Composites and Whitening: How and When to Combine Treatments
Gerard Kugel, DMD, MS, PhD; Susana Ferreira, DDS; and Ronald Perry, DMD, MS
Abstract
Given the objective of today's conservative dentistry to save tooth structure, it is common to combine direct composite restorations and tooth whitening to achieve esthetically pleasing clinical results that also limit the necessity for prosthodontic tooth preparation. Clinicians must consider, however, that with whitening and composites, a certain methodology is necessary to prevent potential failure inherent to this combination. Addressing issues ranging from concerns over loss of tooth structure to lack of funds for prosthodontic work, direct composites and whitening are logical and ideal treatment options dentists can recommend for numerous patients. The authors present one such case study to demonstrate the benefits that are possible when such a course of treatment is properly performed.
Dental research shows the bond strengths of adhesives to bleached hard tissues can be temporarily reduced in some cases.1 The literature states that surface softening and roughening of restorative materials is a concern, particularly in composite.2 However, in this age of the popular concept of conservative dentistry to save tooth structure, it has become very common to combine direct composite restorations and tooth whitening to achieve an esthetic clinical result while limiting the need for prosthodontic tooth preparation.3 In order to marry the two principles—the benefit of combining whitening and composite restorations with the potential for surface degradation in doing so—for ideal treatment and case planning, clinicians should use an evidence-based approach to esthetic treatment.
It is important for clinicians to understand why methodology is important for the use of whitening and composites in clinical practice. Industry researchers studied bond strengths incessantly over the last 15 years, which led to the modification of products, systems, and techniques for the betterment of dentistry. It is of clinical importance not to undermine that progress with whitening materials, which are intended to enhance dental practitioners' work, not hinder it.
The reduction in composite bond strength to bleached dentition can be attributed to several factors; some are considered common knowledge among dentistry's clinical peers while others are more esoteric to research circles. The former is comprised of the following: residual oxygen often inhabits the enamel and dentinal pores post-bleaching; once liberated, the oxygen molecules could prevent adequate resin infiltration into dentin and enamel4 and/or inhibit resin polymerization of those that cure using free-radical mechanisms.5 The ultimate result could be debonding of the restorative material due to a soft interface between hard tissues and composite caused by oxygen-inhibited polymerization.6
The latter factors, often not discussed in clinical lectures or literature, relate to changes in enamel morphology that weaken bond strengths subsequent to whitening. Hydrogen peroxide and its releasing agents may result in decreasing levels of enamel calcium and phosphate in addition to changes in form and structure of the most superficial crystallites in enamel.7 The clinical consequence of these factors is not only potential debonding, but also an enamel surface that appears over-etched; bleached enamel submitted to acid etching produces a deficit of prismatic form, leaving the restoration less esthetic than intended.8 It is important to note that the potential negative effects of whitening on restorative materials are not limited to the surface of a tooth; layers beneath the surface are equally at risk. Polishing the bleached surface of an adhesive material may not suffice to reinstate the physical properties of the fillings.9
Clinically, it is imperative to incorporate the potential risks to new restorations into treatment planning to stave off clinical failure, patient dissatisfaction, and their corollary relationship to the economic consequences of redoing composite restorations. The literature is rife with studies suggesting a lapse between the completion of whitening therapy and the placement of composites (and orthodontic brackets). Since adhesion of resin to bleached enamel is compromised for up to 14 days after bleaching, a two- to three-week waiting period is suggested.10 Furthermore, the necessity to avoid bonding to older composite restorations is commonly understood.
The following case outlines a series of restorations provided to a patient who presented in the clinic at Tufts University School of Dental Medicine in Boston. The authors, utilizing a team approach to diagnosis, decided to restore the patient's mouth in stages using a combination of caries control, whitening, direct composites, and single crowns. The authors elected to perform the dental procedures at a price point well below the affordability of the patient in order to make a case study of his condition and restorations. The patient understood the ramifications of treatment, as well as the alternatives to the therapies proposed in the treatment plan.
Clinical Case
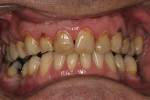
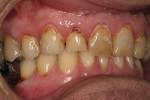
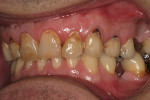
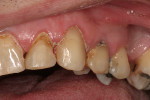
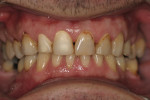
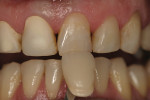
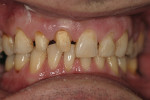
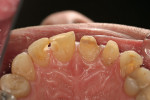
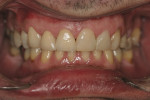
The patient was a 40-year-old male with no medical contraindications to treatment. The patient underwent a comprehensive examination and full-mouth set of radiographs for screening purposes (Figure 1, Figure 2, Figure 3). The authors found generalized rampant decay with a more profound incidence on the maxillary arch. Immediate caries control was deemed necessary in order to allow the patient to start whitening at home as part of his overall treatment plan. The authors decided on an initial treatment plan for the maxillary arch consisting of the following: crown teeth Nos. 7 and 8 and restore teeth Nos. 11 and 12 immediately for caries control; let the patient whiten for a period of 10 days; allow the patient to wait for two weeks before doing cervical composites on teeth Nos. 5, 6, 9, 10. Pending finances, the posterior teeth and the mandibular arch were relegated to phase two of the patient's treatment plan.
