Gum Drop Technique: Minimally Invasive Soft-Tissue Platelet-Rich Fibrin Grafting for Marginal Soft-Tissue Recession
Delia Tuttle, DDS; Gregori M. Kurtzman, DDS; and Ana Luisa Bernotti, DDS
Abstract
Minimally invasive techniques for treatment of marginal soft-tissue recession, or root recession, are conducive to lower morbidity and less postoperative discomfort than techniques that employ surgical flaps. The gum drop technique (GDT) is a novel soft-tissue grafting procedure that combines minimally invasive incisions with blood derivatives from the patient to achieve root coverage. Demonstrating favorable healing without the need for a donor site to provide connective tissue, this papilla-preserving approach offers the benefits of an autogenous, biologically enhanced procedure.
Marginal soft-tissue recession, also known as root recession, is a common problem encountered in dentistry. Recession presents as an esthetic issue and creates exposed root surfaces that may elicit sensitivity and have greater caries potential than roots that are covered. Often patients avoid treating the recession due to fear related to traditional approaches that require flap surgery. Technology has enabled surgical techniques to become minimally invasive, allowing lower morbidity and less postoperative discomfort compared with techniques that utilize surgical flaps. This article will introduce the gum drop technique (GDT), a novel soft-tissue grafting procedure that combines minimally invasive incisions with blood derivatives from the patient to achieve root coverage.
Many root coverage procedures have been described in the literature with varying degrees of success. Although not the first to do so, in the early 1980s Miller discussed the use of free gingival autografting.1,2 Numerous authors, including Matter (1982),3 Marggraf (1985),4 McGuire (1990),5 Laney (1992),6 and others expounded upon this work, discussing various flap techniques to achieve the desired root coverage. As less invasive techniques were sought, modifications were implemented, with Mahn (2001)7 reporting the "tunnel" technique, utilizing smaller incisions with placement of acellular connective tissue to bulk the tissue out and allow coronal placement to cover the receded root surfaces. These techniques eliminated the need to collect donor connective tissue from elsewhere intraorally.
Various surgical techniques have been proposed to obtain root coverage when marginal soft-tissue recession defects are present. Subepithelial connective tissue grafting, introduced by Edel in 1974 and developed by Langer in 1980, in conjunction with the use of coronally advanced flaps has been consistently effective and is currently considered the gold standard for gingival recession treatment. Yet, this approach has shortcomings, including patient morbidity associated with the second surgical site, limited availability of palatal donor tissue, and greater postoperative discomfort associated with these relatively large fields of surgery.8 Collagen matrices of human and porcine origin have been introduced as alternatives to autogenous connective tissue grafts. This removes the limitations of lack of available donor graft while eliminating a donor surgical site to procure the needed connective tissue. Yet, these acellular graft materials have a limitation not found in autogenous grafts, as they do not contain the growth factors that autogenous grafts possess, which aid in the healing process and hasten incorporation of the graft into the desired tissue, ie, connective tissue.
Biological factors derived from the patient's blood have been introduced as solo or combination agents to stimulate wound healing and increase success rates. These blood-derived products, platelet-rich plasma (PRP), were initially suggested for augmenting healing in sites planned for implant placement.9 PRP use to promote tissue regeneration and alveolar bone repair has been well-documented for restoration of extraction sockets, ridge augmentation for defect correction, and implant site development.10,11 As the biologics were studied further, a second generation of patient blood-derived factors were introduced: plasma-rich fibrin (PRF), also referred to as leucocyte- and platelet-rich fibrin (L-PRF), in which autologous platelets and leucocytes are present in a complex fibrin matrix to accelerate the healing of soft and hard tissue. PRF simplified preparation without the need for biochemical blood handling, which was necessary with PRP. Initial analyses revealed that PRF may be an immune regulation node with inflammation retrocontrol ability, which would explain the reduction of postoperative infections when PRF is used as a surgical additive.12-15 That is, it appears based on the available research cited here that PRF is able to turn off the localized inflammation by regulating the immune response. Choukroun also reported that when comparing 4 months of healing time when PRF was included in the graft with a control group (osseous graft material without PRF) after a period of 8 months, histologic maturation between the groups was identical. Moreover, the quantity of newly formed bone was equivalent between the two protocols.16
