Bonded Functional Esthetic Prototype: An Alternative Pre-Treatment Mock-Up Technique and Cost-Effective Medium-Term Esthetic Solution
Abstract:
As the economy has receded in recent years, many patients have been inclined to reject dental treatment beyond what they feel is the minimal amount necessary. Increasingly, there has been reluctance to take on the expense of full-mouth restorations and time-consuming procedures. Consequently, clinicians can benefit from innovative, conservative, interim solutions that enable them to provide segment treatment with long-term stability and esthetics, with lower initial cost. The bonded functional esthetic prototype (BFEP) allows fabrication of up to 14 teeth from composite in 1 hour, providing either a pre-treatment restoration or a long-term provisional solution until further treatment can be completed. As demonstrated herein, the BFEP enables superb function, stability, and esthetics in the interim while dispersing the cost of definitive treatment over time.
The recent global economic environment has caused a paradigm shift in patient receptiveness and acceptance of dental treatments.1,2 Consequently, a growing number of patients concerned about their smile are seeking esthetic correction of only maxillary incisors. Many times, however, these patients require full-mouth rehabilitation to meet their ultimate treatment goals.1,2
Reluctant to incur the expense of full-mouth restorations and concerned with time-consuming procedures, patients are increasingly declining treatment beyond what they feel they can comfortably afford or budget. Therefore, a conservative, interim, cost-effective solution has been needed that will enable dentists to segment treatment with long-term stability and esthetics, yet with lower initial cost. Additionally, materials and techniques have been needed to improve the durability of what have been termed “pre-treatment mock-ups.”
Although patients are more knowledgeable about dental treatments and procedures than in the past, many terms used by dental professionals fail to fully inform them of what the dentist is trying to accomplish.3 For example, when told a temporary or provisional is placed, or the term “mock-up restoration” is used, the patient may believe it will only last for a very short time, which in many cases is true. What the patient fails to realize—and what the dentist must convey—is that a temporary or pre-treatment mock-up restoration, when created using the appropriate material and technique, may function for an extended period of time.4 Dentists should, therefore, use treatment terminology that patients can more readily comprehend such as bonding, function, esthetics, and prototypes, rather than “temporaries” or “pre-treatment mock-ups.”
The Bonded Functional Esthetic Prototype
Addressing the aforementioned issues associated with treatment acceptance, the bonded functional esthetic prototype (BFEP) was created to allow fabrication of 14 teeth from composite in 1 hour and to provide either a pre-treatment restoration (formerly called a mock-up) or a long-term provisional solution until further treatment can be completed. Based on a technique first conceptualized and utilized by K. William “Buddy” Mopper, DDS, the BFEP was developed to provide coverage to prepared dentition while indirect veneers were being fabricated.5 The early freehand technique used to create his prototypes required further simplification in order to reduce chairtime and overall cost to the patient.
Initially, the technique utilized a clear vinyl polysiloxane (VPS) matrix material (eg, RSVP®, Cosmedent, Inc., www.cosmedent.com) to create a temporary that the patient could wear intraorally.5 Providing full coverage to the prepared teeth, the key to this technique was to leave a small area exposed near the gingiva to prevent excessive trimming after placement.5 The material was first placed into the clear VPS matrix onto the prepared tooth surfaces, then cut off at the gingival one-third.5 Then, the last 1 mm to 2 mm of flowable material was placed using a freehand technique.
Another method that employed a technique-sensitive freehand approach to create pre-treatment mock-ups or post-preparation temporaries, although innovative, was time-consuming.7 The technique required significant chairtime (between 4 to 5 hours) and was costly to patients.
