In-Office CAD/CAM Coronal Treatment With Lithium Disilicate Achieved in Efficient, Predictable Manner
Ashton A. Prince, DMD
ABSTRACT
As patient demand for faster, streamlined, and convenient treatments increases, clinicians need to be prepared to provide accurate, esthetic, and predictable restorative solutions that meet these requirements. Among the many options currently available in coronal treatments utilizing a digital workflow, the author's practice has found that the use of a certain lithium-disilicate block in tandem with a self-adhesive resin cement provides such a solution. This case report demonstrates the use of CAD/CAM dentistry with in-office milling to restore a failed No. 14 full-coverage crown.
As CAD/CAM procedures become increasingly mainstream in dental offices worldwide, the advancements being made in this area of dentistry are nothing short of remarkable. Simultaneous to these technological improvements being made, clinical practitioners need to keep up with the expectations of patients regarding their treatments. The use of social media and the simple process of word of mouth has created an environment where clinicians need to be able to provide solutions that are faster, more accurate, more esthetic, and more predictable than ever before.
The author's practice has found that the use of GC Initial® LiSi lithium-disilicate blocks (GC America, gcamerica.com) in conjunction with G-CEM ONE™ self-adhesive resin cement (GC America) provides such solutions as he and his team have navigated their way through the many options currently available in coronal treatments with a digital workflow. The team has also found the use of G-CEM ONE adhesive enhancing primer to provide a greater success rate in situations where retention has been a concern.
The GC Initial LiSi block comprises the manufacturer's fully crystallized proprietary High-Density Micronization lithium disilicate as the basis for the block, which allows for a coronal restoration to be milled in the author's office in the practice's mill in 8 to 14 minutes without the need to fire the restoration. For the practice's workflow, this approach has created a savings of 20 to 30 minutes in the treatment process when compared to other materials that must be milled and then fired. The restoration can then be polished, chemically treated, and ready to seat in as quickly as 3 to 4 minutes after the milling is complete. The use of the aforementioned G-CEM ONE adhesive enhancing primer also greatly helps in areas where retention is less than ideal, as it assists in creating a more idyllic bond, aiding the self-adhesive cement.
Clinical Case, Procedures, and Results
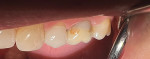
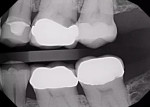
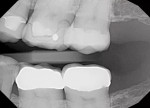
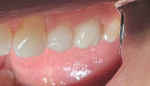
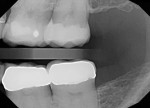
A 52-year-old female patient presented to the author's (ie, clinician's) practice with a failed No. 14 full-coverage crown that had recurrent decay on the distal margin and a failed buccal margin that had been treated with a composite restoration (Figure 1). A radiograph taken at the start of the appointment showed the extent of the breakdown (Figure 2). A discussion was then had with the patient about the concern for endodontic involvement. A periapical image was also taken and endodontic testing was performed with normal results. However, the potential for nerve exposure was present and the patient was made aware of the circumstances.
After application of local anesthetic, the clinician removed the crown by sectioning the restoration with a buccal-to-lingual cut and separated the crown from the tooth with a surgical elevator. While many devices and instruments can be used to remove crowns, with some being more aggressive than others, the clinician has found that an elevator can be very fast in breaking the previous cementation.
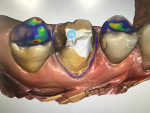
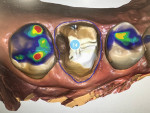
For this case, the previous preparation was then adjusted to include the decayed area. The clinician routinely uses a caries indicator to instill confidence that the bonding will be made to a stable surface, which was done in this case. The clinician intentionally tries to minimize adjustments as much as possible to conserve tooth structure, but if retention can be improved by decreasing the angle of the preparation walls, or undercuts can be filled in with a restorative material, these easy steps can help create a more predictable result. The easier the practitioner can make it for scanning and milling, the better the resulting restoration will likely be (Figure 3 and Figure 4).
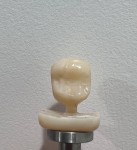
Many patients at the author's practice are fascinated by the milling process (CEREC® MC XL, Dentsply Sirona, dentsplysirona.com) and enjoy watching their crowns being "created" right before their eyes in only a short time (Figure 5 through Figure 9). Once the milling process is completed, the restoration receives an initial polish with Dialite® polish (Brasseler USA, brasselerusa.com) and a goat hair polishing wheel to make the try-in more accurate in relation to what the final result will be (Figure 10). Also, a "pre-cementation" radiograph is taken to ensure a proper seal and ideal outcome (Figure 11).
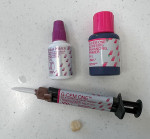
Because the restoration in this case had a proper fit and was comfortable, the final preparatory steps for the cementation were started (Figure 12). Minor adjustments were needed to the occlusal contacts, thus the restoration was polished again. Although retention was not a concern for this case, the intaglio surface of the GC Initial LiSi restoration nonetheless was treated with hydrofluoric acid (9.5%) for 20 seconds and then with G-Multi Primer (GC America) to further prepare the restoration for enhanced bonding with the G-CEM ONE cement. Sandblasting was not used with the GC Initial LiSi restoration so as to avoid possible microfractures.
It was now time to place the restoration, and because the clinician was confident of achieving a quality result, G-CEM ONE self-adhesive resin cement was applied around the margin and within the core of the restoration, with immediate seating. In the author's experience, applying an excess of material to achieve a "bleed out" of the cement when seating is ideal for clean-up with this very thin (5 μm) material (Figure 13). With the excess cement present, a 1-second tack light-cure was done while moderate pressure was applied to the restoration. The excess cement material was then removed with a hand instrument, and the interproximal contacts were cleaned out with floss that was pulled out horizontally from the contact. This was done to provide predictable contact cleaning without dislodging the restoration with a vertical removal of the floss.
Next, the material was fully cured using a calibrated curing light, even though the restoration could have been left alone for 4 minutes with continued pressure applied for a self-setting process. The occlusal contacts and excursions were then double-checked after cementation to ensure the patient would be as comfortable as possible with the result. As is typical for the clinician with this procedure, no postoperative sensitivity was experienced, and the blend of material with the tooth was impressive. A radiograph exhibiting the final restoration post-cementation is shown in Figure 14.
Discussion
This particular case was ideal for the process and protocol used for several reasons. First, the preparation did not require excessive reduction after removal of the previous crown in order to gain the necessary depth for a CAD/CAM crown. Second, the margins were clear for the scan. Third, because the patient had to travel more than an hour to get to the office, she was in need of an immediate restoration. Saving her the need to take off more time from work and not having to travel back to the office at a later date for final cementation was a great benefit to the patient. She continually expressed amazement and excitement with regard to how much better the experience was compared to her previous treatments from 25 years ago. Because clinicians can predictably offer a faster and more accurate procedure with modern-day products compatible with CAD/CAM protocols, such as those used in this case, they are able to treat patients in their offices with improved quality and care.
The digital workflow demonstrated in this case is conducive to allowing practitioners to experience a more stress-free and enjoyable career while keeping patients engaged in improving their oral health. This case is one of many the author has successfully completed utilizing these materials. To quote Maya Angelou, "When you know better, do better." As dental professionals learn and understand more, they can constantly improve, for both themselves and their patients.
DISCLOSURE
This article was commercially supported by GC America.
ABOUT THE AUTHOR
Ashton A. Prince, DMD
Adjunct Faculty, ACT Dental; Private Practice, St. George, Utah