A Modern Guide to Temporization Materials and Techniques
With practice and the right tools, assistants can develop an efficient technique
Dental assistants who are certified to place temporary restorations have a valuable role in the dental office. In order to maximize this role, assistants should stay continually informed on the materials and techniques available for temporization. The good news is that as materials advance, the assistant’s job becomes easier and more streamlined. With the right material and technique, assistants can create temporary restorations that closely resemble the final restoration in both esthetics and function.
Choosing the Best Material
A brief review of the available temporization materials reveals the benefits and drawbacks of each type. One of the oldest types of materials still on the market is acrylic, which has been in use for temporization for more than 80 years. These materials are low in cost, and also provide good esthetics and versatility. However, their ease of use is not as appealing as some newer materials. Acrylics must be hand mixed to the proper consistency, which adds to the dental assistant’s workload. These materials also have a strong odor that is unappealing to patients, and they exhibit shrinkage during setting. Additionally, acrylic temporization materials have an exothermic setting reaction that gives off a significant level of heat. The materials must be used very carefully in order to avoid
pulpal damage.1
Today, products formulated with a self-curing bis-acryl composite resin are some of the most commonly used temporization materials in many practices. This class of materials, which includes brands such as 3M™ ESPE™ Protemp™ Plus Temporization Material (www.3m.com) (Figure 1), Luxatemp® from DMG America (www.dmg-america.com), and Venus® Temp C&B from Heraeus Kulzer (www.heraeus-dental-us.com), offers a number of advantages. The materials typically exhibit very good esthetics, have an imperceptible odor, and generate minimal heat. Some systems are compatible with auto-mix delivery methods. Additionally, these materials can be repaired with composites.1
Some perceived disadvantages of these materials include the fact that they cost more than the older acrylic material options. They also differ from acrylics in that their viscosity cannot be changed. Some of these materials are more brittle than acrylics, requiring extra consideration for where they are used in the mouth. These materials should not be used for long span bridges unless extra reinforcement is placed in the temporary. Finally, composite resin temporization materials form an oxygen-inhibited layer that is sticky, requiring removal with an alcohol swab.1 These materials can be smoothed and made lustrous with the newest class of resin glazes.
However, the qualities offered by newer-generation bis-acrylic temporization materials make them very popular in many dental offices, despite the additional cost. These materials improve on the traditional characteristics of self-curing temporization materials, delivering added benefits in strength as well as esthetics. Materials with nanoparticles, such as Protemp Plus temporization material, provide a smoother surface that requires less finishing to reach a natural gloss (Figure 2). An additional advantage of a smooth surface on the temporary is that it is more comfortable for patients, is easier to keep clean over the time it is in service, and it promotes periodontal health.
Shade Selection
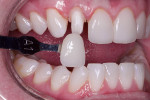
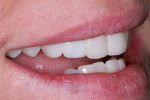
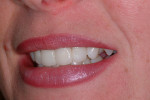
When selecting a material, the dental team should use care to choose a material that is accurate to the shade guide (Figure 3). Some materials suffer from inaccuracies in this area; they may be labeled as A1 but in reality may be closer to A2. This is a problem because although the provisional restoration will be in place only a short while, it is important that it display a similar appearance to the final restoration in order to manage patient expectations and address any possible issues with the final restoration before it has been placed (Figure 4).
When selecting the shade for the provisional, many dental professionals choose to err on the whiter side. The shade should be selected before treatment is started. Cotton rolls and isolation during all the procedures can leave the teeth looking lighter in color due to enamel dehydration. In smile makeover cases, a provisional material that offers a selection of bleach shades is especially helpful. The advantage of using a lighter shade is that it can be darkened if necessary; however, in today’s cosmetically driven practices, patients often prefer to go as bright as possible. Use of a whiter shade in the provisional stage can help patients solidify their thoughts about the level of whiteness they desire from their final restorations.
Efficient Placement Technique
While techniques will vary depending on the clinical situation and the selected material, there is a technique commonly used for anterior provisionals using a “shrink wrap” approach. Using a laboratory diagnostic wax-up, the assistant first takes a putty matrix impression in order to capture the detail of the margins and interproximal areas. After the dentist has finished the crown preparations, the putty matrix is then relined with temporization material. Some dental assistants paint a small amount of glycerine on the gum tissue surrounding the preparations. The putty matrix with the temporization material is then seated on the preparations. Be careful when seating the putty matrix not to push too hard, this will distort the putty. The putty with temporization material is left on the teeth for 90 seconds and removed. The temporary is then teased off the tooth preparations. Using this technique the excess temporization material can be easily peeled away from the gum tissue. This relieves the dentist from having to remove any of the flash with a bur or other instrument. Utilizing the putty matrix impression of the laboratory wax-up helps provide a closer match to the final restoration, and also reduces the amount of finishing and polishing necessary to achieve the proper margins and interproximal details.
With many materials, assistants commonly have to polish with burs, polishing cups, points or discs. However, polishing tools can sometimes dig into the provisional material; therefore the assistant must have significant experience with each material to know how much pressure to use. A significant advantage of newer materials such as Protemp Plus temporization material is that they do not require this type of polishing. They can simply be wiped with a 2x2 gauze soaked in alcohol. This is all that is needed to give the material a high level of polish, which saves the assistant a notable amount of time and effort.
Before the temporary restoration is placed, there are a number of factors that the assistant should confirm for soundness. First, the proximal and occlusal contacts should be checked to ensure they are correct. This helps to maintain gingival tissue health and the proper space for the final restoration, and to prevent supra-eruption and movement of teeth (Figure 5). An additional factor that can impact tissue health is the emergence profile of the temporary. Assistants should ensure a natural emergence profile in order to deflect food away from the gingival tissue. Finally, a proper marginal seal is important to the function of the temporary, as it helps reduce the chances of microleakage and promotes gingival healing.1
Conclusion
With practice and the right tools, assistants can develop an efficient temporization technique that relieves the dentist of extra work and gives patients a strong and esthetic provisional. Assistants who are able to work in this capacity are invaluable assets to the dental team.
References
1. Temporization procedure. 3M ESPE Expertise web site. https://www.3mespetemps.com/assets/temporization/temp_overview.html. Accessed June 7, 2012.
About the Authors
Shannon Pace Brinker, CDA, CDD
Owner
Contemporary Product Solutions
Virginia Beach, Virginia