Creating Great Dental Impressions
The appropriate selection of impression material and tray is integral to the end result
Many dental practices may overlook the importance of good impressions. However, the quality of impressions can greatly affect the clinical results. This article will address some basics to explain how the appropriate selection of impression material and tray is integral to the end result of the impression.
Material Selection
No one impression material fits every clinical situation. Alginate materials are suited well for preliminary impressions and study models or for bleaching trays, occlusal guards, and other uses for which finite accuracy is not critical. However, alginate impression materials must be poured immediately because they lose accuracy as they dehydrate. In addition, due to the delicacy of the material, multiple pours are not possible as the material typically tears upon separation of the cast from the impression. In recent years, alginate substitutes have been introduced, which are less expensive medium-body polyvinyl siloxane (PVS) impression materials. They do not require immediate pouring and usually have sufficient durability to allow multiple pours from the same impression.
Impression materials that are recommended for final impressions are in 2 categories: polyether (eg, ImpregumTM, 3MTM ESPETM, www.3MESPE.com) and PVS. Each of these materials has its proponents and detractors. The dental auxiliary should have an understanding of how best to use these materials, in various clinical situations.
Polyether impression materials are used in a single-step process. As polyether impression materials will not adhere to already-set materials, one cannot reline the impression to capture additional detail; therefore the impression must be taken in a single step. These materials are also stiffer than PVS. When excess undercuts are present, it is recommended that these be blocked out. A softer material is available that can be injected into the marginal detail, and it is advised this also be placed into undercuts, such as under existing bridges, to prevent the impression from locking intraorally.
PVS material can be used in ether a single-stage or two-stage impression technique as new material will bond to already-set material. An added benefit is that PVS material is available in multiple viscosities ranging from thin materials (light bodies and injectables) that will capture minute details to stiffer materials. Medium-body PVS material is well suited for many impression needs. However, when a stiffer material is desired, selection of a universal body material may be better suited for the application. Universal body materials flow similarly to medium-body ones but are much stiffer upon setting. These work well when using dual-arch trays and open-tray implant impressions (addressed later in this article). PVS materials also are available in tray and putty materials, which have good initial body and fairly stiff setting. However, the use of tray and putty materials can result in pulls and drags in the impression, as they do not flow well if they are not combined with a more flowable PVS material.
Whether a polyether or PVS material is selected, the model cannot be immediately poured. As these materials need to “de-gas” prior to pouring, it is recommended to wait at least 30 minutes prior to model fabrication in order to help prevent the surface of the model from being covered by multiple tiny bubbles resulting from hydrogen gas release as the impression material finalizes its set after removal intraorally (Figure 1). Should the model have these microbubbles on the surface, a new model can be poured, provided the impression has not been torn.
Trays
Similar to the impact of appropriate selection of impression material, the selection of the most suitable tray greatly influences the final result.
Trays are divided into 2 categories: stock and custom. Within the stock category, there are 3 subcategories: dual-arch (used for fixed prosthetics), full-arch dentate (used for teeth present in the arch, for study models, and for fixed prosthetics with natural teeth or implants and partial dentures), and full-arch edentulous (used for full-denture impressions). Custom trays are typically used for either fixed prosthetic or removable prosthetic applications.
Dual-arch impressions are popular and, when used properly, provide accurate impressions. There are criteria for their use. It is important that the tray not contact the teeth or soft tissue; otherwise, the tray may distort, rendering the resulting models inaccurate and affecting the prosthetics fabricated from them (Figure 2). As one size does not fit all and manufacturers have dual-arch trays of different dimensions, it is wise to have trays from 2 to 3 manufacturers available so that the correct tray can be selected when needed. Another important criterion is that the tray needs to capture at least 1 full tooth mesial and distal to the prepared teeth so that the impression can be used to mount the resulting models in correct occlusal relationship. The following configurations are available: posterior quadrant, posterior half arch, three-quarters arch, anterior segment, and full arch (Figure 3).
When an impression is needed for capturing the full arch for fixed prosthetics or when a partial denture is planned or for study models, stock trays may be utilized. These trays are available in small, medium, and large for both the maxillary and mandibular arches. However, as with dual-arch trays, the widths vary between manufacturers. The practice should have a selection of trays from 2 to 3 manufacturers so that the most suitable tray shape and size can be used (Figure 4). Segmental single-arch trays are also available, and the selection criteria match those for dual-arch trays.
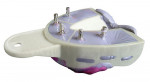
Taking edentulous impressions provides different challenges. An impression for a full denture must capture the vestibule, frenum, and other parts of the anatomy, which are considered unimportant for impressions for fixed prosthetics. Unfortunately, those trays used for fixed prosthetics do not extend into these anatomic areas, and trays designed for edentulous arches are indicated. Several are available, with some being modifiable. The nonmodifiable edentulous trays are fabricated from either metal or plastic materials. However, due to the material or cost of the trays, they are not designed to be modified to fit the particular patient. The MassadTM edentulous impression tray (DENTSPLY Caulk, www.caulk.com) is inexpensive and plastic, allowing it to be modified to create a custom tray chairside for the patient (Figure 5). The trays are available in 5 maxillary and 5 mandibular sizes, making selection of one to fit the arch easier. As the trays are made from a thermoplastic material, they can be modified by heating with an alcohol torch or a hot water bath, and then can be modified intraorally to match the arch, providing a tray that will have a uniform thickness of impression material and improved accuracy.
