Comparison of Clinical Efficacy of Three Professionally Applied Pastes on Immediate and Sustained Reduction of Dentin Hypersensitivity
Yiming Li, DDS, MSD, PhD; Sean Lee, DDS; Luis R. Mateo, MA; Evaristo Delgado, DDS, MSc; and Yun Po Zhang, PhD, DDS(hon)
Abstract
OBJECTIVE: The objective of this study was to compare the clinical efficacy of an in-office desensitizing paste (positive control) to that of a paste containing casein phosphopeptide and amorphous calcium phosphate (CPP-ACP) with 0.2% NaF and a fluoride-free pumice prophylaxis paste (negative control) on dentin hypersensitivity reduction immediately and after 4 weeks following a single professional post-scaling application.
METHODS: Subjects (120) were assigned to one of the three groups: 1) Colgate® Sensitive Pro-Relief™ Desensitizing paste with 8% arginine and calcium carbonate (Arg/CaCO3); 2) MI Paste Plus™ (CPP-ACP); and 3) Nupro®-M prophylaxis paste (negative control). Subjects received a scaling procedure and then a single application of the assigned paste. Dentin hypersensitivity was examined using the Yeaple tactile and air-blast (Schiff Scale) methods immediately after the treatment and again after 4 weeks. Subjects were provided a non-desensitizing dentifrice for toothbrushing at home during the 4-week study period. The analysis of covariance (ANCOVA) was performed to examine the between-treatment effects, and the within-treatment effects were analyzed using paired t-tests. When indicated, a post-hoc Tukey’s multiple comparison test was performed on the pair-wise comparisons.
RESULTS: All 120 subjects complied with the protocol and completed the study. All three groups showed a significant reduction in tactile and air-blast stimulated dentin hypersensitivity immediately and after 4 weeks following the single application (P < 0.05). The subjects assigned to the Arg/CaCO3 group exhibited a significant improvement in mean tactile and air-blast dentin hypersensitivity scores as compared to both the CPP-ACP and negative control pastes (P < 0.05).
CONCLUSIONS: A single post-scaling treatment with the 8% arginine and calcium carbonate desensitizing paste significantly reduces dentin hypersensitivity immediately and after 4 weeks, and it is significantly more effective than the paste containing casein phosphopeptide and amorphous calcium phosphate and negative control pastes.
Tooth sensitivity, or what is more precisely termed “dentin hypersensitivity,” is defined as a short, sharp pain arising from exposed dentin in response to stimuli, typically thermal, evaporative, tactile, osmotic, or chemical, and it cannot be ascribed to any other forms of dental defect or pathology.1 Studies have reported that dentin hypersensitivity affects more than half of dental patients of different lifestyles and cultures, and it appears to peak between 20 to 40 years of age.2-8 It has become one of the most commonly heard complaints in dentistry; Strassler and coworkers called tooth sensitivity the “common cold of dentistry.”9
The hydrodynamic theory is widely accepted for describing the occurrence of dentin hypersensitivity, which holds that the sensation is caused by the activation of mechanoreceptors in intratubular nerves or in the superficial pulp due to changes of the flow and/or volume of fluid within dentinal tubules.10,11 While numerous etiological factors causing dentin hypersensitivity have been identified, a common key characteristic is the exposed dentin that allows the stimuli to affect the dentin tubular fluid and consequently to activate the pulpal nerves for the perception as pain by the patient. Studies have found a high incidence of dentin hypersensitivity—ranging from 60% to 98%—in patients following periodontal treatment, which often results in dentin exposure.3,11,12 Consequently, a major approach for treating or managing dentin hypersensitivity is to eliminate or minimize the changes of dentin tubular fluid by sealing the exposed dentin. Various agents, materials, and measures have been used to occlude the open dentin tubules, including fluoride, casein phosphopeptide-amorphous calcium phosphate (CPP-ACP), potassium oxalate, resin sealers, and lasers.11,13-17 More recently, a novel technology using 8% arginine, an amino acid found in saliva, in dental prophylaxis paste has been introduced to control dentin hypersensitivity.18 The mechanism of this new desensitizing formulation mimics saliva’s natural process of plugging and sealing open dentinal tubules. The formed sealing plugs are composed of arginine, calcium, phosphate, and carbonate, and studies have shown that its strength is adequate to withstand normal pulpal pressures and acid challenges, effectively reducing the dentin flow and, consequently, the sensation of tooth sensitivity.19-22
The objective of this 4-week, parallel, double-blind, stratified, and randomized clinical study was to compare the clinical efficacy in reducing dentin hypersensitivity of Colgate® Sensitive Pro-Relief™ Desensitizing paste (Colgate-Palmolive Co., www.colgateprofessional.com) containing 8% arginine and calcium carbonate to that of MI Paste Plus™ (GC Corporation, www.gcamerica.com) containing CPP-ACP with 0.2% sodium fluoride and Nupro®-M pumice-based fluoride-free prophylaxis paste (DENTSPLY International, www.dentsply.com) instantly after application as a single in-office treatment following a dental scaling procedure. A second objective was to compare the longevity of sensitivity relief after a period of 4 weeks.
