Mixing Allograft and Xenograft for a Predictable Alveolar Ridge Preservation Procedure: A Case Series
Samar Shaikh, BDS, MS; Annie Siliang Li; and Irina F. Dragan, DDS, DMD, MS, eMBA
Abstract: Background: An alveolar ridge preservation (ARP) procedure is commonly performed to preserve ridge width and height for optimal dental implant placement. Mixing different sources of bone grafts may help maximize their properties to obtain predictable ARP results. Objective:The aim of this case series is to highlight the clinical and radiographic outcomes of a combined allograft and xenograft approach for a predictable ARP procedure. Materials and Methods: Eleven clinical cases that required tooth extraction and future implant placement were selected for this case series. All surgeries were performed by a single clinician in a private practice setting. All cases underwent an ARP procedure, which included atraumatic extraction, degranulation, assessment of the socket, and the use of a combination of allograft and xenograft fibers/granules in a 1:1 mixing approach. Based on the socket defect, either a type I or type III collagen membrane was used during the procedure. In all cases CBCT imaging was done prior to surgical implant placement, and digital implant planning was performed integrating interdisciplinary best practices. Implant placement was carried out using manufacturer's recommendations. Results: Five male and five female patients were included in the study, with one of the male patients having two teeth extracted for a total of 11 sites. The reasons for teeth extraction included fracture, endodontic failure, periodontal infection, and subgingival decay. Healing was uneventful after the ARP procedure for all patients. A minimum of 120 days elapsed between ARP and the surgical implant procedure. Complete radiographic bone fill was observed in the CBCT image for all extraction sites, and no additional bone augmentation was needed at the time of implant placement. Conclusion: This case series demonstrates that based on clinical and radiographic outcomes, a combination of allogenic and xenogenic bone substitute can be utilized to obtain predictable results following ARP. Future randomized controlled trials that can compare different ratios between the two biomaterials are indicated to guide clinicians in the mixing protocols and their outcomes.
Tooth extraction often leads to alveolar ridge atrophy to various degrees.1 During the spontaneous healing process after extraction, the bundle bone on the buccal crest of the extraction socket loses its function and is resorbed and replaced by a combination of woven and lamellar bone. This results in thinner buccal bone compared to the lingual/palatal bone. This horizontal resorption can manifest as vertical reduction of the buccal wall leading to the relocation of the center of the alveolar ridge to a more lingual/palatal position that is unfavorable for implant placement.2 Approximately 30% of ridge width is lost within the first 12 weeks and 50% of horizontal bone width is lost up to 1 year after extraction.3,4
Successful implant therapies rely on adequate hard- and soft-tissue contours.5 Approximately 2 mm of buccal bone and 1 mm of palatal/lingual bone is required for optimal implant placement to ensure adequate bone surrounding the implant after the initial remodeling.6 When the extraction site is left to heal spontaneously, a buccal concavity is often observed, resulting in a loss of alveolar ridge width and height, which could be further impacted by anatomic, prosthetic, metabolic, functional, and/or genetic factors.5 To minimize ridge dimension loss after extraction, alveolar ridge preservation (ARP) procedures are performed, which are aimed at preserving ridge dimensions after tooth extraction.7 Such procedures are necessary for implant site development to ensure adequate ridge width and height for implant placement in a restoratively driven position. Additionally, ARP procedures could maintain adequate soft-tissue contours at the extraction site, thereby serving esthetic purposes.5
