A Systematic Approach to Full-Mouth Rehabilitation of a Complex Case Using a Digital Workflow, Proper Isolation
Adamo E. Notarantonio, DDS
Abstract: To achieve excellence in dentistry, a multitude of steps needs to be completed. From performing a thorough history, to diagnosis and treatment planning, all the way to accurate insertion of the restorations, every aspect of the restorative process requires careful thought and precision, especially in a complex case. This article describes a stepwise approach to completing a full-mouth rehabilitation using an entirely digital approach. Additionally, it discusses ideal measures of isolation and bonding as pertaining to all-ceramic restorations. Through utilizing a systematic strategy, the clinician can establish a predictable path to ensure a successful result.
Patients sometimes present with conditions that seem extremely daunting to restore. In some cases the oral environment may appear destroyed to the point where the clinician may wonder how he or she can possibly restore the dentition artificially with long-term success when patients have destroyed what was given to them naturally. Although it may often appear to be an overwhelming task, restoring broken-down dentitions can indeed be accomplished successfully when one follows a systematic approach based on history, diagnosis and treatment planning, and precise execution in delivering provisionals1 and permanent restorations.
History, Communication, Execution
When patients present with massive destruction in their mouth, it is important that clinicians not simply focus solely on what needs to be done mechanically to restore the patient back to health. Taking such an approach can lead to further problems long term. When a patient presents with considerable damage, rather than rushing into the restorative process, sufficient time should be spent on obtaining an accurate medical and dental history in order to ascertain the source of the problems.2 Even though the clinician may be capable of delivering acceptable esthetic and functional results, if the reason(s) for the destruction is not discovered and addressed, the problems likely will inevitably return and destroy the new restorative work, as history is bound to repeat itself.3
When working on complex rehabilitations, the clinician's communication with the dental laboratory is critical. Whether using an analog or digital technique,4 proper dental photography,5 records, and an in-depth lab prescription6 need to be given to the laboratory in order for there to be any chance of attaining a successful result. Often times multiple conversations will be needed to ensure that both parties are in agreement throughout the entire process. In the author's experience, failing to sufficiently communicate with the lab can lead to undesirable, and even catastrophic, outcomes.
In dental practice today, all-ceramic restorations and adhesive dentistry are highly prevalent.7,8 These materials have shown to function well in complex cases with long-term success. However, in order to achieve such success, ideal execution during insertion is crucial. It has been clearly demonstrated that a major reason for bond failures is a contaminated field.9-11 Insertion of ceramic restorations using an adhesive protocol can best be achieved with rubber dam isolation. In the author's opinion, the technique used for inserting the final restorations is as paramount as the pathway that was used to arrive at that point, and total rubber dam isolation when utilizing adhesive protocols is essential.
Case Example
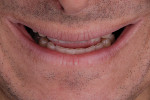
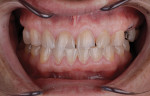
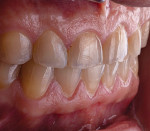
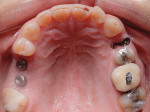
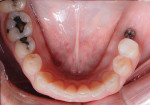
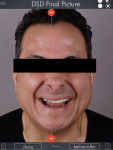
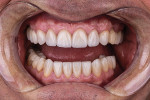
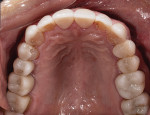
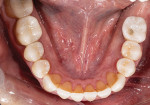
A 58-year-old man initially presented to the author's office for emergency care on tooth No. 19. Initial evaluation revealed multiple missing teeth and severe wear/occlusal issues (Figure 1 through Figure 5). Following emergency treatment, which involved extraction of tooth No. 19, an appointment was made for the patient at which an in-depth analysis of his personal, medical, and dental history was completed. The patient reported a personal history of dental neglect and stated that he typically went to the dentist only for emergency care.
He also reported a history of hypertension but said it had resolved with weight loss and diet. On one treatment visit when he presented for extractions, however, his blood pressure was 180/110 mm Hg. He claimed he had just come from a fitness workout, but due to the high blood pressure reading he was dismissed from the dental visit. He returned the next day for the same procedure but once again recorded a blood pressure of 180/110 mm Hg. He was immediately sent to his physician where he was placed on 50 mg of losartan daily. His hypertension subsequently was under control.