Materials and Methods
Prior to the initiation of the study, the protocol and letter of informed consent were approved by the Institutional Review Board (IRB) of Loma Linda University. Study participants were 120 healthy adults of 18 to 70 years of age, having a minimum of two hypersensitive teeth among incisors, canines, and premolars of cervical erosion/abrasion or gingival recession, each with a tactile hypersensitivity stimuli score of 10 to 50 grams of force, as determined using a calibrated Yeaple Electronic Pressure Sensitive Probe (Model 200A, Yeaple Research, Inc., www.yeapleprobe.com) and an air-blast stimuli score of 2 or 3 (Schiff Cold Air Sensitivity Scale) at the baseline examination. Eligible subjects were required to be available for the 4-week study duration and to sign an informed consent form.
Prospective subjects with the following conditions were excluded for the study: gross oral pathology; chronic oral diseases; advanced periodontal disease; treatment for periodontal disease within 1 year; and sensitive teeth with a mobility greater than one, extensive or defective restorations, suspected pulpitis, caries, cracked enamel, or used as abutments for removable partial dentures. The exclusion was also applied to the following conditions: current use of anticonvulsants, antihistamines, antidepressants, sedatives, tranquilizers, anti-inflammatory drugs, or daily analgesics; pregnant or lactating women; participation in a desensitizing dentifrice study or use of a desensitizing dentifrice within the previous 3 months; currently participating in another clinical study; history of allergy to oral care/personal care consumer products or the test products of the present study; or any existing medical conditions that precluded them from not eating and drinking for periods up to 4 hours.
The study was a three-cell, double-blind, parallel-group, and stratified and randomized clinical investigation. Each enrolled study participant was randomly assigned to one of the three treatment groups, which were balanced using the baseline tactile and air-blast hypersensitivity scores. The three professionally applied pastes were: 1) Positive Control: Colgate® Sensitive Pro-Relief™ Desensitizing paste (Colgate-Palmolive Co.), a fluoride-free desensitizing paste containing 8% arginine and calcium carbonate (Arg/CaCO3); 2) Test Product: MI Paste Plus™ (GC Corporation) containing CPP-APP and 0.2% sodium fluoride; and 3) Negative Control: Nupro®-M (Dentsply International) pumice-based fluoride-free prophylaxis paste.