ARP involves the use of hard-tissue biomaterials, such as bone grafts, and often may also utilize soft-tissue biomaterials, such as membranes. The primary role of bone grafts is to act as a space maintainer and promote bone regeneration in the socket via osteogenesis, osteoinduction, or osteoconduction.8 Four major sources of bone graft materials are used for regeneration: autogenous, allogenic, xenogenic, and synthetic.Autogenous bone graft is considered the "gold standard" for regeneration because of its osteogenic potential, which other sources do not have. However, its fast resorption rate and the need for an additional surgical site make it an undesirable option for ARP.9 Allogenic bone grafts include freeze-dried bone allograft (FDBA) and demineralized FDBA (DFDBA). FDBA is primarily osteoconductive in nature and acts as a scaffold permitting capillary proliferation and migration of host progenitor cells to begin the process of new bone formation.10 Because of its osteoconductive nature, FDBA appears to show a slow resorption rate and thus the ability to maintain dimensional stability.11 DFDBA also possesses osteoconductive properties, but the process of demineralization allows for the release of bone morphogenic proteins, which makes DFDBA the only allograft that is osteoinductive in nature.12 Additionally, allografts also could be cortical or cancellous in nature. Cortical bone grafts are dense and have a highly organized structure, which allows for structural integrity and slower resorption. This organized structure, though, causes the cortical bone graft to lack cellularity and limits its osteoinductive properties. Cancellous bone graft has a larger trabecular surface area that encourages revascularization and incorporation at the recipient site.12,13 These grafts, however, also can be distributed as a mix of demineralized-mineralized and cortico-cancellous bone to utilize properties of each graft. In comparison to autografts and allografts, xenografts are osteoconductive with a slow bone turnover rate and are thus conducive to maintaining long-term volume stability.14
Combining different types of bone grafts to utilize their desirable properties is common practice.15 Most typically, autografts are combined with xenografts or allografts to obtain osteogenic and osteoinductive or osteoconductive properties. While the combination of allograft and xenograft is frequently used for bone augmentation in daily practice, there is limited literature available for the mixing protocols of various bone grafts. This combination could be utilized to maximize the osteoinductive potential of an allograft and the slow bone turnover rate of a xenograft, which could lead to increased differentiation and proliferation of osteogenic cells and long-term volume stability, especially in socket walls with bony defects.16
Considering the limited evidence on the topic of allograft mixed with xenograft, the aim of this case series is to highlight the clinical and radiographic outcomes of a combined allograft and xenograft approach for alveolar ridge preservation to facilitate optimal site development for future implant placement.
Methods
This case series comprised clinical cases in which extraction of restoratively and/or periodontally hopeless teeth was performed, followed by ARP using a combination of allograft and xenograft bone substitute prior to implant placement. All cases were treated in a private practice setting and the surgeries were performed by the same clinician, following standard-of-care procedures. This dataset was extracted as de-identified information, in compliance with the Health Insurance Portability and Accountability Act (HIPAA) requirements. Digital photographs were obtained with a Canon® EOS R7 camera during the procedures and securely stored on a HIPPA-compliant platform upon each appointment to monitor progress.
Inclusion criteria for the patients recruited for the surgical procedures were age >18 years; healthy or controlled systemic conditions; absence of periodontal disease or clinically stable periodontal disease; tooth to be extracted due to caries, endodontic failure, fracture, or chronic periodontal disease; future implant placement planned; bleeding on probing (BOP) index <10%; and plaque-free score >90%. The following exclusion criteria were applied: immunocompromised patient; current smoker; pregnant; complete absence of buccal bone upon extraction.
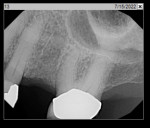
All patients received a comprehensive full-mouth periodontal examination prior to the surgical procedure. This examination included recording of probing depths, attachment loss, BOP, plaque scores, mobility, and furcation involvement, a set of full-mouth radiographs taken within 5 years of the clinical examination, and a recent periapical radiograph of the tooth to be extracted prior to the surgical procedure.
Alveolar Ridge Preservation Procedure
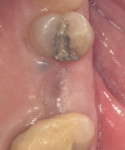
Comprehensive aseptic and sterilization procedures were followed. A thorough review of each participant's medical history was performed prior to the ARP surgical procedure. All patients were anesthetized using local anesthesia (lidocaine 2%, epinephrine 1:100,000) via buccal and lingual/palatal infiltration based on the location of the tooth to be extracted. Teeth were extracted atraumatically using periotomes, elevators, and forceps.
