Digital Workflow With a Triple Scanning Technique for Implant Rehabilitation in the Esthetic Zone
Panos Papaspyridakos, DDS, MS, PhD; Alissa Mariano, DMD; Andre De Souza, DDS, MS; Elli Kotina, DDS, MS; Yukio Kudara, CDT, MDT; and Kiho Kang, DMD, MS
Abstract
This article describes the case of a partially edentulous patient who had undergone template-guided implant placement and was treated using a triple digital scanning protocol that allowed for CAD/CAM prosthodontic rehabilitation in a complete digital workflow. At the impression appointment, the provisional implant-supported screw-retained prosthesis was digitally scanned both intraorally (first scan) and, after removal, extraorally (second scan). After the second scan, scan bodies were placed intraorally and an implant-level digital impression was taken (third scan). The three standard tessellation language (STL) files derived from the three digital scans were imported in a CAD software and superimposed into one file that contained all of the information from the implant 3D position, prosthesis contours, and transmucosal part of the peri-implant soft tissues. The superimposition of the three STL files led to one master file to serve as a blueprint for the definitive prosthesis. The definitive monolithic zirconia prosthesis was CAM copy-milled, externally stained, and inserted. The patient was satisfied with both the esthetic and functional outcome and the minimally invasive, time-efficient, two-visit restorative protocol. In summary, this case report illustrates a technique for a complete digital workflow in an implant rehabilitation for the replacement of multiple missing teeth in the esthetic zone in two visits.
Digital technology is currently gaining popularity, and its different applications in implant dentistry translate into the so-called digital workflow.1-12 Before the restorative workflow can be implemented after implants have been placed to restore multiple teeth missing in the esthetic zone, the most critical step prior to the definitive rehabilitation is the fixed implant provisionalization.13-16 The importance of the provisional prosthesis as a blueprint for the definitive rehabilitation has been shown in both conventional fixed and implant prosthodontics.13-16 The provisional prosthesis in implant prosthodontics aids in the sculpting of the emergence profile, the soft-tissue conditioning of the peri-implant tissues during healing, and the transferring of the mucosal architecture to the definitive restoration.13-15 Several impression techniques to capture the morphology of peri-implant tissues after their sculpting with the provisional prosthesis have been described, especially in relation to the maxillary esthetic zone.17-20
The introduction of digital scanning in implant dentistry has provided additional tools for the impression armamentarium.3,4,7-10 Digital impressions with intraoral scanners are becoming increasingly prevalent, and preclinical and clinical research is validating their application in clinical practice for patients with short-span partial edentulism.7-12,21-24 Typically, the digital scanning of implant scan bodies and the screw-retained interim prosthesis generates standard tessellation language (STL) files, and data superimposition and registration is needed. The presence of teeth as landmarks makes the superimposition of STL data more predictable than with fully edentulous jaws that have an absence of landmarks.8,24,25 A limitation of the digital impression pertains to the difficulty in capturing the transmucosal emergence profile, which can be challenging because the scan body is round and cannot be customized like a traditional impression coping.
This article describes in a step-by-step fashion a triple digital scanning technique to overcome the aforementioned limitation and facilitate a complete digital workflow in implant rehabilitation for replacement of multiple missing teeth in the esthetic zone, without the need to 3D-print a physical cast or make a conventional impression. The number of restorative visits can be reduced, increasing treatment effectiveness and patient satisfaction.
Case Report
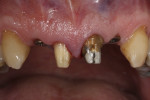
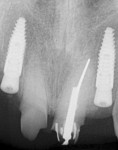
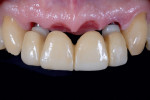
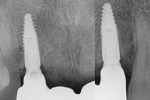
A patient with multiple missing teeth in the anterior maxilla presented to the Postgraduate Prosthodontic clinic at Tufts University School of Dental Medicine seeking prosthodontic consultation. He had received two implants (3.3 mm x 12 mm) (Straumann® Bone Level Tapered, Straumann, straumann.com) in the anterior maxilla to replace his missing lateral incisors (Figure 1). The central incisors previously had been deemed hopeless but were present as temporary abutments for a tooth-supported provisional fixed dental prosthesis (FDP). A preoperative radiograph is shown in Figure 2.
