Rapid Anti-gingivitis Efficacy of a Novel Stannous Fluoride Dentifrice: Results From a 12-week Randomized Controlled Clinical Trial
Malgorzata Klukowska, DDS, PhD; Yuanshu Zou, PhD; Daniel Ponce, DDS; and Pejmon Amini, DDS
ABSTRACT
Objective: To assess the anti-gingivitis and anti-plaque efficacy of a novel bioavailable stannous fluoride (SnF2) dentifrice to a negative control. Methods: This was a 12-week randomized, controlled, double-blind, two-treatment, parallel group clinical study. One hundred generally healthy adults with evidence of plaque and gingivitis were enrolled into the study. Subjects were randomly assigned to one of two dentifrice treatments: (1) novel SnF2 dentifrice containing the amino acid glycine as a stabilizing chelant (Procter & Gamble) or (2) a negative control sodium monofluorophosphate dentifrice. Gingivitis was assessed using the Löe-Silness Gingivitis Index (LSGI) at baseline, Week 1, and Week 12 while plaque was evaluated according to the Turesky Modification of the Quigley-Hein Plaque Index at baseline and Week 12. Results: One hundred subjects completed the trial. Subjects using the novel SnF2 dentifrice demonstrated statistically significantly fewer bleeding sites and a lower LSGI score versus those using the negative control as early as Week 1 (P < .001). The benefit increased throughout the study, with the SnF2 dentifrice showing 33.4% fewer bleeding sites and a 16.5% lower LSGI score versus the negative control at Week 12 (P < .001). Subjects with localized or generalized gingivitis (≥10% bleeding sites) had 6 times better odds of transitioning to generally healthy (<10% bleeding sites) after using the SnF2 dentifrice for 12 weeks versus the negative control. Plaque scores for the SnF2 dentifrice were also statistically significantly lower (P < .001) than those for the negative control at Week 12. Conclusion: The novel SnF2 dentifrice with the amino acid glycine produced statistically significant improvements in gingival health that were seen as early as 1 week and numerically increased throughout the study.
Stannous fluoride (SnF2) has a long history of use in dentistry. The ingredient was originally added to toothpastes as an anti-caries agent.1 SnF2 has also proven to be a useful antimicrobial ingredient for the control of plaque and gingivitis.2-4 Today, the majority of marketed over-the-counter dentifrices in the United States5 with labeled indications for gingivitis prevention/treatment are based on SnF2 technology (eg, Crest® Pro-Health™, Colgate® TotalSF, Parodontax™, and others).
While SnF2 is clinically effective, dentifrices containing the ingredient are difficult to prepare. Formulators must take care to control deactivation of available and bioavailable SnF2 during preparation and storage.6-8 Historically, a number of technical approaches have been applied to improve the stability and efficacy of SnF2 in antimicrobial formulations. One approach to improve SnF2 bioavailability is to use anhydrous glycerin gels where Sn2+ loss due to hydrolysis and oxidation is largely avoided. Water-based formulations containing cleaning abrasives are considerably more difficult to prepare because SnF2 availability can be reduced by abrasive adsorption, hydrolysis, or oxidation. One approach to account for this is to add secondary sources of stannous (so-called reservoirs) such as stannous chloride to boost SnF2 bioavailability.6 Abrasives can also be selected that have lower adsorption affinities for stannous. Lastly, a variety of chelant molecules can be added. Chelants act to form soluble molecular complexes with stannous and are effective in limiting stannous loss to hydrolysis. Suitable chelants added to formulations have included gluconate, citrate, pyrophosphate, hexametaphosphates, and zinc phosphate.6-9
One of the challenges to the application of chelants to formulations with SnF2 is balancing the stabilizing actions of chelants on SnF2 availability (the concentration of soluble stannous in the formulations) while maintaining adequate bioavailability (the reactivity of stannous with biofilm bacteria in dental plaque). For example, it can be challenging for cationic antimicrobial molecules (stannous is positively charged) to penetrate plaque biofilms as there is a tendency for these molecules to be bound on the surface of the dental plaque and not adequately penetrate.10 It is important that formulation components including chelants facilitate to the degree possible SnF2 reactivity including biofilm penetration.
