Provisional–Temporary Cements
Techniques to facilitate placement of provisional restorations
Provisional or temporary cements play an important role in restorative dentistry. Recommendations for the use of provisional cements include the temporary cementation of temporary restorations used to restore tooth preparations for indirect restorations including crowns, fixed partial dentures, inlays and onlays, as well as for temporary cementation of definitive restorations of the same types. Provisional cements are also used for the cementation of implant crowns and fixed partial dentures (fixed bridges). There are specific techniques to make using a temporary cement easier, and different types of temporary cements for certain clinical situations.
Techniques for ease of use of temporary cements
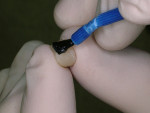
Once the provisional restoration has been adapted, finished, and polished, it is ready for cementation. To facilitate clean-up of the temporary cement, follow two simple tips. First, to avoid leaving a white streak of set provisional cement around the surfaces and margins of the restoration and to simplify removal of excess provisional cement, before placing the cement, lightly paint some petroleum jelly on the outside, polished surfaces of the provisional restoration using a disposable brush. (Figure 1) For a bridge, place a thicker portion of petroleum jelly on the tissue surface side (outside) of a pontic and gingival to the connector of the bridge with a brush. This thicker portion of petrolatum gel will prevent the temporary cement from getting into these difficult-to-access areas once the cement has set. Because the gel is there instead of the cement, it will be easier to remove the temporary cement.
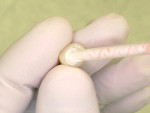
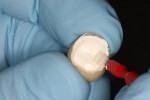
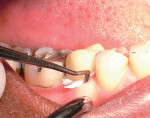
For cement placement into the temporary restoration, either using an automixing tip with a automixed temporary cement and squeezing it into the temporary (Figure 2) or by mixing the cement on a pad or dispensing to a pad after automixing, use a disposable brush to apply the cement to the temporary restoration. In either case, never overfill the inside of the temporary restoration—only enough to coat the inside. The authors prefer using the brush to apply the cement to the internal of a crown, bridge, or inlay/onlay temporary because it is easier to control the amount of temporary cement and where it is applied. The temporary cement should completely coat all the internal surfaces of the restoration (Figure 3). Do not overload the restoration with temporary cement (or even a final cement for a final restoration) because it can lead to difficulty fully seating the restoration and also to a gross excess of cement that will need to be removed. Gross cement can easily be removed after the complete set of the cement with a scaler (Figure 4). In fact, it will easily be removed if petroleum gel was placed.
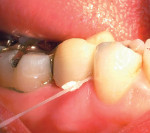
One problem when removing provisional cement for crowns, inlays/onlays, and bridge temporary restorations is removing the cement in the gingival embrasure below the contact area. Flossing the contact will often not remove the cement: the floss will slide between the restoration and the cement and the cement will not be pulled out. For those times when the cement is more difficult to remove from the embrasure space (for teeth with large gingival embrasures), there is a simple solution. For these cases, tie two to three knots into the end of a piece of dental floss, then floss the contact area pulling the floss through so the larger knotted area will pull out the gross set cement (Figure 5). It is critical that all residual temporary cement be removed. Excess cement remaining in the sulcus can result in irritation of the periodontium in the sulcus, and in the most extreme cases result in severe periodontal inflammation with the potential for bone loss. The knotted floss can also be used to remove the set cement under a pontic area by placing the knotted floss on the gingival pontic site before cementation. Once the provisional cement has hardened, pull the floss out.