Implant impressions are taken as either a closed-tray or an open-tray technique. For a closed-tray technique, a tray for a full-arch dentate impression is used even if the arch has no natural teeth. This will allow space for the impression heads and sufficient impression material to capture the impression head within the material and tray. If an open-tray technique is chosen, two options are available. A full-arch dentate tray can be used and holes in the occlusal surface can be cut in order to allow the long impression pin to protrude through the tray once inserted, filled with impression material. It is advised that prior to inserting the tray filled with impression material, the tray be tried in after the occlusal holes have been created in order to verify that the pins protrude through the tray. The holes can be moved or enlarged as needed until they are visible through the tray, and then the impression can be captured. It is important that upon insertion of the filled tray, impression material be wiped from the top of the pins and visualization of all pins is noted while the impression is setting.
Another alternative with open-tray impressions is the Miratray® impression tray (Hager Worldwide, www.hagerworldwide.com). These are unique trays designed specifically for open-tray impressions. The occlusal tray surface is covered with a clear film, eliminating the need to cut occlusal holes. The filled tray is inserted until the pins perforate the clear film, making it easier than when using a tray with holes placed occlusally (Figure 6).
Custom trays are typically made on a preliminary cast either in the office or laboratory. Most practitioners do not use these because an extra patient appointment is required for taking a preliminary impression. Those who wish to use a custom tray may consider utilizing some of the thermoplastic materials designed for an intraoral tray fabrication. These trays are available as wafers, which are heated in a water bath and then molded intraorally. When these wafers reach room temperature, they stiffen and stabilize. They can be ground with an acrylic bur to shape the flanges or to cut retentive holes and elements to retain the impression material. In their softened state, these wafers can easily be trimmed with scissors. Examples are Easy Tray (Septodont, www.septodontusa.com) and SimpleTray (Simple Tray, www.simpletray.net).
The accuracy of the impression material is always highest when the material has uniform thickness. As the impression material sets, polymerization shrinkage will be greater where the material is thickest. With this in mind, the dental auxiliary wants to select a tray that allows a uniform thickness of impression material. This becomes more critical in the maxillary arch as palatal depth will vary among patients. A patient with a deep palate will result in an impression using an unmodified stock tray with a thick mass of impression material palatally with more shrinkage than a patient with a shallow palate. This can be corrected with different methods.
A stock maxillary tray can be modified by placing wax into the palatal aspect of the tray to minimize the volume in this aspect of the impression. It is recommended that an appropriate adhesive be painted over the wax to ensure adhesion of the impression material to the entire tray surface, including the added wax. Alginate adhesives decrease the possibility of separation of the material from the tray, and their use is recommended in order to improve accuracy of alginate material impressions. These alginate adhesives are available as a spray and make application easy prior to impression taking. Tray adhesives are also available for polyether and PVS impression materials, and one should select the adhesive that is recommended for the type of impression material chosen. The adhesives for polyether and PVS impression materials are available as brush-on products. No matter which material is being used, it is recommended that the adhesive not be applied until immediately before the impression is to be taken in order to maximize stickiness.
Implant Impressions
As previously discussed, implant impressions are divided into closed-tray and open-tray methods. Closed-tray implant impressions are subdivided into 2 types based on whether the final stock
abutment is present. Many implant companies have made available “snap-on” type impression components to match the stock abutment heads in their product offering. These allow the abutment head to be placed and left intraorally. A plastic impression head is then snapped onto the abutment and is picked up in the impression. Upon removal of the impression with the embedded coping, an analog replicating the abutment head is snapped into the coping in the impression and the master cast is fabricated (Figure 7). It is recommended that with this method, a universal body impression material is selected, as it must have sufficient stiffness in order to retain the plastic impression coping when removed intraorally.
The other form of closed-tray impression involves fixating a metal impression head to the implant and then taking the impression. Upon setting, the impression is removed. The closed-tray impression head is removed from the implant intraorally. An analog is placed on it, and it is reinserted into the impression. A master model can be fabricated. Unlike the plastic coping method, as the impression coping needs to be reinserted into the impression, it is best to use a medium-body impression material as stiffer materials may hamper insertion of the impression abutment into the impression, affecting the final restoration’s accuracy (Figure 8).
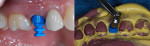
Open-tray impressions require that the impression abutment be accurately retained within the impression, so utilization of a stiffer material is critical. Use of a universal body or putty works best with this technique. One aspect to remember, prior to removal of the set impression, is that all the long pins must be removed; otherwise, impression removal cannot be accomplished without damage to the impression (Figure 9).
Whether using an open tray or a closed tray, in order to eliminate voids at the gingival aspect of the impression around the impression heads, a small amount of impression material of a less viscous nature is injected before seating the tray filled with impression material. A medium-body material can be used for both the open- and closed-tray techniques. Using an intraoral tip on the impression gun, a small amount of material is placed circumferentially around each impression head. With the open-tray method, it is important that only the gingival aspect of the impression abutment have the medium-body material placed around it so that the stiffer material is in intimate contact with the impression abutment. The tendency is for the practitioner to completely cover the impression coping, which may allow micromovement of the impression abutments in relation to each other, affecting the accuracy sought.
Conclusion
Accuracy in dental treatment starts with good impressions, and mistakes are amplified when errors are present in the impressions that dental offices provide the laboratory. Appropriate selection of both the impression material and tray is an important step.
About the Author
Gregori M. Kurtzman, DDS
Private Practice
Silver Spring, Maryland