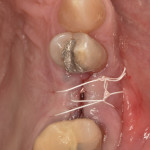
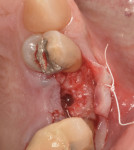
After tooth extraction, the site was degranulated to ensure removal of all granulomatous tissue. The socket walls were assessed using a periodontal probe. In all cases, a combination of allogenic bone granules or fibers (vallos®, Geistlich, geistlich.us) and xenogenic bone granules or block (Bio-Oss® or Bio-Oss® Collagen, Geistlich) was used. The bone graft was hydrated and placed in the extraction site in a 1:1 ratio. The allogenic bone promotes osteoinductive properties and the turning over of natural bone more rapidly, however it lacks volume stability, which may be needed in certain clinical situations. The xenogenic bone promotes long-term bone-volume stability and acts as a scaffold for bone vascularization and new bone formation. The bone graft materials were mixed and hydrated with saline, the patient's blood, or recombinant human platelet-derived growth factors (Lynch Biologics, lynchbiologics.com). A type I collagen matrix (Mucograft® Seal, Geistlich) was used in clinical cases where the socket walls were intact. Alternatively, a type III collagen non-cross-linked membrane (Bio-Gide®, Geistlich)was used in clinical cases presenting with a buccal plate dehiscence or fenestration.
The surgical site was sutured using an internal cross-mattress suturing technique with 5-0 monocryl or nonresorbable 4-0 polytetrafluoroethylene (PTFE) sutures. For pain management, amoxicillin 500 mg three times a day was prescribed for 7 days, including over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs). Patients were advised to start ice application for 24 hours and avoid chewing in the area. Postoperative follow-up data was collected at least 14 days and 120 days after extraction.
Implant Placement Procedure
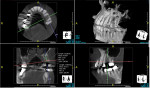
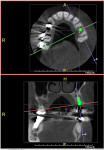
Four to six months after the ARP procedure was completed, all patients received a cone-beam computed tomography (CBCT) scan before implant placement for evaluation of bone condition and surgical implant planning. The final restorative plan was confirmed integrating a digital implant planning procedure.
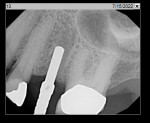
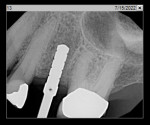
All implant procedures were initiated following standard aseptic protocols. The surgical site was anesthetized using two carpules of 2% lidocaine, 1:100,000 epinephrine via buccal and lingual/palatal infiltration. Full-thickness mucoperiosteal flaps were elevated following a midcrestal incision. The osteotomy was initiated using a spear drill followed by a 2.2 mm twist drill. Periapical radiography was updated with a guide pin to verify angulation. The osteotomy was then completed to the final implant size following manufacturer's recommendations, and the implant was placed to its final position using a surgical handpiece. A cover screw was placed on implants with primary stability <25 Ncm, and a healing abutment was placed on implants with primary stability >25 Ncm. Mucoperiosteal flaps were surgically closed using 4-0 PTFE sutures utilizing a simple interrupted suturing technique.
Results
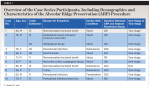
Eleven clinical sites from 10 participants were included in this study, with the patients' ages ranging from 27 to 85 years. Five participants identified as male while five identified as female. The reasons for tooth extraction included hopeless periodontal prognosis, endodontic failure, subgingival decay, and tooth fractures. Upon careful examination of the participants' self-reported medical history, hypertension was the most prevalent condition, while two participants presented with history of cancer and one presented with diabetes, which was well-controlled.
Upon tooth extraction, seven sockets were intact, three presented with dehiscences, and one presented with fenestration. At least 120 days elapsed between ARP and implant placement for nine patients. Implant placement was deferred for one patient due to a medical condition that recommended to delay the procedure. For the former nine patients, dental implants were placed an average of 196 days, with a minimum of 126 days and a maximum of 364 days, after ARP. One implant was placed with a two-stage approach, while all other cases received a one-stage implant approach (Table 1).
