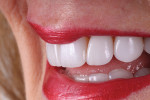
No-Preparation Veneers: A Minimally Invasive Approach for a Naturally Esthetic Smile
Zachary S. Sisler, DDS
Abstract: Typically, dentists spend many years training to learn how to prepare teeth for restorations. Whether the restoration comprises a filling, veneer, crown, inlay, onlay, or bridge, teeth often require preparation to allow adequate space to accommodate the thickness of the restorative material. However, dentists may face a dilemma if a patient inquires about receiving an enhanced smile without tooth preparation. In such cases, the dentist needs to determine the optimal course of action for the patient. This also raises the issue of removing enamel, which is perhaps the most prized commodity in the dentition. This article discusses the question of whether to prepare or not to prepare a tooth for restoration and presents a case demonstrating the meticulous use of eight no-preparation porcelain veneers.
Whether blending the transition of teeth and implants or simply choosing the right restorative material, the realm of esthetic dentistry can be quite challenging. Moreover, patients today seem to present to dental offices more educated than ever due to the plethora of overwhelming information available to them on the Internet. Patients can watch YouTube videos, read blogs, or consult medical websites, such as WebMD®, about their condition and almost diagnose themselves before contacting the practice. They also seem to be more cognizant of the benefits of preserving their natural teeth. Thus, dentists increasingly need to be prepared when patients, especially new ones, insist they want veneers. The practitioner should be able to present a treatment plan to the patient that may allow for minimal, or even no, tooth preparation.
Smile design can become a difficult task when trying to balance the desires of the patient while satisfying the guidelines for a harmonious blend of esthetics from anterior to posterior, as well as macro to micro esthetics.1 The upper central incisors must be determined to be within an acceptable range of deviation for midline facial harmony, and any noticeable cants or asymmetries must be able to be corrected.2,3 Meanwhile, it must be ensured that the functional requirements can be achieved to enable long-term predictability.4
Clinicians must bear in mind, however, that even though they treatment-plan "to ideal," in actuality they must treat "reality." There are very few "ideal" cases that present to the office with the patient asking for esthetic treatment. Most cases have compromises and associated treatment risks that need to be brought to the patient's attention before any treatment is rendered.5 When such cases present, creative "out-of-the-box" planning may be required to achieve beautiful, harmonious results. Oftentimes these can be the most rewarding cases a clinician encounters.
Throughout their dental education, dentists are thoroughly trained to prepare teeth. This begins in dental school on ivorine dentoform teeth and continues in post-graduate residencies or continuing education curriculums. But a debate has persisted over whether or not there is too much tooth preparation being done in the dental profession.6 There is concern over the trimming down and/or removal of tooth enamel. Dentists who focus on smile design work within certain parameters that may require teeth to be prepared, such as when teeth are rotated, maligned, dark, or crowded. However, some might argue that more teeth are being prepared than needed. Examples could include peg laterals, narrow buccal corridors, or certain diastema closures.
Though not an option in every situation, no-preparation, or "no-prep," veneers, when used in the correct environment, can blend seamlessly and be utilized to create a highly conservative and natural-appearing esthetic result. When no or minimal preparation is completed, the mechanical retention is non-existent and the clinician must rely solely on the strong enamel bond of adhesive dentistry.7 In essence, the beauty of esthetics and science meet. Indications for these restorations could include small misshapen teeth, diastema closures, and minor asymmetries within tooth proportions.8 Thus, when posed with the question of whether to prepare or not to prepare a tooth, clinicians must weigh the options carefully to ensure the optimal outcome for the patient.
Case Report
Diagnosis and Treatment Planning
A 58-year-old woman presented somewhat, though not completely, dissatisfied with her smile and wanted to discuss potential options to conservatively enhance the smile. She reported a history that included hard/soft cleft palate repair as a child that, even after two rounds of traditional orthodontics and four bicuspid extractions, caused one of her upper bicuspids to be lingually positioned. The clinician took several photographs, and immediately after seeing the first smile photograph, the patient was in disbelief that the photograph was actually of her own teeth. She then became more intently focused on treating her smile esthetics and stated three clear treatment objectives in order to proceed: (1) After having orthodontic treatment twice, braces or clear aligner therapy were not options. (2) She did not want to have her teeth filed down for crowns or veneers. (3) She did not want her new smile to appear unnatural or look like it was "not my own."
Sometimes it can be extremely helpful when patients are clear and upfront with their desires for treatment. Conversely, however, it can also somewhat limit possible treatment modality options. It became clear to the clinician from the initial consult that this patient wanted treatment strictly one way-no-preparation veneers. With this in mind, the goal of the records appointment was to evaluate the esthetics, function, and risks associated with treating a case in this manner. This afforded the clinician the opportunity to weigh the pros and cons of this approach to determine if it was even a possibility.
