Buccinator Muscle Repositioning: A Case Report
Om N. Baghele, MDS, MBA; and Mangala O. Baghele, BDS
Abstract
Anatomical abnormalities are frequently associated with problems. One such abnormality is crestal attachment of the frenum or muscle on the alveolar process. Crestal attachment of buccinator muscle is a rare phenomenon. It may cause various problems in routine oral exercises or restoring the edentulous area. Presented here is a case of abnormal buccinator muscle attachment, which was relocated apically by surgical means using an acrylic stent. The healing was uneventful, and significant apical repositioning was observed. The area was then considered for prosthodontic therapy. A fixed bridge was fabricated and the long-term results of the fixed bridge therapy were assured, because the patient could maintain oral hygiene well after the muscle repositioning operation.
A healthy periodontal complex is one capable of withstanding the stress of mastication, toothbrushing, trauma from foreign objects, tooth preparation associated with crown and bridge, subgingival restorations, orthodontics, inflammation, and frenulum pull.1 A frenum is a small band or fold of mucosal membrane that attaches the lips and cheeks to the alveolar process and limits their movements.1 Similarly, muscle attachments near the crest of the alveolar bone in edentulous areas or near the marginal tissues in dentate areas may create problems mimicking those of high frenal attachments.
Cohen1 suggested that the frenulum must always be removed when it is so thick and wide that it may interfere with toothbrushing. For the same reason and also for the purposes of appropriate prosthodontic management, coronally attached muscles may require apical repositioning.
The buccinator muscle may pose problems similar to thick, wide, and crestally attached freni in the region of molars near its origin over the maxilla and mandible. The buccinator muscle is a plain, square-shaped bilateral mimic muscle, which composes the mobile and adaptable portion of the cheek. It is frequently referred to as an accessory muscle of mastication because of its role in chewing food and swallowing and compressing the cheeks against the molars, as well as its use for whistling, sucking, and blowing.2
The orbicularis oris, buccinator, and superior constrictor muscles functionally perform as a unit in the acts of swallowing, blowing, sucking, pronouncing vowels, chewing, and coughing. The buccinator and orbicularis oris play a definite role in beginning the process of swallowing by producing a peristaltic-like wave of contractions originating in the oral cavity and passing pharyngeally. The buccinator usually initiates the sequence followed quickly by the orbicularis oris.3 Kang et al4 have also described a tentative physiological role, suggesting that the buccinator and orbicularis oris act as a dilator of the duct for the buccinator muscle fibers, which extend to the terminal portion of the parotid duct.
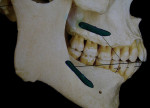
Buccinator muscle arises from the molar portion of the alveolar process of the maxilla, the buccinator crest of the mandible, and the pterygomandibular raphe of the bucco-pharyngeal fascia. The fiber bundles of the muscle are divisible into four sets, all of which extend into the orbicularis oris. The pterygomandibular raphe connects the anterior portion of the superior constrictor muscle of the pharynx with the posterior portion of the buccinator. From the two bone origins (buccal alveolar bone of maxillary and mandibular molars [Figure 1]) and from the pterygomandibular raphe, the fibers of the buccinator muscle run anteriorly, forming the musculature of the cheek.2
Not infrequently, abnormal muscle attachments, such as the buccinators, cause problems in the form of oral hygiene maintenance, proper prosthodontic management, restricted lip and cheek movement, and difficulties in mastication and phonation. One such case with high buccinator muscle attachment causing difficulties in local oral hygiene maintenance and fixed bridge therapy is reported here. Because of various important functions, the muscle cannot be resected, like frenectomy, but it can be repositioned apically.
Case Report
A 30-year-old female patient was referred to the Department of Periodontology for consideration and management of a mandibular partial edentulous area having high muscle attachment. The patient was being considered for a fixed bridge for missing mandibular left first and second permanent molars (teeth Nos. 18 and 19). The high muscle attachment was considered to be an impediment for proper prosthetic management and oral hygiene. The patient’s main concerns were difficulty in chewing food because of the absence of teeth and “restricted” movements of the cheek in the concerned area.
Examination
On examination, the patient was a well-built, adequately nourished, well-oriented, and mentally sound adult. The medical history was noncontributory and no extra-oral abnormalities were noted. The patient did not indulge in alcohol or tobacco.
