Two-Year Clinical Evaluation of a Nanofilled Etch-and-Rinse and a Self-Etch Adhesive System Containing MDPB and Fluoride in Non-carious Cervical Lesions
Fernanda Garcia de Oliveira, DDS, MS, PhD; Lucas Silveira Machado, DDS, MS, PhD; Daniel Sundfeld-Neto, DDS, MS; Marcelo Giannini, DDS, MS, PhD; André Luiz Fraga Briso, DDS, MS, PhD; Paulo Henrique dos Santos, DDS, MS, PhD; Maria Lúcia Marçal Mazza Sundefeld, MS, PhD; and Renato Herman Sundfeld, DDS, MS, PhD
Abstract
Objectives: The aim of this clinical study was to evaluate the performance of restorations for non-carious cervical lesions performed with a two-step etch-and-rinse or with a two-step self-etch adhesive. Materials and Methods: The teeth to be restored (15 patients, N = 90 restorations) were randomly assigned into 3 groups (n = 30), according to the adhesive system: group 1 (G1): Peak LC Bond; group 2 (G2): Clearfil Protect Bond; and group 3 (G3): prior selective acid etching of the enamel margins before bonding with Clearfil Protect Bond. The NCCLs were restored with Amelogen Plus composite resin. Two calibrated examiners evaluated the restorations using modified US Public Health Service criteria. The data of retention, marginal integrity, and marginal discoloration were analyzed using the Kruskal-Wallis and Wilcoxon tests. Results: There were no significant differences in clinical performance among the groups for the variables: retention, marginal integrity, and marginal discoloration after 1 year and 2 years. The alpha rates after 2 years were: 93.3% for G1 and 96.7% for G2 and G3 for retention; 93.3%, 100%, and 90% for G1, G2, and G3 for marginal discoloration; 86.7%, 96.7%, and 90% for G1, G2, and G3 for marginal integrity, respectively. Conclusions: The adhesives presented similar clinical performance at the end of 2 years. Also, the prior etching with phosphoric acid did not significantly improve the clinical performance of self-etch adhesive.
Non-carious cervical lesions (NCCLs) can lead to dental hypersensitivity when exposed to thermal, chemical, and mechanical agents, as well as esthetics problems.1 This mineralized dental tissue loss is irreversible and commonly described as the sum of erosion, abrasion, and abfraction processes.2,3 Regarding the restorative treatments, the use of composite resins is considered the first option4,5 because this treatment provides esthetic results and good wear resistance.5 However, its ineffective bonding to the dental tissues can lead to restoration loss, which is the most objective evaluation parameter for clinical success.6
The adhesion of restorative materials to tooth structure depends considerably on the adhesive system used. Adhesive systems associated with polymerization shrinkage of the composite restorative may lead to undesirable effects, such as marginal infiltration and degradation associated with the appearance of secondary carious lesions. Also, the presence of dental sensitivity and pulp disease7 will act as limiting factors in the longevity of restorations.
Over the years, different materials and clinical procedures to perform the adhesive bonding to dental tissues have been proposed, such as the etch-and-rinse adhesive systems disposed in single-bottle2,8 and the self-etching adhesive systems.2,8,9 Etch-and-rinse adhesives have pH levels that are too high (2.5-4.5) to etch through the smear layer and underlying dentin, hence the requirement for a separate acid-etching step with 32% to 37% phosphoric acid (0.1-1.0).10 The self-etching approach was developed, aiming to induce less postoperative dental sensitivity11 and to reduce the sensitivity of the technique through the simplification of the clinical steps by not performing the previous acid etching. In addition, the self-etching systems provide surface demineralization of enamel and dentin simultaneously with the infiltration of resinous monomers.8,12 A self-etch adhesive was introduced (Clearfil Protect Bond, Kuraray, kuraraydental.com), showing the potential to inhibit secondary caries.13
Doubts arise regarding their quality of adhesion to dental tissues, especially in the enamel, which has a higher resistance to demineralization. Most self-etch adhesives are not able to etch enamel as effectively as the phosphoric acid used in etch-and-rinse adhesives14,15 because the previous acid etching with phosphoric acid can affect the retention, marginal integrity, and marginal discoloration of NCCL restorations and, consequently, their longevity.9,16 An in vitro research17 article reported increased bond strength to enamel when previous phosphoric acid etching was applied before using self-etching primers. Also, Peumans et al18 found the selective enamel etching did improve the enamel marginal integrity when compared with self-etching only.