Recently, a new formulation approach for SnF2 dentifrices has been discovered that includes the incorporation of the amino acid glycine as a stabilizer for SnF2. In laboratory experiments, formulations of SnF2 with added glycine promoted more rapid uptake, deeper penetration, and improved retention of SnF2 within plaque biofilms as compared to SnF2 absent glycine chelant.11 Selected formulations showed up to 80% increases in stannous colocalization with plaque bacteria as compared to control formulations.11
The purpose of this study was to establish the plaque and gingivitis efficacy of a novel 0.454% SnF2 dentifrice with the amino acid glycine, as compared to a negative control dentifrice.
Methods and Materials
This was a 12-week randomized, controlled, two-treatment, parallel-group, double-blind clinical study to compare anti-gingivitis and anti-plaque efficacy of a novel 0.454% SnF2 dentifrice stabilized with amino acid glycine versus a negative control dentifrice. This study was reviewed and approved by an IRB (study #2019051).
The study population comprised 100 generally healthy adults with established clinical plaque and gingivitis. To participate in this study subjects were required to have at least 16 gradable teeth and more than 20 bleeding sites. Subjects were excluded from participation if they used antibiotic, anti-inflammatory, or anti-coagulant medications or anti-gingivitis/anti-bacterial oral care products within 2 weeks of the baseline visit. Other exclusion criteria included self-reported pregnancy or lactation or fixed facial or lingual orthodontic appliances on gradable teeth.
At the baseline visit, a medical history review, demographic information, and inclusion/exclusion criteria were verified and qualifying subjects underwent a gingivitis (Löe-Silness Gingivitis Index12 [LSGI]) and dental plaque (Turesky Modification of the Quigley-Hein Plaque Index13 [TMQHPI]) evaluation. All clinical evaluations were conducted by a licensed dentist trained and qualified in clinical grading methods.14,15 Subjects were stratified based on their baseline LSGI score, number of bleeding sites, whole mouth TMQHPI score, age, and gender and randomly allocated to one of two treatment groups using an encoded program:
· Group 1: SnF2 dentifrice: 0.454% SnF2 stabilized with amino acid glycine (Crest®Pro-Health™Advanced Gum Restore Toothpaste,The Procter & Gamble Company, crest.com)
· Group 2: Negative control: 0.76% sodium monofluorophosphate dentifrice (Colgate® Cavity Protection Toothpaste, Colgate-Palmolive, colgate.com)
Both of the groups received a soft manual toothbrush (Oral-B Indicator, The Procter & Gamble Company) to use together with the assigned toothpaste. Products were over-labeled for blinding purposes and dispensed in a protected area, separate from clinical grading.
Subjects were instructed both verbally and via written instructions to brush thoroughly, twice daily for 1 minute per brushing. The first brushing was done under the supervision of study personnel to ensure compliance. All subjects were instructed to use only the assigned products in place of normal oral hygiene for the duration of the study.
After 1, 2, and 12 weeks of product use subjects returned to the site for gingivitis and plaque evaluations (plaque was assessed at week 12 only). At each visit, continuance criteria were reviewed and a comprehensive oral examination was conducted. General comments and any adverse events (AEs) were recorded.
Clinical Evaluations
Oral Soft-Tissue Evaluation
Assessment of the oral soft tissue was conducted via a visual examination of the oral cavity and perioral area utilizing a standard dental light, dental mirror, and gauze. The structures examined included the gingiva (free and attached), hard and soft palate, oropharynx/uvula, buccal mucosa, tongue, floor of the mouth, labial mucosa, mucobuccal/mucolabial folds, lips, and perioral area. Assessment of the oral hard tissues was conducted via a visual examination of the dentition and restorations utilizing a standard dental light, dental mirror, and air syringe. All abnormal findings and/or AEs were recorded.
Gingivitis Index
The LSGI12 was used to evaluate gingival health on six gingival areas per tooth based on color, consistency, and bleeding upon probing ranging from 0 to 3. The entire dentition, with the exception of the third molars, was evaluated yielding a maximum of 168 sites. Bleeding scores were derived from the LSGI scores at each site. Gingival bleeding site scores were assigned a value of 0 if the GI score was 0 or 1, and a value of 1 if the GI score was a 2 or 3. A full-mouth bleeding score was determined by summing the bleeding scores over all evaluable sites.