With the advent of new materials and placement techniques, and based on the use of a composite mock-up, the BFEP has evolved into a conservative, cost-effective, and long-term temporary restorative solution that can be used pre-treatment or post-preparation. Historically, dental mock-ups or prototypes have allowed patients to preview their anticipated indirect restorative case.6 Although useful for this purpose, prototypes were not considered ideal temporary treatment options because they could not be bonded to teeth.6 The true potential of provisional restorations now has been realized with advancements in material sciences that enable the creation of highly esthetic and long-lasting prototypes that can be adhesively bonded to tooth surfaces.4,6
Ultimately, it was determined that the best solution to simplify the temporary process was to use a stock plastic impression tray and matrix for direct composite placement.8 Unfortunately, stock plastic trays didn’t fit well in the mouth, tended to expand, and, consequently, adapted poorly to tooth surfaces. Therefore, the use of a hard, clear VPS material in a hard carrier tray that would not expand and, therefore, would adapt well to the teeth was incorporated into the technique.8 However, even this approach remained in its infancy because although proven composite materials were available, they had yet to fully evolve for this indication, primarily due to their high viscosity.
Material Considerations for BFEPs
Although the author’s proposed BFEP technique is simple, much of its success is directly related to treatment considerations and proper material selection. To provide patients with the best results, dentists must consider the different clinical and functional treatment aspects that will ultimately affect the outcome and longevity of provisionalization. These considerations should include the length of time the prototype will be in service, etching pattern used, amount of coverage needed, and how compliant the patient will be with treatment and hygiene protocol.
Bonding Agents
When placing a BFEP, a 4th- or 5th-generation bonding agent is recommended. Fifth-generation materials are formulated with a premixed primer adhesive and are much less technique-sensitive than previous versions of bonding agents.9 Important to note, self-adhesive resin cements should be avoided when placing the BFEP, because they are all-in-one adhesive agents and don’t bond as well as when a separate primer adhesive step is done.10,11 Self-adhesive cements are essentially an etchant, primer, adhesive, and cement all combined into one material, which, research has shown, does not adhere well to enamel.9,10 Some self-etch, self-adhesive resin cement systems, which allow for separate application of primer and adhesive, do provide a stable and long-term bond to dentin.9,10 However, their efficacy on uncut enamel remains suspect.10,11
Bis-acryl
Widely studied and proven, bis-acryl materials are commonly used for provisional restorations.12,13 Demonstrating minimal shrinkage, simple characterization, and excellent polishability, bis-acryl has remained popular for temporary restorations.12,13 However, in cases requiring full-mouth provisional restorations, bis-acryl can be challenging to work with because the material is inherently brittle and tends to demonstrate excessive wear.13 Further, bis-acryl materials are notoriously difficult to add to or reline when adjustments are needed, and typically are more expensive than other materials, such as composites.13
Although bis-acryl is not the ideal material in all BFEP cases, some indications will benefit from the use of it versus composite.13 For example, when a BFEP will only be in place for 8 to 12 weeks, bis-acryl is recommended because it is very flowable and will provide the longevity needed.12,13 However, when function beyond 8 to 12 weeks is required, composite should be used because it is more durable.13
Composites
With advances in material sciences, composites have evolved to demonstrate improved wear resistance, higher strength, long-term stability intraorally, and better adhesion to dental substrates when placed as definitive restorations.14-16 Among their many favorable characteristics, composites have proven an ideal material for long-term provisionalization.14,15 Most notably, composites allow dentists the flexibility and ability to trial a case, provide stability, and change or alter the vertical dimension of occlusion using prototypes as splints.14,15 When larger and more comprehensive full-mouth and implant cases are completed, the need for long-term stability is critical.17
When the BFEP technique was developed, only traditional composite materials were available, which contributed to technique sensitivity and significant chairtime. Although the materials worked well intraorally and demonstrated excellent shade characteristics, their viscosity made them difficult to place in a matrix and adapt to teeth. Additionally, the viscosity of conventional composite materials made it difficult to add material to the tray. For example, in a typical case presenting an 8 mm central incisor that needed to be 10 mm, conventional composite would be applied on the internal surface of the tray and placed over the tooth. However, the viscosity of composite made the tray difficult to seat completely, and upon tray removal there was often excess composite, causing the teeth to be longer than the desired 10 mm. This defeated the purpose of the BFEP technique, requiring the dentist to then have to spend additional time grinding, adjusting, and polishing the composite and tooth. Thus, a new composite was needed that would offer the physical and wear characteristics of a microhybrid but in a flowable viscosity.
In general, flowable materials are not highly filled, which allows them to flex, move, and be placed into deep preparations.18 Lower filled and more flexible materials have poorer physical properties, eg, wear characteristics and strength. Therefore, conventional flowables would not work well in functional areas.