After a comprehensive diagnostic wax-up was completed, treatment options were discussed with the patient, who elected to proceed with a fixed implant rehabilitation with a four-unit implant-supported FDP after extraction of the hopeless supraerupted central incisors. Reportedly, for the replacement of the four missing maxillary incisors, implants may be placed in the sites of the central incisors to reduce the length of lever arms and number of bending moments when the arch is curved.15 However, in the present treatment the patient presented with the implants already placed in the lateral incisor positions.
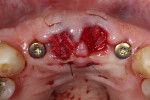
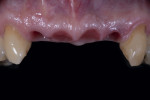
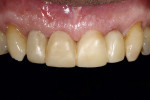
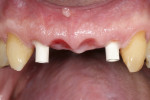
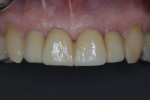
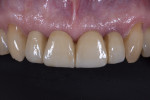
At the next visit, the central incisors were extracted and socket grafting was performed (Figure 3). After the extractions, a screw-retained four-unit implant-supported provisional prosthesis with ovate pontics on the central incisors was inserted in order to condition the soft tissues during the post-extraction healing time.16 After 3 more months of soft-tissue conditioning and maturation (Figure 4), the decision was made to move forward to the definitive prosthesis. The implant-supported provisional prosthesis was deemed adequate in terms of white and pink esthetics, function, and speech (Figure 5).
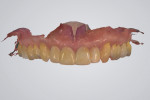
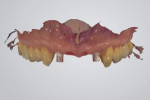
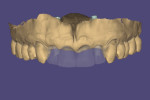
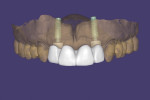
At the impression appointment, a triple digital scanning technique was implemented. The implant-supported provisional screw-retained prosthesis was digitally scanned both intraorally (first scan) and, after it was removed, extraorally (second scan) with a white light intraoral scanner (TRIOS®, 3Shape, 3shape.com) (Figure 6 and Figure 7). Subsequently, scan bodies were immediately attached to the implants and hand-tightened (Figure 8). Flowable composite (Filtek™ Z350, 3M Oral Care, 3m.com) was injected around the scan bodies and light-cured in order to maintain the contours of the peri-implant soft tissues sculpted by the provisional prosthesis. An implant-level digital impression was taken (third scan) (Figure 9). The three STL files derived from the triple digital scanning protocol were imported in CAD software (exocad® DentalCAD, exocad, exocad.com) and superimposed into one master file that contained all of the information from the implant 3D position, prosthesis contours, and transmucosal part of the peri-implant soft tissues (Figure 10 and Figure 11).
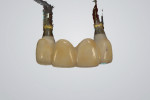
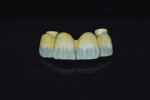
CAD software was used to design a screw-retained FDP supported by two titanium-base abutments (Narrow CrossFit® Variobase®, GH 2 mm, Straumann), and then the prosthesis was copy-milled on a CAM milling unit (Tizian Cut eco plus, Schütz Dental, schuetz-dental.de) from prefabricated monolithic zirconia blocks (Katana™ ML, Kuraray, kuraraydental.com). After the sintering and staining process, titanium-base inserts were cemented to the zirconia FDP at the laboratory (Figure 12). The internal surfaces of the zirconia FDP were silica-sandblasted, etched for 20 seconds with 4.9% hydrofluoric acid, rinsed with water for 1 minute, and air-dried with oil-free air.6 Then, a 10-methacryloyloxydecyl dihydrogen phosphate (10-MDP)-containing bonding/silane coupling agent mixture (Clearfil Ceramic Primer, Kuraray) was applied on both the zirconia FDP and the titanium-base inserts for 60 seconds before adhesive cementation was performed.6 Additionally, self-adhesive resin cement (Clearfil SA Cement, Kuraray) was used for the bonding procedure.
At the next clinical visit, the screw-retained monolithic zirconia FDP was tried in. The accuracy of fit was confirmed clinically and with periapical radiographs.6,12 Red articulating paper (AccuFilm® II, Parkell, parkell.com), shimstock foil (GMH, Hanel Medizinal), and fine diamonds under copious water irrigation were used for minor occlusal adjustment. The zirconia FDP was then inserted by torqueing the abutment screws to 35 Ncm. The screw-access holes were filled with Teflon tape and composite resin (Figure 13 through Figure 15). The patient was given oral hygiene instructions to assist him in cleaning around the prosthesis. The 6-month follow-up visit showed a stable outcome (Figure 16).