These observations have been buoyed by other studies supporting an acceleration in healing without detrimental effect on the quality of the resulting bone and an improvement in overall osseous regeneration and soft-tissue healing in response to PRF.17 PRF induced a significantly higher proliferation rate of osteoblasts and fibroblasts at 3 and 5 days when compared to PRP.18 This may be related to the increase that growth factors in PRF have on new blood vessel proliferation (angiogenesis), which is crucial to maturation of the hard-tissue graft and soft-tissue healing.19 Additionally, the concentrated fibrin component acts like a tissue glue holding hard-tissue graft material together into a moldable material and making it adhere to the underlying bone and overlying soft tissue. When used in soft-tissue procedures it binds the tissue into position, allowing improved healing and better immobilization of the flap with reported accelerated wound and site healing.20
The fibrin clot that is derived from the centrifuged blood at 1300 rpm/8 min becomes a membrane that can be used in place of autogenous connective tissue or acellular membranes in various procedures. This is referred to as advanced-PRF (A-PRF). The injectable version of PRF (i-PRF) centrifuged at 700 rpm/3 min, has demonstrated the ability to release higher concentrations of various growth factors and has induced higher fibroblast migration and growth factor expression (PDGF, TGF-ß, and collagen 1) when compared with PRF used alone, improving soft-tissue healing, which would be important in treatment of gingival recession.21 The low speed and low centrifugation concept (settings from 2700 rpm/12 min to 1300 rpm/8 min) changed the entire dynamics of the clot, increasing not only the number of cells and vessels but the matrix as well by increasing the growth factors, cytokines, and fibronectin.
Gum Drop Technique (GDT)
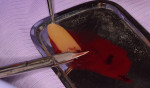
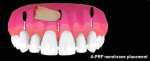
The Gum Drop Technique encompasses the positive benefits of an autogenous graft material and minimally invasive, biologically enhanced soft-tissue procedure. At the surgical appointment, prior to surgery, peripheral blood is collected from the patient in 10-ml vials. The tubes do not contain anticoagulant and are immediately centrifuged to 1300 rpm for 8 minutes. After completion of centrifuging, the fibrin clot is separated from the red blood cell (RBC) component using tweezers to remove the clot from the tube and scissors to separate the RBC portion from the fibrin (Figure 1 and 2). The fibrin clot is placed onto a metal tray (ie, PRF box) (Figure 3), and a weighted cover is placed over the clots for 3 minutes to express any residual fluid, creating an A-PRF membrane (Figure 4).
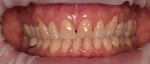
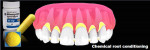
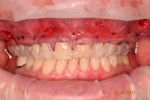
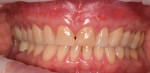
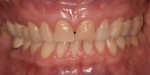
Teeth being treated for correction of marginal soft-tissue recession may also present with abfraction-type lesions that will require modification as part of the recession correction treatment. To perform the GDT, 1 mm to 2 mm of keratinized tissue must be present (Figure 5). The roots on the teeth being treated are mechanically cleaned of any calculus using hand and piezo scalers before initiating surgery. Fine diamond finishing burs in a high-speed handpiece are then utilized to smooth the cervical area of the teeth being treated and remove any sharp edges that may be present that are related to abfraction-type lesions (Figure 6 and Figure 7). The roots are then chemically decontaminated with minocycline, which is created by emptying a capsule of the antibiotic into a dappen dish and adding saline to create a paste. The paste is then applied to the root surfaces for 2 to 3 minutes and then rinsed off (Figure 8 and Figure 9).
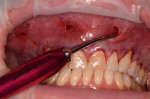
The surgical procedure is initiated by placement of holes in the gingiva apical to the mucogingival line using a small soft-tissue piercing instrument (Figure 10). These holes are comparable to those used in laparoscopic procedures for medical surgeries. Four holes are usually sufficient to treat the entire arch.