All patients were seen for a postoperative follow-up appointment no sooner than at least 14 days after ARP. In all the clinical cases, healing was uneventful and the patients reported minor swelling, discomfort, or pain, which reportedly subsided by days 5 through 7. All extraction/ARP sites presented with adequate (>2 mm) keratinized tissue thickness and width. Radiographic assessment on CBCT, taken at least 3 months after ARP, showed complete radiographic bone fill. No additional hard-tissue augmentation procedures were needed at the time of implant placement.
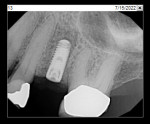
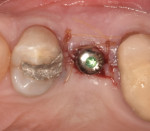
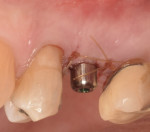
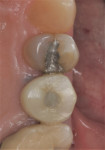
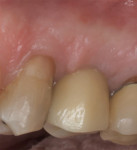
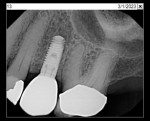
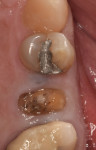
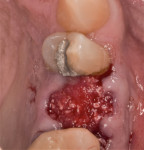
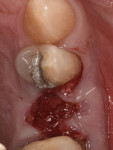
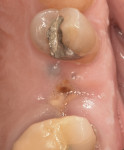
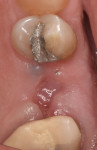
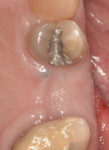
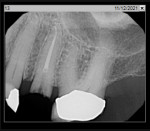
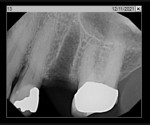
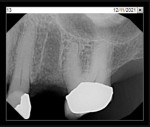
A representative case (patient case No. 1) depicting both the ARP and implant placement procedures is presented. Figure 1 through Figure 9 show the various stages of the bone grafting procedure, Figure 10 and Figure 11 display the digital implant planning, and Figure 12 through Figure 19 show the implant placement procedure. Second-stage implant uncovery and final restoration are depicted in Figure 20 through Figure 24.
Discussion
This case series reports on the clinical and radiographic outcomes following ARP utilizing a combination of allogenic and xenogenic bone substitute in a mixing approach. These clinical cases demonstrate that a mix of allogenic and xenogenic bone substitute can be successfully used to achieve and retain ridge dimensions following tooth extraction allowing for optimal implant placement. Furthermore, implants were placed at different follow-up periods ranging from 3 months to 7 months. At all timepoints, primary stability was achieved and the implant was able to be restored successfully within, on average, 3 months after implant placement.
While studies reporting the use of combined allograft and xenograft for ARP procedures are limited, the present study's findings are in agreement with the sparse literature on this topic. In a study by Poulias et al comparing the clinical and histological outcomes of sockets treated with a mineralized cancellous allograft alone and a mineralized cancellous allograft with a facial xenograft overlay, the results showed significantly higher prevention of ridge width loss and preservation of buccal contour with the combination layering technique.17 At the crest, the allograft alone group resulted in a mean loss of 1.6 mm of ridge width, whereas the allograft and layered xenograft group had a mean loss of 0.3 mm of ridge width. Meanwhile, 5 mm apical to the crest, the allograft alone group lost a mean of 0.8 mm ridge width and the combination group gained a mean of 0.5 mm of ridge width. Histologically, at 4 months the socket group healed with 35% vital bone and 13% non-vital bone, and the overlay socket group had 40% vital bone and 17% non-vital bone with no significant differences between the two groups.17 In the present study, complete radiographic bone fill was observed during CBCT imaging at a minimum of 4 months after implant placement.