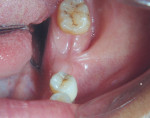
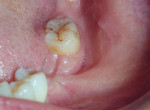
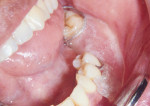
Intraoral examination showed good oral and periodontal hygiene. Teeth Nos. 18 and 19 were missing, and the reason for extraction was decayed teeth. The height and width of the edentulous ridge was maintained. On retracting the cheek, the authors observed a frenum-like band of soft tissue attached at the crest of the edentulous ridge. Closure examination, anatomic reference points, and the nature of attached tissue revealed that it was the buccinator muscle whose attachment was abnormal. The attachment (origin) extended to the crest of the alveolar ridge. The vestibular fornix (depth) was almost nonexistent in that area (Figure 2 and Figure 3).
The muscle was actually impeding the movements of the toothbrush, leading to suboptimal oral hygiene. The attachment would have definitely created a space problem for the pontics and an area of food impaction, further worsening the situation. A decision to reposition the attachment apically was undertaken. Discussed with the patient were treatment options such as fenestration surgery, apical repositioning with free gingival grafts, ‘frenectomy’ plus free gingival grafts, and apical repositioning with an acrylic stent. The patient accepted the last option and gave written consent.
Investigations
Routine hematological investigations were carried out and were within normal limits.
Treatment
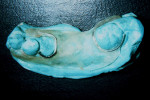
An irreversible hydrocolloid (alginate) impression of the lower arch was taken and a cast made in gypsum. It was decided to construct an acrylic surgical stent, as a periodontal dressing would have not stayed in proper apical position due to counteracting forces created by muscle activity. Approximating the anticipated loss of tissue resulting from the surgical procedure, the cast was marked and scored to ensure close contact of the stent with the alveolar ridge (Figure 4). A passive fit of the stent was checked in the patient’s mouth, and final adjustments were accomplished (Figure 5). The stent was then smoothed and highly polished to minimize the accumulation of biofilms.
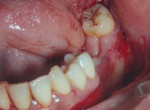
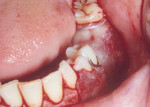
Under local anesthetic (2% lignocain with 1:80,000 epinephrine) to obtain a localized field block, a crestal incision was performed, keeping the incision slightly buccal. The incision was extended anteriorly two to three teeth and posteriorly distal to the last molar. The muscle attachment was detached from the crest and dissection was continued inferiorly for approximately 1.5 cm to 2 cm. Deeper to that, the dissection continued apically while keeping the periosteum intact (split-thickness). The achieved vestibular depth and muscle repositioning was checked by retracting the cheek (Figure 6). After adequate depth was achieved, the area was irrigated, the hemorrhage controlled, and the surgical stent stabilized in place (Figure 7).
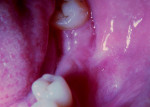
Written postoperative instructions were provided, and a course of amoxicillin 500 mg t.i.d. and paracetamol 625 mg t.i.d. was given for 5 days. The stent was retained in position for 15 days to allow complete healing with regular irrigations and oral hygiene instructions. The area healed uneventfully. After 2 months of healing (Figure 8), there was significant gain in vestibular depth, and the muscle was relocated to an apical position, thus allowing the toothbrush head to be positioned properly for maintenance of proper oral hygiene. The final fixed prosthesis was delivered after 3 months of healing.
Discussion
The three most common indications for apical extension of vestibular depth are5: frenal or muscle attachments in close proximity to the marginal gingiva or alveolar crest; approximation of the gingival margin and mucogingival junction following gingivectomy or gingival recession; and deep periodontal pockets whose apical extension is at or apical to the mucogingival junction.
Vestibular alterations in the mandibular molar area, because of abnormal buccinator attachment, may be required for proper oral hygiene maintenance or for prosthetic reasons.