The BFEP requires a different type of composite material to ensure proper adaptation to tooth surfaces when utilizing a tray. To address the limitations of conventional composites when placed using the BFEP technique, a new highly filled flowable composite (Reveal™, BISCO, Inc., www.bisco.com) was developed to enable simplified tray use and bonding. A highly filled, flowable composite would ideally demonstrate wear characteristics, flexural strength, durability, and polishability similar to those of microhybrid composites. Overall, Reveal has been developed to meet the needs of the BFEP while also simplifying the bonding technique for other indications. Additionally, this material provides esthetics, function, and durability in a BFEP for at least 2 to 5 years while the patient is undergoing segmented treatment.
BFEP Technique
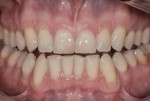
Although simpler than provisional treatments of the past, the BFEP remains a technique-sensitive protocol and is, ideally, 100% additive (ie, the teeth are built up or added to for correcting esthetic issues like excessive wear or discoloration) (Figure 1). However, there are instances when slight reduction is necessary. For example, if a tooth is slightly labial, it should be placed in a more lingual position prior to BFEP placement by orthodontic movement or slight tooth preparation. Although the author prefers to avoid instant orthodontics with a bur, many times it is necessary to complete a small amount of enameloplasty at the line angle, without crossing the dento-enamel junction, to reshape the tooth. But if excessive reduction is required, this should be avoided in favor of orthodontics.
Consultation and Comprehensive Examination—Initially, the patient and dentist should discuss the patient’s needs, desires, timeframe, and budget before agreeing to treatment. Then, the patient should undergo a comprehensive examination to ensure there are no other concerns, such as untreated active caries, prior to placement of the BFEP, because any existing issues will be more difficult to address with composite in place.
Occasionally in cases requiring a BFEP, patients may present with some muscle issues. A short-term splint can be used initially to determine whether the patient can tolerate the BFEP for an extended time. After completing the muscle trial, the patient can also be given a non-bonded esthetic trial or mock-up using bis-acryl to ensure that the BFEP will meet his or her demands. If the patient has accepted the muscle and esthetic trials, the dentist can proceed to the BFEP using the composite technique.
Prior Restorations—The BFEP may be completed when prior amalgam, ceramic, or composite restorations exist. However, these should be evaluated to ensure they are biologically stable and viable. If they are, the BFEP can be placed directly over the restorations and treatment may proceed. Any defective restoration should be replaced with a conventional composite technique. When placing the BFEP over an existing metal-based restoration, sandblasting the restoration and applying a metal primer is suggested. Adhesive should then be placed on the primed metal and cured.
In the case of porcelain, if the restoration is intact, the protocol is similar to bonding to chipped porcelain. First, lightly sandblast the porcelain to break the glaze; then use a 9.5% concentration hydrofluoric acid intraorally for 90 seconds to etch the surface. After etching, place silane on the porcelain, followed by adhesive, and cure.19 Finally, the BFEP composite is placed over it, cured, and finished.
Diagnostics—Besides correcting or repairing previous restorative work, diagnostic information should be collected prior to designing and treating the case. An occlusal analysis should be performed initially using a semi-adjustable articulator, which is recommended because it facilitates adjustments to the plane of occlusion and vertical dimension of occlusion. A facebow record should be taken and transferred, along with jaw registration mounting, especially if the patient’s vertical dimension must be altered.
Impressions—Detailed impressions are made and, crucial to the success of the BFEP, should demonstrate ideal interproximal and gingival margin detail, without voids or air bubbles. When an impression is free of defects and highly detailed, the matrix will fit the teeth tightly and the composite will adapt well to the tooth surfaces. If a proper impression is taken and the matrix fits well, the BFEP will only need minimal finishing after placement. Then, prior to creating the 2-dimensional (2-D) smile design, stone casts are created from the preoperative impressions and a caliper used to measure the height of the maxillary central incisors (Figure 2).