Discussion
This clinical report describes a technique for complete digital workflow in implant rehabilitation for replacement of multiple missing teeth in the esthetic zone. Use of the presented triple scanning protocol is capable of reducing chairside time and lowering the overall treatment time and cost of implant treatment. Additionally, patient satisfaction potentially may increase.
The advantage of this expedited protocol is that all of the information necessary for final prosthesis fabrication is acquired from the three scans, which leads to STL files that can be imported into CAD software, simplifying the design and fabrication of the final prosthesis. Prior to implementation of this protocol, it is incumbent that the provisional prosthesis has ideal contours and satisfies all requirements of function and esthetics. The accurate superimposition of the STL files leads to the CAD/CAM fabrication of the definitive prosthesis. If the provisional prosthesis is not ideal the clinician may desire to mill a prosthesis prototype in polymethyl methacrylate (PMMA) for try-in prior to fabrication of the definitive prosthesis. In such a clinical situation, the PMMA prosthesis prototype is tried in, adjusted accordingly if necessary, and then rescanned for the milling of the definitive prosthesis.25 If during the assessment of fit of the prosthesis prototype it is determined that misfit exists, then the prototype can be easily sectioned and reconnected intraorally with additional PMMA material to verify fit; this represents an additional checkpoint step for quality control.25
Additionally, the triple scanning technique is simple and allows for the fabrication of the prosthesis prototype or definitive prosthesis with a complete digital workflow and without any physical cast. Alternatively, a physical cast may be printed from the STL file of the digital scan, but the accuracy of 3D-printed implant casts is still being investigated.9,10,25,26
A limitation of the present technique is that it is directly dependent on the accuracy of the digital implant impression. The digital workflow relies on the accuracy of the digital scanning, which is also coupled with the accuracy of the intraoral scan. Comparative preclinical and clinical studies are currently emerging showing that partial-arch digital implant impressions display similar accuracy with conventional ones.7-12,21-24 The clinical implications suggest that a complete digital workflow for fixed implant rehabilitation with multiple-unit FDPs could be routine procedure in the near future. If desired, a verification jig can always be made to generate an index cast for the fabrication of the definitive prosthesis and to ensure the accuracy of fit.
Regarding prosthetic materials and design, in the present clinical case the definitive prosthesis was milled in monolithic zirconia with only external staining. The monolithic prosthetic design with zirconia has been reported to obtain satisfactory esthetic results for both partially and fully edentulous patients.27-32 A modified monolithic design is frequently implemented with minor facial cut-back to allow for veneering porcelain to enhance esthetics and avoid porcelain chipping from occlusal bearing surfaces, which had been reported to be the most frequent technical complication for single crowns, FDPs, and full-arch fixed prostheses.28-36 Recent advances in the fabrication of multilayered blocks enable total monolithic design without cut-back, making the use of monolithic zirconia in the esthetic zone feasible.37 Monolithic design or modified monolithic design with only facial cut-back aids in eliminating porcelain chipping, the most common complication often encountered with metal-ceramic implant FDPs.28 Adequate connector size is also important to avoid fracture of zirconia when pontics are present, as per established guidelines.26-30
The triple scanning technique is a simple, efficient, and straightforward approach that can be used for the rehabilitation of short-span implant FDPs supported with two implants. To date, the authors have successfully implemented this technique for the rehabilitation of three patients. In the authors' experience, key for mainstream and predictable implementation of this proof-of-concept, two-visit protocol may be the fabrication of a verification jig during the triple scan appointment (first visit) so that any misfit during the insertion of the definitive prosthesis (second visit) is eliminated.
Summary
This two-visit restorative protocol using the triple scanning technique as outlined enables customized CAD/CAM prosthodontic rehabilitation with a complete digital workflow. The triple scanning technique may reduce treatment time and the number of clinical visits.
