed, reseated, and spot-cured again. After final removal and confirmation of seating, the post is cured outside the canal. This technique is similar to the Duralay® cast post technique with a salt and pepper application to a plastic dowel.16,17 All surfaces must then be cleaned of the separating medium, and the polymerized assembly is oriented and cemented into place (Figure 6).
This technique requires no special materials and is highly intuitive to an experienced clinician. Grandini et al reported a very uniform film thickness of cement,18 while others such as Caceres et al noted fewer internal voids.19 Other studies have documented reduced stress transmission,20 less microleakage versus fiber post alone,21 greater bond adherence,22,23 and a reduced risk of catastrophic failures.24,25
Oval Post
Several prefabricated posts are available with an oval shape in the coronal section (Figure 7). Figure 8 and Figure 9 show how much cement could be displaced using a fiber post that is round at the apical end and ovoid at the coronal end. In many cases, this would seem an easy clinical solution. However, it requires an additional inventory of posts-of predetermined flare and diameter-and the oval space must be made to accommodate the oval posts, or vice versa.
Oval posts have been shown to displace cement, providing better adaptation,26 and this technique provides additional fracture resistance compared with the fiber bundle approach (described below.27 Kilinc et al determined that in deeper (10 mm) oval canals, oval posts provided more fracture resistance than round posts of the same composition.28 Finite element analysis evaluation indicates that oval fiber posts distribute interfacial stress better than circular posts, reducing adhesive and cohesive risks.29
Individually Formed Posts
In the 1990s, individually formed posts using "bundles" or strips of polyethylene or glass fibers (eg, Ribbond®, Ribbond, ribbond.com; FibreKor™, Pentron, pentron.com; EverStick®, GC America, gcamerica.com) were introduced as an alternative to prefabricated fiber posts.These low-modulus materials meet the necessary mechanical compatibility factor and yield high survival rates.30 Also, in vivo testing has revealed a tendency for reduced microleakage compared with metallic and zirconia posts.31,32 In an in vitro study by Azeem et al, the individually formed "bundle" approach provided higher fracture resistance than a popular preformed fiber post in oval-shaped canals.33 Al-Tayyan et al showed their retention comparable to a prefabricated fiber post.34 However, a 3-year clinical trial showed significantly higher survival rates for the teeth restored with a quartz glass fiber post compared with those restored with the polyethylene bundle post alone, but with similar failure modes.35 Managing the fibers in this technique, however, can be technique sensitive, as the fibers tend to wrap around instruments, not stay where they've been placed, and otherwise resist the dentist's attempts to pack them into the canals. These materials have a very low fracture/flexural strength compared with prefabricated fiber posts.
Fiber-Augmented Post
The fiber-augmented post technique, which first appeared in the mainstream literature in 2000,36 has been described in both a direct and a direct/indirect version. The technique mimics the anatomic post technique described earlier but uses unidirectional, pre-wetted reinforcing fiber to displace the composite. It is well known that the addition of fibers to composite resin improves the resin's mechanical properties. (Unfortunately, when these fibers are left exposed on the surface it presents esthetic and other problems.) The drawbacks are generally subjective: some clinicians find bundled fibers more difficult to handle and insert than the more rigid accessory posts. The direct fiber-augmented post technique is illustrated in Figure 10 through Figure 12.
The fiber-augmented technique has shown superior fracture resistance compared with restorations using fiber post alone.37 Moreover, the technique offered higher fracture resistance in flared canals than did those restored with rigid zirconia posts, with 100% non-catastrophic failures.38
Accessory Post
The accessory post technique has been in the literature since 2007. Posts in this technique are made from the same materials as full-sized fiber posts, with the same elastic modulus and radiopacity, with the elastic modulus ranging from 13 GPa to 50 GPa, (calculated at 30 degrees), and the radiopacity possibly reaching six times that of aluminum, depending on brand and post diameter. The accessory posts available on the market measure 0.5 mm at the apex and 0.8 mm at the coronal end and are tapered.
