The Dental Implant Workflow: Choosing a Pathway That Best Serves the Patient and Practice
Eugene Antenucci, DDS
Abstract: Workflows that not only are efficient but also place a high premium on the patient's needs are critical to the production of a dental practice. In this article, the clinician, who himself was being treated for a fractured tooth, was able to evaluate his practice's workflows from a patient's perspective by comparing three workflows to determine the optimum approach to restoring a single implant with a ceramic crown. Factors such as clinical time involved in the workflow process, costs, patient comfort, profitability, and, of course, esthetic results were judged.
Two years ago, I fractured endodontically treated tooth No. 14 while eating hard food. The tooth was nonrestorable. My oral surgeon performed the extraction, and the area was allowed to heal. The preoperative periapical showed only 4 mm of available bone from the ridge crest to the floor of the sinus. Leaving the space unrestored was not an option for me, and now as a patient, I was ready to consider my treatment options.
As a clinician, this was a rare opportunity to evaluate my practice's workflows from a patient's perspective. Essentially, a workflow is a repeatable pattern of activities or steps that relies on the use of resources and processes in a systematic way.1 For every task involving patient care, a dental practice has a workflow. It may be streamlined or it may be "hodge-podge," but it is a workflow, through which a problem is diagnosed and a course of action is determined. For the present case, I decided to approach the situation as a study and "test" three different workflow options to arrive at the same outcome: an esthetically pleasing, functional, and comfortable ceramic crown.
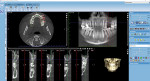
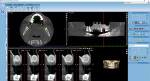
Restorative considerations included a three-unit bridge with Nos. 15 and 13 as abutments, or an implant abutment and crown for No. 14. As I would have recommended to my patients, I opted for the implant. In my case, a sinus graft would be necessary. My oral surgeon took a cone-beam computed tomography (CBCT) scan (Planmeca ProMax® 3D Classic, Planmeca, planmeca.com), and together we evaluated the implant site using Planmeca Romexis® implant planning software (Figure 1). Following the oral surgeon's treatment planning methodology was simple since we both use Planmeca 3D in our practices. A sinus graft was planned and performed in May 2018. The surgery was uneventful, with surprisingly little postoperative pain or concern (Figure 2).
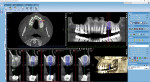
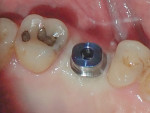
In February 2019, I returned for a preoperative implant planning scan, and using Planmeca Romexis an implant (NobelActive® 5.5-mm x 16-mm, Nobel Biocare, nobelbiocare.com) was virtually placed (Figure 3). The oral surgeon's workflow and mine differ at this point. I routinely use Planmeca Romexis to plan and design a surgical guide to be printed in-office for use during implant surgery. This allows a guided, flapless approach. The surgeon placed the implant after a full-thickness flap, and closed with sutures and a transmucosal healing abutment.
My associate, Ziwei Gao, DDS, and I reviewed the possible methods available to restore the case. We began with the final restoration in mind-a ceramic crown-and arrived at three different pathways to achieve the same desired result:
Physical impression workflows: This is a conventional approach to implant restoration using tray impressions and bite registration, with a laboratory fabricating a custom abutment and crown.
Scanning a stock abutment: This would entail using a stock abutment intraorally and fabricating a crown (e.max®, Ivoclar Vivadent, ivoclarvivadent.com) chairside.
Scanning a scan body with custom abutment fabrication and crown design: A laboratory would fabricate the custom abutment from the scan, design a crown virtually, and send us the abutment along with a STL file to mill the e.max crown in-office.2
Our goal was to see if one workflow was superior to the others from both the patient's and clinician's perspective when restoring a single implant. For each workflow we evaluated the following: clinical time involved in the process, including laboratory or computer time; cost, including laboratory, implant prosthetic components, and materials; perception of comfort during the dental procedure; and esthetic result.
The Impression Workflows
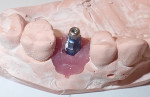
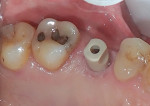
My associate began with a conventional impression, and we purchased an impression abutment for the NobelActive 5.5-mm wide-platform (WP) implant from the manufacturer (Nobel Biocare). The transmucosal cover screw was removed, and the impression abutment was seated and hand-tightened. A plastic tray quadrant was tried in for proper fit. Putty and wash material (Flexitime®, Kulzer, kulzer.com) were used for the closed-tray impression. Mix and set time was 4.5 minutes. A mandibular quadrant tray was used for a lower counter using alginate. A bite registration was taken with vinylpolysiloxane material (Blu Mousse®, Parkell, parkell.com) (45 seconds). The impression abutment was retrieved, and the healing abutment was re-placed.