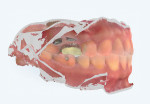
At his new patient hygiene appointment the patient had also reported a dental history of localized bleeding in an area (upper left quadrant) where an overhung amalgam existed. He also reported a history of decay, fractured teeth, and lost fillings. After completing a detailed analysis of all the data and performing a periodontal, biomechanical, functional, and dentofacial risk assessment,12 the clinician constructed a treatment plan, which the patient approved. At this appointment, intraoral scans were taken with the patient in maximum intercuspation (MIP) (Figure 6) in order to fabricate a Kois deprogrammer (Kois Center, koiscenter.com), which is designed to prevent interlocking of the teeth and thereby allow the patient's lower jaw to gradually relax and settle into an ideal position in relation to the teeth. MIP was notable because, since it was coincident with centric relation (CR), and the patient answered "no" to all bite and joint questions, this indicated that he currently was in acceptable function. In this case, vertical dimension was being altered, and the deprogrammer would allow the clinician to move the joint position to CR.
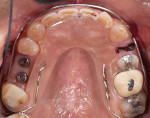
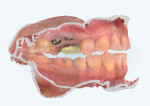
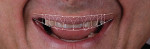
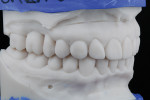
At the subsequent visit the deprogrammer was delivered (Figure 7) and the patient was instructed to wear it at all times except when eating. An appointment was scheduled 2 weeks later and the patient was instructed to come to the office as soon as he woke up without removing the deprogrammer so that a CR bite could be recorded.13 A second scan with the deprogrammer was sent to the laboratory with instructions to return one upper model mounted on an articulator along with a lower model mounted in MIP, and a second set of models mounted in CR. This would allow the operator to see if there was any discrepancy between MIP and centric occlusion. In this case there was no discrepancy, and because the patient denied any orthodontics, the CR position at an open vertical dimension (Figure 8) was utilized as the starting reference point for the full-mouth rehabilitation.14
After taking many more photographs, the clinician had an in-depth conversation with the laboratory regarding the maxillary teeth in terms of position. The lab then sent a 2-dimensional smile design (Figure 9 and Figure 10), and, following approval, the maxillary design was converted to a 3-dimensional model (Figure 11).15-17 The mandibular arch was functionally developed via a digital pathway following completion of the maxillary arch. The lab was then instructed to send one set of models with only the upper and lower six anteriors completed along with a provisional matrix for each, and then a second set of models with both arches completed and a provisional matrix for each arch as well.
On the day of provisionalization, the entire mouth was completed at the same time with rough preparations on each tooth, allowing for enough room for provisional material.18 These restorations were permanently cemented in so the patient could avoid having temporaries dislodge while test driving the new esthetic and occlusal scheme. The patient remained in these provisionals for 12 weeks, with weekly evaluations to check for chipping, pain, and other potential issues. These provisionals serve as the "road map" toward the final restorations, as they are duplicated exactly, assuming the esthetics and function are ideal. After this analysis, the decision was made to proceed with the final restorations.
The author's sequence toward final lithium-disilicate restorations begins with the upper and lower anteriors under absolute isolation. By "absolute" isolation, the author is referring to isolation of individual teeth with the appropriate gauge rubber dam so that ideal inversion is achieved, as well as utilizing accessory clamps for proper retraction. Each step in a complex case like this one, from core build-up, to preparation design, to final insertion (Figure 12 through Figure 14) should be done with the same precision as the diagnosis and planning. In this case, a heavy-gauge latex dam was used. Heavy-gauge was used because in the author's experience it does an outstanding job of inverting itself, retracts the soft tissue, and prevents saliva or blood from coming through the sulcus. Accessory clamps can be utilized for further tissue retraction. Although there is not an abundance of evidence that supports the use of rubber dam, many practitioners feel it is an absolute necessity. Celine Higton, BDS, may have said it best19: "Do we need to see evidence that supports the use of a parachute? No, but I know for sure I want to use one if I ever jump out of a plane."
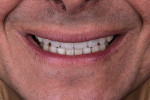
In the present case, after the upper and lower anteriors were completed, the upper posterior was done under the same isolation and bonding protocols as the upper and lower anteriors.20,21 The lower posterior teeth are treated last, because if the anteriors happen to be a bit constricted, which may occur sometimes, this allows the option of opening the vertical dimension by utilizing the lower posteriors without affecting the upper functional and esthetic arch form.22 In this particular case there was no need to open the vertical dimension any further. The final restorations are depicted in Figure 15 through Figure 18.
Follow-up for this patient, as with most full-mouth rehabilitation cases by the author, included 3-month recare appointments. Caries management with anticavity toothpaste (CTx4™ gel, Carifree, carifree.com) was also a part of this patient's follow-up.