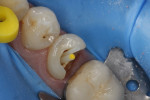
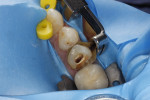
For widely flared and/or unusually shaped canals, the apical end of the space is prepared for the "master" post, as usual, with drills provided. During the trial fit, accessory posts also can be inserted to predetermine quantity, placement location, and even length. Once the cement is appropriately placed, the master post is inserted into place, followed immediately by the accessory posts (Figure 13).
More published data support this technique than the previous four approaches. The accessory post technique has been shown to minimize the cement thickness and volumes subject to shrinkage phenomena and reduce contraction or C-factor-related stress on the internal surfaces.39-41 This can lead to higher bond strength and better bond survival.42
The technique results in restored flared canals (extracted teeth) with flexural strength similar to cast post but with much improved failure modes.43-47 The use of accessory posts with a master fiber post showed fracture resistance higher than oval or round posts by themselves,38,47-49 cement or composite alone,50 and relined/anatomic post.51 Other examples of this technique are shown in Figure 14 through Figure 26.
Conclusion
Evolved technology in adhesives and composites, along with innovations in fiber reinforcement now afford the clinician numerous options for restoration of severely compromised teeth that previously would have been considered doomed to extraction, or subjected to threat of antiquated, labor-intensive, unesthetic restorative techniques such as custom cast posts and/or retention pins. C-factor management in root canals is critical to establishing and maintaining a robust dentin bond that will survive years of stress and strain. This article has presented evidenced-based techniques for assessing C-factor in canals and prescribing treatment modalities that will eliminate or minimize its efforts. Techniques that are effective and can be performed in a timely manner will help the modern dentist.
Acknowledgments
Dentistry and photography courtesy of Prof. Alejandro Bertoldi Hepburn, UDD, Concepcion, Chile, and Prof. Daniel Torassa, Univ. of Cordoba, Argentina; photography courtesy of Prof. Abelardo Baez Rosales, UMNAB, Vina del Mar, Chile. The authors would like to thank Ultradent Products, Inc. for its generous contribution of the UniCore Post and Drill System and Accessory Posts. The authors would also like to thank Zest Dental Solutions/Danville Materials for the Prelude SE Adhesive System.
About the Authors
Patrick L. Roetzer, DDS
Assistant Clinical Professor, Director of Operative Dentistry, Arthur A. Dugoni School of Dentistry, University of the Pacific, San Francisco, California
Shika Gupta, DDS
Associate Professor of Clinical Oral Health, Arthur A. Dugoni School of Dentistry, University of the Pacific, San Francisco, California
Karen A. Schulze DDS, PhD
Associate Professor of Preventive and Restorative Dentistry,Arthur A. Dugoni School of Dentistry, University of the Pacific, San Francisco, California
References
1. Weine FS. Endodontic Therapy. 4th ed. St. Louis, MO: Mosby; 1989:225-269.
2. Ahmed SN, Donovan TE, Ghuman T. Survey of dentists to determine contemporary use of endodontic posts. J Prosthet Dent.2017;115(7):642-645.
3.Cagidiaco MC, Goracci C, Garcia-Godoy F, Ferrari M. Clinical studies of fiber posts: a literature review. Int J Prosthodont. 2008;21(4):328-336.
4. Bitter K, Kielbassa AM. Post-endodontic restorations with adhesively luted fiber-reinforced composite post systems: a review. Am J Dent. 2007;20(6):353-60
5. Ferrari M, Cagidiaco C, Goracci C, et al. Long-term retrospective study of the clinical performance of fiber posts. Am J Dent. 2007;20(5):287-291.
6. Rosenstiel SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 3rd ed. Yearbook Medical Publications; 2000.
7. Burgess JO, Ghuman T. A practical guide to the use of luting cements. Academy of Dental Therapeutics and Stomatology. 2008:1-11.
8. Egilmez F, Ergun G, Cekic-Nagas I, et al. Influence of cement thickness on the bond strength of tooth-colored posts to root dentin after thermal cycling. Acta Odontol Scand. 2013;71(1):175-182.
9.Drummond JL, Lenke JW, Randolph RG. Compressive strength comparison and crystal morphology of dental cements. Dent Mater. 1988;4(1):38-40
10. Lu H, Lee YK, Oguri M, Powers JM. Properties of a dental resin composite with a spherical inorganic filler. Oper Dent. 2006;31(6):734-740
11. Stewardson DA, Shortall AC, Marquis PM, Lumley PJ. The flexural properties of endodontic post materials. Dent Mater. 2010;26(8):730-736.
