Fabrication of a Dual-Purpose Implant Surgical Guide
Thomas H. Yoo, DMD, MS; Caleb J. Cross, DMD, MBA; Brian M. Kasten, DMD; Harold S. Baumgarten, DMD; and Howard P. Fraiman, DMD
ABSTRACT
While surgical guides have allowed for more highly accurate immediate implant placement in the esthetic zone, only a few techniques have been described to predictably position an immediate implant provisional. Even fewer techniques have addressed repositioning a patient's extracted tooth for use as the interim implant restoration. This article describes a workflow for the fabrication of a dual-purpose surgical guide that allows for guidance of implant placement as well as repositioning of a decoronated tooth that will serve as a provisional. While other provisional techniques aim to recreate proper gingival contour, the benefit of repositioning of the original tooth is the preservation of the existing gingival margin position and existing critical contour of the emergence profile.
Immediate implant placement has become a common treatment modality for the replacement of a tooth with a hopeless prognosis in the esthetic zone. While both immediate and delayed implant placement procedures have been shown to achieve similar survival rates, achieving an esthetic outcome with immediate implant placement can be challenging due to the hard- and soft-tissue remodeling process.1-4 A minimally traumatic extraction combined with a palatal and subcrestal implant placement have been proposed to preserve hard and soft tissues.4-8 With advancements in digital technology and diagnostic radiographic imaging, virtual implant surgery planning and static surgical guide fabrication have led to more highly accurate 3-dimensional implant positioning.9-11
Besides utilizing optimal immediate implant placement positioning, an additional technique to further maintain the midfacial soft-tissue level in the esthetic zone is immediate provisionalization.12-14 However, arbitrary positioning of the interim implant restoration in comparison to the original tooth can affect gingival level and zenith location, influencing the esthetic outcome and predictability of the final implant restoration. Analog approaches have been described to position the implant-supported interim restoration (extracted tooth or provisional shell) using a self-curing acrylic resin, silicon matrix, or light-cured resin.15-17 Subsequently, a digital workflow was introduced that adds proximal wings that adapt to adjacent teeth on either end of a milled provisional shell.18 This, however, requires further chairside time to remove the proximal wings after relining the provisional shell onto the prosthetic implant abutment. Furthermore, this technique cannot be used when converting an extracted tooth to an interim implant prosthesis and must rely on analog-fabricated positioning jigs.
This article describes a digital workflow for the fabrication of a static guide that serves as both a surgical guide for implant placement and a prosthetic positioning guide for immediate implant provisionalization.
Case Presentation: Extraction of Tooth No. 9, Immediate Implant, and Immediate Provisionalization
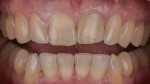
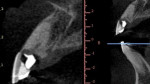
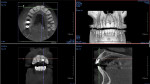
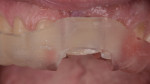
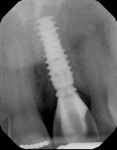
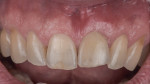
A 65-year-old male patient was referred for evaluation of tooth No. 9 (Figure 1). Upon intraoral and radiographic evaluation, including cone-beam computed tomography (CBCT) imaging, the tooth was diagnosed with external root resorption, and the treatment plan included extraction, immediate implant placement, and immediate implant provisionalization using the decoronated extracted tooth No. 9 (Figure 2 and Figure 3).
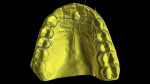
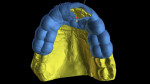
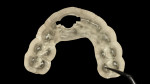
The patient specifically requested that the provisional restoration demonstrate no alteration in the existing anatomic position when compared to the original tooth. A digital impression was made using an intraoral scanner (iTero®, Align Technology, Inc., itero.com), and the stereolithography (STL) file was exported into an implant planning software (Blue Sky Bio, BlueSkyBio, blueskybio.com). The STL file was superimposed with the patient's digital imaging and communications in medicine (DICOM) file from the CBCT scan. After finalizing the implant position, a tooth-supported dual-purpose surgical guide was planned on the superimposed STL file from the initial intraoral scan, and the guide was 3D-printed (Pro S, SprintRay, sprintray.com) using photopolymer resin (Surgical Guide 2, SprintRay) (Figure 4 through Figure 6).