Teeth Nos. 7 and 8 were prepared and provisionalized for zirconia restorations. At the time of the initial visit, the average tooth shadea on the maxillary anterior teeth was determined to be A3.5 in value order. Anticipating effects from whitening, a temporary crown shade of A2 was selected. This same shade was chosen for the composite material on teeth Nos. 11 and 12.
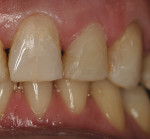
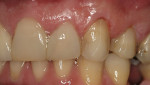
Tooth No. 11 was treated for cervical decay using a Class V composite preparation (Figure 4). The tooth was etched with an etchantb and bonded with a bonding agent,c then restored with an A2 shaded enamel composite.d Tooth No. 12 had a pre-existing MOD composite restoration with marginal leakage and was described as uncomfortable by the patient. Also, a Class V preparation was necessary to restore the decay in the cervical area. Both restorations on tooth No. 12 were placed using the same armamentarium as tooth No. 11. All composites were finished using a finishing bure and polished with a polishing kit.f
At that initial visit, the patient was prescribed a 10-day treatment of a take-home whitening system and an over-the-counter sensitivity dentifrice. This type of whitening was chosen due to the gratis nature of the case and the product's particular convenience because it afforded the patient an opportunity to skip a visit to receive whitening trays in an already taxing clinical appointment schedule.
After five days of whitening, the patient presented for a coping try-in for the anterior crowns (Figure 5). At that visit, the patient complained of extra sensitivity on teeth Nos. 9 and 10. It was hypothesized that the cause of this sensitivity was two-fold: many carious lesions and transient sensitivity common in whitening; examination excluded pulpal involvement. The clinicians agreed on the need for caries control using immediate composites on those two teeth (Figure 6). The temporary restorations were placed using the previously utilized shade A2 enamel composite, with the expectation that the composites would be redone at the crown insertion appointment so that shade matching among the anterior teeth would be possible (Figure 7).
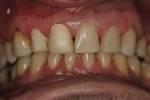
The patient resumed whitening for another five days to complete the full treatment (Figure 8). Two weeks after completing the home whitening, the patient returned to the school for shade selection of the anterior crowns. It was important to wait for the teeth to rehydrate because a slight relapse in color is expected immediately after external whitening.11 An average shade of A2 was selected for the crowns, with some variations in the hue and chroma at different points on the body of the crowns (Figure 9). The composite restorations were not placed on this date because the final crowns—needed for use as a reference to match the anterior composites—were not finalized.
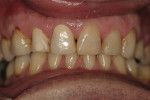
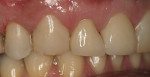
Three days later, after an expedited laboratory fabrication, the crowns for teeth Nos. 7 and 8 were cemented, composites on teeth Nos. 9 and 10 were replaced, and a pre-existing defective restoration on tooth No. 6 was removed and the tooth was restored (Figure 10 and Figure 11). The authors were comfortable with this treatment date given the two-week span necessary to maximize the adhesion of the new resin to the bleached enamel. The crowns were placed into the mouth without cement initially to facilitate shade matching and contouring of the adjacent composites. Both composite restorations on teeth Nos. 9 and 10 were placed using an etchant,b a bonding agent,c and A2 dentin shade of composited on the cervical margin; an A1 enamel shade of composited was layered over the cervical and onto the body toward the incisal edge. The incisal was restored using a custom medium translucent shade of composite.d The composite restorations were finished with the burse and polished with a polishing paste.f
At this visit, the needs of tooth No. 5 were addressed in order to remove the cervical and mesial decay, and in tooth No. 6, which had cervical decay and a pre-existing distal/lingual defective restoration. These teeth were restored using the same etchant and bonding agent as the previous teeth, and the authors layered shade A2 dentin composited on the cervical margin and an A2 enamel shaded on the remainder of the affected area. These teeth were finished and polished in the same manner.
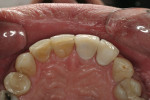
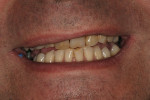
At that point, the crowns were inserted and the patient was instructed to return in one week for observation (Figure 12, Figure 13, Figure 14 and Figure 15). The patient expressed overwhelming satisfaction with the results and is expected to return for further treatment on the mandibular arch (Figure 16 and Figure 17).
