Dysfunction Prompts Comprehensive Oral Health Assessment
Christopher Pickel, DDS
Abstract
A patient presented to the clinician’s office as a result of discomfort from a fractured root. A systematic risk assessment revealed a combined periodontal/endodontic lesion associated with tooth No. 2, as well as the patient’s history of orthodontic treatment, periodontal disease, and extensive restorative dentistry. It was also established that the patient was dissatisfied with her smile, which affected her self-esteem. Using a 10-step management system, the clinician was able to not only address the presenting complaint but also discover and treat the patient’s cosmetic concerns. This case illustrates that through proper, comprehensive assessment of oral dysfunction dentists can do more than correct biomechanical and functional problems—they can also improve a patient’s quality of life.
Many patients are not aware of the extent of their dental disease until they have an opportunity to have a methodical and comprehensive analysis of their oral condition. They are usually only motivated to seek their clinician’s advice after experiencing discomfort or when an issue arises that interferes with their quality of life. Given this opportunity, clinicians can utilize the Kois system of risk assessment and risk management to identify the factors contributing to disease and to assist in developing a treatment plan to address those factors. This comprehensive approach enables clinicians to find solutions to problems that influence how patients feel about their oral health, smile, and self-esteem.
Clinical Case Overview
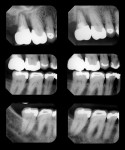
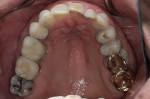
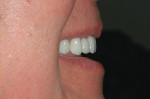
Patient History and Chief Complaint: A 53-year-old woman presented with a chief complaint of low-grade pain in the maxillary right quadrant for a 4-month duration. Radiographic and clinical analysis established a combined periodontal/endodontic lesion associated with tooth No. 2 as the pain source (Figure 1). The patient was previously diagnosed with periodontal disease and placed on a 4-month recare schedule, but her visits were intermittent.
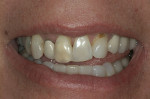
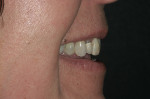
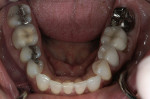
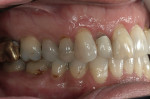
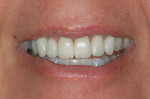
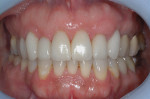
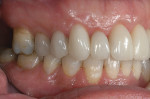
After further discussion, she revealed that she had always been unhappy with the appearance of her smile and was very self-conscious about it (Figure 2 and Figure 3). She had undergone orthodontic treatment in her late 30s and was never satisfied with the esthetic outcome. She agreed to a comprehensive assessment to evaluate her condition and discuss her options.
The patient’s dental history included many years of restorative work that was satisfactory to her from a comfort perspective. However, she was displeased with the appearance of some of the restorations. She reported a family history of periodontal disease and that she was of Hispanic descent. Bone loss, mainly in the maxillary posterior quadrants, was noted. She had active caries, a significant amount of existing restorative treatment, and multiple areas of cervical abrasion/erosion. Minor orthodontic relapse was noted.
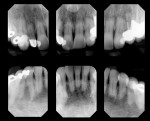
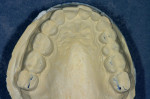
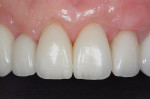
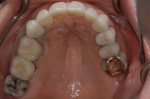
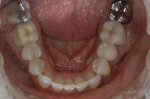
Tooth Nos. 10, 12, and 25 were missing, and tooth No. 7 was a peg lateral incisor restored with a porcelain-fused-to-metal (PFM) crown. The missing teeth had not been replaced, and the spaces were consolidated orthodontically (Figure 4 and Figure 5). The anterior teeth exhibited moderate root resorption from orthodontic treatment, resulting in less favorable crown-to-root ratios but minimal mobility. She stated that she had multiple bites and a difficult time chewing.
Diagnostic Findings
Periodontal: Periodontal pocket depths measured 2 mm to 3 mm in the anterior sextants, and 2 mm to 5 mm in the posterior. Radiographically, generalized mild to moderate horizontal bone loss of between 1 mm and 3 mm was visible. Tooth No. 2, the source of the chief complaint, exhibited circumferential bone loss, with probing depths of 6 mm to 9 mm, secondary occlusal traumatism, and a suspected vertical root fracture. A periodontal diagnosis of AAP type III was made. Recession and abrasion were present on most of her maxillary teeth and the posterior mandibular teeth. This likely resulted from an aggressive toothbrush habit and predisposing anatomy.1 Apical root resorption was noted on tooth Nos. 7 through 9, 11, 23, 24, and 26 (Figure 6).
