Transitional Bonding with the Kois Deprogrammer: A Conservative Treatment Approach
Abstract
Restoration of a worn dentition has many challenges and considerations for the restorative dentist. Decisions on how to reconstruct the tooth structure that was lost as well as eliminating the risk factors that caused the problem must be addressed. Adding to the complexity is the ever-present demand for minimal dentistry that will satisfy the goals of the treatment while not increasing the long-term risks. A systematic approach to analyze periodontal, biomechanial, functional, and dentofactial risk must be considered before making treatment recommendations to the patient. The patient’s esthetic concerns were addressed in this case using minimal- to no-preparation techniques. The placement of transitional bonding with the aid of a Kois deprogrammer allowed the restorative dentist and laboratory technician to meet the functional and esthetic requirements of the case.
As the goal of any restorative plan should be to minimize risk and improve prognosis, the treatment plan must always first assess periodontal, biomechanical, functional, and dentofacial risk. In this case, the Kois deprogrammer made it possible for the practitioner to find, establish, maintain, and verify an acceptable vertical dimension in centric relation throughout the process. In keeping with dentofacial requirements, direct composite was applied to the incisal edges in a non-invasive approach. Tooth preparations were supragingival and remained in enamel in consideration of biomechanical and periodontal risks; and functional risk due to bruxism was managed but not eliminated with a night guard. The end result was a restorative plan using a predictable and conservative approach that fulfilled the patient’s esthetic desires while managing risk.
Clinical Case Overview
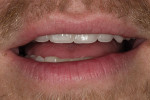
Patient History and Chief Complaint: A 30-year-old man presented with a chief complaint regarding the esthetics of his smile, particularly the lack of visible tooth display. He expressed the desire for a whiter color and longer teeth. Upon further discussion, he elaborated that the wear to his anterior teeth made him appear much older than his age, and being in the entertainment business, this was of major concern.
The patient’s medical history was non-contributory. His dental history revealed he was sporadic in his dental re-care appointments. He reported no dental pain or discomfort. He had a history of consuming sports drinks while playing team sports, but that habit was no longer active.
Diagnostic Findings
Periodontal: Upon periodontal probing, the majority of depths were 3 mm or less, with no bleeding. There were isolated 4-mm probing depths and light bleeding upon probing around three molars. Clinically, there were no signs of mobility. Bone levels were within 2 mm of the cementoenamel junction with no infrabony defects. There were no shared risk factors for bone loss. Slight recession of less than 1 mm was exhibited on teeth Nos. 20 through 22 and 27 through 29. The periodontal diagnosis was AAP Type 1.
Risk: Low
Prognosis: Good
Biomechancial: There were no active caries present; however, the examination revealed several older posterior amalgams that were questionable. Tooth No. 31 was structurally compromised due to the size of the current restoration, and tooth No. 12 also had prior endodontic treatment. There was moderate erosion on the occlusal surfaces of teeth Nos. 18 and 19, and there was minimal erosion on the occlusal surfaces of teeth Nos. 2, 3, 14, 15, 30, and 31. There was evidence of interproximal enamel demineralization on teeth Nos. 7 through 10.
Risk: Moderate
Prognosis: Fair
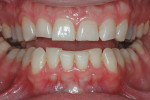
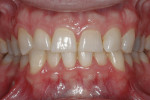
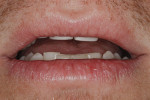
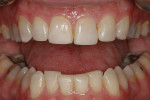
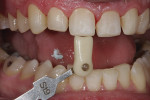
Functional: The patient had a normal range of opening. The immobilization test and loading test produced no joint pain or muscle discomfort, and no temporomandibular joint noises were present. Severe attrition was evident on teeth Nos. 5 through 12 and 20 through 29, and there was moderate attrition on teeth Nos. 2 through 4, 13 through 15, 18, 19, 30, and 31. There was no history of neurologic disorders, and the patient reported a lack of awareness of any sleep bruxism. The amount of attrition present on the teeth was significant, and given the patient’s age, the long-term prognosis was guarded. The generalized wear facets presenting on the posterior teeth as well as the maxillary and mandibular incisal edges was consistent with an inefficient use of the masticatory muscles creating an inefficient chewing pattern. A diagnosis of occlusal dysfunction was made, although the generalized moderate-to-severe attrition may also have been caused by adaptive mechanisms and/or parafunction. The possibility of parafunction (nocturnal bruxism) combined with occlusal dysfunction may have exacerbated the breakdown in the system. A combined diagnosis of occlusal dysfunction and parafunction was rendered (Figure 1 and Figure 2).1
Risk: Moderate-High. Dysfunction would be moderate risk; bruxism would make it high risk.
Prognosis: Fair if just dysfunction; poor if combined with parafunction.