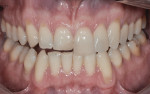
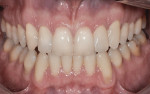
Smile Design—The concept and use of digital smile design has become common practice in many dental offices and can be completed without using challenging or expensive equipment. Instead, the author prefers to begin with a cost-effective, user-friendly 2-D digital editing software (Photoshop® CS5, Adobe, www.adobe.com), in a technique called Photoshop® Smile Design (PSD). Various photographic editing tools provided with the software (eg, Clone, Liquefy, Dodge, Grids) enable the operator to move and graft sections of tooth structure, close spaces, adjust the smile line, and bleach the teeth within the image (Figure 3 and Figure 4). Important to note, it must be made clear to patients that although the altered photographic image enables them to preview how treatment may appear, it does not represent the definitive treatment results.
Design Wax-Up—After completing the 2-D smile design and obtaining patient approval of the treatment plan, the case is created in a 3-dimensional (3-D) design wax-up (Figure 5). Although commonly referred to as a diagnostic wax-up, the term “diagnostic” does not truly apply to wax because nothing is being diagnosed, but simply designed. Therefore, the author refers to the wax-up as the “design wax-up” or “treatment plan wax-up,” which may help patients better understand its actual purpose.
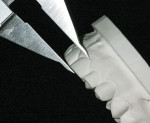
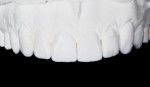
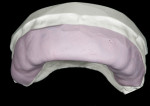
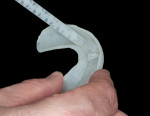
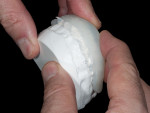
Carrier Tray Fabrication—The design wax-up serves as a foundation for fabricating a custom hard tray by placing a 2-mm thick spacer of laboratory putty (COE, GC America Inc., www.gcamerica.com) on the design model and utilizing a colorless and translucent urethane dimethacrylate-based material (Triad® TranSheet® Colorless, DENTSPLY International, prosthetics.dentsply.com) (Figure 6 and Figure 7). The custom tray is then cured in a specialized light-curing unit (Triad®, DENTSPLY International) with a tungsten halogen light source (Figure 8).
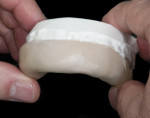
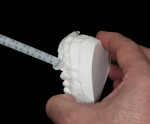
Matrix Fabrication—Then, the matrix used for BFEP fabrication is made by first spraying the design model with a thin layer of silicone as a separator. A clear VPS material is placed into the tray and onto the design model (Figure 9 and Figure 10). With the tray seated securely on the design model, excess VPS material is trimmed (Figure 11). When the matrix is complete, it should provide great detail and allow the composite to adapt well to the teeth. Important to note, when the patient returns to the office for placement of the BFEP, the matrix should be tried-in to ensure a proper fit (Figure 12). To save time, the dentist may have the trays, wax-up, and matrix made by the laboratory.
Preparation—Unlike other esthetic restorative techniques, utilizing the BFEP requires very little (ie, nearly an immeasurable amount of tooth structure lost) to no tooth preparation. Although the enamel of the teeth receiving treatment must be etched, the procedure is almost reversible. Many are hesitant to call a treatment reversible, because even with the BFEP, enamel is still lost during the etching process and, if removed, slight amounts of tooth structure will inevitably be lost. However, this treatment is the closest to reversible as any other prior treatment.
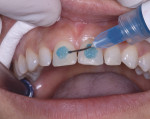
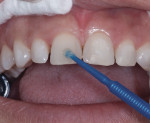
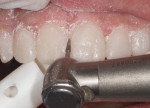
Etching Pattern—Once a definitive BFEP material (ie, composite or bis-acryl) has been selected based on the aforementioned requirements, an etching pattern is then selected that will achieve the best temporary bond. Like BFEP material selection, selecting the etch pattern is based on the length of time the BFEP is expected to function. In cases for which the prototype will remain in use for only a few weeks—to a maximum of 8 weeks—only 3 mm of spot-etching (Scotchbond™, 3M ESPE, www.3MESPE.com) should be completed on the facial surface of the teeth (Figure 13). When spot-etching this type of case, it is important to prevent etching near the interproximal margins and incisal edges. Eliminating the need to remove excess composite materials on these areas simplifies finishing and polishing.
