Lateral Access Pouch Technique to Treat Implants With Gingival Recession
Douglas H. Mahn, DDS
Abstract
Connective tissue grafting is a means of developing stable and natural-looking soft-tissue architecture. The use of a subepithelial connective tissue graft (SCTG) has been successful in achieving root coverage and augmenting tissue thickness. Tunnel techniques enable root coverage with results that appear natural. These techniques can be applied to the treatment of dental implants with gingival recession. The purpose of this article is to demonstrate the use of a SCTG and a lateral access pouch in the treatment of multiple gingival recession defects affecting adjacent implants.
The aim of connective tissue grafting is to develop stable and natural-appearing soft-tissue architecture. Use of a subepithelial connective tissue graft (SCTG) in conjunction with a coronally advanced flap has been shown to be a highly successful method in gaining root coverage and augmenting tissue thickness.1,2 The SCTG is considered a therapeutic mainstay of soft-tissue grafting.3
The interdental papillae can be a delicate structure that is difficult to reconstruct once lost. A lateral pouch technique to correct an edentulous facial ridge deformity while protecting crestal tissues has been reported.4 Mucogingival tunnel techniques have been developed that protect the interdental papillae when performing soft-tissue grafting.5 The modified tunnel6,7 and vestibular incision subperiosteal tunnel access (VISTA)8 techniques permit placement of graft material using a lateral approach. A lateral access approach also offers the benefit of simplifying placement of larger grafts into the mucogingival tunnel.9
Connective tissue grafting over exposed implant surfaces and implant abutments follows similar principles as grafting over exposed root surfaces. Coverage of the rough implant surfaces has been deemed important in the reduction of biofilm accumulation.10 The lack of keratinized mucosa has also been associated with increased plaque accumulation, tissue inflammation, mucosal recession, and attachment loss.11,12 The use of a SCTG in the treatment of an implant with gingival recession and peri-implantitis was reported by the author.13
The purpose of this article is to demonstrate the use of a SCTG and a lateral access pouch in the treatment of multiple gingival recession defects affecting adjacent implants.
Case Report
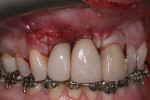
A 43-year-old woman, a non-smoker, was referred by her orthodontist for evaluation and treatment of gingival recession affecting dental implants in sites Nos. 7 and 8. The patient reported that teeth Nos. 7 and 8 were lost as a result of trauma approximately 5 years earlier. At that time, the teeth were removed and immediate implants were placed. The patient believed bone grafts were used. She reported that the crowns on the implants always looked longer than teeth Nos. 9 and 10 and that gingival recession exposing the implant surfaces occurred within a year of implant restoration. The patient tolerated the appearance of the implant restorations because her lip posture covered the gingival half of her teeth when she smiled. The patient advised that she wanted to keep the implants but did not want to endure multiple surgeries to correct the problem. She was concerned with both discomfort and finances.
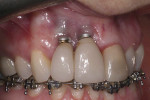
The implants in sites Nos. 7 and 8 were found to have facial gingival recession (Figure 1). The abutment, implant collar, and roughened threaded surfaces were exposed. The implant surfaces were found to have plaque accumulations, but minimal inflammation. The facial gingival margin was about 2 mm apical from the prosthetic table, and approximately 25% of the circumference of the implant body was exposed at the level of the prosthetic table. There was no facial attached keratinized gingiva. The dark color of the implant body was visible through the mucogingival tissues. The straight facial probing depth was 2 mm, and bleeding was not present on probing. No implant mobility was present.
After discussing the findings, treatment options, benefits, and risks with the patient, she agreed to treatment of the implants with connective tissue grafting.
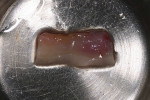
Profound local anesthesia, using 2% lidocaine with 1:100,000 epinephrine, was achieved in the right palatal donor site and in the area of implant sites Nos. 7 and 8. A SCTG, approximately 20 mm x 8 mm x 2 mm, was harvested from the palate (Figure 2). A continuous 4.0 plain gut suture was used to secure the palatal donor site.
Careful mechanical decontamination of the implant surface was performed with titanium curettes. The surgical site was then profusely irrigated with 3% hydrogen peroxide for 60 seconds followed by a thorough sterile saline rinse.