For each visit, subjects were instructed to refrain from oral hygiene procedures and chewing gum for 8 hours and from eating and drinking for 4 hours prior to their examination. After the baseline evaluation of oral tissues and dentin hypersensitivity of the two identified teeth using the Yeaple tactile probe and Schiff cold air-blast method,23 each subject received a professionally administered scaling procedure and then the application of the assigned paste that consisted of two consecutive 3-second applications of the product using a rotating prophy cup aimed at the gingivo-facial one-third of the teeth. Professional scaling and product application were performed by a dental hygienist who, like the study examiner, was blinded to product identity. Immediately after the product application, tactile and air-blast hypersensitivity examinations were again performed by the study examiner. Subjects were then provided with a commercially available, non-desensitizing dentifrice containing 0.243% sodium fluoride (Crest® Anti-Cavity Fluoride Toothpaste, Procter & Gamble Co., www.pg.com) and an adult soft-bristled toothbrush (Colgate Extra Clean Toothbrush—adult/soft/full head, Colgate-Palmolive Co.), and instructed to brush their teeth at home, twice daily, each time for 1 minute for the next 4 weeks. The subjects were also instructed not to use any other oral hygiene products. There were no restrictions regarding diet or smoking habits during the course of the study. Assessments of oral tissues and tactile and air-blast dentin hypersensitivity were repeated after 4 weeks by the same examiner using the same methods. At each visit, each subject was also interviewed regarding adverse events and the use of concomitant medications.
Subjects and study examiner remained blinded to product assignment and application for the duration of the study. The three pastes provided to the investigator were overwrapped and identified only with a product code. The examiner was not present when the assigned paste was applied.
For the measurement of Yeaple tactile hypersensitivity, the instrument was calibrated daily following manufacturer’s instructions. Scores were recorded in terms of the quantified reproducible force (grams applied through a #19 explorer tip) that was required to elicit discomfort using the established procedures.24,25 Briefly, the subject was instructed to respond at the point where he or she first experienced discomfort. The explorer tip of the probe was applied to the buccal surface of each hypersensitive tooth at the cemento-enamel junction (CEJ). The explorer tip was stroked perpendicular to the tooth beginning at a pre-set force of 10 grams and increased by 10-gram increments until the subject experienced discomfort, or until 50 grams of force was applied.
For evaluating the air-blast hypersensitivity, the tooth to be examined was isolated from the adjacent teeth (mesial and distal) by placing the examiner’s fingers over the adjacent teeth. Air was delivered from a standard dental unit air syringe at 60 psi (± 5 psi) and 70°F (± 3°F), directing at the exposed buccal surface of the hypersensitive tooth for 1 second from a distance of approximately 1 cm. The Schiff Cold Air Sensitivity Scale23 was used to assess subject response to this stimulus, as follows:
0: Subject did not respond to air stimulus.
1: Subject responded to air stimulus but did not request discontinuation of stimulus.
2: Subject responded to air stimulus and requested discontinuation or moved from stimulus.
3: Subject responded to air stimulus, considered stimulus to be painful, and requested discontinuation of the stimulus.
The oral tissue examination included visual assessment of the soft and hard palate, gingival and buccal mucosa, mucogingival fold areas, tongue, sublingual and submandibular areas, salivary glands, and the tonsilar and pharyngeal areas.
The codes of the three groups were broken after the completion of the study and data analyses. The tactile and air-blast scores were calculated separately by averaging the values measured on the two qualified teeth for each subject, and the baseline data were analyzed using the analysis of variances (ANOVA). The paired t-test was performed to examine the within-treatment effects. The treatment groups with respect to baseline-adjusted tactile hypersensitivity and air-blast hypersensitivity scores at the follow-up examinations were compared using the analysis of covariance (ANCOVA). If a statistical significant difference was detected among the treatment groups by the ANCOVA analysis, a post-hoc Tukey’s multiple comparison test was performed on the pair-wise comparisons. All statistical tests were two-sided using a level of significance of α = 0.05.
Results
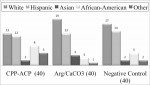
All 120 subjects completed the study. As shown in Table 1, the demographic compositions are comparable among the three groups. The average age was 44.0, 44.7, and 42.3, and the females accounted for 72.5%, 80.0%, and 77.5% for the Arg/CaCO3, CPP-ACP, and negative control groups, respectively. The race composition was also similar among the three groups (Figure 1).
Table 2 presents the baseline Yeaple tactile and Schiff air-blast hypersensitivity scores, which were comparable among the three groups. The baseline tactile force to induce the sensitivity was 21.13, 22.88, and 22.00 grams for the Arg/CaCO3, CPP-ACP, and negative control groups, respectively. Immediately after the single application of the pastes, the mean tactile force increased to 46.63, 29.75, and 29.25 for the Arg/CaCO3, CPP-ACP, and negative control groups, respectively (Table 3). The changes of Yeaple tactile force compared with the baseline were 120.7% for Arg/CaCO3 paste, 30.0% for CPP-ACP paste, and 33.0% for negative control paste; the changes were statistically significant (P < 0.05) for all three groups (Figure 2 and Table 3).