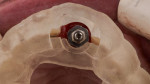
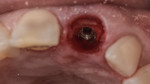
On the day of the procedure, the surgical area was anesthetized and then tooth No. 9 was extracted as minimally traumatic as possible, while keeping the buccal bone intact. The socket was degranulated and rinsed with saline solution. Using the 3D-printed surgical guide, an implant (NobelActive RP, 4.3 mm x 15 mm, Nobel Biocare, nobelbiocare.com) was placed with primary stability of 45 Ncm (Figure 7), and the buccal gap was grafted with xenograft (Bio-Oss® Collagen, Geistlich, geistlich-pharma.com) (Figure 8). A temporary abutment was attached to the implant and, with the use of the dual-purpose surgical guide, the decoronated coronal of tooth No. 9 was positioned intraorally buccal to the abutment to replicate the same anatomical tooth position as before the extraction (Figure 9 and Figure 10). Flowable composite (Filtek™ Supreme Ultra Flowable Restorative, 3M Oral Care, 3m.com) was used to attach the tooth to the titanium abutment and fill in the subgingival (subcritical) contour. The interim restoration consisting of the titanium abutment and coronal portion of the extracted tooth was placed on the implant and torqued to 15 Ncm. Occlusion was adjusted and, with the use of articulating paper, verified to be free from any contacts in maximum intercuspation position and excursive movements. Figure 11 shows a post-treatment periapical radiograph.
The patient presented for a 2-week follow-up visit with no signs of infection and intact papillae. At the 6-month follow-up, intraoral examination revealed no changes to the gingival margin position and the provisional remained intact (Figure 12).
Discussion
This article describes a workflow to fabricate a surgical guide that not only guides the implant position but also can be used to position the interim implant prosthesis for immediate implant provisionalization. The use of this workflow to fabricate a guide for implant placement and interim implant restoration positioning enabled all treatment goals to be met, including the patient's request to have an unaltered anatomic tooth position, a prosthetically driven 3-dimensional implant position, and fabrication of a provisional restoration with ideal gingival contours.
To achieve a positive esthetic outcome for an immediate implant placement into a post-extraction socket, the anatomy and 3-dimensional position of the implant and the provisional must be considered. Preoperatively, a diagnostic CBCT evaluation is necessary to examine intact buccal bone. Additionally, extraction must be performed in a manner that is as minimally traumatic as possible to preserve existing anatomical hard and soft tissue.19 The implant's position should allow for a screw channel in the cingulum of the implant restoration and accommodate space for an emergence profile.5,6 The emergence profile contour may be broken down into two distinct areas: the critical contour, defined as the area extending from the gingival margin to 1 mm-1.5 mm apical to the gingival margin; and the subcritical contour, which comprises the area that extends from the critical contour to the implant abutment junction.20,21 The critical contour is the portion of the provisional that will determine the level and morphology of the gingival margin on an implant restoration. An inability to replicate the position of the existing critical contour can alter the position of the gingival margin and thus compromise the esthetics. Therefore, the precision of positioning of both the implant and the provisional is a crucial factor to ensure an optimal and predictable treatment outcome in immediate implant placement and immediate implant provisionalization.
Conclusion
This article demonstrates the design and fabrication of a dual-purpose surgical guide to position the patient's decoronated extracted tooth for the purpose of immediate provisionalization. This approach allows clinicians to predictably replicate the existing 3-dimensional anatomic position of the patient's tooth, thereby maintaining the current gingival margin position and the all-important critical contour. Additionally, the workflow can be used to design and fabricate a guide that can position a provisional shell by planning the surgical guide directly on a virtual wax-up model.
ABOUT THE AUTHORS
Thomas H. Yoo, DMD, MS
Clinical Assistant Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Private Practice, Philadelphia, Pennsylvania
Caleb J. Cross, DMD, MBA
Private Practice, Philadelphia, Pennsylvania
Brian M. Kasten, DMD
Clinical Assistant Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Private Practice, Philadelphia, Pennsylvania
Harold S. Baumgarten, DMD
Clinical Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Private Practice, Philadelphia, Pennsylvania
Howard P. Fraiman, DMD
Director, Postdoctoral Periodontal Prosthesis Program, Clinical Associate Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania; Private Practice, Philadelphia, Pennsylvania
REFERENCES
1. Garber DA, Belser UC. Restoration-driven implant placement with restoration-generated site development. Compend Contin Educ Dent. 1995;16(8):796-804.