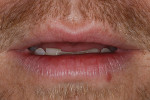
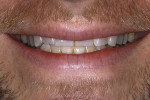
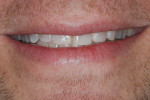
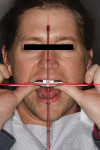
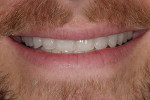
Dentofacial: The maxillary incisal edge position relative to face and lip was deficient and unacceptable for the patient. In the resting position, there was no display of maxillary teeth (Figure 3). Clinical photography was essential to capture the patient’s true and unguarded smile; the patient had learned to posture his lips and teeth in a particular fashion that unnaturally maximized the amount of tooth display (Figure 4). The full-face photographs displayed a brachycephalic facial form with hypertrophy of the masseter muscles (Figure 5). There was a slight gingival architecture asymmetry with the lips retracted, but this was not a concern, given the lack of gingival display. Exceeding the patient’s vision would present less of a challenge, given the medium lip dynamics, incomplete tooth display, and inability to display gingival architecture. While tooth reveal was low, the patient’s profession before the public increased his dentofacial risk.
Risk: Moderate
Prognosis: Fair
Treatment Plan
The patient’s primary goal was to enhance the esthetics with more visible tooth display, while minimizing the risks for future loss of tooth structure. The only uncertainty in the diagnosis was related to function. The patient did not want to take the time to wear a bite splint prior to treatment to verify or refute nighttime bruxism. However, he was willing to wear a bite splint following any restorative treatment. To determine the amount of dentistry involved, it would be necessary to first establish the appropriate length, size, and shape of the anterior teeth. The desired incisal edge position would, in effect, determine the degree to which the vertical dimension should be increased. The concept of conservative dentistry, using minimal tooth preparation, was also discussed. The patient was concerned about an alteration of his existing occlusion. Although the system was functioning inefficiently and contributing to substantial attrition, it had not caused him any pain in his joints or muscles, and he was unrestricted in the foods he was able to chew. These variables were discussed, and it was decided to phase the treatment to allow a transition period to enable the patient to be comfortable with the esthetics as well as the new occlusal relationship.2
Treatment Phases
Phase I: Establish Centric Relationship and Complete Transitional Bonding
The initial preparation required the fabrication of a Kois deprogrammer that was used to establish a centric relation position. The patient wore the appliance continuously for 2 weeks, except during meals. Although the patient had no symptoms before treatment, it is necessary to ensure that no new symptoms are created from wearing the appliance. A reproducible, single point of contact with the absence of symptoms was accomplished and verified.
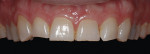
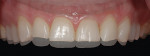
The next protocol was to establish the maxillary incisal edge position that would satisfy the patient’s esthetic desires. Pumice Preppies™ (Whipmix, www.whipmix.com) in a rubber cup were used to clean the facial and incisal edges of teeth Nos. 4 through 13 and 20 through 29. The unprepared enamel on teeth Nos. 8 and 9 was etched with 35% phosphoric acid (Ultra-Etch®, Ultradent Products, Inc., www.ultradent.com) for 60 seconds, bonded with adhesive resin (iBond®, Heraeus Kulzer, www.heraeus-dental-us.com), and composite resin (Venus Diamond®, Heraeus Kulzer) was placed to establish an acceptable incisal edge position. Tooth No. 8 displayed about 2 mm in repose, and tooth No. 9 was given more length to display about 3 mm (Figure 6). This allowed the patient to visualize slightly different lengths and approve the esthetic goal (Figure 7). The laterals were bonded using the same protocol. It was then necessary to verify that the new anterior tooth length did not encroach on the envelope of function. Adjustments were made to the deprogrammer platform that would open the vertical dimension just enough to allow this. With the deprogrammer in place, the canines were simultaneously built up to that vertical dimension and checked with shimstock (Almore International, www.almore.com). The same protocol was used to build the premolars and first molars. At that point, the vertical dimension was established, the deprogrammer was removed, and the posterior contact points were refined with Trollfoil articulating paper (TrollPlast, www.trollplast.com) and verified with shimstock. The chewing envelope was then evaluated by sitting the patient up and having him chew on a piece of gum with 200-micron articulating paper (Bausch Dental, www.bauschdental.com). All streaks to the linguals of the maxillary centrals and laterals were removed to ensure there was no friction.3,4
Phase II: Restorative
The patient was allowed to fully function with the transitional bonding for a period of 1 month. There was an absence of any symptoms or chipping with the new vertical dimension and incisal length. A Kois face-bow transfer (Panadent, www.panadent.com) was taken to capture and communicate the esthetic considerations of the maxillary arch (Figure 8). Tooth No. 9 was chosen by the patient to be the more acceptable length and was referenced to be the vertical incisal edge position on the face-bow platform (Figure 9). Because the additive equilibration established a mandibular position coinciding with centric relation, it was possible to make jaw relation records in maximum intercusptation using bite registration material (Futar® D Fast, Kettenbach USA, www.kettenbach.us).