Choices in Temporary Cements
There are many choices with temporary cements (Table 1). Dentists select cements based upon their experience with a product, or recommendations that have been made by others, or through continuing education courses. There are many important factors in the physical properties and handling of the cement that make a difference.1 These properties include:
1. good retention of the indirect restoration with the provisional cement (good adhesion to the tooth preparation and restoration)
2. easy to dispense, mix and apply to the restoration
3. easy removal of excess from the external surfaces of the restoration after cementation
4. adequate working time and setting time
5. viscosity and handling properties for ease of placement to restoration to be cemented and/or tooth preparation
6. easy removal of the indirect restoration from the tooth preparation when cemented with the provisional cement without damaging the soft tissues, tooth preparation or pulp
7. easy removal of provisional cement from tooth preparation during clean-up from dentin and enamel, core materials (cast metal, amalgam, composite resin) and implant abutment materials
8. easy removal of the provisional cement from the internal surfaces of the restoration when the restoration needs to be recemented
9. no or minimal chemical reaction of the provisional cement to the restorative material in the restoration restorative material (eg, zinc-oxide eugenol cements can contaminate and soften acrylic resins)
10. biocompatibility to soft tissues, pulp and tooth structure
11. no interference with adhesion of a final cement
12. good shelf life
While no one product fulfills all these properties, the choice of a provisional cement should depend on the clinical circumstance for which it is chosen.
Clinical Situations
Provisional restorations are important. The provisional restoration protects the tooth by minimizing extreme changes in temperature due to food and beverages ingested. In addition, when cemented, it provides a seal against microleakage for the period of time that the provisional restoration will be in place and reduces sensitivity while the laboratory is fabricating the crown or inlay/onlay.2,3 The provisional cement plays a key role in keeping the temporary restoration on the tooth while the patient is waiting for the final restoration to return from the dental laboratory.4,5 While the cement helps retain the temporary restoration, it also has to provide for easy removal of the provisional restoration without harming the periodontium, tooth preparation, or pulp when the final restoration is tried-in and adjusted.
Some practitioners will temporarily cement some final restorations, usually all metal or porcelain-metal, to evaluate the restoration’s contours and margins. In the case of a fixed partial denture (fixed bridge) with a pontic, some clinicians prefer to provisionally cement the restoration first with a provisional cement to assess the periodontal response of the restoration and the adaptation of the tissue-borne side of a pontic. In the past, provisional cements were opaque in color due to the materials being used. Recently more tooth-colored provisional cements have been introduced to not interfere with the color evaluation of translucent restoration materials. Examples of color neutral, shaded or translucent provisional materials include Zone (Dux® Dental, www.duxdental.com, NexTemp™ (Premier Dental, www.premusa.com), TempBond® Clear (Kerr Corporation, www.kerrdental.com), and Systemp®.link (Ivoclar Vivadent®, www.ivoclarvivadent.us). In some cases, for a patient who relates a history of dentinal hypersensitivity after the tooth preparation and provisional restoration placement, the definitive restoration may be temporarily cemented with a provisional cement to assess pulpal health. In these cases, the use of a eugenol-containing provisional cement may have a sedative affect on the pulp.6 Eugenol-containing provisional cements with residual eugenol remaining after setting can result in softening of an acrylic resin—not allowing additional acrylic resin added to a previously made temporary crown or bridge to set completely.7,8 With the newer eugenol-containing provisional cements, the amount of unreacted eugenol can be minimized by using the correct mixing proportions recommended by the manufacturer.4
The practitioner will determine the best temporary cement for any given clinical situation. In most cases there is not a one-size-fits-all choice in provisional cements. When using a provisional cement it is critical that the tooth surfaces of the preparation be adequately cleaned to remove the residual provisional cement. Techniques to remove residual provisional cements from tooth preparations include scraping the tooth with a hand instrument (usually a scaler or curet), cleaning the tooth preparation with a prophylaxis cup with a water–pumice paste slurry, and the use of an intraoral sandblaster. Of the three methods, the intraoral sandblaster method is the most reliable, followed by a prophylaxis cup with a water–pumice paste slurry. To be certain the final cementation is optimized, the tooth preparation must be clean.9-11
When placing final restorations for implant-supported prostheses, some practitioners place the final restoration with a provisional cement so it can be more easily removed on a regular basis; or if one or more of the abutments of a fixed partial denture come loose, the prosthesis can be removed and recemented. Once again, the choice of cement depends on the clinical situation.