Serrano et al compared the clinical and histomorphometric outcomes of a combination of allograft and xenograft utilizing a 50/50 and a 70/30 xenograft/allograft ratio using a mixing approach. The results of the study at 4 months reported a mean vertical gain of 1 mm at the center of the socket area and a loss of 1.6 mm of bone width. The histological analysis revealed a large variability in tissue proportions of new bone and residual new bone ranging from 1.8% to 35.2% and residual biomaterial between 5.5% and 45.8%.18 Similarly, the use of a 50/50 allograft/xenograft mixing approach in the present study resulted in successful implant placements with primary stability at a minimum of 4 months without the need for additional grafting.
ARP is a surgical procedure to preserve the alveolar ridge dimensions and help facilitate optimal implant placement. Because of the limited availability and high resorption rate of autografts, despite their osteogenic potential, they are rarely used as a bone graft of choice for ARP. Allografts have been widely used for the purpose of ARP either alone or in conjunction with autografts. Allografts are available as cancellous, cortical, cortico-cancellous, and freeze-dried bone graft and demineralized freeze-dried bone graft.9 Their osteoinductive and osteoconductive properties make them appealing to use for ARP especially in intact sockets where long-term volume stability is not an issue and implants can be placed within 3 months of the ARP procedure.12 Xenogenic bone substitutes alone, due their slow bone turnover rate, have been the graft of choice for lateral sinus augmentation where a large amount of bone regeneration is required.19
Combining different sources of bone grafts has been routinely documented in the literature. Borg and Mealey compared the use of FDBA and a combination of FDBA and DFDBA for ARP; there were no clinically significant differences observed, however the combination group showed a larger percentage of new bone and a lower percentage of residual biomaterials.12 In a randomized trial comparing 50/50 cortico-cancellous FDBA to a 100% cortical or cancellous FDBA in ARP, no difference was noted between the groups regarding percentage of vital bone or connective tissue.11 Wang et al introduced the concept of a layering bone graft/"sandwich technique" for bone regeneration utilizing xenograft and allograft. Their rationale was to utilize a slowly resorbing outer layer of grafting material to resist resorption and a rapidly resorbing inner graft layer that would be replaced by newly formed bone faster, resulting in more vital bone for implant placement in the center of the socket.15
After tooth extraction, the socket condition may present with either an intact socket wall, dehiscence or fenestration, or missing buccal wall.20 Complete bone regeneration of the bony defect or missing wall requires adequate time for osteoblasts to repopulate and regenerate bone. The moderate bone turnover rate of solely allografts could lead to inadequate bone regeneration in the socket, resulting in deficient ridge dimensions for implant placement. A combination of allograft and xenograft may be needed to allow for osteoinduction along with long-term volume stability.18 Therefore, combining xenogenic bone graft and allogenic bone graft in extraction sockets may be beneficial in the long term, leading to appropriate regeneration of the bony wall, which, in turn, could reduce the chances of the need for additional augmentation at the time of implant placement.
Conclusion
This case series highlights the use of mixing allogenic and xenogenic bone substitutes to acquire the desirable properties of varying bone substitutes for predictable alveolar ridge preservation procedures. Future randomized controlled trials that can compare different ratios between the two biomaterials are indicated to guide clinicians in the mixing protocols and their outcomes.
Acknowledgment
Annie Siliang Li completed this work as a 2022 Laidlaw Scholar at Tufts University. The authors would like to thank the team at Brookline Periodontal Associates, Brookline, Massachusetts, for their support with this project, especially Doreen Barton and Velita Person.
Disclosure
Drs. Shaikh and Dragan serve as speakers for Geistlich Pharma North America on an ad hoc basis.
About the Authors
Samar Shaikh, BDS, MS
Assistant Professor of Periodontology, Tufts University School of Dental Medicine, Boston, Massachusetts
Annie Siliang Li
2022 Laidlaw Scholar, Tufts University School of Dental Medicine, Boston, Massachusetts
Irina F. Dragan, DDS, DMD, MS, eMBA
Adjunct Associate Professor of Periodontology, Tufts University School of Dental Medicine, Boston, Massachusetts; Lecturer, Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts; Private Practice limited to Periodontology and Implant Dentistry, Brookline, Massachusetts
References
1. Couso-Queiruga E, Weber HA, Garaicoa-Pazmino C, et al. Influence of healing time on the outcomes of alveolar ridge preservation using a collagenated bovine bone xenograft: a randomized clinical trial. J Clin Periodontol. 2023;50(2):132-146.
2. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32(2):212-218.
3. Hämmerle CH, Araújo MG, Simion M; Osteology Consensus Group 2011. Evidence-based knowledge on the biology and treatment of extraction sockets. Clin Oral Implants Res. 2012;23(suppl 5):80-82.
4. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
5. Darby I, Chen S, De Poi R. Ridge preservation: what is it and when should it be considered Aust Dent J. 2008;53(1):11-21.
6. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 suppl:43-61.
7. American Academy of Periodontology. Glossary of Periodontal Terms. AAP website. https://members.perio.org/libraries/glossary?ssopc=1. Accessed August 11, 2023.
8. Pagni G, Pellegrini G, Giannobile WV, Rasperini G. Postextraction alveolar ridge preservation: biological basis and treatments. Int J Dent. 2012;2012:151030. doi: 10.1155/2012/151030.
9. Position paper: periodontal regeneration. J Periodontol. 2005;76(9):
1601-1622.
10. Goldberg VM, Stevenson S. Natural history of autografts and allografts. Clin Orthop Relat Res. 1987;(225):7-16.
11. Demetter RS, Calahan BG, Mealey BL. Histologic evaluation of wound healing after ridge preservation with cortical, cancellous, and combined cortico-cancellous freeze-dried bone allograft: a randomized controlled clinical trial. J Periodontol. 2017;88(9):860-868.
12. Borg TD, Mealey BL. Histologic healing following tooth extraction with ridge preservation using mineralized versus combined mineralized-demineralized freeze-dried bone allograft: a randomized controlled clinical trial. J Periodontol. 2015;86(3):348-355.
13. Roberts TT, Rosenbaum AJ. Bone grafts, bone substitutes and orthobiologics: the bridge between basic science and clinical advancements in fracture healing. Organogenesis. 2012;8(4):114-124.
14. Araújo M, Linder E, Wennström J, Lindhe J. The influence of Bio-Oss Collagen on healing of an extraction socket: an experimental study in the dog. Int J Periodontics Restorative Dent. 2008;28(2):123-135.
15. Wang HL, Misch C, Neiva RF. "Sandwich" bone augmentation technique: rationale and report of pilot cases. Int J Periodontics Restorative Dent. 2004;24(3):232-245.
16. Molnár B, Jung AK, Papp Z, et al. Comparative analysis of lateral maxillary sinus augmentation with a xenogeneic bone substitute material in combination with piezosurgical preparation and bony wall repositioning or rotary instrumentation and membrane coverage: a prospective randomized clinical and histological study. Clin Oral Investig. 2022;26(8):5261-5272.
17. Poulias E, Greenwell H, Hill M, et al. Ridge preservation comparing socket allograft alone to socket allograft plus facial overlay xenograft: a clinical and histologic study in humans. J Periodontol. 2013;84(11):1567-1575.
18. Serrano CA, Castellanos P, Botticelli D. Use of combination of allografts and xenografts for alveolar ridge preservation procedures: a clinical and histological case series. Implant Dent. 2018;27(4):467-473.
19. Urban IA, Nagursky H, Lozada JL, Nagy K. Horizontal ridge augmentation with a collagen membrane and a combination of particulated autogenous bone and anorganic bovine bone-derived mineral: a prospective case series in 25 patients. Int J Periodontics Restorative Dent. 2013;33(3):299-307.
20. Frost NA, Banjar AA, Galloway PB, et al. The decision-making process for ridge preservation procedures after tooth extraction. Clin Adv Perio. 2014;4(1):56-63.



![Figure 14 Fig 14. Implant placement (after guide pin
placement [not shown] had been done to verify angulation).](/media/thumbnail/103292/150x150)