When the tactile data were compared among the three groups, the Arg/CaCO3 paste was significantly more effective (P < 0.05) than the CPP-ACP paste (56.7%) and the negative control paste (59.4%) in reducing the tactile hypersensitivity immediately after a single application (Table 3). The two groups of CPP-ACP and negative control pastes were statistically comparable, with a difference of only 1.7% (Table 3).
The results obtained from the air-blast examination were consistent with and supportive of the effectiveness of the single use of the Arg/CaCO3 paste to reduce the dentin hypersensitivity (Figure 3 and Table 4). The mean baseline air-blast hypersensitivity score for Arg/CaCO3 paste was 2.40 (Table 2), which, immediately after the single application, decreased to 1.01, which is a reduction of 57.9%, while the percentage reductions for the CPP-ACP and negative control pastes were 29.0% and 29.9%, respectively. The changes were statistically significant (P < 0.05) for all three groups (Table 4).
The analysis of between-treatment effect showed that the Arg/CaCO3 paste was significantly more effective (P < 0.05) in reducing air-blast hypersensitivity immediately after a single application than the CPP-ACP paste (40.9%) and the negative control paste (40.9%). The post-treatment air-blast hypersensitivity scores for CPP-ACP and negative control pastes were the same (Table 4).
The 4-week results were similar to those obtained from the immediate post-treatment. The average Yeaple tactile force that induced the hypersensitivity was 46.38 g for the Arg/CaCO3 paste, 29.00 g for the CPP-ACP paste, and 28.25 g for the negative control paste, which remained essentially the same as those of immediately after the single application of corresponding products (Figure 2 and Table 5). The changes from baseline were 119.5%, 26.7%, and 28.4% for the Arg/CaCO3 paste, the CPP-ACP paste, and the negative control paste, respectively; the within-treatment effect was again significant (P < 0.05) for all three groups (Table 5). The between-treatment analysis showed that the Arg/CaCO3 paste maintained its superiority compared to the CPP-ACP paste (59.0%) and the negative control paste (64.2%); and the differences were significant (P < 0.05). The difference between CPP-ACP paste and the negative control paste was 2.7%, and their mean values were statistically comparable (Table 5).
Table 6 presents the results of the 4-week air-blast hypersensitivity examination and the statistical analysis of the within- and between-treatment effects. Again, the overall data were consistent with and supportive of those obtained from the Yeaple tactile method (Figure 3 and Table 6). The average air-blast sensitivity score of the Arg/CaCO3 paste group further reduced slightly to 0.79, while for the CPP-ACP paste and the negative control paste groups, the means were 1.73 and 1.64, respectively. The percent changes from baseline were 67.1% for Arg/CaCO3 paste, 28.2% for the CPP-ACP paste, and 32.8% for the negative control paste, of which all groups were statistically significant (P < 0.05). The analysis of between-treatment effects indicated that after 4 weeks, the Arg/CaCO3 paste group maintained a significantly greater reduction in air-blast hypersensitivity (P < 0.05) than the CPP-ACP and negative control paste groups (54.3% and 51.8%, respectively), while the latter two groups were statistically comparable, with a difference of 5.5% (Table 6).
There were no adverse effects on oral hard and soft tissues detected in any of the three groups at any of the visits.
Discussion
Dental prophylaxis is a routine and effective procedure for removing dental plaque and calculus and reducing associated risks; it also removes tooth-surface stains. The use of a prophylaxis paste enhances the cleaning efficacy and polishes the cleaned tooth surfaces. However, the process of scaling and polishing can increase the risk of dentin hypersensitivity, especially in patients with exposed dentin. The unpleasant sensation of dentin hypersensitivity after the dental prophylaxis may temporarily interfere with normal oral hygiene practice and even eating and drinking, and the individual may thus be discouraged to keep a regular schedule for dental prophylaxis. Consequently, various desensitizing agents have been incorporated into prophylaxis pastes to reduce post-procedure dentin hypersensitivity.