This process is significant.12,13,16,19 However, the clinical follow-up of restorative procedures is considered crucial over time,1,4,5,9 because the techniques and materials are analyzed using real conditions. The aims of this clinical research article were to evaluate the performance of adhesive systems in NCCL restorations, performed with a two-step etch-and-rinse or with a two-step self-etching adhesive system, with or without selective enamel etching. Clinical assessments were performed at periods immediately 1 year and 2 years after placement. The null hypothesis tested is that the restorative techniques employed with both adhesive systems would not show the same clinical performance.
Materials and Methods
Patients Recruitment
A total of 90 non-carious cervical restorations were placed in 15 patients (6 males and 9 females; age range: 20 to 54 years). The study was approved by the Ethics Committee of Araçatuba Dental School, Paulista State University, and the patients were from the Araçatuba Dental School, Paulista State University. The selected teeth were restored because they presented dental sensitivity when stimulated, to prevent lesion progression and to reestablish the dental esthetic condition. Each patient had a minimum of 20 teeth and at least 3 cavities with NCCLs under occlusion and with similar dimensions. The shape of the cavities was conical with divergent walls measuring approximate a 4-mm width by 2-mm height by 2-mm depth categorized with a periodontal probe. The lesions were caries free, nonsclerotic, and nonretentive and presented the cervical wall at the marginal gingival level and with the incisal or occlusal walls in enamel. Patients with unsatisfactory oral hygiene, moderate or severe periodontitis, or accentuated bruxism were excluded. The procedures were explained to the patients, who gave written consent to participate. Dental sensitivity was assessed for its presence or absence, through stimulation using air jets for 3 seconds applied directly at the cavity (initial examination) or at the restoration site, from a distance of 1 inch.
Clinical Procedures and Groups Distribution
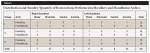
Three groups were formed containing 30 teeth each. Each patient had at least one restoration performed with one of the techniques employed in this study, which were randomly assigned to each NCCL restoration (Table 1). One operator placed the restorations. The operator was calibrated by performing several NCCL restorations in patients from master’s program and from the clinical dentistry school. All restorative procedures were performed after anesthesia and dental prophylaxis with slurry of pumice and water. The operative field was isolated with a buccal expander (Expandex, JON Comércio de Produtos Odontológicos Ltda), followed by the use of cotton rolls and high-power suction. When the cervical margins were below the marginal gingiva, retraction cords were used. A 1-mm to 2-mm enamel bevel was prepared using a No. 1190F diamond tip bur (KG Sorensen Ind & Com Lt) on the cavo-surface angle of the incisal or occlusal walls of all NCCLs.
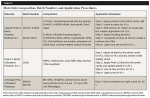
In teeth belonging to group 1 (G1), the entire cavity and 2 mm to 4 mm of the enamel beyond the cavity margin were etched with 35% phosphoric acid (Ultra-Etch®, Ultradent Products Inc., ultradent.com) for 15 seconds, rinsed with oil-free air/water spray, and air-dried, leaving a slightly moist dentin substrate. After that, a 7.5% nanofilled two-step etch-and-rinse adhesive system, Peak® LC Bond (Ultradent Products), was applied in accordance with the manufacturer’s instructions and light cured for 10 seconds with a light-emitting diode VALO® (Ultradent Products) with an irradiance of 1.000 mW/cm² (Table 2). Each increment of the microhybrid resin composite (Amelogen® Plus, Ultradent Products) was inserted in 2-mm layers and light cured for 20 seconds. The restorations were finished using No. 1190F diamond burs (K.G. Sorensen Ind & Com Ltda.) at a high speed and polished with No. 850 Jiffy® Regular Brush polishing points (Ultradent Products) under water cooling.