Dental Plaque Clinical Examinations
The TMQHPI13 was used to evaluate the dental plaque levels at baseline and week 12. Subjects rinsed with Trace® Disclosing Solution (Young™ Dental, youngdental.com) prior to grading. Plaque areas were scored on six surfaces per tooth (mesiofacial, facial, distofacial, mesiolingual, lingual, and distolingual) according the following index below, summarized and divided by the number of graded teeth for an average score per subject:
Score Criteria
0 No plaque
1 Isolated areas of plaque at gingival margin
2 Thin band of plaque at gingival margin less than 1 mm
3 Plaque covering up to 1/3 tooth surface
4 Plaque covering between 1/3 and 2/3 tooth surface
5 Plaque covering >2/3 of tooth surface
Statistical Analysis
Sufficient subjects were screened to randomize 100, with a goal of 94 subjects (47 per arm) completing the study, allowing for a 5% non-completion rate. It was determined that 47 subjects per group would allow for a treatment difference of 9.86 in number of bleeding sites, 0.11 in LSGI and 0.30 in whole mouth TMQHPI to be detected with at least 90% power in a two-sided two sample t-test of significance level 0.05 assuming group standard deviation of 13.78, 0.15, and 0.42. These differences were based on results from a prior study at the same site.
Baseline subject demographic data were compared between test groups via analysis of variance (ANOVA) for age and Fisher’s exact test for gender and ethnicity. Summary statistics (eg, means, standard deviations, frequencies, etc) of the demographic characteristics as well as efficacy measurements were calculated for each treatment group and visit. The efficacy statistical analyses were based on whole mouth average LSGI scores, the number of bleeding sites using bleeding scores, and whole mouth average TMQHPI scores. A paired t-test was used for comparisons to baseline for each index within each treatment group for each post-baseline visit. Using analysis of covariance (ANCOVA) with the corresponding baseline score as a covariate, a statistical between-treatment group comparison was conducted at each post-baseline visit. Statistical tests were two-sided using a 5% significance level. The primary comparison was number of bleeding sites at the week 12 time point.
The current Gingivitis Case Definition from the 2017 World Workshop in Periodontology was used to classify subject-level gingival bleeding at baseline and the 12-week visit: generally healthy (<10% bleeding sites), localized gingivitis (10% to 30% bleeding sites), or generalized gingivitis (>30% bleeding sites).16 Transition rates by treatment were then calculated and used to generate odds ratios with 95% confidence intervals.
Results
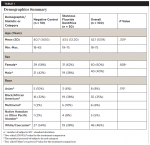
Demographic characteristics of study subjects are summarized in Table 1. One hundred subjects were initially enrolled in the study. Subjects were evenly balanced for all demographic characteristics between assigned treatment groups(P ≥ .176). All subjects completed the trial. The mean age (standard deviation [SD]) of subjects was 42.1 years (13.19) and 60% were female. Forty-six subjects (46%) were Caucasian, 35 subjects (35%) were Black, 8 subjects (8%) were Asian, 6 subjects (6%) were Multiracial and 5 subjects (5%) were Native Hawaiian or Other Pacific Islander.
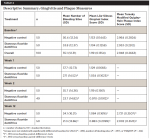
Table 2 presents descriptive summaries of number of bleeding sites, LSGI scores, and TMQHPI scores throughout the study. At baseline, subjects were balanced for all gingivitis and plaque measures (P ≥ .282). Subjects using the novel SnF2 dentifrice produced statistically significant (P < 0.001) reductions in number of bleeding sites and LSGI scores from baseline at week 1, week 2, and week 12. Subjects using the negative control dentifrice only exhibited a statistically significant benefit from baseline for reduction in LSGI scores at week 12 (P = .005). For plaque, both the novel SnF2 dentifrice group and the negative control group demonstrated statistically significantly lower (P < .001) mean overnight TMQHPI scores at week 12 versus baseline.