The present study compared Colgate Sensitive Pro-Relief Desensitizing paste to MI Paste Plus and Nupro-M paste for their effectiveness in reducing dentin hypersensitivity immediately after a dental scaling, and again after a period of 4 weeks. The data showed that all three pastes provided the immediate benefit of reducing both the tactile and thermal dentin hypersensitivity (Table 3 and Table 4), which was statistically significant (P < 0.05) and sustained for 4 weeks (Table 4 and Table 6). Nupro-M paste contains no fluoride or other obvious active ingredients for dentin hypersensitivity; therefore, the Hawthorne effect26 and/or the strong placebo effect27 that is often observed in dentin hypersensitivity clinical trials cannot be excluded. These findings indicate the importance of designing and conducting clinical studies with adequate blindness to both the subjects and examiners.
The concept of delivering calcium and phosphate to form calcium phosphate at the proposed site of action has been one of longstanding interest for dentin hypersensitivity relief as well as for anti-caries purposes. It has historically been a challenge to develop stable materials that can deliver a clinically proven benefit derived from the release of calcium and phosphate into an environment such as that encountered in the oral cavity, which is already supersaturated with calcium and phosphate. While several approaches to deposition of amorphous calcium phosphate on the tooth surface have been investigated, published clinical data demonstrating effective dentin hypersensitivity relief from products delivering amorphous calcium phosphate are sparse.28 MI Paste Plus contains CPP-ACP and 0.2% sodium fluoride. The CPP is a casein phosphopeptide, which is capable of stabilizing insoluble amorphous calcium phosphate, as the CPP-ACP complex.29,30 MI Paste Plus is proposed to promote remineralization through the deposition of fluoride-containing calcium-phosphate precipitates, to help prevent dental caries and dentin hypersensitivity. However, the results of the studies published in the literature are inconsistent.17,31-33 A 2008 systematic review of the literature by Azarpazhooh and Limeback concluded that “there is insufficient clinical trial evidence (in quantity, quality or both) to make a recommendation regarding the long-term effectiveness of casein derivatives, specifically CPP-ACP, in preventing caries in vivo and in treating dentin hypersensitivity or dry mouth.”16 The authors questioned the potential possibility of interactions between fluoride and ACP that may precipitate out as calcium fluoride, rendering both inorganic components ineffective. This assumption may help explain the observation in the present clinical trial that dentin hypersensitivity decreased to a similar degree for subjects assigned to the MI Paste Plus group and for those assigned to the negative control group.
The results of the present study demonstrate that, at both the post-treatment and 4-week evaluation points, Colgate Sensitive Pro-Relief Desensitizing paste provides significantly higher efficacy in reducing dentin hypersensitivity than both MI Paste Plus and Nupro-M paste. The data are consistent for the tactile and air-blast evaluations, as well as with previous studies on the same and similar formulations of 8% Arg/CaCO3.19,21,22,34 The overall data are also supportive of and consistent with laboratory investigations on mechanism of action of the 8% Arg/CaCO3-based products using various state-of-the-art technologies and instruments, including atomic-force microscopy, confocal laser scanning microscopy, electron spectroscopy, and high-resolution scanning electron, which clearly showed their effective and robust occlusion of open dentin tubules.18,20
The present study included a comprehensive examination of oral soft and hard tissues, which found no evidence of any abnormalities or adverse changes of the tissues throughout the 6-month period. In addition, when questioned, none of the subjects reported any experience of adverse effects, related or non-related to the study products, at any of the clinical visits. This confirms that Colgate Sensitive Pro-Relief Desensitizing paste is clinically safe and effective.