From my perspective as a patient, the impressions were uncomfortable and annoying, but tolerable. Removing and re-placing the healing abutment and impression abutment was comfortable and tolerable. For Dr. Gao as treating dentist, the workflow was familiar and straightforward.
The impression abutment was joined to its implant analog and placed properly in the impression. With physical impressions, our practice routinely performs this step to assure proper positioning of the analog in the model, and the laboratory is instructed to not remove the impression abutment prior to model pouring. We also routinely pour all alginate impressions immediately and trim the model prior to laboratory packaging. The stone model pouring, set, and finishing took 1 hour, 15 minutes of which was auxiliary time taken to pour and retrieve the model and clean the area, impression tray, and mixing materials. Finally, the impression and model were sprayed with a disinfectant.
A laboratory prescription was prepared and logged, with specific instructions for a custom titanium abutment supporting the soft tissue and a cementable zirconium crown shade A3/A2 with mild occlusal groove characterization. The laboratory (Tetra Dynamics, tetradynamics.com) was instructed to supply all components necessary. After 2 weeks, the abutment and crown were returned. We steam-cleaned and dried them. The abutment was tried in and tightened to 20 Ncm torque. Teflon tape and temporary sealing material (Tempit®, Centrix, centrixdental.com) were used to seal the access. The porcelain-to-zirconium crown was tried in and contacts and occlusion were adjusted. The crown could be luted with a variety of cements.
The process for this workflow is depicted in Figure 4 through Figure 9.
Scanning a Stock Abutment
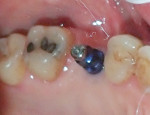
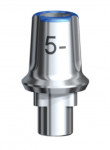
A stock abutment (NobelActive 5.5-mm WP) was placed by Dr. Gao after removal of the healing abutment. This stock abutment has a pre-set tissue contour and finish lines. The tissue area was slightly overcontoured. There was some difficulty in properly positioning and engaging the abutment. Once properly oriented, the abutment seated further, which placed more pressure on the surrounding tissue and caused blanching. This process took longer than placing the impression abutment, and, as a patient, was uncomfortable.
After several minutes the tissue tone returned to normal, and the discomfort completely dissipated. The gingival height was marked on the abutment so the margins could be properly placed. The abutment was removed, and in the laboratory it was prepared with a high-speed handpiece and carbide bur for proper height, axial preparation, and margins. The abutment was steam-cleaned and re-placed in the mouth. The screw was tightened to 20 Ncm torque with a driver, and the access was sealed with Teflon tape and temporary sealing material (Tempit). Retraction paste (Take 1™ Retraction Paste, KaVo Kerr, kerrdental.com) was injected around the margins of the abutment, and a large compression cap was compressed with biting pressure for 3 minutes. The area was then washed with water and air-dried.
A scan was taken with an intraoral scanner (Planmeca Emerald™) and conveyed to Planmeca Romexis PlanCAD® Design Center software. It began with an upper arch scan, progressed to a lower arch scan, and was completed with a bite registration scan. This was my associate's first experience using this scanner intraorally, and despite her unfamiliarity with it, the impression scan was completed in 3.5 minutes. The lower scan impression was completed in 2 minutes, and the bite registration scan was done in 15 seconds. There was no need to pour any casts. From my experience, the entire impression process, including preparation, counter, and bite, for a quadrant such as this would typically require only 1 to 1.5 minutes. As a patient, I could attest that the scan process was much preferable to physical impressions.
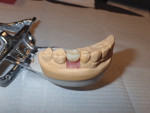
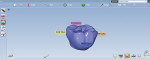
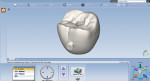
The design phase is a simple and quick process, taking no more than 5 minutes in total. Virtual models and articulation are reviewed. The margin line is drawn, and the software crown proposal is refined, with close attention paid to contour, contacts, and occlusion. The finished design is sent via software to the Planmeca PlanMill® 40 milling machine in the office. An e.max CAD 14 shade A2 block was selected and placed in the mill. The milling process took less than 15 minutes, resulting in a fully milled and completed crown. Contacts and occlusion were checked intraorally. Minimal adjustments were required. The crown was then placed in a ceramic oven (Programat®, Ivoclar Vivadent) for 15 minutes after application of A3 stain cervically and mahogany stain in the grooves, along with glaze.3
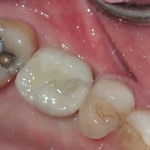
After the oven cycle was complete, the restoration was cooled for 5 minutes and then tried in the mouth. Contacts were verified with floss, and occlusion was checked with articulating paper. No polishing or finishing was required, and the restoration would now be ready for placement.
This process is depicted in Figure 10 through Figure 14.