Types of Provisional Cements
The earliest provisional cements were made from zinc-oxide powder and eugenol liquid (ZOE). Today the dental office has many choices with provisional–temporary cements. Because ZOE cements can have negative effects on the acrylic resin and adhesive tooth cementation with composite resin cements, in recent years a number of manufacturers have addressed this problem by introducing provisional cements that are eugenol-free. Some eugenol-free cements do not set as hard as eugenol-containing cements, which can lead to a temporary crown or bridge becoming uncemented, requiring an additional office visit to recement the temporary.
Some eugenol-free provisional cements have been formulated to address problems identified with past cements.12,13 There was a need for a more rigid provisional cement to improve retention of the restoration and facilitate clean-up of the provisional cement from the preparation and restoration. A clinician may use a different provisional cement for certain circumstances to achieve easier removal of the restoration at a later time, compared to the need for a more rigid provisional cement that will allow for better retention on a crown preparation that is not retentive due to its occlusogingival height or the presence of excess taper to the axial walls of the crown preparation.12,13 TempoSIL (Coltène/Whaledent, www.coltane.com) achieves both goals. It has a unique formulation as an addition-cured silicone-based zinc oxide temporary cement with a silane agent for improved adhesion and marginal integrity. This formula produces a firm, yet elastic temporary cement that can be easily peeled off the tooth preparation (either natural tooth, core of restorative material, or implant abutment) and removed from the internal surfaces of both provisional and final restorations. Other provisional cements, UltraTemp (Ultradent Products, www.ultradent.com) and Hy-Bond® Polycarboxylate Temporary Cement (Shofu, www.shofu.com), use a polycarboxylate formulation and are eugenol-free. UltraTemp addresses the need for greater rigidity for restoration retention and is available in two different formulas (regular and rigid set), while Hy-Bond has one formula for a more rigid set. TempSpan® CMT (Pentron Clinical, www.pentron.com) and NexTemp (Premier Dental) are two resin-based formulations that provide for translucent color, greater rigidity, and a two-stage gel setting reaction for easy removal of excess. TempSpan CMT also has the additives of sodium fluoride, potassium nitrate, and calcium phosphate for a reported decrease in postoperative sensitivity.
Convenience Packaging
In the past, many temporary cements were packaged in paste squeeze tubes. There are problems associated with dispensing of material and maintenance of these tubes. Excess cement extrudes from the tube, making the outside of the tube making the tube sticky and difficult to clean due to the oily consistency of the pastes. Convenience packaging has made the use of provisional cements easier with more consistent dispensing. For those times when a ZOE provisional cement is desired, Embonte and Embonte 2 (Dux Dental) afford convenient and easy-to-use packaging. Embonte is provided in unit dose packaging, which allows the chairside assistant to dispense the right amount of both base and catalyst paste for a single unit provisional crown cementation without any excess and waste. Embonte2 uses the same ZOE formulation and is dispensed in a dual-cartridge auto-aspirating syringe that eliminates the waste of conventional squeeze tubes with its patented auto aspirating feature.
If convenience packaging is desired with a eugenol-free provisional cement, there are a number of good choices with the advantages for ease of use. What could be more convenient than a moisture sensitive and self-setting single paste available in a unit dose? Eugenol-free NoMIX® Temporary Cement (Centrix, www.centrixdental.com) is a single-paste no-mix moisture-activated temporary cement. When the practitioner is ready to cement the restoration, the interior of the restoration is wetted with water before the cement is dispensed. Initial set for clean-up is 5 minutes with complete setting in 15 minutes. This extended working time allows for use with single units and multiple units. Also, this temporary cement is packaged in unit dose so that patients can take it with them to recement their own provisional restoration.
Many of the newest provisional cements are available in a double-barreled automixing syringe or in the case of TempoCem® NE (Zenith DMG, www.dmg-america.com), a double barreled cartridge that is dispensed through gun-type applicator similar to those used with bis-acryl provisional composite resins. Automixing dual-tube provisional cements allows the chairside assistant to dispense the right amount for a single unit or multiple units directly into the provisional restoration. (Figure 2). It also means that each mix is consistent because the catalyst and base paste will always be dispensed through the mixing tip in the optimal volume ratio and mixed in a consistent fashion through the automix tip. It also minimizes waste and eliminates the clean-up of a cement spatula and mixing pad.14 Some of the products that are available in this automix double-barreled syringe are Temp Advantage® (GC America, www.gcamerica.com), TempSpan CMT (Pentron Clinical), Zone (Dux Dental), Systemp.Cem (Ivoclar), and TempoSIL (Coltène/Whaledent), among others.