For group 2 (G2), the teeth were bonded with a two-step self-etching primer Clearfil™ SE Protect Bond (Kuraray Medical Inc., kuraraydental.com) in accordance with the manufacturer’s instructions and light cured for 10 seconds with the light source (Table 2). The cavities were restored, finished, and polished, using the same protocol described for G1.
For the group 3 (G3), the enamel was etched 2 mm to 4 mm beyond the cavity margin with 35% phosphoric acid (Ultra-Etch) for 15 seconds prior to application of Clearfil Protect Bond Primer. The application of the self-etching adhesive followed the same manner as the G2 and the restorations were finished similarly to G1 and G2.
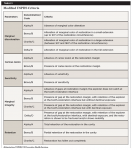
Two duly calibrated examiners, who were not the operators and blinded to the technique used, performed the clinical evaluations of the restorations at three different times: immediately after, at 1 year, and at 2 years. The examiners were calibrated before the baseline evaluation and not enrolled to this clinical study. Similar evaluations were performed at each recall session. Because of disparate results, the restorations were reevaluated to obtain a consensus. Using the modified US Public Health Service criteria (Table 3), the factors considered were: retention, marginal integrity, marginal discoloration, presence of caries, and dental sensitivity,
Statistical Analysis
The groups were compared using the statistical non-parametric Mann-Whitney and Wilcoxon tests with a significance level of 5% (P < .05).
Results
The recall rate at 1 year and 2 years was 100%. At baseline and 1 year, all restorations were cataloged with alpha criterion for the variables: retention, marginal integrity, marginal discoloration, and caries lesion.
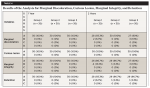
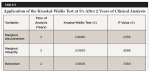
At 2 years, it was scored with Bravo criterion (scoring based on partial retention of the restoration in the cavity) for: retention: 2 (6.7%) restorations in G1 and 1(3.3%) restoration in G2 and G3; marginal discoloration: 2 (6.7%) in G1 and 3 (10.0%) restorations in G3; and marginal integrity: 4 (13.3%) restorations in G1, 1 (3.3%) restoration in G2, and 3 (10.0%) restorations of G3. The other restorations were cataloged with Alpha criterion (Table 4). The application of the Kruskal-Wallis test showed no difference among the study groups in this period of analysis for the variables retention (P = .7369), marginal discoloration (P = .2336), and marginal integrity (P = .3566) (Table 5).
Previously to insertion of the restorations, 79 teeth presented a stimulated sensitivity (Table 6). One year after, only 2 (6.7%) teeth in G1 and 1 (3.3%) tooth in G3 showed sensitivity and were cataloged with Bravo criterion (Table 6). The teeth that showed sensitivity at 1 year of analysis presented it before performing the restoration. After 2 years, all teeth received criterion of alpha, and it was not verified the presence of dental sensitivity in any dental element. No caries lesions were present at 1 year and 2 years of clinical analysis (Table 4).
Discussion
The null hypothesis can be accepted because both adhesive systems showed similar clinical performance at the evaluated times. Moretto et al20 mentioned an adequate recall rate is one of the main requirements to achieve a successful validation of a clinical trial. In this study, the recall rate was 100% at 1 year and 2 years. The NCCLs are considered ideal models to evaluate the clinical performance of adhesive systems in the process of adhesion between the resin materials and dental tissues, mainly by presenting a nonretentive cavity and allow to assess the adhesion in both enamel and dentin.7,21
One of the most relevant parameters during the clinical longitudinal evaluation of NCCL restorations are related to their retention rates, which may be directly related to the effectiveness of the adhesive system tested.6,7,9 Indeed, in this study, the clinical analysis at 1 year and 2 years showed a high retention rate (alpha criterion) for both etch-and-rinse and self-etch adhesive systems, with or without enamel selective etching. The remaining restorations were cataloged with Bravo criterion and were considered clinically acceptable and did not need to be repaired. There was no debonding of any restorations over 2 years of analysis.