Risk: Moderate
Prognosis: Good (hopeless for tooth No. 2 only)
Biomechanical: The examination revealed active caries interproximally on tooth No. 5 and cervical caries on tooth Nos. 19 and 28 through 30. Tooth Nos. 5 through 8 and 20 had defective restorations. Tooth Nos. 3, 11, 28, and 29 had questionable restorations, and tooth Nos. 2 through 7, 13 through 16, 18 through 20, 29, and 30 were structurally compromised due to the size of their current restorations (Figure 7 and Figure 8).2 Of particular note was the stained erosion on tooth Nos. 5, 6, 8, 11, 29, and 30 (Figure 9). The patient admitted to drinking six cans of diet cola and 2 to 4 cups of sugared coffee per day, and she reported episodic xerostomia. In addition, the root canal treatment on tooth No. 2 was failing.
Risk: High
Prognosis: Fair (hopeless for tooth No. 2 and teeth with untreated decay: Nos. 5, 19, and 28 through 30).
Functional: The majority of the unrestored teeth exhibited minimal attrition. Moderate wear was noted on tooth No. 29. Joint sounds and joint loading findings were negative, and muscle palpations were all within normal limits. Maximum opening was 46 mm. The patient demonstrated an acceptable range. Primary occlusal traumatism (+1 mobility) was noted on tooth Nos. 8, 9, 23, 24, and 26 due to the compromised crown-to-root ratio from apical resorption. Secondary occlusal traumatism (Class 2 mobility) was present on tooth No. 2. The cephalometric tracings indicated a Class 2 skeletal relationship, with a slightly retrognathic mandible, increased lower face height, and upright incisors. The upright interincisal angle may have resulted from orthodontic space consolidation due to missing tooth Nos. 10 and 12.
While the exact diagnosis was not initially clear, it was evident the patient had unacceptable function. Based on positive answers to the dental history (eg, her perception of multiple bites and difficulty chewing challenging foods), the initial impression was a diagnosis of occlusal dysfunction. The patient wore a Kois deprogrammer for 4 weeks to make a definitive functional diagnosis. After deprogramming was confirmed, the initial tooth-to-tooth contact was determined to be on a posterior tooth, and a diagnosis of occlusal dysfunction was made.
Risk: Moderate
Prognosis: Fair
Dentofacial: Due to the medium lip dynamics of the maxillary arch and the patient’s dissatisfaction with her smile, dentofacial risk was deemed moderate. Complicating factors included the ectopic position of tooth Nos. 11 through 15 (No. 11 in No. 10 space, No. 13 in No. 11 space, No. 14 in No. 12 space, No. 15 in No. 13 space, etc).3 This arrangement contributed to gingival tissue asymmetries and an uneven maxillary occlusal plane. Tooth No. 8 exhibited significant discoloration and hypocalcification. Although the patient’s dysmorphic lip and chin could not be changed, corrections to the teeth and gingiva offered significant opportunities for an improved smile.
Risk: Moderate
Prognosis: Fair
Medical: The patient’s medical history included a history of thyroid cancer. Her thyroid was removed at age 21, but she required multiple surgeries to treat recurrent pathology from age 21 to 35, resulting in damage to her vocal cords. She had been in remission since age 35. She also had a dysmorphic chin, neck, and lower lip from these surgeries (Figure 10). Her salivary flow rate was slightly compromised, and she reported episodes of dry mouth. Her medications were levothyroxine and hormone replacement therapy. She smoked a half a pack of cigarettes per day from ages 16 through 25. Her remaining medical history was insignificant. She was classified as ASA 2 due to her thyroid condition.
Risk: Moderate
Prognosis: Good
Treatment Goals
Treatment goals included improving periodontal health and treating decay and defective restorations, as well as the clinician’s instituting a preventive regimen with a caries management program and diet counseling. Additional goals included reducing functional risk by treating the occlusal dysfunction and addressing the patient’s dissatisfaction with her smile by altering gingival contours, tooth shape, and position.
Treatment Plan and Phases
Two options were presented to the patient. Both would address the chief complaint, as well as all the functional, biomechanical, and esthetic concerns that had been identified through the history and clinical examination.
Option A: This option included orthodontic treatment to move her anterior teeth into more ideal locations to facilitate proper anatomical form and tooth location. Specifically, tooth Nos. 11 through 15 would be moved distally to place No. 11 back in an ideal arch location, establish Class 1 cuspid occlusion, level the maxillary occlusal plane to minimize the lip dysmorphia, and create a space to restore the missing No. 10 with an implant. In addition, tooth Nos. 5 through 11 would be restored with porcelain crowns, and tooth No. 16 would be extracted.
Option B: In this restorative-only approach, the gingival asymmetry would be corrected with periodontal surgery. Tooth Nos. 5 through 13 would be restored with porcelain crowns, and length would be added to tooth No. 13 to correct the maxillary occlusal plane. The teeth would also be prepared with minimal reduction in order to avoid increasing the biomechanical risk.