When the BFEP will be functioning longer (eg, 8 weeks to 6 months), a larger etch pattern is required to prevent chipping, breaking, leaking, and dislodging, because more stress will be placed on the bonded surfaces.20,21 The full-facial etch pattern just short of the gingival margins and proximal contacts18,19 is the most commonly used. It is critical to remain short of the gingival margins, because when the very thin composite finish line is placed it will be very difficult to see, even under magnification. As a result, when the BFEP is removed during normal preparation for veneer placement, removing the composite in these regions will be easier. Also, if the composite is not removed during preparation it might come off during classic temporary removal at the cement appointment, leaving a void at the margins, affecting the fit of the final.
Further, depending on the coverage necessary, the incisal edge may require etching also on the lingual.20,21 For example, when only lengthening by 1 mm, often a small slot is placed on the incisal edge to help prevent BFEP fracture during function. When restoring the lingual, the same protocol is followed (ie, 2 mm to 3 mm spot-etch and avoid the margins).
Occasionally, a full-etch pattern is done on every area of the tooth to receive composite. Cases that will be in the mouth for longer than 6 months for any reason should be fully etched and bonded to prevent microleakage and recurrent caries. This technique will make it more difficult to finish and ultimately remove composite at the preparation appointment.
Bonding Pattern Selection—Patient compliance with home care instructions and length of function of the BFEP are considerations when selecting an appropriate bonding pattern for applying the recommended 5th-generation bonding agent. The bonding agent (All-Bond, BISCO, Inc.) is first placed on the etched tooth and cured separately from the composite (Figure 14). Then, the composite may be placed in the matrix and over the prepared teeth.
When the dentist is concerned with patient compliance and maintaining appointments, the 5th-generation bonding agent is placed on all tooth surfaces receiving BFEP treatment, even areas that were not etched. This bonding pattern provides some sealing and enhances retention, even when the teeth have only undergone a 3-mm to 4-mm etch.20,21 In the author’s experience, an acceptable short-term bond is still achievable in areas that have not been etched.
However, if the dentist is convinced that the patient will follow his or her treatment and appointment schedule, the bonding agent may be restricted to only etched tooth surfaces. This ensures easy and swift removal of the prototype when the final restorations are placed.
Seating—Prior to placing the tray and matrix intraorally, the dentist should ensure that the two can be easily separated, which is essential for complete curing of the BFEP composite. Because the tray and matrix are both 2-mm thick, if they cannot be separated, curing is more difficult and time-consuming. Additionally, when the tray and matrix are separated, the dentist can better view the BFEP and ensure complete coverage and seating.
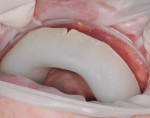
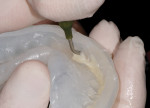
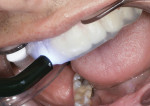
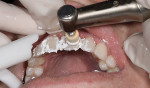
The flowable composite (Reveal) is placed in the matrix that is carried in the hard tray, and then seated intraorally (Figure 15 and Figure 16). After the composite is allowed to flow, the hard tray is removed and the loaded matrix remains on the teeth. At this time, the matrix is evaluated to ensure complete seating. If the matrix is not completely seated, the hard tray is repositioned onto it and pressure is applied again.
After determining that the matrix is seated properly, the BFEP is cured through the matrix (Figure 17); if the matrix encompassed molars, light-curing should begin at the posterior, where it tends to be more challenging to control saliva. To further prevent contamination of the posterior composite, cotton rolls, dry angles, and the saliva ejector have proven useful. Specialized curing lights (Isodry/Isolite, Isolite Systems, www.isolitesystems.com) may also be used that provide retraction and suction when curing to expedite this process. However, these tools may only be utilized when curing one quadrant at a time, per manufacturer’s instructions.
Finishing and Polishing—With the BFEP bonded in place, finishing and polishing become predictable tasks, provided the impressions were free of voids and the definitive matrix fit well. In some cases the composite may appear slightly underfilled or overfilled. When underfilled, there may be a void at a margin that can be easily corrected by flowing more of the same composite into the void, then curing. When overfilled, the resultant flange will require simple trimming or adjustment with a carbide or diamond bur, provided the BFEP fits tightly. However, if the BFEP appears grossly underfilled or overfilled, the case may need to be redone, since composite will either dislodge or appear very porous.