Conclusions
A single professionally applied post-scaling treatment of the positive control, Colgate Sensitive Pro-Relief Desensitizing paste containing 8% arginine and calcium carbonate, provides statistically significant reductions in dentin hypersensitivity immediately after its application, as compared to the negative control, Nupro-M paste, and the efficacy is maintained for a period of 4 weeks post-application. In addition, the single post-scaling treatment with Colgate Sensitive Pro-Relief Desensitizing paste is statistically significantly more effective than the test product, MI Paste Plus, immediately after application and after a period of 4 weeks, while the effect of MI Paste Plus is not statistically significantly different from Nupro-M paste. All three professionally applied pastes are safe to use on oral tissues when used as instructed.
Disclosure
The study was supported by a grant from the Colgate-Palmolive Company.
About the Authors
Yiming Li, DDS, MSD, PhD
Professor and Director
Center for Dental Research
Loma Linda University School of Dentistry
Loma Linda, California
Sean Lee, DDS
Professor and Director
Clinical Research Core
Center for Dental Research
Loma Linda University School of Dentistry
Loma Linda, California
Luis R. Mateo, MA
President
LRM Statistical Consulting
Hoboken, New Jersey
Evaristo Delgado, DDS, MSc
Manager of Technology
Clinical Dental Research
Colgate-Palmolive Company
Piscataway, New Jersey
Yun Po Zhang, PhD, DDS(hon)
Director
Clinical Dental Research
Colgate-Palmolive Company
Piscataway, New Jersey
References
1. Ajcharanukul O, Kraivaphan P, Wanachantararak S, et al. Effects of potassium ions on dentine sensitivity in man. Arch Oral Biol. 2007;52(7):632-639.
2. Addy M. Dentine hypersensitivity: new perspectives on an old problem. Int Dent J. 2002;52(suppl 5):367-375.
3. Addy M. Etiology and clinical implications of dentine hypersensitivity. Dent Clin North Am. 1990;34(3):503-514.
4. Irwin CR, McCusker P. Prevalence of dentine hypersensitivity in a general dental population. J Ir Dent Assoc. 1997;43(1):7-9.
5. Liu HC, Lan WH, Hsieh CC. Prevalence and distribution of cervical dentin hypersensitivity in a population in Taipei, Taiwan. J Endod. 1998;24(1):45-47.
6. Rees JS, Addy M. A cross-sectional study of dentine hypersensitivity. J Clin Periodontol. 2002;29(11):997-1003.
7. Al-Wahadni A, Linden GJ. Dentine hypersensitivity in Jordanian dental attenders: A case control study. J Clin Periodontol. 2002;29(8):688-693.
8. West NX. Dentine hypersensitivity. In: Lussi A. Dental Erosion. Monogr Oral Sci. Basel, Switzerland: Karger; 2006;20:173-189.
9. Strassler HE, Drisko CL, Alexander DC. Dentin hypersensivity: its inter-relationship to gingival recession and acid erosion. Compend Contin Educ Dent. 2008;29(5)(spec iss):1-9.
10. Matthews B, Vongsavan N. Interactions between neural and hydrodynamic mechanisms in dentine and pulp. Arch Oral Biol. 1994;39(suppl):87S-95S.
11. Pashley DH, Tay FR, Haywood VB, et al. Consensus-based recommendations for the diagnosis and management of dentin hypersensitivity. Inside Dentistry. 2008;4(9)(spec iss):1-35.
12. Drisko CH. Dentine hypersensitivity: dental hygiene and periodontal considerations. Int Dent J. 2002;52:385-393.
13. Schwarz F, Arweiler N, Georg T, Reich E. Desensitizing effects of an Er:YAG laser on hypersensitive dentine. J Clin Periodontol. 2002;29(3):211-215.
14. Suge T, Kawasaki A, Ishikawa K, et al. Comparison of the occluding ability of dentinal tubules with different morphology between calcium phosphate precipitation method and potassium oxalate treatment. Dent Mater J. 2005;24(4):522-529.
15. Birang R, Poursamimi J, Gutknecht N, et al. Comparative evaluation of the effects of Nd:YAG and Er:YAG laser in dentin hypersensitivity treatment. Lasers Med Sci. 2007;22(1):21-24.
16. Azarpazhooh A, Limeback H. Clinical efficacy of casein derivatives: a systematic review of the literature. J Am Dent Assoc. 2008;139(7):915-924.