Eager to begin treatment, the patient selected Option B. This plan would address her esthetic concerns, but would lower risk only in the biomechanical and functional categories.
Phase I: Extraction, Periodontal Surgery, Caries Control
An occlusal record was made of the deprogrammed centric relation position.4 The casts were mounted to that record, and the first point of contact was tooth No. 2 (Figure 11). This tooth was extracted and a vertical root fracture was verified. A socket-preservation technique was applied, and the site was grafted for future implant placement. The occlusion was reevaluated after tooth No. 2 was removed by taking new impressions and mounting them to the deprogrammed bite registration. The resulting mounting indicated that very little occlusal adjustment was necessary to establish an even-intensity, simultaneous contact of the posterior teeth (P2).
Four quadrants of scaling and root planing were completed. Local chemotherapeutics were used in two posterior quadrants that exhibited 5-mm probing depths.5 A recare appointment 4 months later revealed complete resolution of bleeding on probing and a generalized reduction in pocket depths.
The patient was referred to her physician to determine if gastric reflux was a contributing factor to the erosion. Test results for gastric reflux were negative, thereby reducing the probability of intrinsic causes as the source of the erosion. Extrinsic dietary acids were determined to be likely contributors to the erosive lesions.6-8 A reduction or elimination of soda and coffee consumption was recommended. The patient agreed to comply, and within a month noted increased salivary flow.
A caries management program was also implemented, which consisted of fluoride varnish applications at restorative and hygiene visits, home use of an alkaline pH rinse (CariFree® Treatment Rinse, Oral BioTech, www.carifree.com), a fluoride rinse (CariFree® Maintenance Rinse, Oral BioTech),9,10 and a casein phosphopeptite (CPP) and amorphous calcium-phosphate-fortified paste (MI Paste™, GC America Inc., www.gcamerica.com) to remineralize the erosive areas. No saliva substitute was necessary.
All carious lesions were removed from tooth Nos. 5, 19, 20, and 28 through 30, and the teeth were restored with composite restorations. Foundation restorations were placed in tooth Nos. 5, 6, and 20.
Phase II: Equilibration and Crown Lengthening
Based on the findings of the functional analysis, a full-mouth equilibration was completed to achieve equal-intensity bilateral contacts on posterior teeth (the cuspids would be captured later with definitive restorations on the anterior teeth). Vertical dimension remained unchanged.
The clinical crown lengths of tooth Nos. 5 through 13 were asymmetrical. The ectopic position of the teeth was the primary cause. A diagnostic wax-up was fabricated to simulate ideal tooth length/shape and arch form. Of note, tooth No. 7 was 8.5-mm long while tooth No. 11 (which was in the No. 10 location) was 11.5-mm long. A periodontist performed crown lengthening on tooth No. 7 and a connective tissue graft on No. 11 to establish symmetry and reduce the 3-mm discrepancy. The remaining tooth length discrepancies would be addressed with restorative correction. After a 2-month healing period, the patient was ready for restorative treatment.
Phase III: Wax-Up, Provisionalization, Definitive Restorations
A diagnostic wax-up to guide the periodontist in leveling the gingival tissues was made prior to periodontal surgery. The wax-up was designed using steps 1 through 5 of the Kois 10-Step Management System (www.koiscenter.com). While none of the patient’s existing maxillary teeth were positioned ideally, tooth No. 9 was closest to being in an ideal position. Alterations to tooth No. 9 to achieve the desired tooth contours and position included lengthening the tooth by 0.5 mm and moving it labially by 0.5 mm and axially to the left by 0.5 mm. The remaining anterior teeth were then placed in an ideal arch form relative to the position, shape, and contours established for tooth No. 9. Crowding, rotations, and overlap were corrected. The maxillary occlusal plane was leveled appropriately. The mandibular incisal edge and occlusal plane were acceptable, therefore no changes were planned.
Tooth Nos. 5 through 13 and 20 were prepared for lithium-disilicate ceramic crowns. With the exception of tooth Nos. 8, 9, and 11, all teeth had previous and extensive restorations. Tooth Nos. 5 through 7, 11 and 13 were restored with core-supported restorations. Tooth No. 11 would also be core-supported due to the reduction required to make it the size and shape of a lateral incisor. Tooth Nos. 8 and 9 had minimal existing restorations and were prepared for adhesively supported enamel restorations. The cervical limitations of intracrevicular tooth preparations and gingival management were concerns due to the differing crest types across the anterior segment.11,12
With the exception of tooth Nos. 7 and 11, all teeth had normal crests. Crown lengthening on tooth No. 7 created a high crest, and the connective tissue graft on tooth No. 11 created a low crest. The coronal limits of the restorative margin locations were different for each crest type. The coronal limit for tooth No. 7 was less than 0.5-mm apical to the free gingival margin. The coronal limit for tooth No. 11 was at the free gingival margin. The remaining teeth had a normal crest, with a coronal limit of 0.5-mm to 1-mm apical to the free gingival margin.13
Final impressions and occlusal registrations were made. Provisional restorations fabricated from the wax-up were seated and equilibrated. An impression of the provisionals and occlusal registration also was taken 1 week later.