ABOUT THE AUTHORS
Panos Papaspyridakos, DDS, MS, PhD
Associate Professor, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Alissa Mariano, DMD
Private Practice in Prosthodontics, Boston, Massachusetts
Andre De Souza, DDS, MS
Assistant Professor, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Elli Kotina, DDS, MS
Private Practice in Prosthodontics, Athens, Greece
Yukio Kudara, CDT, MDT
Assistant Professor, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Kiho Kang, DMD, MS
Professor, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
REFERENCES
1. Chochlidakis KM, Papaspyridakos P, Geminiani A, et al. Digital versus conventional impressions for fixed prosthodontics: a systematic review and meta-analysis. JProsthet Dent. 2016;116(2):184-190.
2. Joda T, Ferrari M, Gallucci GO, et al. Digital technology in fixed implant prosthodontics. Periodontol 2000. 2017;73(1):178-192.
3. Joda T, Bragger U, Zitzmann NU. CAD/CAM implant crowns in a digital workflow: five-year follow-up of a prospective clinical trial. Clin Implant Dent Relat Res. 2019;21(1):169-174.
4. Joda T, Bragger U. Time-efficiency analysis of the treatment with monolithic implant crowns in a digital workflow: a randomized controlled trial. Clin Oral Implants Res. 2016;27(11):1401-1406.
5. Wöhrle PS. Predictably replacing maxillary incisors with implants using 3-D planning and guided implant surgery. Compend Contin Educ Dent. 2014;35(10):758-768.
6. Papaspyridakos P, Chochlidakis K, Kang K, et al. Digital workflow for implant rehabilitation with double full-arch monolithic zirconia prostheses. J Prosthodont. 2020;29(6):460-465.
7. Basaki K, Alkumru H, De Souza G, Finer Y. Accuracy of digital vs conventional implant impression approach: a three-dimensional comparative in vitro analysis. Int J Oral Maxillofac Implants. 2017;32(4):792-799.
8. Monaco C, Evangelisti E, Scotti R, et al. A fully digital approach to replicate peri-implant soft tissue contours and emergence profile in the esthetic zone. Clin Oral Implants Res. 2016;27(12):1511-1514.
9. Marghalani A, Weber HP, Finkelman M, et al. Digital versus conventional implant impressions for partially edentulous arches: an evaluation of accuracy. J Prosthet Dent. 2018;119(4):574-579.
10. Alshawaf B, Weber HP, Finkelman M, et al. Accuracy of printed casts generated from digital implant impressions versus stone casts from conventional implant impressions: a comparative in vitro study. Clin Oral Implants Res. 2018;29(8):835-842.
11. Jiang X, Lin Y, Cui HY, Di P. Immediate loading of multiple splinted implants via complete digital workflow: a pilot clinical study with 1-year follow-up. Clin Implant Dent Relat Res. 2019;21(3):446-453.
12. Sailer I, Mühlemann S, Fehmer V, et al. Randomized controlled clinical trial of digital and conventional workflows for the fabrication of zirconia-ceramic fixed partial dentures. Part I: Time efficiency of complete-arch digital scans versus conventional impressions. J Prosthet Dent. 2019;121(1):69-75.
13. Wittneben JG, Buser D, Belser UC, Brägger U. Peri-implant soft tissue conditioning with provisional restorations in the esthetic zone: the dynamic compression technique. Int J Periodontics Restorative Dent. 2013;33(4):447-455.
14. Martin WC, Pollini A, Morton D. The influence of restorative procedures on esthetic outcomes in implant dentistry: a systematic review. Int J Oral Maxillofac Implants. 2014;29(suppl):142-154.
15. Papaspyridakos P, Tarnow DP, Eckert SE, Weber HP. Replacing six missing adjacent teeth in the anterior maxilla with implant prostheses: a case series. Compend Contin Educ Dent. 2018;39(6):e1-e4.
16. Kim TH, Cascione D, Knezevic A. Simulated tissue using a unique pontic design: a clinical report. J Prosthet Dent. 2009;102(4):205-210.
17. Lops D, Bressan E, Cea N, et al. Reproducibility of buccal gingival profile using a custom pick-up impression technique: a 2-year prospective multicenter study. J Esthet Restor Dent. 2016;28(1):43-55.
18. Schoenbaum TR, Swift EJ Jr. Abutment emergence contours for single-unit implants. J Esthet Restor Dent. 2015;27(1):1-3.