17. Tang B, Millar BJ. Effect of chewing gum on tooth sensitivity following whitening. Br Dent J. 2010;208(12):571-577.
18. Cummins D. Dentin hypersensitivity: from diagnosis to a breakthrough therapy for everyday sensitivity relief. J Clin Dent. 2009;20(1):1-9.
19. Hamlin D, Williams KP, Delgado E, et al. Clinical evaluation of the efficacy of a desensitizing paste containing 8% arginine and calcium carbonate for the in-office relief of dentin hypersensitivity associated with dental prophylaxis. Am J Dent. 2009;22(spec no A):16A-20A.
20. Petrou I, Heu R, Stranick M, et al. A breakthrough therapy for dentin hypersensitivity: how dental products containing 8% arginine and calcium carbonate work to deliver effective relief of sensitive teeth. J Clin Dent. 2009;20(1):23-31.
21. Panagakos F, Schiff T, Guignon A. Dentin hypersensitivity: effective treatment with an in-office desensitizing paste containing 8% arginine and calcium carbonate. Am J Dent. 2009;22(spec no A):3A-7A.
22. Schiff T, Delgado E, Zhang YP, et al. Clinical evaluation of the efficacy of an in-office desensitizing paste containing 8% arginine and calcium carbonate in providing instant and lasting relief of dentin hypersensitivity. Am J Dent. 2009;22(spec no A):8A-15A.
23. Schiff T, Dotson M, Cohen S, et al. Efficacy of a dentifrice containing potassium nitrate, soluble pyrophosphate, PVM/MA copolymer, and sodium fluoride on dentinal hypersensitivity: a twelve-week clinical study. J Clin Dent. 1994;5(spec no):87-92.
24. Clark GE, Troullos ES. Designing hypersensitivity clinical studies. Dent Clin North Am. 1990;34(3):531-544.
25. Gillam DG, Bulman JS, Jackson RJ, Newman HN. Efficacy of a potassium nitrate mouthwash in alleviating cervical dentine sensitivity (CDS). J Clin Periodontol. 1996;23(11):993-997.
26. Leonard KL. Is patient satisfaction sensitive to changes in the quality of care? An exploitation of the Hawthorne effect. J Health Econ. 2008;27(2):444-459.
27. West NX, Addy M, Jackson RJ, Ridge DB. Dentin hypersensitivity and the placebo response. A comparison of the effect of strontium acetate, potassium nitrate and fluoride toothpastes. J Clin Periodontol. 1997;24(4):209-215.
28. Cummins D. Recent advances in dentin hypersensitivity: clinically proven treatments for instant and lasting sensitivity relief. Am J Dent. 2010;23(spec no A):3A-13A.
29. Reynolds EC, Cain CJ, Webber FL, et al. Anticariogenicity of calcium phosphate complexes of tryptic casein phosphopeptides in the rat. J Dent Res. 1995;74(6):1272-1279.
30. Reynolds EC. Anticariogenic complexes of amorphous calcium phosphate stabilized by casein phosphopeptides: a review. Spec Care Dentist. 1998;18(1):8-16.
31. Suge T, Ishikawa K, Kawasaki A, et al. Calcium phosphate precipitation method for the treatment of dentin hypersensitivity. Am J Dent. 2002;15(4):220-226.
32. Kowalczyk A, Botuliński B, Jaworska M, et al. Evaluation of the product based on Recaldent technology in the treatment of dentin hypersensitivity. Adv Med Sci. 2006;51(suppl 1):40-42.
33. Martinez-Mier EA. Casein phosphopeptide used in toothpaste suggests an efficacy similar to toothpaste containing sodium monofluorophosphate for caries prevention. J Evid Based Dent Pract. 2010;10(3):154-155.
34. Garcia-Godoy F, Garcia-Godoy A, Garcia-Godoy C. Effect of a desensitizing paste containing 8% arginine and calcium carbonate on the surface roughness of dental materials and human dental enamel. Am J Dent. 2009;22(spec no A):21A-24A.