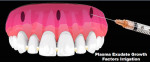
Appropriate instruments are used to create a full-thickness tunnel between the entrance holes and the cementoenamel junction (CEJ) of each tooth. The tissue is detached at the CEJ to allow repositioning of the soft tissue to cover the marginal soft-tissue recession. The papilla is spared and not detached from the underlying bone. The procedure will create a tension-free flap allowing movement of the gingival margin in a more coronal direction to cover the roots being treated. The tunnel created under the elevated tissue is irrigated with plasma exudate to place growth factors into the site and aid in wound healing (Figure 11). The A-PRF membranes previously created are introduced through the entrance holes under the elevated soft tissue (Figure 12 and Figure 13). Membranes are introduced into the gingival holes using cotton pliers. Multiple A-PRF and membranes are placed until sufficient bulking of the gingival tissue is achieved. Typically, 25 to 30 membranes per arch are required. The soft tissue is advanced toward the CEJ as the membranes are placed over the roots and under the papillae. The level of coronal placement of the flap plays an important role in increasing the possibility of achieving 100% root coverage.22 Ideally, the flap should be sutured 2 mm coronal to the CEJ.
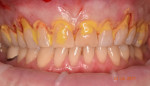
The coronally advanced flap is maintained in position using an apical mattress suture. In a study by Zucchelli et al, not all cases treated using the GDT reconstructed the CEJ using composite restoration despite Zucchelli's theory regarding recession-abrasion-abfraction defects.23 A long-term resorbable polyglycolic acid suture is recommended, because the sutures need to remain for 3 to 4 weeks as the tissue reattaches to the underlying bone and stays in close proximity to the roots. A 5-0 suture material works well for this treatment. The apical mattress suture technique is used across the arch to stabilize the soft tissue in the desired position.24 Composite is temporarily bonded at the contacts at the incisal aspect to give the sutures a positive point to create stabilization of the soft tissue (Figure 14 and Figure 15).
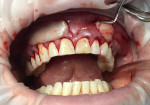
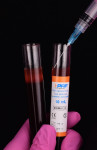
At the completion of surgery another blood drawing is taken to obtain the i-PRF (700 rpm/3 min) and A-PRF liquid (1300 rpm/4 min). The i-PRF liquid above from the red layer of RBCs is drawn off into a syringe from the tube (Figure 16). This is injected into the surgical sites at the mesial and distal aspects into the periodontal ligament (PDL) to stimulate wound healing and into the facial aspect of the gingiva (Figure 17). The A-PRF liquid will be injected on top of the tunnel. The fibrin glue properties of the PRF will coalesce all the membranes within the tunnel, stabilizing the clot and providing mechanical immobilization of the flap. The growth factors and mesenchymal cells from the i-PRF further stimulate fibroblast growth and cell migration that will repopulate the root surface to assist the attachment of the flap to the root surface.
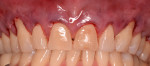
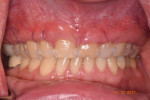
At 2 weeks post surgery, there was minimal inflammation and tissue appeared healthy. The sutures and bonding stabilization were removed (Figure 18). Follow-up at 1 month demonstrated an absence of inflammation and stability of the repositioned tissue as well as correction of the marginal soft-tissue recession (Figure 19). Sixteen-month recall demonstrated long-term recession correction with stability of the gingival margin at the same position as was observed at 1-month recall (Figure 20).
Discussion
For regeneration to begin, tissue must sense an injury, initiate a regenerative response, and then properly direct growth. Normal regeneration has been shown to require cell death.25-27 The dying cells release signals that stimulate the regenerative response in progenitor cells in the injured area.28 Progenitor cells that were once stimulated by the trauma from the localized injury interact with the cells in the PRF that has been placed into the surgical site. Stimulation of the periosteum with blunt instruments as the tunnel is elevated provides the trauma to initiate wound healing and potential regeneration. Injection of the i-PRF into the site provides cells required to fuel regeneration of the tissue and PDL.
The growth factors released from platelets and leucocytes within the A-PRF and i-PRF stimulate new blood vessel growth through vascular endothelial growth factor (VEGF) and fibroblast growth factor (FGF). This has a stimulating effect that encourages new attachment of the gingival tissue to the root surface, creating a stable attachment.