After 2 years, the high retention rate for restorations performed with Peak LC Bond may be related to the prior enamel and dentin etching with phosphoric acid, which provides an effective conditioned tooth structure,9,22 dentin hybridization and a strong mechanical interlocking created in enamel.12,16 However, the etch-and-rinse technique can lead to incomplete adhesive resin monomers infiltration into the demineralized dentin network due to adhesive viscosity, improper application and by over-etching time.23 This situation may lead to unprotected collagen fibrils, which can be degradated by metalloproteinases.24-26 The same way, the self-etching adhesive systems also lead to increased matrix metalloproteinases activities27,28 and then may bring on degradation of dentin/adhesive interface, but less often due to the presumed capacity of dentin demineralization and infiltration of the adhesive. This category of bonding agents would cause the smallest exposure of non-infiltrated collagen fibrils located below the hybrid layer adhesion.27 Degradation of adhesive interfaces is known to be the combined result of polymer plasticization and collagenolytic activity by host-derived dentin matrix metalloproteinases (MMPs).10 Peak LC Bond is 7.5% nanofilled, and its presumed higher elastic modulus due to filler content makes it less susceptible to early plasticization, and, as a consequence, more resistant to premature failure. Giannini et al29 found nanofiller technology is supposed to strengthen both the adhesive and hybrid layers into which the system infiltrates, so improved marginal integrity and an increase in bond strength should be expected. However, the present study showed no evidence of interface degradation after 2 years.
The excellent retention rate at 1 year and 2 years using Clearfil Protect Bond can be explained by having a separate acidic primer and adhesive bottles. Emphasizing that, it is possible to apply separately the acidic monomers of hydrophobic components. The self-etching systems dispensed in two bottles are considered more effective because the hydrophobic adhesive layer applied separately provides better adhesion.4,28 It was postulated for the self-etching adhesives that the reduction of residual water in the cavity compared to the etch-and-rinse approach allows better penetration of resin monomers among the collagen fibrils, improves the degree of conversion, controls the process of degradation by hydrolysis, and helps with the longevity of the adhesive interface.4,28,30,31
Depending on the self-etching or demineralization intensity, self-etch adhesives can be divided into four categories: ultra mild (pH ≥ 2.5), mild (pH ≈ 2), intermediately strong (pH ≈1.5), and strong (pH <1).32 The bonding agent used in this study is considered ultra mild due to its pH level (> 2.5).9,33 It has been mentioned, when treating the enamel surface, the acidic primers are not as efficient as that observed with the etch-and-rinse adhesive systems.9,16,18 Thus, to provide better micromechanical retention to the restorations, to control, or even to prevent the gap formation and consequently the marginal enamel discoloration,16 the prior enamel selective etching was performed before the acidic primer application. However, in up to 2 years of clinical analysis, it was not possible to observe the real need for enamel selective etching because both techniques showed no statistical significant difference. Similar results were reported by Abdalla et al,34 which found acid etching prior to the application of self-etch adhesive did not improve the overall quality of the restorations. The bonding agent contains 10-methacryloyloxydecyl dihydrogen phosphate (10-MDP) functional monomer, which has been rated as the most effective monomer for ionic binding to hydroxyapatite, thereby definitely contributing to the bond stability for the long term.35 The chemical reaction and micromechanical retention provided by hybridization yield a strong and durable adhesion to dental substrate. Also, 10-MDP seems to produce more stable chemical reaction with hydroxyapatite than other adhesive monomers, such as 4-methacryloyloxyethy trimellitate anhydride (4-META), 4-methacryloxyethyl trimellitic (4-MET), MAC10, and 4-Phenyl-P.33,36,37