The restorations for tooth Nos. 5 through 13 and 20 were seated 4 weeks later (Figure 12 and Figure 13). All units except for tooth Nos. 8 and 9 were seated with a cohesive protocol using self-adhesive resin cement (RelyX™ Unicem, 3M ESPE, www.3MESPE.com) (Figure 14 and Figure 15). Tooth Nos. 8 and 9 were seated with an adhesive protocol using a one-step dental adhesive (ONE-STEP®, Bisco, Inc., www.bisco.com) and adhesive resin cement (RelyX™ ARC, 3M ESPE) (Figure 16 ). Occlusion was adjusted, resulting in cuspid coupling and very light lateral and central contacts in maximum intercuspation.(Figure 17). Anterior guidance was unchanged and established with cuspid disclusion of the posterior teeth in functional excursions.
Four weeks after seating all the units, occlusion was again evaluated. It was noted that the mobility that existed preoperatively on the anterior teeth was reduced. Tooth Nos. 8, 9, and 26 demonstrated improved stability (Figure 18 and Figure 19 ).
Conclusion
Had it not been for dysfunction, this patient might not have undergone these life-changing improvements to her smile. She had been dissatisfied with her appearance for many years and assumed significant improvements were unattainable. Discomfort from a fractured root, likely the result of occlusal dysfunction, provided the opportunity to utilize the Kois Diagnostic Opinion Criteria to comprehensively evaluate all aspects of oral health and educate the patient about possibilities of which she was previously unaware. The patient was provided with the opportunity to not only reduce disease and discomfort, but also reduce the distress created by her esthetic concerns.
Utilizing the 10-Step Management System also simplified the treatment-planning phase for the treating dentist. The patient’s problems were explored to a deeper level, after which they were addressed in a meaningful way that was relevant to the patient. This case illustrates how dentists can reduce biomechanical and functional risk, feel good about that accomplishment, and change a patient’s quality of life.
Acknowledgment
The author would like to thank Bobby Butler, DDS, Seattle, Washington, for performing the esthetic periodontal therapy, and Leon Hermanides of Protea Dental Studio, Redmond, Washington, for laboratory services.
References
1. Dzakovich JJ, Oslak RR. In vitro reproduction of noncarious cervical lesions. J Prosthet Dent. 2008;100(1):1-10.
2. Fan P, Nicholls JI, Kois JC. Load fatigue of five restoration modalities in structurally compromised premolars. Int J Prosthodont. 1995;8(3):213-220.
3. Arnett GW, Gunson MJ. Facial analysis: the key to successful dental treatment planning. J Cosmet Dent. 2005;21(3): 20-33.
4. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. J Cosmet Dent. 2006;21(4):96-102.
5. Greenstein G. The efficacy of minocycline microspheres in the treatment of chronic periodontitis: statistical vs clinical significance. Compen Contin Educ Dent. 2003;24(2):121-133.
6. Lussi A, Hellwig E, Ganss C, Jaeggi T. Buonocore Memorial Lecture. Dental erosion. Oper Dent. 2009;34(3):251-262.
7. Auad S, Moynihan P. Diet and dental erosion. Quintessence Int. 2007;38(2):130-133.
8. von Fraunhofer JA, Rogers MM. Dissolution of dental enamel in soft drinks. Gen Dent. 2004; 52(4):308-312.
9. Kutsch VK. Dental caries: A new look at an old disease. Inside Dentistry. 2009;5(5):60-65.
10. Marsh PD. Dental plaque as a biofilm: the significance of pH in health and caries. Compend Contin Educ Dent. 2009;30(2):76-88.
11. Kois JC. Altering gingival levels: the restorative connection part 1: biologic variables. J Esthet Dent. 1994;6(1):3-7.
12. Kois JC. The restorative-periodontal interface: biological parameters. Periodontol 2000. 1996;11:29-38.
13. Günay H, Seeger A, Tschernitschek H, Geurtsen W. Placement of the preparation line and periodontal health—a prospective 2-year clinical study. Int J Periodontics Restorative Dent. 2000;20(2):171-181.
About the Author
Christopher Pickel, DDS
Private Practice
North Seattle Dental
Seattle, Washington