12. D'Arcangelo C, De Angelis F, Vadini M, et al. In vitro fracture resistance and deflection of pulpless teeth restored with fiber posts and prepared for veneers. J Endod. 2008;34(7):838-341.
13. Hajizadeh H, Namazikhah MS, Moghaddas, MJ, et al. Effect of posts on the fracture resistance of load cycled endodontically treated premolars restored with direct composite resin. J Contemp Dent Pract. 2009;10(3):1-10.
14. Mangold, JT, Kern, M. What quit making a noiseInfluence of glass-fiber posts on the fracture resistance and failure pattern of endodontically treated premolars with varying substance loss: An in vitro study. J Prosthet Dent. 2011;105(6):387-393.
15. Boksman L, Hepburn AB, Kogan E, et al. Fiber post techniques for anatomical root variations. Dent Today. 2011;30(5):104,106-111.
16. Sabbak, S. Simplified technique for fabrication of cast posts and cores. J Prosthet Dent. 2000;83(6):686-687.
17. David R. Retro fabrication of a cast post and core to an existing crown. J Can Dent Assoc. 2005;71(5):335-338.
18. Grandini S, Goracci C, Monticelli F, et al. SEM evaluation of the cement layer thickness after luting two different posts. J Adhes Dent. 2005;7(3):235-240.
19. Caceres EA, Sampaio CS, Atria PJ, et al. Void and gap evaluation using microcomputed tomography of different fiber post cementation techniques. J Prosthet Dent. 2018;119(1):103-107.
20. Belli S, Eraslan O, Eraslan O, Eskitascioglu G. Effect of post-restoration on stress-distribution in roots with over-flared canals. J Dent Res. 2012;91(spec iss B): Abstract 160067.
21. Geramipanah F, Rezaei SM, Sichani SF, et al. Microleakage of different post systems and a custom adapted fiber post. J Dent (Tehran).2013;10(1):94-102.
22. Goncalves L, Rocha A, Carvalho C, Tavarez R. Effect of relining fiber post on retention to root canals. J Dent Res. 2016;95(spec iss A): Abstract 1072.
23. Rocha AT, Gonçalves LM, Vasconcelos AJC, et al. Effect of anatomical customization of the fiber post on the bond strength of a self-adhesive resin cement. Int J Dent. 2017;2017:5010712.
24. Raposo LHA, Silva GR, Santos-Filho PCF, et al. Effect of posts and materials on flared teeth's mechanical behavior. J Dent Res. 2011;90(spec iss A): Abstract 1862.
25. Clavijo VG, Reis JM, Kabbach W, et al. Fracture strength of flared bovine roots restored with different intraradicular posts. J Appl Oral Sci. 2009;17(6):574-578.
26. Coniglio I, Carvalho CA, Magni E, et al. Post space debridement in oval-shaped canals: the use of a new ultrasonic tip with oval section. J Endod. 2008;34(6):752-755.
27. Akkayan B, Atalay S, Gaucher H, Alkumru H. Effect of post geometry on the resistance to fracture of endodontically treated teeth with oval-shaped root canals. Canadian J Restorative Dent and Prosthodontics. 2010:20-26. https://www.dentalnews.com.br/downloads/artigos-cientificos/pinos-RTD/Akkayan;%20The%20effect%20of%20post%20geometry.pdf.pdf. Accessed May 22, 2018.
28. Kılınç H, Aslan T, Kılıç K, et al. Fracture resistance of teeth with oval canal morphology restored using oval and circular posts. J Oral Sci. 2016;58(3):339-345.
29. Er O, Kilic K, Esim E, et al. Stress distribution of oval and circular fiber posts in a mandibular premolar: a three-dimensional finite element analysis. J Adv Prosthodont. 2013;5(4):434-439.
30. Jimenez MP, Yaman P, Dennison JD, et al. Fracture resistance of endodontically treated teeth restored with composite posts. J Dent Res.2002;81(spec iss A): Abstract 0323.
31. Erkut S, Gulsahi K, Caglar A, et al. Microleakage in overflared root canals restored with different fiber reinforced dowels. Oper Dent. 2008;33(1):96-105.
