Temporary Cements Revisited
A dental assistant who knows the nuances of temporary cements is an asset
Selecting a temporary cement to use during a dental procedure is not as simple as it seems. An inappropriate choice can affect the success or failure of the restorative process. Some states permit dental assistants to place temporary restorations under the dentist’s limited supervision, so dental assistants must clearly understand the options available and the specific uses for the many choices in temporary cements available in dentistry today.
Choosing an appropriate temporary cement must be based on the following factors: how long the temporary is needed, what type of temporary or permanent restoration is being placed, and which type of tooth to which the provisional is being cemented. Other concerns include cement solubility, retentive qualities, marginal seal, ease of removal (if bonding will be done later), and esthetics. Temporary cements with higher compressive strength will withstand occlusal pressures, but will make the temporary restoration harder to remove. Poor choices of temporary cement can compromise the look and function of the temporary, affect the permanent restoration, traumatize the tooth, and cause open margins after the cement dissolves. Microscopic remnants of temporary cement can also remain on the tooth and preparation surfaces after temporization removal and interfere with the bond of the permanent restoration. As a result, the cement chosen must be easily removed, and the tooth surface completely cleaned.
The cements available for use in various provisional procedures include zinc oxide eugenol (including reinforced), zinc oxide non-eugenol, resin temporary cement, glass ionomer temporization cement, and polycarboxylate cement. Looking at the properties and uses of each of these cements will allow the dental assistant to make appropriate choices that will only be to the comfort and advantage of the patient and contribute to the success of the dental procedure.
Zinc Oxide Eugenol
Utilized in dental procedures at least since the 1930s, zinc oxide eugenol (ZOE) is a functional, flexible, and adequate cement to use for both temporary crown cementation, as well as for temporary restorations and bases under some restorations. The eugenol has palliative qualities and is antimicrobial, which aids in soothing irritated tooth tissues that have been traumatized by caries and preparation procedures.
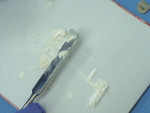
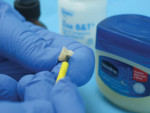
ZOE can be purchased in a powder/liquid form in regular or reinforced type, both of which can be mixed to a creamy consistency for temporary crown cementation, or a putty consistency for base or temporary restoration placement. ZOE can be used with methylmethacrylate acrylic temporaries, and also to cement aluminum and stainless steel temporary crowns. It is adequately retentive for temporary cementation, but may be difficult to remove from acrylic surfaces. Adding a small amount of petroleum jelly to the mix will decrease the retentive properties of the powder/liquid form of the cement (Figure 1). In addition, a small amount of petroleum jelly can be wiped on the outside surface of the acrylic temporary crown, at the marginal area, to aid in removal of excesses after cementation (Figure 2). Care must be taken to avoid the use of eugenol and petroleum products with some acrylic resins, as they can interfere with the polymerization of the acrylic. Paste/paste types of cements tend to be less retentive than the powder/liquid form, and are selected when easy removal of the provisional is critical.
Resins are often used in permanent cements, temporary crowns, and core buildup materials. Eugenol can inhibit the polymerization of some resins by interefering with the free radical chemical reaction in the resin, and can soften the acrylic resin surface. Due to its positive characteristic of penetrating and desensitizing dentin, eugenol has also been identified as an ingredient that can reduce the bond strength of permamently cemented crowns, especially with resin-based cements, by interfering with the ability of those materials to penetrate the tooth surface and bond. Eugenol can also cause cracks and crazelines in acrylics and in crowns made of polycarbonate materials. Because of these properties, ZOE is not always the best choice of cements for all temporization procedures.
Zinc Oxide Non-eugenol
Zinc oxide non-eugenol is an opaque two-paste version of the ZOE described previously, but without eugenol. Because eugenol inhibits the polymerization of some acrylic resins used for temporaries and can interfere with the setting of permanent resin cements, this non-eugenol form of ZOE might be a better choice for some procedures. This type of cement has a thin film thickness, allowing restorations to be seated completely in an accurate fit. It has good adhesion properties, but is also easy to remove and to clean. Residual cement tends to stay inside the crown rather than on the tooth when the crown is removed. This type of cement cannot be used for a temporary restoration, as it cannot be mixed to a thicker consistency. However, zinc oxide non-eugenol is frequently used for temporary cementation of provisional and permanent restorations.
A new and improved version of zinc oxide non-eugenol is available, which is translucent and can esthetically blend with specific restoration shades, making it especially ideal for esthetic restoration. This new form of cement is manufactured with or without triclosan, an ingredient that the Food and Drug Administration is currently reviewing for safety regarding triclosan’s effect on hormone regulation. Triclosan is used in dental products as a desensitizing agent. The dental assistant may want to consider this concern when choosing the type of non-eugenol–based zinc oxide cement to use for the specific temporization process.