After evaluating the fit of the BFEP, any small amount of flash on the margins is trimmed and the embrasures opened with a carbide or diamond bur (Figure 18). For this process, 12-fluted red-stripe ET carbide burs are recommended, since these will not cut through tooth structure.22 Additionally, red-stripe ET carbide burs work well on composite.22 However, if the composite is too thick, red-stripe ET diamonds are more effective.22 Only use red-stripe burs/diamonds for this process; white and yellow have been found to be ineffective for this technique. After removing the flash, slightly open the interproximal using a serrated cutting instrument (eg, Ceri-Saw™, DenMat, www.denmat.com; IPR Strips, ContacEZ, www.contacez.com). The interproximal should be opened only enough to allow the patient to use a floss threader.
Because the BFEP is basically a 14-unit splint, the dentist must decide whether or not to separate the teeth. However, separating each individual tooth can only be accomplished during the matrix design stage of fabrication.
After trimming and opening the interproximal spaces (Figure 18), occlusal adjustments are completed using the articulating paper, bite down, and protrude technique. If any occlusal or protrusive adjustments are necessary, a fine diamond is used.22 Once occlusal and protrusive adjustments have been made, final finishing and polishing can be completed.
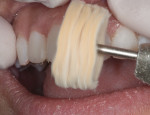
Definitive Finishing and Polishing Technique—To impart a natural and lifelike appearance to the BFEP, a silicone point (Enhance®, DENTSPLY Caulk, www.caulk.com) is quickly grazed over the surface of the composite.23 Water should be used at this point to prevent scorching.23 The composite is then gone over quickly with a diamond-impregnated point (PoGo®, DENTSPLY Caulk).23 Polishing paste (Enhance) is placed on the same point (Enhance), and the composite is polished.
Once a satisfactory polish is achieved, the process is repeated with a felt cup or felt point (FlexiCups/FlexiPoints, Cosmedent) and the same polishing paste (Enhance) to give the BFEP even more luster (Figure 19).23 Final polishing is then completed with a leather buff (Brasseler USA, www.brasselerusa.com) and polishing paste to enhance the gloss (Figure 20). Further, if the dentist would like to bring the final polish to the line angle, leather buffs designed for laboratory use are useful. However, the buffs are particularly large and can only be used to the first bicuspid.
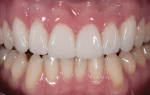
Overall, the entire finishing and polishing technique should take only 2 to 5 minutes per tooth. Further, when finished, the composite BFEP should display a pleasing luster and polish and the esthetics required to meet the needs of the patient until the definitive treatment can be completed (Figure 21 and Figure 22).23
Discussion and Conclusion
Although the BFEP is a simplified treatment to satisfy immediate needs, a certain skill-set is required and, therefore, dentists should not provide full-arch treatment initially. Instead, they should begin with relatively straightforward cases that require only four to six provisionals to gain experience in fabricating proper BFEPs. During this time, it may also be beneficial to complete all restorative dentistry cases in composite to understand the form, function, and esthetics of the different materials available. This will enable dentists to base their BFEP material decisions on the shape, strength, and esthetics required of each case.
After two or three cases, working only back to the bicuspids, the dentist may feel sufficiently comfortable to treat more complex cases. Eventually, after mastering the BFEP concept, the dentist can provide patients with flexible options that incorporate BFEPs for 14 teeth in 1 hour.