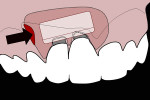
A lateral pouch surgical design that would protect the interdental papillae was chosen (Figure 3). Following the surgical design, a vertical incision was made using a #15 scalpel blade (Bard-Parker #15 scalpel blade, Patterson Dental, pattersondental.com) distal to implant site No. 7 (Figure 4). From this incision line, the pouch was elevated using an Orban knife and periotomes. Care was taken not to tear or detach the interdental papillae. The boundaries of the pouch closely followed those shown in Figure 3. The mucogingival pouch extended horizontally to the distal of implant site No. 9. Vertically, the pouch extended from beneath the vestibule toward the interdental papillae and gingival margins. Passive repositioning of the mucogingival tissues over the implant abutments was verified. Using a titanium curette, it was determined that four subgingival implant threads were supracrestal on the facial aspect of both implants.
The SCTG was placed into the pouch and positioned over the implant sites. The epithelial surface of the SCTG was positioned toward the buccal and coronal aspects. The coronal positioning of the SCTG was verified by using the tip of the suture needle. The SCTG and mucogingival tissues were secured over the implant bodies and abutments using a single continuous 4.0 chromic gut suture. One interrupted 4.0 chromic gut suture was used to close the vertical incision (Figure 5).
The patient was prescribed 500 mg of amoxicillin to be taken every 8 hours for 10 days and 600 mg of ibuprofen for discomfort. She was instructed not to brush the surgical site for 7 days, but to rinse the area with 0.12% chlorhexidine gluconate (Peridex™, Proctor & Gamble, us.pg.com) then expectorate, twice a day. After 7 days, the patient was instructed to discontinue the rinse and to begin to gently brush the implant site in a coronal direction only. After 6 weeks, she was instructed in the modified Bass technique and encouraged to perform excellent oral hygiene.
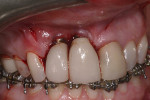
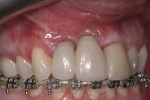
The patient was seen for re-evaluations at 1 week, 6 weeks, and 6 months after surgery. At the 6-month evaluation, the surgical site was found to have healed well with no signs of inflammation (Figure 6). The oral hygiene of the patient was improved. There was complete coverage of the implants and the implant abutments. The facial keratinized tissue width was improved, the mucogingival tissues appeared thicker, and the dark implant bodies were no longer visible. The volume of the interdental papillae appeared unchanged and filled the embrasure spaces between sites Nos. 6 through 9. The straight facial probing depths were 2 mm and were found to be without bleeding or suppuration.
Discussion
Given the reported treatment history of the patient and the appearance of the sites before treatment, the primary etiology of the peri-implant gingival recession may have been inadequate implant site management. It is known that failure to develop adequate bone volume and poor implant placement can lead to gingival recession.14 In addition, the overcontoured restoration also could have played a part.14 An ideal result may have been achieved by performing soft-tissue grafting on the sites without the restorations in place.15 New restorations with a proper emergence profile would then have been placed after the grafted sites healed. The patient refused this treatment because of her concerns of experiencing discomfort, the need for multiple surgeries, the amount of time necessary to complete the treatment, and the cost of the treatment.
Implant surface decontamination was performed mechanically using titanium curettes, followed by 3% hydrogen peroxide and sterile saline rinses. This protocol has been reported as being successful in the treatment of peri-implantitis sites.16
Treatment of peri-implant gingival recession may be an important step in preventing peri-implant diseases. The formation of a biofilm plays a significant role in the initiation and progression of peri-implant diseases,10 and a low rate of biofilm accumulation and tight peri-implant mucosal attachment are necessary for healthy peri-implant mucosa.17 The use of a SCTG can help correct an implant with gingival recession and increase the zone of keratinized gingiva.13,18 For this patient, complete implant coverage was achieved and almost no residual abutment was left exposed. Moreover, the mucogingival tissues appeared thicker and healthy.