A parallel can be made with the present study and Perdigao et al,38 which stated that ultra mild self-etch adhesive (pH ≈ 2.7) shallowly interacts with enamel. All NCCLs in the present study were beveled, therefore, promoting the removal of the aprismatic enamel layer, which may have helped with the marginal sealing of cervical restorations, especially with those that received only the application of the acidic primer (G2). Indeed, it has been observed that the beveling provides better esthetics, improves the adhesive interface and its interaction to tooth tissues, and enhances bond strength. It also reduces the stress generated in the bond interface by polymerization, temperature changes, or masticatory loads.2,38
Facing such surveys and equivalence of clinical outcomes for retention, marginal integrity, and marginal discoloration, the present study is in accordance with previous studies that suggested that the ultra-mild self-etching adhesives do not require enamel selective etching.9,39,40 Peumans et al19 reported a subtle clinical superiority of restorations that received the selective conditioning of enamel using a two-step self-etch adhesive after 8 years. The marginal discolorations, when present, were subtle and located only in the interface dentin/restoration, which can be justified by the excellent hybridization of adhesive systems to enamel. Can Say et al33 found a significantly higher percentage of marginal discoloration in the non-etched group than in the previously etched group after 3 years, but the bevel was not performed. The present study also observed at 1 year and 2 years of clinical analysis a significant decrease in tooth sensitivity. This excellent result can be explained by dentin hybridization and satisfactory sealing of the enamel and dentin interfaces, because formation of the hybrid layer and resin tags within the dentin tubules were able to reduce the permeability of the exposed dentin,41,43 noting the most common manifestation of this adhesion would be the postoperative sensitivity.41,44
The improper use of any adhesive system can lead to undesirable effects over time, including recurrent caries around restorations.11,20 According to our results, no restoration showed secondary caries, which is a similar finding in other research.4,9,18,32,39,40 Studies19,45,46 have demonstrated the incorporation of the antibacterial monomer methacryloyloxydodecylpyridinium bromide (MDPB) into an adhesive system reduces bacterial contamination and contributes to preventing secondary caries at the tooth-restoration interface. In addition, MDPB is a more hydrophobic monomer than the 2-hydroxyethyl methacrylate (HEMA) present in most adhesives, which can help with the hydrolytic stability of the adhesive interface.19,45
Along with the monomer MDPB, Clearfil Protect Bond contains sodium fluoride in its composition,13 which helps to control and prevent caries around the restoration.47 Moreover, fluoride can assist in obtaining greater stability of the adhesive interface and help with the formation of acid-base resistant zone, present in adhesives, which also aids in controlling secondary carious lesions.33,48 A recent in vitro study49 found sodium fluoride decreased the activities of salivary MMPs (in this case, it was MMP-2 and MMP-9). It is premature to presume sodium fluoride inside an adhesive might act against dentin MMPs, but it is a thrilling and encouraging result for further studies. Considering the limitations of this study, it can be concluded that the nanofilled two-step etch-and-rinse and the two-step self-etch containing MDPB and fluoride adhesive systems showed satisfactory clinical performance over 1 year and 2 years, regardless if the previous acid etching was performed.
Clinical Implications
No clinical relevant difference between a nanofilled two-step etch-and-rinse and self-etch adhesive containing MDPB and fluoride was found following the USPHS criteria after 2 years.
Conclusion
It can be concluded that the nanofilled two-step etch-and-rinse and the two-step self-etch containing MDPB and fluoride adhesive systems showed satisfactory clinical performance over 1 year and 2 years. This was regardless of whether the previous acid etching was performed, considering that the enamel bevel was performed on all evaluated restorations.