In periodontal regeneration, the re-establishment of the PDL coronally requires cementum and supporting alveolar bone. Agents that promote periodontal ligament fibroblast proliferation and migration as well as collagen biosynthesis appear to be mediators for enhancing new PDL formation.29 The PDL contains fibroblast cells that, through undifferentiated mesenchymal cells, are able to differentiate into bone and cementum PRF is rich in VEGF and platelet derivative growth factor (PDGF). The success of any grafting procedure depends on the blood supply and vascularization of the tissues involved. VEGF contributes to angiogenesis to the new tissue.30 In one study, angiogenesis and migration of endogenous stem cells were much more abundant in the presence of VEGF,31 whereas PDGF is a mitogen (stimulator) for cells of mesenchymal origin, including fibroblasts, thereby providing a role in periodontal regeneration.32 However, not all blood-derived membranes are the same. L-PRF membranes are still intact after 7 days, while PRP membranes resorb within 5 days. This demonstrates that the polymerization and final architecture of the fibrin matrix influences the strength and growth factor trapping/release potential of the membrane. This also suggests that the leukocyte populations have a strong influence on the release of some growth factors.33
Two main components of the GDT assist in flap reattachment to the root surface: growth factors in the A-PRF/i-PRF and the apical mattress suture fixating the repositioned tissue to its new position in a tension-free manner. Moreover, the fibrin matrix provides mechanical adhesive properties, functioning like fibrin glue. This maintains the flap in a stable position, allowing the growth factors to induce vascularization and wound healing while reducing tissue necrosis and promoting soft-tissue reattachment.
Conclusion
This novel biological approach involving blood derivatives A-PRF and i-PRF combined with a minimally invasive surgical method for the treatment of marginal soft-tissue recession demonstrates favorable healing without the need for a donor site to provide connective tissue. The morbidity of the GDT is thought to be less than traditional techniques that are used to treat single or multiple marginal soft-tissue recession defects in the natural dentition and around dental implants. This technique also preserves the papilla, increasing the thickness of the soft tissue and utilizes a minimally invasive surgical approach.
Acknowledgment
The illustrations (Figures 7, 9, 11, 13, 14, and 17) were provided by Ana Luisa Bernotti, DDS.
About the Authors
Delia Tuttle, DDS
Private Practice, Lake Elsinore, California
Gregori M. Kurtzman, DDS
Private Practice, Silver Spring, Maryland; Master, Academy of General Dentistry; Diplomate, International Congress of Oral Implantologists
Ana Luisa Bernotti, DDS
Private Practice, periodontist and implantologist, Caracas, Venezuela
References
1. Miller PD Jr. Root coverage using a free soft tissue autograft following citric acid application. Part 1: Technique. Int J Periodontics Restorative Dent. 1982;2(1):65-70.
2. Miller PD Jr. Root coverage using the free soft tissue autograft following citric acid application. II. Treatment of the carious root. Int J Periodontics Restorative Dent. 1983;3(5):38-51.
3. Matter J. Free gingival grafts for the treatment of gingival recession. A review of some techniques. J Clin Periodontol. 1982;9(2):103-114.
4. Marggraf E. A direct technique with a double lateral bridging flap for coverage of denuded root surface and gingiva extension. Clinical evaluation after 2 years. J Clin Periodontol. 1985;12(1):69-76.
5. McGuire MK. Coverage of the denuded root surface using the free soft tissue autograft. J Am Dent Assoc. 1990;121(2):277-279.
6. Laney JB, Saunders VG, Garnick JJ. A comparison of two techniques for attaining root coverage. J Periodontol. 1992;63(1):19-23.
7. Mahn DH. Treatment of gingival recession with a modified "tunnel" technique and an acellular dermal connective tissue allograft. Pract Proced Aesthet Dent. 2001;13(1):69-74.
8. Kasaj A. Gingival recession coverage: do we still need autogenous grafts? Quintessence Int. 2016;47(9):775-783.
9. Anitua E. Plasma rich in growth factors: preliminary results of use in the preparation of future sites for implants. Int J Oral Maxillofac Implants. 1999;14(4):529-535.
10. Tözüm TF, Demiralp B. Platelet-rich plasma: a promising innovation in dentistry. J Can Dent Assoc. 2003;69(10):664.
11. Tischler M. Platelet rich plasma. The use of autologous growth factors to enhance bone and soft tissue grafts. N Y State Dent J. 2002;68(3):22-24.
12. Dohan DM, Choukroun J, Diss A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part I: technological concepts and evolution. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e37-e44.
13. Dohan DM, Choukroun J, Diss A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part II: platelet-related biologic features. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e45-e50.