The BFEP allows dentists to provide complete dentistry for patients who demand the best in treatment in a short amount time, in an economical manner. Although the author prefers to work in porcelain, the BFEP allows the best in function, stability, and esthetics in the interim, all while spreading the cost of definitive treatment over time to reduce the initial economic impact to the patient.24
ABOUT THE AUTHOR
Edward A. McLaren, DDS, MDC
Clinical Professor, Founder and Director, UCLA Post Graduate Esthetics, Director UCLA Center for Esthetic Dentistry, Founder and Director, UCLA Master Dental Ceramist Program, UCLA School of Dentistry, Los Angeles, California; Private Practice limited to Prosthodontics and Esthetic Dentistry, Los Angeles, California
REFERENCES
1. Junnila T. Growing your practice in a down economy. Northwest Dent. 2010;89(3):49-51.
2. Levin RP. How dentistry weathers a slow economy. J Am Dent Assoc. 2007;138(3):391-392.
3. Alexander RE. Readability of published dental educational materials. J Am Dent Assoc. 2000;131(7):937-942.
4. Lodding DW. Long-term esthetic provisional restorations in dentistry. Curr Opin Cosmet Dent. 1997;4:16-21.
5. Mopper KW. How do composite resins stand the test of time? Dent Today. 2004;23(5):74-76, 78-79.
6. Morley J. The role of cosmetic dentistry in restoring a youthful appearance. J Am Dent Assoc. 1999;130(8):1166-1172.
7. Dietschi D. Free-hand composite resin restorations: a key to anterior aesthetics. Pract Periodontics Aesthet Dent. 1995;7(7):15-25.
8. Raigrodski AJ, Sadan A, Mendez AJ. Use of a customized rigid clear matrix for fabricating provisional veneers. J Esthet Dent. 1999;11(1):16-22.
9. Kugel G, Ferrari M. The science of bonding: from first to sixth generation. J Am Dent Assoc. 2000;(suppl 131):20S-25S.
10. Radovic I, Monticelli F, Goracci C, et al. Self-adhesive resin cements: a literature review. J Adhes Dent. 2008;10(4):251-258.
11. Lührs AK, Guhr S, Günay H, Geurtsen W. Shear bond strength of self-adhesive resins compared to resin cements with etch and rinse adhesives to enamel and dentin in vitro. Clin Oral Investig. 2010;14(2):193-199.
12. Strassler HE, Anolik C, Frey C. High-strength, aesthetic provisional restorations using a bis-acryl composite. Dent Today. 2007;26(11):128, 130-133.
13. Gürel G, Bichacho N. Permanent diagnostic provisional restorations for predictable results when redesigning the smile. Pract Proced Aesthet Dent. 2006;18(5):281-286.
14. Nixon RL. Provisionalization for ceramic laminate veneer restorations: a clinical update. Pract Periodontics Aesthet Dent. 1997;9(1):
17-27.
15. Gegauff AG. Provisional restorations. In: Rosensteil SF, Land MF, Fujimoto J, eds. Contemporary Fixed Prosthodontics. 2nd ed. St. Louis, MO: Mosby-Year Book; 1995:325,329
16. Fahl Júnior N. The direct/indirect composite resin veneers: a case report. Pract Periodontics Aesthet Dent. 1996;8(7):627-638.
17. LeSage BP. Improving implant aesthetics: prosthetically generated papilla through tissue modeling with composite. Pract Proced Aesthet Dent. 2006;18(4):257-263.
18. Hervás-García A, Martínez-Lozano MA, Cabanes-Vila J, et al. Composite resins. A review of the materials and clinical indications. Med Oral Patol Oral Cir Bucal. 2006;11(2):E215-E220.
19. Barghi N. To silanate or not to silanate: making a clinical decision. Compend Contin Educ Dent. 2000;21(8):659-662, 664.
20. Lopes GC, Thys DG, Klaus P, et al. Enamel acid etching: a review. Compend Contin Educ Dent. 2007;28(1):18-24.
21. Hobson RS, McCabe JF, Rugg-Gunn AJ. The relationship between acid-etch patterns and bond survival in vivo. Am J Orthod Dentofacial Orthop. 2002;121(5):502-509.
22. Jefferies SR. The art and science of abrasive finishing and polishing in restorative dentistry. Dent Clin North Am. 1998;42(4):613-627.
23. Jefferies SR. Abrasive finishing and polishing in restorative dentistry: a state-of-the-art review. Dent Clin North Am. 2007;51(2):379-397.
24. McLaren EA, LeSage B. Feldspathic veneers: what are their indications? Compend Contin Educ Dent. 2011;32(3):44-49.
Related Content:
For more information, read Combine Conventional and Digital Methods to Maximize Shade Matching at