In premolar and molar areas, it is not uncommon to find a shortened vertical height of alveolar bone with a high mucobuccal fold due to the level of attachment of the buccinators muscle. A frenectomy results in the formation of a shallow vestibule. The procedure of choice in these cases is a combination of frenectomy and vestibular extension.5
It was not clear whether the coronal attachment was pre-extraction (because of shallow vestibule due to high external oblique ridge) or if it developed after extraction of the involved teeth. Development of a shallow buccal vestibule following extraction may have several causes:
• loss of vertical ridge height during traumatic extractions
• loss of soft tissue and improper suturing (coronal pulling) during extraction
• horizontal loss of alveolar ridge due to periodontal diseases compounded by bone loss during extraction
• disuse atrophy, because of loss of functional stimulation
• a combination of the above causes
Research addressing vestibular extension using various surgical techniques has produced differing results. Bohannan6-8 reported shallowing out of the vestibule in all cases for vestibular extensions regardless of the technique employed. For Bohannan’s “complete denudation” technique,6 approximately 45% of the operative extension was retained at the end of the 26-week period of the study. Of the 55% of the operative extension lost during the healing process, practically all (90%) loss occurred within the first 4 post-operative weeks.6 Also, he noted that 50% of original gain in vestibular depth was lost over the 6 months post-surgical healing unless the fenestration technique was accomplished.8 As the majority of the operative extension is lost during the first month, the results of the present case at the end of 3 months may indicate initial stability. The results of this isolated case may not be appropriate to compare with other studies, as the observation period is short, and over time the authors may expect shallowing out of the achieved vestibular depth. The positive results of this case may also be attributed to the rigid acrylic stent used, which prevented any early coronal migration or displacement of the flap. Ochsenbein9 reported that the vestibular fornix cannot be increased in depth on a predictable basis. Corn’s10 observations were more positive; he reported a greatly increased zone of attached gingiva and that the mucogingival junction was positioned more apically. The greatest permanent increase in depth of the fornix followed complete denudation of the fibrous periosteum from the alveolar margin to the base of the deepened vestibule.
In the current case report, the posterior mandible is a difficult site for vestibular extension. As noted by Bradin,11 “any area which forms broad shelf-like projections in the mandible on the labial or buccal surfaces hinders the amount of attached gingiva and vestibular extension, unless extensive bony reshaping is done. The most common site is the external oblique ridge area about the second and third molar and next commonly the midline of the mandible. In these areas one has to be content with a shallow vestibule and about 1 mm or 2 mm of attached gingiva.”
A surgical acrylic stent was used in this case for long-term retention and proper stabilization. As Bradin11 also noted, “for vestibular extensions to be successful, pack should be in position for at least 3 weeks. Many cases fail because packs cannot be maintained.” The pack should be maintained at the extended apical depth that is required to obtain the desired outcome. Desired results are frequently compromised by occlusal displacement of soft packs during the polymerization process. Aids in pack retention such as wire ligature, copper bands, or stents can be employed.
Conclusion
Alterations of the vestibule and mucobuccal fold are valuable adjuncts in periodontal-prosthetic management. Appreciation, understanding, and proper utilization of recommended procedures will definitely contribute to more favorable and lasting results. Apical repositioning of an aberrant muscle attachment will preserve all important functions of the muscle as well. Instead of restoring suboptimal edentulous areas, which may complicate future hygiene maintenance, pre-prosthetic surgeries should be considered to achieve appropriate ridges for restorations.
References
1. Cohen ES. Atlas of Cosmetic and Reconstructive Periodontal Surgery. 3rd ed. Hamilton, Ontario, Canada: BC Decker Incorporation; 2007:45-85.
2. D’Andrea E, Barbaix E. Anatomic research on the perioral muscles, functional matrix of the maxillary and mandibular bones. Surg Radiol Anat. 2006;28(3):261-266.
3. Perkins RE, Blanton PL, Biggs NL. Electromyographic analysis of the “buccinator mechanism” in human beings. J Dent Res. 1977;56(7):783-794.
4. Kang HC, Kwak HH, Hu KS, et al. An anatomical study of the buccinator muscle fibers that extend to the terminal portion of the parotid duct, and their functional roles in salivary secretion. J Anat. 2006;208(5):601-607.
5. Rosenberg MM. Vestibular alterations in periodontics. J Periodontol. 1960;31:231-237.
6. Bohannan HM. Studies in the alteration of vestibular depth. I. Complete denudation. J Periodontol. 1962;33:120-128.
7. Bohannan HM. Studies in the alteration of vestibular depth. II. Periosteum retention. J Periodontol. 1962;33:354-359.
8. Bohannan HM. Studies in the alteration of vestibular depth III. Vestibular incision. J Periodontol. 1963;34:209-215.
9. Ochsenbein C. Newer concepts of mucogingival surgery. J Periodontol. 1960;31:175-185.
10. Corn H. Periosteal separation: its clinical significance. J Periodontol. 1962;33:140-153.
11. Bradin M. Precautions and hazards in periodontal surgery. J Periodontol. 1962;33:154-163.
About the Authors
Om N. Baghele, MDS, MBA
Professor
Department of Periodontology and Oral Implantology
SMBT Dental College and Hospital
Sangamner, Maharashtra, India
Mangala O. Baghele, BDS
Private Practice
Mumbai, Maharashtra, India