Maximizing Esthetics While Preserving Bone and Tooth Structure in a Young Adult Patient Utilizing Digital Technologies
Ellen Pikus-Katz, DDS
Abstract: As digital workflows become increasingly common in dentistry, clinicians are able to quickly demonstrate esthetic possibilities to their patients and easily implement the digitally designed outcome. In this case presentation of a young patient, it was critical to maintain maximum tooth structure and alveolar bone when treating her esthetic concerns. Chairside confirmation of the proposed treatment plan, coupled with careful multidisciplinary consultations, led to improved oral health and an excellent esthetic outcome without increasing the patient's risk for future disease.
Digital techniques in dentistry are rapidly advancing, aiding clinicians in providing enhanced patient care. However, it is important that clinical confirmation and evaluation of digital processes are part of the dentist's workflow. In complex cases, such as the one presented here in which a six-phase treatment plan was implemented, thorough diagnosis and accurate risk assessment are essential to obtain an optimal outcome. The case describes a facially driven treatment plan in which minimally invasive, adhesively retained veneers were used to address a young woman's frustration with her smile.
Clinical Case Overview
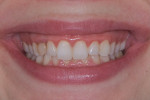
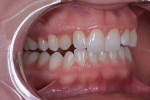
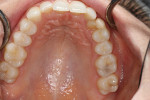
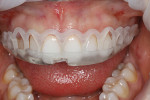
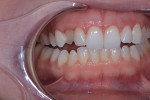
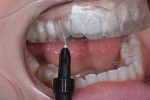
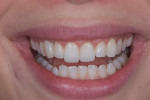
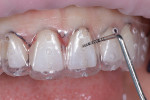
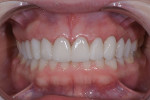
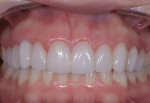
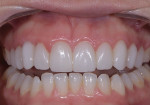
A 25-year-old patient presented with the chief concern that she did not like her smile (Figure 1 and Figure 2). She had received two rounds of orthodontic treatment over 7 years and had never been satisfied with the outcome. Tooth No. 6 was partially erupted.1 An unesthetic bonded composite restoration cantilevered from tooth No. 5 had been placed to mask the appearance of tooth No. 6. The restoration contours led to food impaction and prevented flossing in the area (Figure 3 and Figure 4). She requested natural-looking teeth, less gingival display when smiling, and an upper right cuspid that did not catch food and was cleansable.
Medical and Dental History
The patient's medical history was negative except for a penicillin allergy, resulting in an American Society of Anesthesiologists (ASA) I classification. On the dental history form, she reported that she wanted to change the appearance of her teeth, had previously bleached her teeth, was self-conscious about the appearance of her teeth, and had been disappointed with the esthetic look of previous dental work. All other dental history questions were negative.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: The alveolar bone levels were within 2 mm of the cementoenamel junction. All pocket depths were 4 mm or less, with generalized bleeding on probing. Generalized heavy biofilm deposits were noted. The free gingival margins were moderately inflamed. She was diagnosed with American Academy of Periodontology (AAP) stage I, grade A.
Risk:Low, with moderate for teeth Nos. 5 through 7
Prognosis: Good
Biomechanical: The only restorations present were occlusal composites on teeth Nos. 3 and 19, which had been placed within the past year. Class I interproximal carious lesions were noted on the posterior teeth in all quadrants.2 Radiographs from 3 years prior were reviewed, and no changes in the appearance of the lesions were noted. The patient had no history of interproximal caries. Tooth No. 6 was partially impacted with intact enamel.
Risk: Low
Prognosis: Good
Functional: The patient had no functional concerns and gave no positive responses to any dental history questions concerning function. She had full range of mandibular motion with no deviation upon opening or closing, and her dentition exhibited no wear. She had a diagnosis of acceptable function.