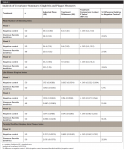
Comparisons of clinical indices for the novel SnF2 and negative control are shown in Table 3. Subjects using the SnF2 dentifrice exhibited statistically significantly reduced number of bleeding sites, LSGI scores, and TMQHPI scores compared to the negative control at each evaluation period, with the gingival benefit increasing in magnitude from week 1 to week 12. At the week 12 evaluation, the number of gingival bleeding sites, LSGI scores, and TMQHPI scores for subjects using the novel SnF2 dentifrice were reduced by 33.4%, 16.5%, and 25.6%, respectively, compared to the negative control dentifrice.
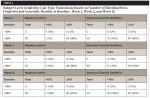
All of the study subjects were classified as being localized or generalized gingivitis case types (≥10% bleeding sites) at baseline (Table 4). Of the 50 subjects in the SnF2 treatment group with localized or generalized gingivitis at baseline, 10 (20%) had already transitioned to generally healthy at week 1 compared to only 1 subject (2%) in the negative control group. By week 2, 31% of subjects in the SnF2 group had transitioned to generally healthy compared to only 4% in the negative control group. After 12 weeks, 40% of subjects in the SnF2 group were classified as generally healthy while only 10% of subjects in the negative control group had improved to generally healthy. These transitions indicate that subjects with localized or generalized gingivitis had 12.3 times better odds (95% CI [1.5, 99.8]) of shifting to generally healthy using SnF2 versus a negative control at week 1, 10.6 times better odds (95% CI [2.3,49.4]) at week 2, and 6 times better odds (95% CI [2.8,12.9]) at week 12.
Treatments were well tolerated and there were no dropouts or safety issues.
Discussion
SnF2 dentifrice stabilized with the amino acid glycine was observed to produce significant reductions in gingival inflammation and bleeding as compared to the negative control dentifrice at all clinical measurement points, including as early as the 1-week assessment. The efficacy of the novel SnF2 dentifrice in this study further supports the general effectiveness of SnF2 in a variety of formulations for suppression of gingivitis and promotion of gingival health.2-4 SnF2 is an antibacterial fluoride, unlike sodium monofluorophosphate, and its sustained antimicrobial properties contribute to its ability to reduce plaque regrowth and improve gingival health.8
The potential for improved penetrability of SnF2 from optimized formulations may be clinically significant based upon contemporary discoveries concerning the mechanism of action of SnF2. A clinical study has demonstrated that SnF2 can penetrate into subgingival crevicular fluid and stannous is retained in subgingival plaque.17 SnF2 has been shown to decrease biofilm virulence via attaching to lipopolysaccharide and lipoteicoic acid molecular patterns on bacterial surfaces interfering with pathogen stimulation of toll receptors,18,19 the latter of which are associated with the initialization of the inflammatory processes involved in periodontal disease.20-26 Samples of plaque from subgingival areas in subjects brushing with SnF2 dentifrice have been shown to exhibit decreased virulence ex vivo.27,28 In addition, SnF2 formulations have been shown to reduce bacterial metabolic products, including short chain fatty acids propionic and butyric acid, which are derived from bacterial metabolism in deeper parts of plaque biofilms in anaerobic environments.29 As mentioned earlier, laboratory studies with the SnF2 dentifrice and the amino acid glycine dentifrice have shown increased uptake in plaque biofilms versus positive control SnF2 without glycine.11
The effect of SnF2 on plaque biofilm translates into reduction of bleeding on probing, which may be clinically important to the gingival health of patients. The absence of sulcular bleeding over repeated dental examinations has been shown to be a reliable predictor for the maintenance of periodontal health, as measured by lack of attachment loss.30-35 New guidelines were recently proposed to establish clinical criteria associated with periodontal health and diseases.16 Patients with <10% bleeding sites, without attachment loss and radiographic bone loss, were defined as periodontally healthy; patients with bleeding sites ranging from 10% to 30% were defined as suffering from localized gingivitis; patients with gingivitis levels greater than 30% of sites were defined as having generalized gingivitis. Based on these definitions, subjects on average starting this clinical trial presented with localized gingivitis with baseline levels of gingivitis averaging close to 20% of graded sites. As quickly as 1 week into the trial, 20% of patients using the SnF2 dentifrices improved to gingival health status, compared to only 2% of those using the negative control, as defined by the guidelines proposed by the World Workshop on Periodontal Diseases.16 This translates to 12.3 times greater odds of moving to generally healthy for the SnF2 dentifrice versus the negative control. The percentage of subjects using SnF2 with the amino acid glycine who transitioned to generally healthy doubled to 40% following 12 weeks of brushing, signifying 6 times greater odds of improving to generally healthy status compared to the negative control. These odds of transitioning to generally healthy status are above the range that has been reported with use of SnF2 dentifrice without the amino acid glycine as a stabilizer.3
Conclusion and Clinical Implications
In this randomized clinical trial, the novel SnF2 dentifrice with the amino acid glycine demonstrated statistically significant gingival health improvements as early as 1 week that numerically increased during the trial. These findings indicate SnF2 dentifrice stabilized with the amino acid glycine may represent an important advance in dentifrice technology to improve gingival health of patients.