A complete set of records, including a full series of photographs, radiographs, periodontal probings, and facebow-mounted casts in centric relation, was taken to assess that the smile would be functionally stable and naturally esthetic. All of the functional requirements for occlusal stability could be achieved on the lingual surfaces of the upper anterior teeth with a simple equilibration. This allowed for immediate posterior disclusion through canine guidance.9 Because the patient was highly demanding, an equilibration was completed to ensure a more predictable, functionally stable occlusion and to prevent any porcelain fractures or unintentional de-laminations.10
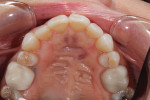
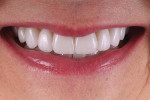
The patient had existing crowns on Nos. 3 and 14 that she did not want to replace. Tooth No. 5 was lingually positioned (Figure 1), which was a major concern of the patient, and she was especially focused on teeth Nos. 5 through 12, which were all virgin teeth with no restorations. Therefore, premolars Nos. 5 and 12 were included in the treatment rather than just the "social six," ie, Nos. 6 through 11. This was done to try to create a harmonious blend transitioning from the anterior to the posterior.11 It also allowed for a slightly broader smile and more esthetic buccal corridor.12
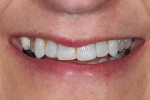
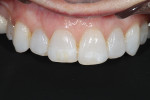
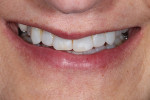
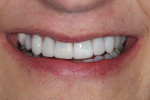
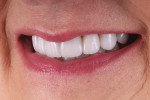
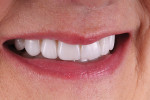
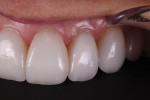
The patient displayed a low-lip smile line with uneven incisal edges (Figure 2). Retracted review showed that the gingival levels provided symmetry within normal limits, with the lateral incisors slightly lower than the central incisors and canines (Figure 3).13 Because the upper incisors were short of the lower lip, the option of adding length to fill the frame of the smile would be considered. From the tipped-down smile view, there appeared to be adequate space for the upper incisal edge position to be moved facially without compromising the neutral zone or encroaching upon the lip closure path (Figure 4). After thorough treatment planning, it quickly became apparent that no-preparation veneers were not only an option but perhaps the best course of treatment to meet the patient's requirements.14
The next decision was choosing the right material to achieve a high esthetic yield with long-term predictability. The patient was adamant that she did not want to worry about what she ate or the fear of new veneers breaking easily. With the patient giving clear and concise input, it was decided to use indirect lithium-disilicate porcelain veneers with cut-back and layering rather than traditional feldspathic or composite veneers.
The final treatment plan would include an equilibration with eight no-preparation, lithium-disilicate porcelain veneers from teeth Nos. 5 through 12.
Clinical Protocol
Direct mock-up-Because a strictly additive approach was used in this case, no local anesthetic was administered for the direct intraoral mock-up. After an equilibration was performed to allow for a stable occlusion and a master final impression of the unprepared teeth was obtained, preparation shade photographs were taken to communicate the natural tooth shade to the laboratory.15 Direct composites were then placed using a freehand technique to establish a prototype restoration so the patient could evaluate esthetics, phonetics, and function. The teeth were isolated and spot-etched, and bonding agent was applied to temporarily adhere the composite to the teeth in a shade of VITA B1. The composite was shaped to define the line angles and embrasures to provide a more symmetrical and uniform tooth form. This approach also achieves a natural transition of embrasure form and proximal contact points moving anteriorly-posteriorly.16,17
Approved mock-up-The patient was given 1 week to evaluate the esthetics and new shape of the teeth. She was very pleased with the shape and overall contours of the teeth but wanted a lighter shade to be used for the final porcelain veneers (Figure 5). She reported her speech was unaffected by the new incisal edge position and was happy to proceed with the final restorations.18 A new polyvinyl siloxane impression, facebow, and series of photographs were taken to document the new contours and tooth form for the laboratory to make the final restorations.
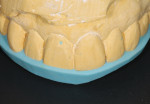
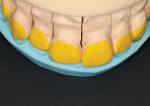
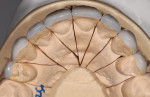
Laboratory component-Based on information gleaned from the photographs and the approved prototype model (APM), the dental laboratory fabricated the final restorations to the same thickness of the mock-up. This method ensures that the restorations will fit within the functional esthetic matrix of the patient. A putty matrix was made on the APM (Figure 6) and then transferred to the preoperative, unprepared teeth model (Figure 7), which allowed the technician to visualize the space available to fabricate final restorations (Figure 8).
Final restorations-For delivery of the final lithium-disilicate porcelain restorations, the composite prototypes were carefully removed and the teeth were meticulously polished to ensure they were free of all composite and bonding agents. This is critical, because any small spicules of composite inadvertently left behind may inhibit complete seating of the veneers. The restorations were tried in individually and then together to ensure a passive fit, which enabled a smooth delivery. Try-in paste was then applied to the veneers, and the patient was allowed to view them in multiple forms of light. She approved the new shade and shape of the final restorations. The restorations were removed, treated with a cleaning paste (Ivoclean®, Ivoclar Vivadent, ivoclarvivadent.com), and silanated in preparation for final bonding placement.