Risk: Low
Prognosis: Excellent
Dentofacial: The patient presented with excessive lip mobility and excessive gingival display. With the lips in repose, the left cuspid displayed +1 mm of tooth structure.3 The bonded restoration on tooth No. 6 was short, so it was not used for evaluation.
Risk: High
Prognosis: Poor or hopeless
Treatment Goals
The patient's main concern was excessive tooth and gum display. A comprehensive orthodontic consult was obtained, which included the option to move tooth No. 6 into proper position. The patient refused further orthodontic treatment due to the required length of treatment time as well as her previous disappointment with orthodontic outcomes. She accepted a treatment plan comprised of crown lengthening and porcelain veneers. Digital treatment planning procedures would be used for planning both the crown lengthening and restorative phases of treatment. Tooth No. 6 would be restored to a length and contour that would be esthetically pleasing and allow good oral hygiene in the area.
Treatment Plan
The treatment plan would be carried out in six phases:
Delay restorative treatment until gingival inflammation resolved. Implement at-home caries prevention.
Create a facially driven treatment plan. Design and insert a trial smile to verify the proposed tooth position and gingival margins both esthetically and during speech.
Perform periodontal crown lengthening surgery using a surgical guide created and printed from the final CAD software design (exocad, exocad.com).
Create a provisional bonded composite restoration for tooth No. 6 using a chairside injection molding technique to allow the patient to floss and also to determine if tooth No. 6 possessed adequate exposed enamel to reliably retain an adhesive restoration.
Place minimally invasive, adhesively retained veneers on teeth Nos. 4 through 13.
Develop and implement ongoing preventive protocols.
Treatment Phases
Phase 1
The patient received full-mouth scaling and was provided detailed oral hygiene instructions. She was placed on an anticavity rinse (CTx4 Treatment Rinse, CariFree, carifree.com) and returned monthly for periodontal and gingival assessment. After 3 months, the tissue was healthy, and her oral hygiene continued to be effective. She was then appointed to begin the next phase of treatment.
Phase 2
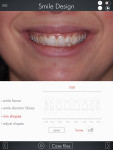
Six full-face and six close-up photographs were taken while the patient wore glasses (Kois Facial Reference Glasses, Kois Center, koiscenter.com) designed to standardize the recording of the maxillary occlusal plane while capturing dynamic lip movement.4 Photographs were taken with the lips in repose, with the patient saying "shush," and with a wide (Duchenne) smile (Figure 5).5 The photographs were transferred into the digital smile design app (DSD, Digital Smile Design, digitalsmiledesign.com), and a 2-dimensional smile was created to demonstrate how the patient's smile might look (Figure 6). She was pleased with the proposed changes and agreed to proceed with treatment.
The 12 photographs along with a video that was made of the patient "being herself" while talking and laughing were used to create the facially driven treatment plan. The video captured her lip movement in a natural, dynamic environment. After both the patient and clinician reviewed multiple frames and further discussed the treatment plan, it was determined that the Duchenne smile revealed a lip mobility of 8 mm and best captured the patient's natural smile. The gingival margin would be raised 2 mm and the buccal corridor widened to meet her esthetic goals. The lower anterior tooth display was acceptable. Due to her class II division 2 malocclusion, the central incisors were retroclined. Using lateral facial photographs, the position of the lips and incisors in relation to the SNA (sella, nasion, A point) angle was measured, and it was determined that the middle and incisal thirds of the central incisors needed to be proclined 2 mm to provide esthetic lip support. These changes could be accomplished primarily with additive adhesive dentistry.
A 3-dimensional design was then created in exocad. The upper and lower arches were scanned, and a maximum intercuspation (MIP) bite was used, as the patient had acceptable function. After reviewing and refining the exocad files, the models were printed and putty provisional stents were made.