2. Esposito M, Grusovin MG, Willings M, et al. The effectiveness of immediate, early, and conventional loading of dental implants: a Cochrane systematic review of randomized controlled clinical trials. Int J Oral Maxillofac Implants. 2007;22(6):893-904.
3. Couso-Queiruga E, Stuhr S, Tattan M, et al. Post-extraction dimensional changes: a systematic review and meta-analysis. J Clin Periodontol. 2021;48(1):126-144.
4. Monje A, González-Martín O, Ávila-Ortiz G. Impact of peri-implant soft tissue characteristics on health and esthetics. J Esthet Restor Dent. 2023;35(1):183-196.
5. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 suppl:43-61.
6. Grunder U, Gracis S, Capelli M. Influence of the 3-D bone-to-implant relationship on esthetics. Int J Periodontics Restorative Dent. 2005;25(2):113-119.
7. Evans CD, Chen ST. Esthetic outcomes of immediate implant placements. Clin Oral Implants Res. 2008;19(1):73-80.
8. Levine RA, Ganeles J, Gonzaga L, et al. 10 keys for successful esthetic-zone single immediate implants. Compend Contin Educ Dent. 2017;38(4):248-260.
9. Tahmaseb A, Wismeijer D, Coucke W, Derksen W. Computer technology applications in surgical implant dentistry: a systematic review. Int J Oral Maxillofac Implants. 2014;29 suppl:25-42.
10. Vercruyssen M, Cox C, Coucke W, et al. A randomized clinical trial comparing guided implant surgery (bone- or mucosa-supported) with mental navigation or the use of a pilot-drill template. J Clin Periodontol. 2014;41(7):717-723.
11. Younes F, Cosyn J, De Bruyckere T, et al. A randomized controlled study on the accuracy of free-handed, pilot-drill guided and fully guided implant surgery in partially edentulous patients. J Clin Periodontol. 2018;45(6):721-732.
12. De Rouck T, Collys K, Wyn I, Cosyn J. Instant provisionalization of immediate single-tooth implants is essential to optimize esthetic treatment outcome. Clin Oral Implants Res. 2009;20(6):566-570.
13. Block MS, Mercante DE, Lirette D, et al. Prospective evaluation of immediate and delayed provisional single tooth restorations. J Oral Maxillofac Surg. 2009;67(11 suppl):89-107.
14. Cooper LF, Raes F, Reside GJ, et al. Comparison of radiographic and clinical outcomes following immediate provisionalization of single-tooth dental implants placed in healed alveolar ridges and extraction sockets. Int J Oral Maxillofac Implants. 2010;25(6):1222-1232.
15. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;10(9):1107-1116.
16. Ladino LG, Rosselli D. Use of extracted anterior teeth as provisional restorations and surgical guide for immediate multiple implant placement: a clinical case report. J Esthet Restor Dent. 2019;31(3):209-212.
17. Zhu J, Xie C, Wang Y, Yu H. A digital workflow for accurately and rapidly creating an immediate provisional restoration with natural emergence profile using extracted tooth. J Esthet Restor Dent. 2022;34(5):741-749.
18. Pozzi A, Arcuri L, Moy PK. Temporary shell proof-of-concept technique: digital-assisted workflow to enable customized immediate function in two visits in partially edentulous patients. Compend Contin Educ Dent. 2018;39(3):e9-e12.
19. Barone A, Toti P, Piattelli A, et al. Extraction socket healing in humans after ridge preservation techniques: comparison between flapless and flapped procedures in a randomized clinical trial. J Periodontol. 2014;85(1):14-23.
20. Su H, Gonzalez-Martin O, Weisgold A, Lee E. Considerations of implant abutment and crown contour: critical contour and subcritical contour. Int J Periodontics Restorative Dent. 2010;30(4):335-343.
21. González-Martín O, Lee E, Weisgold A, et al. Contour management of implant restorations for optimal emergence profiles: guidelines for immediate and delayed provisional restorations. Int J Periodontics Restorative Dent. 2020;40(1):61-70.