A lateral pouch using a vertical incision in the mucogingival tissues for the correction of an edentulous facial ridge deformity was described more than 30 years ago.4 Later, the modified tunnel, which uses vertical incisions on both sides of the mucogingival tunnel,6,7 was delineated for the treatment of gingival recession affecting root surfaces. After this, the VISTA8 technique, which also uses a vertical incision for placement of a graft within a mucogingival tunnel, was reported. These techniques are intended to spare the interdental papillae from trauma and minimize tissue shrinkage. For this patient, the use of a lateral access may have been responsible for the preservation of the interdental papillae.
Conclusion
The use of a SCTG and a lateral pouch technique can be successful in the treatment of multiple gingival recession defects affecting adjacent dental structures and preserving their interdental papillae. More clinical cases demonstrating this technique are needed to provide further evidence of its success.
About the Author
Douglas H. Mahn, DDS
Private Practice
Manassas, Virginia
References
1. Langer B, Langer L. The subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
2. Cairo F, Pagliaro U, Nieri M. Treatment of gingival recession with coronally advanced flap procedures: A systematic review. J Clin Periodontol. 2008;35(8 suppl):136-162.
3. Chambrone L, Chambrone D, Pustiglioni FE, et al. Can subepithelial connective tissue grafts be considered the gold standard procedure in the treatment of Miller Class I and II recession-type defects? J Dent. 2008;36(9):659-671.
4. Garber DA, Rosenbert ES. The edentulous ridge in fixed prosthodontics. Compend Contin Educ Dent. 1981;2(4):212-223.
5. Allen AL. Use of a supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodontics Restorative Dent. 1994;14(3):216-227.
6. Mahn DH. Treatment of gingival recession with a modified “tunnel” technique and an acellular dermal connective tissue allograft. Pract Proced Aesthet Dent. 2001;13(1):69-74.
7. Mahn DH. Esthetic correction of gingival recession using a modified tunnel technique and an acellular dermal connective tissue allograft. J Esth Rest Dent. 2002;14(1):18-22.
8. Zadeh H. Minimally invasive treatment of maxillary anterior gingival recession defects by vestibular incision subperiosteal tunnel access and platelet-derived growth factor BB. Int J Periodontics Restorative Dent. 2011;31(6):653-660.
9. Mahn DH. Use of double-layer of acellular dermal matrix and modified tunnel technique to treat multiple adjacent gingival recession defects. Compend Contin Educ Dent. 2016;37(8):e9-e12.
10. Elter C, Heuer W, Demling A, et al. Supra- and subgingival biofilm formation on implant abutments with different surface characteristics. Int J Oral Maxillofac Implants. 2008;23(2);327-334.
11. Adibrad M, Shahabuei M, Sahabi M. Significance of the width of keratinized mucosa on the health status of the supporting tissue around implants supporting overdentures. J Oral Implantol. 2009;35(5):232-237.
12. Lin GH, Chan HL, Wang HL. The significance of keratinized mucosa on implant health: a systematic review. J Periodontol. 2013;84(12):1755-1767.
13. Mahn DH. Use of an autogenous connective tissue graft to treat peri-implantitis with gingival recession affecting an implant supporting an overdenture. Clin Adv Periodontics. 2016;6(4):161-165.
14. Chu SJ, Tarnow DP. Managing esthetic challenges with anterior implants. Part 1: midfacial recession defects from etiology to resolution. Compend Contin Educ Dent. 2013;34(spec iss 7):26-31.
15. Tarnow DP, Chu SJ, Fletcher PD. Clinical decisions: determining when to save or remove an ailing implant. Compend Contin Educ Dent. 2016;37(4):233-244.
16. Roos-Jansåker AM, Renvert H, Lindahl C, Renvert S. Surgical treatment of peri-implantitis using a bone substitute with or without a resorbable membrane: a prospective cohort study. J Clin Periodontol. 2007;34(7):625-632.
17. Berglundh T, Lindhe J, Ericsson I, et al. The soft tissue barrier at implants and teeth. Clin Oral Implants Res. 1991;2(2):81-90.
18. Froum SJ, Froum SH, Rosen PS. Successful management of peri-implantitis with a regenerative approach: a consecutive series of 51 treated patients with 3- to 7.5-year follow-up. Int J Periodontics Restorative Dent. 2012;32(1):11-20.