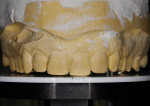
The records, models, and digital photography were sent to the laboratory technician to fabricate a diagnostic wax-up for teeth Nos. 4 through 13 using tooth No. 9 as the reference point to build the esthetics. Although a stable occlusion at the new vertical dimension was established, the anatomical cusp tips of some of the mandibular teeth were unnaturally shaped (Figure 10). Given that the laboratory technician already had the correct functional and esthetic parameters, there was an opportunity to create a more ideal cusp-to-fossa relationship by refining the mandibular cusp tips and adding to the opposing teeth. This helped achieve more esthetic balance and harmony while maintaining the same vertical dimension. Tooth preparation was finished entirely in enamel and restoration margins were supragingival because most of the reduction was in the transitional bonding (Figure 11).
Final impressions were taken using a light body wash and monophase polyvinylsiloxane (Aquasil Ultra®, DENTSPLY Caulk, www.caulk.com ). The provisional restorations were fabricated with a bis-acryl material (Luxatemp®, DMG America, www.dmg-america.com), and the occlusion was verified by using the previously fabricated deprogrammer to ensure equal-intensity, bilateral simultaneous contacts from the canines to first molars. The provisional restorations were used to evaluate tooth form and contour in the smile since the vertical dimension and new incisal edge position had already been established with the transitional bonding. The final porcelain restorations were placed using an adhesively retained bonding protocol. Tooth treatment included microabrasion with 27-micron aluminous oxide with a PrepStart™ (Danville Materials, www.danvillematerials.com) at 40 psi, 35% phosphoric acid for 15 seconds (Ultra-Etch®), and several layers of unfilled adhesive resin (One-Step®, Bisco, Inc., www.bisco.com) applied and light-cured. Internal restoration treatment was done by etching with 35% phosphoric acid and applying silane primer (RelyX® Ceramic Primer, 3M ESPE, www.3MESPE.com). Porcelain restorations were luted with light-cure-only resin (RelyX® Veneer, 3M ESPE) and light “tacked,” excessive cement was removed, and final light cure was applied. The occlusion was refined using the deprogrammer. An upper occlusal splint was made to prevent any damage if parafunction was indeed present (Figure 12 through Figure 15).5-8
At subsequent re-care visits, it was observed that the patient’s full-face photographs showed a decrease in masseter muscle size although the patient maintained the same body weight (Figure 16). The upper occlusal splint, which the patient wears nightly, displayed horizontal tracks that confirmed a diagnosis of parafunction.
Conclusion
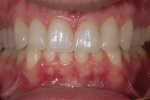
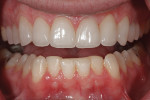
Fulfilling a patient’s esthetic desires may be an end goal, but the treatment plan must always take account of risk assessment, including periodontal, biomechanical, functional, and dentofacial risk. The goal of any restorative plan should be to minimize risk and improve prognosis. The dentofacial requirements in this case were the first to be established using direct composite applied to the incisal edges in a non-invasive approach. The Kois deprogrammer allowed the clinician to find, establish, maintain, and verify an acceptable vertical dimension in centric relation throughout the process. The functional needs and esthetic requirements were met initially through the additive protocols of transitional bonding. This proved valuable to the clinician in that it allowed the newly designed occlusion and smile to be evaluated before commencing the final restorative process. The patient, in turn, benefitted from being able to preview a new incisal length and chewing system before committing to porcelain restorations. Proper communication between the dentist and the laboratory technician was important in order to appropriately satisfy the expectations of the patient. The intra-oral composite mock-up and transitional bonding gave the laboratory technician set parameters from which to build the case esthetically and functionally. The use of the deprogrammer in this case was an integral component for the dentist, patient, and laboratory technician. The biomechanical and periodontal risks were not increased because the tooth preparations were supragingival and remained in enamel. The functional risk was managed but not eliminated. The patient was made aware that his bruxism put him at increased risk for future chipping of the restorations. Nightly use of the night guard will help manage but not eliminate those risks. The final result exceeded the patient’s expectations and was accomplished using a predictable and conservative approach (Figure 17 through Figure 19).
Acknowledgment
The author would like to acknowledge and thank Brad Patrick, BSc, for the ceramic restorations fabricated in this case, and John Kois, DMD, MSD, for his educational instruction through the years.
References
1. Kois JC. Functional Occlusion: Science Driven Management Manual. Seattle, WA: Kois Center; January 2011:79.
2. Bakeman EM, Kois JC. Maximizing esthetics/minimizing risk: the line of predictable success. Inside Dentistry. 2005;1(1):16-24.
3. Kois JC, Philips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1177.
4. Dawson PE. Centric relation. In: Dawson PE. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1989:28-55.
5. Chiche GJ, Pinault A. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994.
6. Rufenacht CR. Principles of Esthetic Integration. Chicago, IL: Quintessence Publishing; 2000.
7. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, IL: Quintessence Publishing; 2002.
8. Terry DA, Leinfelder KF, Geller W, eds. Aesthetic and Restorative Dentistry: Material Selection and Technique. 1st ed. Stillwater, MN: Everest Publishing Media; 2009.
About the Author
Amanda Seay, DDS
Private Practice
Mount Pleasant, South Carolina