Conclusion
While there is no one provisional cement that meets all the requirements of an ideal product, the current generation of provisional cements offers a number of advantages over what has been used in the past. If a practitioner is having success with a provisional cement, there is no reason to make a change. However, if the practice has expanded the types of restorations to include all-ceramic and implants, there may be a need for more than one brand of provisional cements. The advantages of a more rigid setting provisional cement may be necessary for a number of clinical situations, including a crown with compromised retention or a patient with parafunctional habits. If there are issues with postoperative sensitivity, a provisional cement containing eugenol or a eugenol-free provisional cement with additives for desensitizing may solve these problems.
There is no one provisional cement to meet all clinical needs. It may be necessary to have at least two different provisional cements to accommodate the dental practice. Whatever product is used, it is important that the provisional cement be cleaned thoroughly from the tooth before definitive cementation.
References
1. Strassler HE. Provisional cements. Inside Dentistry. January 2008. https://www.dentalaegis.com/id/2008/01/provisional-cements. Accessed June 28, 2012.
2. Mash LK, Beninger CK, Bullard JT, Staffanou RS. Leakage of various types of luting agents. J Prosthet Dent. 1991;66(6):763-766.
3. Pan YH, Ramp LC, Lin CK, Liu PR. Comparison of 7 luting protocols and their effect on the retention and marginal leakage of a cement-retained dental implant restoration. Int J Oral Maxillofac Implants. 2006;21(4):587-592..
4. Geganuff AG, Holloway JA. Provisional restorations. In: Rosensteil SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. Mosby Elsevier. St. Louis; 2006:466-504.
5. Shillingburg HT Jr. Provisional restorations. In: Shillingburg HT, Hobo S, Whitsett LD, et al. Fundamentals of Fixed Prosthodontics. 3rd ed. Quintessence Publishing: Chicago; 1997:225-256.
6. Pashley EL, Tao L, Pashley DH. Sealing properties of temporary filling materials. J Prosthet Dent. 1988;60(3):292-297.
7. Gegauff AG, Rosensteil SF. Effect of provisional luting agents on provisional resin additions. Quintessence Int. 1987;18(12):841-845.
8. Millstein PL, Nathanson D. Effect of eugenol on cured composite resin. J Prosthet Dent. 1983;50(2):211-215.
9. Fonseca RB, Martins LR, Quagliatto PS, Soares CJ. Influence of provisional cements on ultimate bond strength of indirect composite restorations to dentin. J Adhes Dent. 2005;7(3):225-230.
10. Grasso CA, Caluori DM, Goldstein GR, Hittelman E. In vivo evaluation of three cleansing techniques for prepared abutment teeth. J Prosthet Dent. 2002;88(4):437-441.
11. Rosensteil SF. Luting agents and cementation procedures. In: Rosensteil SF, Land MF, Fujimoto J. Contemporary Fixed Prosthodontics. 4th ed. Mosby Elsevier. St. Louis; 2006:909-927.
12. Sadan A. Clinical considerations in cement selection for provisional restorations—Part I. Pract Periodontics Aesthet Dent. 2000;12(7): 638.
13. Sadan A. Clinical considerations in cement selection for provisional restorations—Part 2. Pract Periodontics Aesthet Dent. 2001;13(1):16.
14. Strassler HE, Tomona N, Serio CL. Anterior provisional restorations with a translucent prefabricated crown form. Contemporary Esthetics and Restorative Practice. 2004;8(9):44-48.
About the Authors
Howard E. Strassler, DMD
Professor and Director of Operative Dentistry
Department of Endodontics, Prosthodontics and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland
Roseanna J. Morgan, CDA
Clinic Coordinator
Postgraduate Prosthodontics
University of Maryland Dental School
Baltimore, Maryland