ACKNOWLEDGMENT
The authors acknowledge Alborz Amini, ChE; Erinn Conde, BS; Theresa Fafard; and Marsha Gabbard, AA, for assistance with study execution and data analysis, and Donald J. White, PhD, for manuscript preparation.
DISCLOSURE
The study was funded by The Procter & Gamble Company. Drs. Klukowska and Zou are employees of The Procter & Gamble Company.
ABOUT THE AUTHORS
Malgorzata Klukowska, DDS, PhD
Clinical Scientist-Dentist, The Procter & Gamble Company, Mason, Ohio
Yuanshu Zou, PhD
Senior Scientist/Statistician, The Procter & Gamble Company, Mason, Ohio
Daniel Ponce, DDS
Subinvestigator, Silverstone Research Group, Las Vegas, Nevada
Pejmon Amini, DDS
Principal Investigator,Silverstone Research Group, Las Vegas, Nevada
REFERENCES
1. Makin SA. Stannous fluoride dentifrices. Am J Dent. 2013;26 spec no A:3A‐9A.
2. Valkenburg C, Van der Weijden FA, Slot DE. Plaque control and reduction of gingivitis: the evidence for dentifrices. Periodontol 2000. 2019;79(1):221-232.
3. Biesbrock A, He T, DiGennaro J, et al. The effects of bioavailable gluconate chelated stannous fluoride dentifrice on gingival bleeding: meta-analysis of eighteen randomized controlled trials. J Clin Periodontol. 2019;46(12):1205‐1216.
4. Sanz M, Serrano J, Iniesta M, et al. Antiplaque and antigingivitis toothpastes. Monogr Oral Sci. 2013;23:27-44.
5. Food and Drug Administration. Oral Health Care Drug Products for Over-the-Counter Human Use; Antigingivitis/Antiplaque Drug Products; Establishment of a Monograph; Proposed Rules. US Dept of Health and Human Services; 2003. 21 CFR Part 356.
6. White DJ. A “return” to stannous fluoride dentifrices. J Clin Dent. 1995;6 spec no:29-36.
7. Baig A, He T. A novel dentifrice technology for advanced oral health protection: a review of technical and clinical data. Compend Contin Educ Dent. 2005;26(9 suppl 1):4-11.
8. Myers CP, Pappas I, Makwana E, et al. Solving the problem with stannous fluoride: formulation, stabilization, and antimicrobial action. J Am Dent Assoc. 2019;150:(4S):S5-S13.
9. Li Y, Suprono M, Mateo LR, et al. Solving the problem with stannous fluoride: extrinsic stain. J Am Dent Assoc. 2019;150(4S):S38‐S46.
10. Zaura-Arite E, van Marle J, ten Cate JM. Conofocal microscopy study of undisturbed and chlorhexidine-treated dental biofilm. J Dent Res. 2001;80(5):1436‐1440.
11. Strand R, Shi Y, inventors. Oral care compositions for promoting gum health. US patent 10,596,089 B2. March 24, 2020.
12. Löe H, Silness J. Periodontal disease in pregnancy. I. Prevalence and severity. Acta Odontol Scand. 1963;21:533-551.
13. Turesky S, Gilmore ND, Glickman I. Reduced plaque formation by the chloromethyl analogue of victamine C. J Periodontol. 1970;41(1):41-43.
14. Akwagyiram I, Amini P, Bosma ML, et al. Efficacy and tolerability of sodium bicarbonate toothpaste in subjects with gingivitis: a 6-month randomized controlled study. Oral Health Prev Dent. 2018;16(5):401-407.