The teeth were isolated from Nos. 3 through 14 with a non-latex rubber dam using a split-dam technique. This is done to prevent any contamination during the bonding process and to ensure a good long-term prognosis.19 The teeth were air-abraded and then acid-etched. A disinfectant scrub (Consepsis®, Ultradent Products Inc, ultradent.com) was then applied to help prevent sensitivity and bond degradation. The veneers were then held with a small suction tip while resin cement was applied to their intaglio surfaces. Once all veneers were placed, gross excess resin was removed using a microbrush and the units were tack-cured. Further resin clean-up was completed and followed by a final cure and polish. The occlusion was verified to be unchanged and still stable.
The patient was extremely pleased with the final outcome. Her smile had the natural esthetic appeal that she desired, as a uniform blend had been created from teeth Nos. 5 through 12 (Figure 9 through Figure 11). The margins were finished to provide a healthy and cleansable environment for the patient to maintain long-term. When margins are kept equigingival or even supragingival, it allows for optimal patient tissue response.20 With the clinician paying rigorous attention to detail, the surface texture and translucency that can be established in a restoration that is 0.5 mm to 0.7 mm thick, as in this case, are what set the smile apart (Figure 12 through Figure 15).
Conclusion
Listening to the patient's objectives and determining that they can be met is an extremely critical step in the diagnosis and treatment planning of functional and esthetic smile design. No-preparation veneers are a viable, minimally invasive option when used in the appropriate situation.
Acknowledgments
The author would like to acknowledge Juan Rego, CDT, FAACD, of Smile Designs by Rego, Santa Fe Springs, California, for his artistic ability with the ceramic restorations in this case.
About the Author
Zachary S. Sisler, DDS
Associate Faculty, The Dawson Academy, St. Petersburg, Florida;
Private Practice, Shippensburg, Pennsylvania
References
1. Morley J, Eubank J. Macroesthetic elements of smile design. J Am Dent Assoc. 2001;132(1):39-45.
2. Kokich VO Jr, Kiyak HA, Shapiro PA. Comparing the perception of dentists and lay people to altered dental esthetics. J Esthet Dent. 1999; 11(6):311-324.
3. Kokich VO, Kokich VG, Kiyak HA. Perceptions of dental professionals and laypersons to altered dental esthetics: asymmetric and symmetric situations. Am J Orthod Dentofacial Orthop. 2006;130(2):141-151.
4. Cranham JC, Finlay SW. Timeless principles in esthetic dentistry. J Cosmetic Dent. 2012;28(3):64-73.
5. Kois JC. New challenges in treatment planning-Part 1: Shifting the paradigm toward risk assessment and perceived value. J Cosmetic Dent. 2011;26(4):62-69.
6. Christensen GJ. Has tooth structure been replaced? J Am Dent Assoc. 2002;133(1):103-105.
7. Magne P, Belser U. Tooth preparation, impression, and provisionalization. In: Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, IL: Quintessence Publishing; 2002:239-291.
8. Wells D. "No prep" veneers: demand and desire for more conservative preparations begins to drive this new area of esthetic dentistry. Inside Dentistry. 2010;6(8):56-60.
9. Dawson P. Functional smile design. In: Functional Occlusion: From TMJ to Smile Design. St. Louis, MO: Mosby; 2007:149-158.
10. Calamia JR, Calamia CS. Porcelain laminate veneers: reasons for 25 years of success. Dent Clin North Am. 2007;51(2):399-417.
11. Olitsky J. Seven worst violations of smile design: achieve better esthetics by understanding common mistakes. Inside Dentistry. 2015;11(9):60-68.
12. Moore T, Southard KA, Casko JS, et al. Buccal corridors and smile esthetics. Am J Orthod Dentofacial Orthop. 2005;127(2):208-213.
13. Garber DA, Salama MA. The aesthetic smile: diagnosis and treatment. Periodontol 2000. 1996;11:18-28.
14. LeSage B, Wells D. Myths vs. realities: two viewpoints on prepared veneers and prep-less veneers. J Cosmetic Dent. 2011;27(2):66-76.
15. Rosenstiel S, Land M, Fujimoto J. Treatment planning. In: Contemporary Fixed Prosthodontics. 4th ed. St. Louis, MO: Mosby; 2006:82-109.
16. Baharav H, Kupershmit I, Oman M, Cardash H. Comparison between incisal embrasures of natural and prosthetically restored maxillary anterior teeth. J Prosthet Dent. 2009;101(3):200-204.
17. Stappert CF, Tarnow DP, Tan JH, Chu S. Proximal contact areas of the maxillary anterior dentition. Int J Periodontics Restorative Dent. 2010;30(5):471-477.
18. Vig RG, Brundo GC. The kinetics of anterior tooth display. J Prosthet Dent. 1978;39(5):502-504.
19. Sadowsky SJ. An overview of treatment considerations for esthetic restorations: a review of the literature. J Prosthet Dent. 2006;96(6):433-442.
20. Spear FM, Cooney JP. Restorative interrelationships. In: Newman MG, Takei HH, Klokkevold PR, Carranza FA, eds. Carranza's Clinical Periodontology. St. Louis, MO: Saunders Elsevier: 2006:1050-1069.