14. Dohan DM, Choukroun J, Diss A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part III: leucocyte activation: a new feature for platelet concentrates? Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e51-e55.
15. Choukroun J, Diss A, Simonpieri A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part IV: clinical effects on tissue healing. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e56-e60.
16. Choukroun J, Diss A, Simonpieri A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part V: histologic evaluations of PRF effects on bone allograft maturation in sinus lift. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):299-303.
17. Varghese MP, Manuel S, Kumar LKS. Potential for osseous regeneration of platelet-rich fibrin - a comparative study in mandibular third molar impaction sockets. J Oral Maxillofac Surg. 2017;75(7):1322-1329.
18. Wang X, Zhang Y, Choukroun J, et al. Effects of an injectable platelet-rich fibrin on osteoblast behavior and bone tissue formation in comparison to platelet-rich plasma. Platelets. 2018;29(1):48-55.
19. Dohle E, El Bagdadi K, Sader R, et al. Platelet-rich fibrin-based matrices to improve angiogenesis in an in vitro co-culture model for bone tissue engineering. J Tissue Eng Regen Med. 2018;12(3):598-610.
20. Miron RJ, Fujioka-Kobayashi M, Bishara M, et al. Platelet-rich fibrin and soft tissue wound healing: a systematic review. Tissue Eng Part B Rev. 2017;23(1):83-99.
21. Miron RJ, Fujioka-Kobayashi M, Hernandez M, et al. Injectable platelet rich fibrin (i-PRF): opportunities in regenerative dentistry? Clin Oral Investig. 2017;21(8):2619-2627.
22. Pini Prato GP, Baldi C, Nieri M, et al. Coronally advanced flap: the post-surgical position of the gingival margin is an important factor for achieving complete root coverage. J Periodontol. 2005;76(5):713-722.
23. Zucchelli G, Testori T, De Sanctis M. Clinical and anatomical factors limiting treatment outcomes of gingival recession: a new method to predetermine the line of root coverage. J Periodontol. 2006;77(4):714-721.
24. Kurtzman GM, Silverstein LH, Shatz PC, Kurtzman D. Suturing for surgical success. Dent Today. 2005;24(10):96-102.
25. Ryoo HD, Gorenc T, Steller H. Apoptotic cells can induce compensatory cell proliferation through the JNK and the Wingless signaling pathways. Dev Cell. 2004;7(4):491-501.
26. Tseng AS, Adams DS, Qiu D, et al. Apoptosis is required during early stages of tail regeneration in Xenopus laevis. Dev Biol. 2007;301(1):62-69.
27. Li F, Huang Q, Chen J, et al. Apoptotic cells activate the "phoenix rising" pathway to promote wound healing and tissue regeneration. Sci Signal. 2010;3(110):ra13.
28. Chera S, Ghila L, Dobretz K, et al. Apoptotic cells provide an unexpected source of Wnt3 signaling to drive hydra head regeneration. Dev Cell. 2009;17(2):279-289.
29. Raja S, Byakod G, Pudakalkatti P. Growth factors in periodontal regeneration. Int J Dent Hyg. 2009;7(2):82-89.
30. Yoshino H, Morita I, Murota SI, Ishikawa I. Mechanical stress induces production of angiogenic regulators in cultured human gingival and periodontal ligament fibroblasts. J Periodontal Res. 2003;38(4):405-410.
31. Katagiri W, Kawai T, Osugi M, et al. Angiogenesis in newly regenerated bone by secretomes of human mesenchymal stem cells. Maxillofac Plast Reconstr Surg. 2017;39(1):8.
32. Sant'Ana AC, Marques MM, Barroso TE, et al. Effects of TGF-beta1, PDGF-BB, and IGF-1 on the rate of proliferation and adhesion of a periodontal ligament cell lineage in vitro. J Periodontol. 2007;78(10):2007-2017.
33. Dohan Ehrenfest DM, Bielecki T, Jimbo R, et al. Do the fibrin architecture and leukocyte content influence the growth factor release of platelet concentrates? An evidence-based answer comparing a pure platelet-rich plasma (P-PRP) gel and a leukocyte- and platelet-rich fibrin (L-PRF). Curr Pharm Biotechnol. 2012;13(7):1145-1152.