19. Elian N, Tabourian G, Jalbout ZN, et al. Accurate transfer of peri-implant soft tissue emergence profile from the provisional crown to the final prosthesis using an emergence profile cast. J Esthet Restor Dent. 2007;19(6):306-314.
20. Tsai BY. Use of provisional restorations as implant impression copings. J Prosthet Dent. 2007;97(6):395-396.
21. Alsharbaty MHM, Alikhasi M, Zarrati S, Shamshiri AR. A clinical comparative study of 3-dimensional accuracy between digital and conventional implant impression techniques. J Prosthodont. 2019;28(4):e902-e908.
22. Chia VA, Esguerra RJ, Teoh KH, et al. In vitro three-dimensional accuracy of digital implant impressions: the effect of implant angulation. Int J Oral Maxillofac Implants. 2017;32(2):313-321.
23. Bohner L, Hanisch M, De Luca Canto G, et al. Accuracy of casts fabricated by digital and conventional implant impressions. J Oral Implantol. 2019;45(2):94-99.
24. Chew AA, Esguerra RJ, Teoh KH, et al. Three-dimensional accuracy of digital implant impressions: effects of different scanners and implant level. Int J Oral Maxillofac Implants. 2017;32(1):70-80.
25. Papaspyridakos P, Chen YW, Gonzalez-Gusmao I, Att W. Complete digital workflow in prosthesis prototype fabrication for complete-arch implant rehabilitation: a technique. J Prosthet Dent. 2019;122(3):189-192.
26. Renne WG, Evans ZP, Mennito A, Ludlow M. A novel technique for reference point generation to aid in intraoral scan alignment. J Esthet Restor Dent. 2017;29(6):391-395.
27. Cheng CW, Chien CH, Chen CJ, Papaspyridakos P. Clinical results and technical complications of posterior implant-supported modified monolithic zirconia single crowns and short-span fixed dental prostheses: a 2-year pilot study. J Prosthodont. 2018;27(2):108-114.
28. Sailer I, Strasding M, Valente NA, et al. A systematic review of the survival and complication rates of zirconia-ceramic and metal-ceramic multiple-unit fixed dental prostheses. Clin Oral Implants Res. 2018;29(suppl 16):184-198.
29. Spies BC, Witkowski S, Vach K, Kohal RJ. Clinical and patient-reported outcomes of zirconia-based implant fixed dental prostheses: results of a prospective case series 5 years after implant placement. Clin Oral Implants Res. 2018;29(1):91-99.
30. Cheng CW, Chien CH, Chen CJ, Papaspyridakos P. Randomized controlled clinical trial to compare posterior implant-supported modified monolithic zirconia and metal-ceramic single crowns: one-year results. J Prosthodont. 2019;28(1):15-21.
31. Tischler M, Patch C, Bidra AS. Rehabilitation of edentulous jaws with zirconia complete-arch fixed implant-supported prostheses: an up to 4-year retrospective clinical study. J Prosthet Dent. 2018;120(2):204-209.
32. Moscovitch M. Consecutive case series of monolithic and minimally veneered zirconia restorations on teeth and implants: up to 68 months. Int J Periodontics Restorative Dent. 2015;35(3):315-323.
33. Pjetursson BE, Valente NA, Strasding M, et al. A systematic review of the survival and complication rates of zirconia-ceramic and metal-ceramic single crowns. Clin Oral Implants Res. 2018;29(suppl 16):199-214.
34. Papaspyridakos P, Bordin TB, Natto ZS, et al. Complications and survival rates of 55 metal-ceramic implant-supported fixed complete-arch prostheses: a cohort study with mean 5-year follow-up. J Prosthet Dent. 2019;122(5):441-449.
35. Papaspyridakos P, Barizan Bordin T, Kim YJ, et al. Implant survival rates and biologic complications with implant-supported fixed complete dental prostheses: a retrospective study with up to 12-year follow-up. Clin Oral Implants Res. 2018;29(8):881-893.
36. Heitz-Mayfield LJ, Needleman I, Salvi GE, Pjetursson BE. Consensus statements and clinical recommendations for prevention and management of biologic and technical implant complications. Int J Oral Maxillofac Implants. 2014;29(suppl):346-350.
37. Yu NK, Park MG. Effect of different coloring liquids on the flexural strength of multilayered zirconia. J Adv Prosthodont. 2019;11(4):209-214.