The patient returned for placement of the intraoral trial smile. A glycerin-based gel (DeOx™, Ultradent, ultradent.com) was placed over the existing teeth to facilitate easy removal. A bisacryl provisional material (Luxatemp®, DMG America, dmg-america.com) was placed in the putty matrix and inserted in the mouth. Once the material was set, photographs and a video were taken to evaluate the proposed smile from all perspectives. The patient's speech was also evaluated to ensure that it was not impacted by the proposed length and angulation of the teeth. Upon resolution of all esthetic and functional concerns, the trial smile was scanned.
The scanned trial smile, photographs, and video were uploaded to an iPad® tablet for review. It was determined that the gingival margin on the upper left side should be raised and the final tooth shape and size slightly modified. The desired changes were drawn on the iPad using Procreate® (Savage, procreate.art) to allow a detailed discussion via Zoom video conferencing among the dentist, ceramist, and digital designer. This step enabled careful evaluation of the patient's primary concern of excessive gingival display. After final approval, a surgical guide with the final gingival margin position was fabricated.
Phase 3
This phase involved periodontal surgery with a surgical guide. A consult with the periodontist was completed, and a clear resin surgical guide was printed using the trial smile information. The superior margin of the guide was located 3 mm above the desired position of the gingival margin, which was delineated by the lower border of the guide (Figure 7).
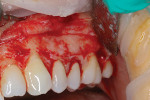
The periodontist used the guide to mark the new gingival margins with a laser. He then identified the distance from the desired gingival margin location to the osseous crest and reduced the bone as necessary to avoid any biologic width violation (Figure 8).6 A full-thickness flap and a papilla-sparing technique was used. The patient reported no postoperative pain.
Phase 4
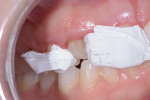
During the 12-week postoperative healing period, the existing composite was removed from tooth No. 6 (Figure 9). An injection molding technique was used to directly bond a provisional composite restoration to tooth No. 6. A clear acrylic matrix (EXACLEAR, GC America, gcamerica.com) was made from the 3D wax-up. Teeth Nos. 5 and 7 were isolated with polytetrafluoroethylene tape (Figure 10). Tooth No. 6 was acid-etched for 15 seconds, rinsed, and dried. Bonding agent (All-Bond Universal®, BISCO, ) was applied, air-dried, and light-cured. An opening was made in the matrix at the incisal to exactly fit the composite syringe tip. Composite (G-aenial™ Universal Injectable, GC America) was injected through the incisal hole starting at the gingival margin and moving incisally (Figure 11). The provisional composite restoration on tooth No. 6 was contoured to facilitate flossing, enhance esthetics, and confirm that there was adequate supragingival enamel to retain the restoration (Figure 12).
Phase 5
Next came the definitive restorations phase. At the tooth preparation appointment, teeth Nos. 4 through 13 were minimally prepared to preserve enamel. To minimize tooth structure removal, a reduction guide based on the final trial smile was created by the dental laboratory (Figure 13). Bisacryl provisional material (Luxatemp) was placed in the provisional putty matrix and inserted over the maxillary teeth. Depth cuts were made in the provisional overlay. Little to no buccal reduction was necessary since the buccal corridor was to be widened.
After the preparations were done, 000 cord was placed and a final impression was taken using a putty and light-body technique (Panasil® Putty Soft and Panasil® Initial Contact Light, Kettenbach Dental, kettenbach-dental.us). A bite registration was taken (Futar®, Kettenbach Dental), the shade of the prepared teeth was recorded, and bisacryl provisionals (Luxatemp) were made using a putty matrix created from the 3D wax-up and then luted in place with a spot-etch and spot-bond (All-Bond Universal) technique. Any repairs or additions to the provisionals were done with a repair composite (LuxaFlow®, DMG America). The gingival embrasures of the provisionals were contoured to allow optimal oral hygiene (Figure 14).
