Implications of Tattoos That Oral Healthcare Providers Should Consider
Mohammed A. Bindakhil, DDS; Thomas P. Sollecito, DMD; and Eric T. Stoopler, DMD
Abstract
Occasionally, a patient may present with an intraoral tattoo, such as the patient in this instance who presented with one on the lower orolabial mucosa. Both extraoral and intraoral tattooing could be considered a potential indicator of risk-taking behaviors and possible increased risk of mental health or sleep disorders in this patient population. This article discusses risks of ornamental tattooing and the role oral healthcare providers can play in early identification of possible systemic diseases.
Tattoos have become increasingly common in Western countries, with the percentage of the population with tattoos ranging from 10% to 30%.1 Motivators for seeking tattoos include body embellishment, ego bolstering, societal inclusion, and camouflage of cutaneous pathology.1 Tattoo placement typically involves the use of a machine that delivers suspensions of pigment ("ink") into the dermis by repeatedly puncturing the skin to a depth of 1 mm to 2 mm.2 Various colors and shades of inks are produced by different combinations of pigments.2
Several complications associated with tattoos have been reported, including infection, inflammation, allergy, and cutaneous malignancies.1,2 Bloodborne infections are a possible consequence of the tattooing process.3 Individuals with body art are more likely to be diagnosed with a mental illness or a sleep disorder and are more likely to engage in risk-taking behaviors than individuals without tattoos.3,4 Drug use, suicidal ideation, and violence are thought to be examples of behaviors that are more common in individuals with tattoos and body piercings.3
This article discusses a rare case of a patient with an intraoral tattoo and describes the role of dentists in identifying risk-taking behaviors and recognizing early stages of mental health disorders.
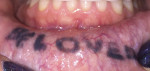
A 35-year-old female patient presented for oral health evaluation, and a tattoo on the lower orolabial mucosa that read "Be Loved" was noted during clinical examination (Figure 1). The patient stated that she had obtained the tattoo 15 years earlier at a time in her life when she was making "poor decisions" and in a moment of what she called "extreme excitement."
The black ink used for the tattoo contained carbon black 7, acrylic resin, and isopropyl alcohol. The patient reported that she had experienced no complications during the tattooing procedure or afterward. Detailed medical, family, and social histories provided no other relevant information. The patient appeared to be emotionally and mentally stable at the time of visit, however she admitted that she maintained a somewhat risker behavior around the age period during which she received the tattoo.
The incidence of facial tattooing is approximately 4%, and intraoral tattoos have been reported to be primarily on gingival tissues.5,6 Certain African cultures have used botanical resins for gingival tattooing of females in order to produce physical attributes regarded as more desirable.6,7 It is unknown whether people with facial tattoos engage in riskier behaviors than those with tattoos in other body areas. Ornamental tattooing of the orolabial mucosa is very rare.5 Successful removal of tattoos from such surfaces using a Q-switched Nd:YAG laser has been reported.5 Methods of removing tattoos from non-cutaneous mucosal surfaces include cryosurgery and dermabrasion.5
Most mental disorders are detected and managed in a primary care setting.8 However, dentists can play an important role in early identification of systemic diseases, including mental disorders, as patients often visit dentists more frequently than physicians.9 Dentists do not require advanced training in the field of mental health to recognize early signs of mental disorders, such as irritability and depression.8,10,11 Obtaining detailed information through the medical history will help dentists identify potential signs of unstable behavior and psychopathology at an earlier stage.10
Dental patients may be reluctant to provide unsolicited information regarding their mental health because they may believe the dentist does not require this type of medical information to provide treatment, or they may feel ashamed.10 This may be overcome through the use of a questionnaire, such as the Patient Health Questionnaire (PHQ), to screen dental patients for common psychiatric illnesses, such as anxiety, depression, and somatization.8,12 Such an approach can reduce the likelihood of dentists being viewed as intruding into uninvited areas of the patient's life when gathering detailed information regarding the patient's mental state.8 When dentists identify troubling behavior that may be psychological in origin, they should promptly refer the patient to an appropriate healthcare provider (eg, psychologist or psychiatrist) for evaluation of mental well-being and proper management.10
Mental health problems may also interfere with provision of dental care.10 For instance, patients with psychopathology may be more likely to have phobic anxiety and more likely to refuse to cooperate with the dentist.10 In addition, these patients may be at higher risk of dental erosion due to potential eating disorders and less likely to conduct adequate self-care and oral hygiene.10 Assessment of the mental health of dental patients allows for appropriate treatment planning and the avoidance of possible treatment complications linked to unstable behavior. It is also important for dentists to closely monitor the emotional health of patients who exhibit risk-taking behaviors and especially recognize suicidal ideation to possibly prevent suicide attempts.8 Oral healthcare providers should regard both extraoral and intraoral tattooing as a potential indicator of risk-taking behaviors and increased risk of mental health disorders in this patient population.
About the Authors
Mohammed A. Bindakhil, DDS
Postdoctoral Fellow, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Thomas P. Sollecito, DMD
Professor and Chairman, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Fellowship in Dental Surgery of the Royal College of Surgeons of Edinburgh (FDS RCSEd)
Eric T. Stoopler, DMD
Professor of Oral Medicine, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Fellowship in Dental Surgery of the Royal College of Surgeons of Edinburgh and England (FDSRCS); Fellowship in Dental Surgery of the Royal College of Physicians and Surgeons of Glasgow (FDSRCPS)
References
1. Kluger N, De Cuyper C. A practical guide about tattooing in patients with chronic skin disorders and other medical conditions. Am J Clin Dermatol. 2018;19(2):167-180.
2. Shinohara MM, Nguyen J, Gardner J, et al. The histopathologic spectrum of decorative tattoo complications. J Cutan Pathol. 2012;39(12):1110-1118.
3. Heywood W, Patrick K, Smith AMA. Who gets tattoos? Demographic and behavioral correlates of ever being tattooed in a representative sample of men and women. Ann Epidemiol. 2012;22(1):51-56.
4. French MT, Mortensen K, Timming AR. Are tattoos associated with employment and wage discrimination? Analyzing the relationships between body art and labor market outcomes. Human Relations. 2019;72(5):962-987.
5. Kirby W, Chen C, Desai A, Desai T. Successful treatment of cosmetic mucosal tattoos via Q-switched laser. Dermatol Surg. 2011;37(12):1767-1769.
6. Brooks JK, Reynolds MA. Ethnobotanical tattooing of the gingiva: literature review and report of a case. J Am Dent Assoc. 2007;138(8):1097-1101.
7. Rawal SY, Burrell R, Hamidi CS, et al. Diffuse pigmentation of maxillary attached gingiva: four cases of the cultural practice of gingival tattoo. J Periodontol. 2007;78(1):170-176.
8. Dworkin SF. The dentist as biobehavioral clinician. J Dent Educ. 2001;65(12):1417-1429.
9. Sun M, Sollecito TP, Stoopler ET. Human papilloma virus vaccinations: primary prevention by dentists. Compend Contin Educ Dent. 2019;40(9):625.
10. de Jongh A, Adair P. Mental disorders in dental practice: a case report of body dysmorphic disorder. Spec Care Dentist. 2004;24(2):61-64.
11. Suka M, Yamauchi T, Sugimori H. Help-seeking intentions for early signs of mental illness and their associated factors: comparison across four kinds of health problems. BMC Public Health. 2016;16:301.
12. Kroenke K, Spitzer RL, Williams JBW, Löwe B. The patient health questionnaire somatic, anxiety, and depressive symptom scales: a systematic review. Gen Hosp Psychiatry. 2010;32(4):345-359.