Scanning a Scan Body With Lab Abutment Fabrication and Crown STL Design
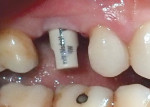
A scan body was placed after removing the healing abutment. Scan bodies have a unique configuration that the software recognizes, which allows for virtual positioning of a given implant. Each scan body relates to a specific implant, and each laboratory will select lab-specific scan bodies. For this case, we chose TruAbutment Inc. (truabutment.com), an Irvine, California, laboratory with which our practice has had success for several years. We purchased a TruAbutment NobelActive 5.5-mm implant scan body, and it was placed to torque. The scanner (Planmeca Emerald) was used again, this time to capture the preparation arch with the scan body in place along with the opposing arch and bite registration. An additional scan was taken without the scan body to capture the soft-tissue contour in order to match the tissue surface of the abutment to the soft tissue. These scans took a total of 6 minutes.
The scans were then uploaded in TruAbutment's portal, along with a digital prescription for a titanium custom abutment to support the soft tissue with 0.5 mm subgingival margins. The lab was also instructed to design a screw-retained crown to be milled in e.max by my office on the PlanMill 40. The next day, the lab emailed me images of the abutment and crown designs for approval. I viewed them online, approved the designs, and received the STL file of the crown via email and the completed abutment in 3 days. The STL was imported into Planmeca Romexis software and sent to the PlanMill 40 for milling an e.max 14 shade A2 block. The crystallizing and finishing of the crown was identical to the process previously described. The abutment and crown were tried in, and minor adjustments were made.
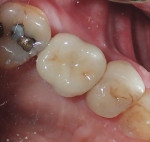
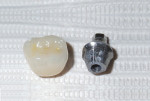
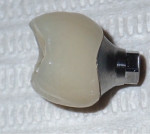
Being a screw-retained format, the abutment and crown were removed and steam-cleaned. The crown was internally etched and silanated, then luted to the abutment extraorally using a self-adhesive, self-curing resin cement (SpeedCEM®, Ivoclar Vivadent) with care taken to keep the cement away from the screw hole. The result was a one-unit screw-retained crown and abutment to be delivered to the implant site and torqued into place at 20 Ncm. After occlusion was checked, a Teflon tape plug was put in the access hole, and shade A2 composite (Tetric EvoCeram®, Ivoclar Vivadent) was placed, contoured, and polished.
This workflow process is depicted in Figure 15 through Figure 21.
Choosing the Right Workflow
Workflows are critical to a dental practice's production. Improved workflows increase efficiency in terms of time, money, patient acceptance, and outcome. Based on the exercise presented in this article, from my perspective as both a patient and a dentist, a scanning workflow of a scan body was preferred, with a scan of a stock abutment as a close second choice. (Table 1 provides a breakdown of the results of the three workflows.) The laboratory workflow is a proven method, and esthetic results are predictably excellent; however, cost is high. As a patient, digital intraoral impressions were preferable. Impression trays and material were uncomfortable, and from clinical experience over many years, I have found this approach to result in more inaccuracies than its digital counterpart.
A workflow that utilizes a scan impression, and then electronically sends that scan to a capable laboratory for custom abutment fabrication and virtual crown design for in-office milling can be an excellent workflow. With the Planmeca ProMax 3D system, radiation exposure is limited due to the Planmeca Ultra Low Dose technology it utilizes.4 Also, this workflow allows for the most amount of information to be available. The scan lets the clinician diagnose and plan the implant as well as a surgical guide for printing in the office. The intraoral scanner takes the impression and provides the opportunity for the restoration to be to milled and finished in-office. With time at a premium for most clinicians, the scanning of a scan body with custom abutment and crown design approach offers an efficient, effective means of restoring a single implant.
About the Author
Eugene Antenucci, DDS
Private Practice, Bay Shore, New York; Diplomate, International Congress of Oral Implantologists; Fellow, Academy of General Dentistry
References
1. Sharp A, McDermott P. Workflow Modeling: Tools for Process Improvement and Applications Development. Norwood, MA: Artech House, Inc; 2009.
2. Culp L, Wong NY, Misch CE. Digital technology in implant dentistry. In: Misch CE. Dental Implant Prosthetics. 2nd ed. St. Louis, MO: Elsevier Mosby; 2015.
3. Bindl A. Computer-aided crown design - fabrication of CAD/CAM crowns chairside. Dental Tribune website. April 7, 2013. https://www.dental-tribune.com/clinical/computer-aided-crown-design-fabrication-of-cadcam-crowns-chairside/. Accessed October 9, 2019.
4. Ludlow JB, Koivisto J. Dosimetry of orthodontic diagnostic FOVs using low dose CBCT protocol [abstract]. J Dent Res. 2015;94(spec iss A):Abstract 0920.