32. Usumez A, Cobankara FK, Ozturk N, et al. Microleakage of endodontically treated teeth with different dowel systems. J Prosthet Dent. 2004;92(2):163-169.
33. Abo El-Ela, O.A., et al.Fracture resistance of anterior teeth restored with a novel nonmetallic post. JCDA, June 2008, Vol.74 No5
34. Al-Tayyan MH, Watts DC, Kurer HG, Qualtrough AJ. Is a "flexible" glass fiber-bundle dowel system as retentive as a "rigid" quartz fiber dowel system? J Prosthodont. 2008;17(7):532-537.
35. Ferrari M, Cagidiaco M, Vichi A, et al. Post placement and residual coronal structure affect root-treated premolars' survival. J Dent Res.2007;86(spec iss A): Abstract 1385.
36. Kimmel SS. Restoration and reinforcement of endodontically treated teeth with a polyethylene ribbon and prefabricated fiberglass post. Gen Dent. 2000;48(6):700-706.
37. Mortazavi V, Fathi M, Katiraei N, et al. Fracture resistance of structurally compromised and normal endodontically treated teeth restored with different post systems: an in vitro study. Dent Res J (Isfahan).2012;9(2):185-191.
38. daCosta RG, Morais ECC, Moreira-Da-Silva SML, et al. Fatigue and fracture resistance of customized fiber dowel. J Dent Res.2011;90(spec iss A): Abstract 3103.
39. Maceri F, Martignoni M, Vairo G. Mechanical behaviour of endodontic restorations with multiple prefabricated posts: a finite-element approach. J Biomech. 2007;40(11):2386-2398.
40. Balasubramanian S, Schulze K, Roetzer P, et al. Push-out-bond-strength of fiber posts and failure analysis. J Dent Res. 2017;96(spec iss A): Abstract 2614.
41. Salvio L, Gonini A Jr, Moura SK, et al. Resin cement and glass fibre accessories posts: photoelastic analysis. J Dent Res. 2009;88(spec iss A): Abstract 1840.
42. Alkumru H, Akkayan B, Gaucher H, Atalay S. Fracture strength of teeth in oval-shaped root canals restored with posts and accessory post systems. Canadian J Restorative Dent and Prosthodontics. 2013;6(1):1-9.
43. Bonfante G, Kaizer OB, Pegoraro LF, do Valle AL. Fracture strength of teeth with flared root canals restored with glass fibre posts. Int Dent J. 2007;57(3):153-160.
44. da Silva GR, Santos-Filho PC, Simamoto-Júnior PC, et al. Effect of post type and restorative techniques on the strain and fracture resistance of flared incisor roots. Braz Dent J. 2011;22(3):230-237.
45. Martelli H Jr, Pellizzer EP, Rosa BT, et al. Fracture resistance of structurally compromised root filled bovine teeth restored with accessory glass fibre posts. Int Endod J. 2008;41(8):685-692.
46. Raposo LHA, Silva GR, Santos-Filho PCF, et al. Effect of posts and materials on flared teeth's mechanical behavior. J Dent Res. 2011;90(spec iss A): Abstract 1862.
47. Li Q, Xu B, Wang Y, Cai Y. Effects of auxiliary fiber posts on endodontically treated teeth with flared canals. Oper Dent. 2011;36(4):380-389.
48.Baldissara PV, Valandro LF, Arena A, Scotti R. Non-axial loading of crowns supported by new fiber post systems. J Dent Res.2010;89(spec iss B): Abstract 2195.
49. Porciani P, Vano M, Radovic I, et al. Fracture resistance of fiber posts: combinations of several small posts vs. standardized single post. Am J Dent. 2008;21(6):373-376.
50. Moosavi, H, Maleknejad, F, Kimyai S. Fracture resistance of endodontically-treated teeth restored using three root-reinforcement methods. J Contemp Dent Pract. 2008;(9)1:30-37.
51. Gomes GM, Gomes OM, Gomes JC, et al. Evaluation of different restorative techniques for filling flared root canals: fracture resistance and bond strength after mechanical fatigue. J Adhes Dent.2014;16(3):267-276.