The patient returned 1 week later for evaluation of oral hygiene and careful assessment of the function, occlusion, and esthetics of the provisional restorations, as these serve as a valuable blueprint to guide the fabrication of the definitive restorations. The provisional restorations required no esthetic or functional changes. To improve the cleansability of the restorations, the gingival embrasures were widened with a mosquito extra-fine carbide bur. Home care instructions were reviewed and emphasized with the patient to help ensure that the gingival tissue would remain free of inflammation.
Once the gingival embrasure widening changes were made and the patient gave final approval to her new smile, the provisionals were scanned with an intraoral scanner (i500, Medit, medit.com), then photographs and videos were taken to aid the laboratory in creating the final restorations.
The patient returned 4 weeks later for placement of lithium-disilicate glass-ceramic veneers (IPS e.max®, Ivoclar Vivadent, ivoclar.com). A lithium-disilicate-based press ingot (Amber® Press LTW2, Hass, hassbio.com) was used with GC Initial® LiSi micro-layering (GC America). She reported no problems with the provisional restorations, and the gingival tissue was healthy. The veneers were adhesively placed with a luting composite (Variolink® Esthetic LC, Ivoclar Vivadent). The occlusion was evaluated in MIP, followed by a functional evaluation with the patient sitting up and biting on blue 200-µm articulating paper. All blue streaks were removed on the central and lateral incisors to ensure that no friction was present in the chewing envelope. Post-treatment photographs are shown in Figure 15 through Figure 17.
Phase 6
A recall interval of every 4 months was recommended, which could increase to a 6-month interval if the patient maintains excellent oral hygiene and gingival health. A daily at-home fluoride regimen (CTx4 Gel 1100, CariFree) was recommended after completion of the restorative treatment due to the presence of the enamel decalcifications.
Conclusion
The use of digital techniques in dentistry is progressing swiftly, but clinical confirmation and evaluation of digital processes are critical elements to include in the restorative workflow. Careful diagnosis and risk assessment, as demonstrated in this complex case, will help clinicians provide the best outcomes.
ACKNOWLEDGMENTS
The author thanks John Kois, DMD, MSD, for support, guidance, structure, mentorship, and restorative systems; Edgard El Chaar, DDS, MS, for excellent periodontal skills and collaboration on this case; Jean Martin, DDS, MPH, for editing and being a motivator; and Justin McElroy and Jimmy So of Midwest Dental Arts Laboratory for beautiful indirect ceramic restorations and digital design.
About the Author
Ellen Pikus-Katz, DDS
Co-Clinical Director, Full Mouth Rehabilitation CE course, and Adjunct Clinical Instructor, Department of Cariology and Comprehensive Care, New York University College of Dentistry, New York, New York; Private Practice, Manalapan, New Jersey, and New York, New York
References
1. Coslet JG, Vanarsdall R, Weisgold A. Diagnosis and classification of delayed passive eruption of the dentogingival junction in the adult. Alpha Omegan. 1977;70(3):24-28.
2. Pitts NB, Ekstrand KR, ICDAS Foundation. International Caries Detection and Assessment System (ICDAS) and its International Caries Classification and Management System (ICCMS) - methods for staging of the caries process and enabling dentists to manage caries. Community Dent Oral Epidemiol. 2013;41(1):e41-e52.
3. Misch CE. Guidelines for maxillary incisal edge position - a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
4. Kois JC, Kois DE, Zeitler JM, Martin J. Digital to analog facially generated interchangeable facebow transfer: capturing a standardized reference position. J Prosthodont. 2021; doi: 10.1111/jopr.13437.
5. Walter RD, Goodacre BJ, Goodacre CJ, et al. A comparison of gingival display with a requested smile, Duchenne smile, grimace of disgust, and funnel-shaped expression. J Prosthet Dent. 2014;112(2):220-227.
6. Nugala B, Kumar BS, Sahitya S, Krishna PM. Biologic width and its importance in periodontal and restorative dentistry. J Conserv Dent. 2012;15(1):12-17.