Conclusion
Meticulous record-taking, diagnosis, planning, and execution are critical in complex cases. With good communication and an excellent laboratory partner, difficult situations can be diagnosed and treated with precision and predictability. Such cases may take time, and clinicians must resist the urge to take shortcuts.
Acknowledgment
The author thanks Midwest Dental Arts Laboratory (midwestdentalarts.
com) for the outstanding work in this case from start to finish.
About the Author
Adamo E. Notarantonio, DDS
Clinical Instructor, Honors Program in Aesthetic Dentistry, New York University College of Dentistry, New York, New York; Fellow, American Academy of Cosmetic Dentistry; Private Practice, Huntington, New York
References
1. Keys WF, Keirby N, Ricketts DNJ. Provisional restorations - a permanent problem? Dent Update. 2016;43(10):908-914.
2. Nakagawa B. When single-tooth dentistry fails: a comprehensive approach to manage risk and restore function. Compend Contin Educ Dent. 2020;41(3):164-169.
3. Glebocki J. Correction of dysfunctional wear results in esthetic outcome for reluctant patient. Compend Contin Educ Dent. 2019;40(5):302-306.
4. Seay A. Utilizing digital technology to facilitate dentofacial integration. Compend Contin Educ Dent. 2018;39(10):696-704.
5. Weston JF, Haupt E. Creating aesthetic success through proper clinician and laboratory technical communication. Dent Clin North Am. 2011;55(2):371-382.
6. Leith R, Lowry L, O'Sullivan M. Communication between dentists and laboratory technicians. J Ir Dent Assoc. 2000;46(1):5-10.
7. Butt K, Thanabalan N, Ayub K, Bourne G. Demystifying modern dental ceramics. Prim Dent J. 2019;8(3):28-33.
8. Blatz MB, Chiche G, Bahat O, et al. Evolution of aesthetic dentistry. J Dent Res. 2019;98(12):1294-1304.
9. Eiriksson SO, Pereira PN, Swift EJ, et al. Effects of blood contamination on resin-resin bond strength. Dent Mater. 2004;20(2):184-190.
10. Eiriksson SO, Pereira PN, Swift EJ Jr, et al. Effects of saliva contamination on resin-resin bond strength. Dent Mater. 2004;20(1):37-44.
11. Shimazu K, Karibe H, Oguchi R, Ogata K. Influence of artificial saliva contamination on adhesion in class V restorations. Dent Mater J. 2020;
39(3):429-434.
12. Kois DE, Kois JC. Comprehensive risk-based diagnostically driven treatment planning: developing sequentially generated treatment. Dent Clin North Am. 2015;59(3):593-608.
13. Wiens JP, Goldstein GR, Andrawis M, et al. Defining centric relation. J Prosthet Dent. 2018;120(1):114-122.
14. Calamita M, Coachman C, Sesma N, Kois J. Occlusal vertical dimension: treatment planning decisions and management considerations. Int J Esthet Dent. 2019;14(2):166-181.
15. Cervino G, Fiorillo L, Arzukanyan AV, et al. Dental restorative digital workflow: digital smile design from aesthetic to function. Dent J (Basel). 2019;7(2):30.
16. Stanley M, Paz AG, Miguel I, Coachman C. Fully digital workflow, integrating dental scan, smile design and CAD-CAM: case report. BMC Oral Health. 2018;18(1):134.
17. Coachman C, Calamita MA, Sesma N. Dynamic documentation of the smile and the 2D/3D digital smile design process. Int J Periodontics Restorative Dent. 2017;37(2):183-193.
18. Sesemann M. Diagnostic full coverage provisionals for accurately communicating esthetic and functional. Functional Esthetic Restorative Dentistry. 2008;2(2):8-14.
19. Higton C. Rubber dam isolation: the cornerstone of modern dentistry. Lecture presented virtually at: Penn Dental Medicine Excellence in Restorative Dentistry Lecture Series; February 16, 2021.
20. Krummel A, Garling A, Sasse M, Kern M. Influence of bonding surface and bonding methods on the fracture resistance and survival rate of full-coverage occlusal veneers made from lithium disilicate ceramic after cyclic loading. Dent Mater. 2019;35(10):1351-1359.
21. Maluly-Proni AT, Oliveira-Reis B, Jardim VR, et al. Influence of the application and light-curing of bonding adhesives inside lithium disilicate ceramic crowns. Eur J Prosthodont Restor Dent. 2020;28(2):65-74.
22. Dawson PE. Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007.