Conclusion
Studies evaluating the effects of whitening therapies on hardness and morphology of dental restorative materials are prevalent. Although the results of the numerous trials vary regarding the scope and severity of the effects, most researchers and clinicians agree that some deleterious outcomes are possible, if not probable. A conservative strategy for esthetic dentistry, a combined treatment of whitening and composite restorations may be ideal for many patients. Dentists must keep in mind that with whitening and composites, a certain methodology is necessary to ensure against potential failure inherent to this combination. Addressing issues ranging from concerns over loss of tooth structure to lack of funds for prosthodontic work, direct composites and whitening are logical and ideal plans for many patients.
In this case study, the authors admittedly only have begun to restore this patient to optimum function and esthetics; posterior maxillary teeth and the full mandibular arch still must be addressed. The patient will be monitored at Tufts University School of Dental Medicine on an ongoing basis. The authors understand that crown and bridge procedures may be a likely outcome in the future, but consider their treatment plan ideal for this individual patient at this point in time.
As a team, the authors had several discussions over the sequencing and timing of the different treatment steps in this plan. Perhaps the most important point decided was the two-week lapse between the final whitening and the application of new composite materials; this was done in an attempt to minimize the possibility of debonding due to soft surface structure and roughness. Ultimately, conservative measures resulted in a highly satisfied patient with an interesting case study.
Acknowledgments
The authors would like to thank Dr. Shradha Sharma of Tufts University and John Orfanidis of Orfan Dental Laboratory for clinical assistance with this case, in addition to Jennifer Towers of Tufts University for her editing and grammatical composition, which was very much appreciated.
References
1. Cavalli V, Reis AF, Giannini M, et al. The effect of elapsed time following bleaching on enamel bond strength of resin composite. Oper Dent. 2001;26:597-602.
2. Attin T, Hannig C, Wiegand A, et al. Effect of bleaching on restorative materials and restorations—a systematic review. Dent Mater. 2004;20:852-861.
3. Deliperi S, Bardwell DN. Two-year clinical evaluation of nonvital tooth whitening and resin composite restorations. J Esthet Restor Dent. 2005;7:369-378.
4. McGuckin RS, Thurmond BA, Osovitz S. Enamel shear bond strengths after vital bleaching. Am J Dent. 1992;5:216-222.
5. Rueggeberg FA, Margeson DH. The effect of oxygen inhibition on an unfilled/ filled composite system. J Dent Res. 1990;69:1652-1658.
6. Cadenaro M, Breschi L, Antoniolli F, et al. Influence of whitening on the degree of conversion of dental adhesives on dentin. Eur J Oral Sci. 2006;114:257-262.
7. Perdigao J, Francci C, Swift EJ Jr, et al. Ultra-morphological study of the interaction of dental adhesives with carbamide peroxide-bleached enamel. Am J Dent. 1998;11:291-301.
8. Josey AL, Meyers IA, Romaniuk K, et al. The effect of a vital bleaching technique on enamel surface morphology and the bonding of composite resin to enamel. J Oral Rehabil. 1996;23:244-250.
9. Attin T, Buchalla W, Wiegand A. Adhesion, ceramics and bleaching—a critical evaluation. Academy of Dental Materials Transactions. 2006;20:132.
10. Titley KC, Torneck CD, Ruse ND, et al. Adhesion of a resin composite to bleached and unbleached human enamel. J Endod. 1993;19:112-115.
11. Matis B, Cochran MA, Eckert G, et al. The efficacy and safety of a 10% carbamide peroxide bleaching gel. Quintessence Int. 1998;29:555-563.
a VITA Shade Scale, Vident™, Brea, CA
b Ultra-Etch™, Ultradent Products, Inc., South Jordan, UT
c Adper™ Singlebond™ , 3M™ ESPE™, St. Paul, MN
d 4 Seasons, Ivoclar Vivadent, Amherst, NY
e ET Finishing Burs, Brasseler® USA, Savannah, GA
f CompoSite® Polishing Paste, Shofu Dental Corporation, Menlo Park, CA
g Opalescence Trèswhite Supreme, Ultradent Products, Inc., South Jordan, UT
About the Authors
Gerard Kugel, DMD, MS, PhD
Associate Dean for Research, Tufts University School of Dental Medicine
Boston, Massachusetts
Susana Ferreira, DDS
Assistant Clinical Professor, Tufts University School of Dental Medicine
Boston, Massachusetts
Ronald Perry, DMD, MS
Director, Gavel Center for Restorative Research
Assistant Clinical Professor, Tufts University School of Dental Medicine
Boston, Massachusetts