15. Amini P, Tao H, Peters J, Farrell S. Clinical plaque and gingivitis effects of bioavailable SnF2 dentifrice. J Dent Res. 2020;99(spec iss A):Abstract 3067.
16. Trombelli L, Farina R, Silva CO, Tatakis DN. Plaque-induced gingivitis: case definition and diagnostic considerations. J Periodontol. 2018;89(suppl 1):S46-S73.
17. Klukowska MA, Ramji N, Combs C, et al. Subgingival uptake and retention of stannous fluoride from dentifrice: gingival crevicular fluid concentrations in sulci post-brushing. Am J Dent. 2018;31(4):184-188.
18. Haught JC, Xie S, Circello B, et al. Lipopolysaccharide and lipoteichoic acid binding by antimicrobials used in oral care formulations. Am J Dent. 2016;29(6):328-332.
19. Haught C, Xie S, Circello B, et al. Lipopolysaccharide and lipoteichoic acid virulence deactivation by stannous fluoride. J Clin Dent. 2016;27(3):84-89.
20. Ginsburg I. Role of lipoteichoic acid in infection and inflammation. Lancet Infect Dis. 2002;2(3):171-179.
21. Hamada S, Takada, H, Ogawa T, et al. Lipopolysaccharides of oral anaerobes associated with chronic inflammation: chemical and immunomodulating properties. Int Rev Immunol. 1990;6(4):247-261.
22. Holt SC, Bramanti TE. Factors in virulence expression and their role in periodontal disease pathogenesis. Crit Rev Oral Biol Med. 1991;2(2):177-281.
23. Madianos PN, Bobetis YA, Kinane DF. Generation of inflammatory stimuli: how bacteria set up inflammatory responses in the gingiva. J Clin Periodontol. 2005;32(suppl 6):57-71.
24. Beutler B, Jiang Z, Georgel P, et al. Genetic analysis of host resistance: toll-like receptor signaling and immunity at large. Annu Rev Immunol. 2006;24:353-389.
25. Hans M, Hans VM. Toll-like receptors and their dual role in periodontitis: a review. J Oral Sci. 2011;53(3):263-271.
26. Takeda K, Akira S. Toll-like receptors in innate immunity. Int Immunol. 2005;17(1):1-14.
27. Klukowska M, Haught JC, Xie S, et al. Clinical effects of stabilized stannous fluoride dentifrice in reducing plaque microbial virulence I: microbiological and receptor cell findings. J Clin Dent. 2017;28(2):16-26.
28. Xie S, Haught JC, Tansky CS, et al. Clinical effects of stannous fluoride dentifrice in reducing plaque microbial virulence III: lipopolysaccharide and TLR2 reporter cell gene activation. Am J Dent. 2018;31(4):215-224.
29. Cannon M, Khambe D, Klukowska M, et al. Clinical effects of stabilized stannous fluoride dentifrice in reducing plaque microbial virulence II: metabonomic changes. J Clin Dent. 2018;29(1):1-12.
30. Lang NP, Adler R, Joss A, Nyman S. Absence of bleeding on probing. An indicator of periodontal stability. J Clin Periodontol. 1990;17(10):714-721.
31. Schätzle, M, Löe H, Bürgin W, et al. Clinical course of periodontitis. I. Role of gingivitis. J Clin Periodontol. 2003;30(10):887-901.
32. Heitz-Mayfield LJ, Schätzle M, Löe H, et al. Clinical course of chronic periodontitis. II. Incidence, characteristics and time of occurrence of the initial periodontal lesion. J Clin Periodontol. 2003;30(10):902-908.
33. Ramseier CA, Anerud A, Dulac M, et al. Natural history of periodontitis: disease progression and tooth loss over 40 years. J Clin Periodontol. 2017;44(12):1182-1191.
34. Schätzle M, Löe H, Lang NP, et al. Clinical course of chronic periodontitis. III. Patterns, variations and risks of attachment loss. J Clin Periodontol. 2003;30(10):909-918.
35. Schätzle M, Löe H, Lang NP, et al. The clinical course of chronic periodontitis. J Clin Periodontol. 2004;31(12):1122-1127.