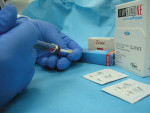
Zinc oxide non-eugenol is available in base/catalyst tubes and in single-dose packets, both of which are mixed with a spatula, and in unit-dose tubes and automix syringes (Figure 3).
Resin Temporary Cement
For maximum hold and low-solubility factors, resin temporary cement might be a good choice for temporary cementation. These cements have high strength and retention abilities, and are more esthetic and easier to clean up. They tend to be compatible with temporary resins, resin core buildup materials, permanent cements, and bonding materials. Some contain desensitizing agents, such as potassium nitrate, to help reduce postoperative sensitivity. These cements can absorb odors and discolor, and microleakage may occur, especially with a poorly constructed temporary crown. After cementing a provisional, the material will become rubbery, which allows for easy removal of excess cement, but will harden when it reaches its final setting time.
Resin temporary cement is often used for cementation of implant provisionals, as there is adequate hold, but the temporary can also be somewhat easily removed without traumatizing the implant itself. This type of cement usually comes in an automix cartridge system, with a base and catalyst component, which combines when expelled through a mixing tip. Resin temporary cement is used to cement crowns and bridges temporarily, as well as for provisional cementation of implant-retained crowns, but some forms of this cement should not be used to cement inlays, onlays, or permanent restorations temporarily. Resin temporary cement can also come in a type of “hybrid,” which combines the best properties of resin cement with the best of carboxylate cement.
Glass-Ionomer Temporary Cement
A lower-viscosity glass-ionomer cement can be used as an intermediate restoration for endodontically treated teeth and for temporization of noncavitated or rampant carious areas, as would be seen in early childhood caries cases. It can also be used to temporarily cement metal, resin or ceramic restorations, temporary and permanent, and works well with provisionals cemented on teeth or implants, with excellent results as a long-term temporary cement. Glass-ionomer cement also releases fluoride into the tooth tissues, which would help with the control of caries as well as making wounded tissues less sensitive. It has a thin film thickness, which allows for complete seating of the restoration being temporized. Clean up of excess cement around the restoration can be accomplished in approximately 1 minute after seating. Manufacturers say that this cement does not adversely affect the ability of the permanent cement to bond to the tooth.
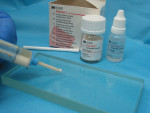
The type of glass ionomer that is used for intermediate restorations may come in opaque or pink shades. Although pink is not esthetically pleasing to the patient, the color may encourage the patient to return for the permanent restorations while at the same time reminding the patient that the restorations are temporary and have a limited lifespan (Figure 4). Glass-ionomer temporary cement is available in a two-paste cartridge dispensing system or a capsule dispenser system that is mixed on an amalgamator and then applied with a gun.
Polycarboxylate Cement
Sometimes called a semi-permanent cement, polycarboxylate cement is a good choice for longer-term temporary restorations or temporaries that require greater retention, such as stainless steel crowns, and for cementing some long-term temporary orthodontic appliances. This type of cement is kind to the tooth tissues as well as the gingival tissues, while possessing adequate retentive properties to hold the restoration or appliance in place during an extended period. It has reasonably low-solubility properties and is easy to remove after cementation.
If the dentist is concerned about remaining cement on the preparation interfering with the bond of the permanent cement, polycarboxylate would prove to be a good choice as it is easy to clean off of the tooth. Polycarboxylate is available as a powder/liquid form, as well as a paste/paste automix syringe, and must be quickly and accurately mixed to avoid manipulation past the working time of the material (Figure 5). This luting cement can be mixed to a thinner consistency if being used for temporary purposes. Because of its pink/opaque color, this cement could show through some esthetic provisionals and change the shade and the esthetics of the temporary. Some of these polycarboxylate temporary cements are resin reinforced for added strength and improved properties.
Conclusion
Understanding the various properties of temporary cements will allow the dental assistant to assist the dentist in treating the patient with accurately selected materials that will allow the treatment to go smoothly and without error. A dental assistant who understands the advantages and disadvantages and the unique properties of each type of temporary cement available will be an invaluable asset for a good and successful dental practice.
References
1. Margeas RC. Temporary cement options. Inside Dentistry. 2011;7(7). Accessed Jan. 29, 2014. https://www.dentalaegis.com/id/2011/08/variety-of-cements-offer-many-benefits
2. Santos GC Jr, Santos MJMC. Selecting a temporary cement: a case report. Dentistry Today. March 12, 2012. Accessed Jan. 29, 2014. https://www.dentistrytoday.com/dental-materials/7096-selecting-a-temporary-cement-a-case-report.
About the Author
Stephanie Joyce Schmidt, CDA, CPFDA, CRFDA, CDT, RDAEF2, FADAA, MS
Associate Professor
Pasadena City College Dental Assisting Program
Pasadena, California