About the Authors
Fernanda Garcia de Oliveira, DDS, MS, PhD
Professor
Department of Restorative Dentistry
UNESP – Univ Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
Lucas Silveira Machado, DDS, MS, PhD
Professor
Department of Restorative Dentistry
UNESP – University Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
Daniel Sundfeld-Neto, DDS, MS
PhD Candidate Department of Restorative Dentistry
UNICAMP – University of Campinas Piracicaba Dental School
Piracicaba, São Paulo, Brazil
Marcelo Giannini, DDS, MS, PhD
Professor
Department of Restorative Dentistry
UNICAMP – University of Campinas Piracicaba Dental School
Piracicaba, São Paulo, Brazil
André Luiz Fraga Briso, DDS, MS, PhD
Professor
Department of Restorative Dentistry
UNESP – Univ Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
Paulo Henrique dos Santos, DDS, MS, PhD
Professor
Department of Dental Materials and Prosthodontics
UNESP – Univ Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
Maria Lúcia Marçal Mazza Sundefeld, MS, PhD
Professor
Department of Pediatric and Community Dentistry
UNESP – Univ Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
Renato Herman Sundfeld, DDS, MS, PhD
Department of Restorative Dentistry
UNESP – Univ Estadual Paulista
Araçatuba Dental School
Araçatuba, São Paulo, Brazil
References
1. van Dijken JW, Pallesen U. Long-term dentin retention of etch-and-rinse and self-etch adhesives and a resin-modified glass ionomer cement in non-carious cervical lesions. Dent Mater. 2008;24(7):915-922.
2. Kubo S, Yokota H, Yokota H, Hayashi Y. Challenges to the clinical placement and evaluation of adhesively-bonded, cervical composite restorations. Dent Mater. 2013;29(1):10-27.
3. Grippo JO, Simring M, Coleman TA. Abfraction, abrasion, biocorrosion, and the enigma of noncarious cervical lesions: a 20-year perspective. J Esthet Restor Dent. 2012;24(1):10-23.
4. Loguercio AD, Mânica D, Ferneda F, et al. A randomized clinical evaluation of a one- and two-step self-etch adhesive over 24 months. Oper Dent. 2010;35(3):265-272.
5. Oliveira FG, Machado LS, Rocha EP, et al. Clinical evaluation of a composite resin and a resin-modified glass-ionomer cement in non-carious cervical lesions: one-year results. Int J Clin Dent. 2012;5(1):155-166.
6. Peumans M, Kanumilli P, De Munck J, et al. Clinical effectiveness of contemporary adhesives: a systematic review of current clinical trials. Dent Mater. 2005;21(9):864-881.
7. Carvalho RM, Manso AP, Geraldeli S, et al. Durability of bonds and clinical success of adhesive restorations. Dent Mater. 2012;28(1):72-86.
8. Chee B, Rickman LJ, Satterthwaite JD. Adhesives for the restoration of non-carious cervical lesions: a systematic review. J Dent. 2012;40(6):443-452.
9. Ozel E, Say EC, Yurdaguven H, Soyman M. One-year clinical evaluation of a two-step self-etch adhesive with and without additional enamel etching technique in cervical lesions. Aust Dent J. 2010;55(2):156-161.
10. Sabatini C. Effect of a chlorhexidine-containing adhesive on dentin bond strength stability. Oper Dent. 2013;38(6):609-617.
11. Christensen GJ. Preventing postoperative tooth sensitivity in class I, II and V restorations. J Am Dent Assoc. 2002;133(2):229-231.
12. Sundfeld RH, Valentino TA, de Alexandre RS, et al. Hybrid layer thickness and resin tag length of a self-etching adhesive bonded to sound dentin. J Dent. 2005;33(8):675-681.
13. Pinto CF, Paes-Leme AF, Ambrosano GM, Giannini M. In vitro secondary caries inhibition by adhesive systems in enamel around composite restorations. Oper Dent. 2010;35(3):345-352.
14. Moura SK, Reis A, Pelizzaro A, et al. Bond strength and morphology of enamel using self-etching adhesive systems with different acidities. J Appl Oral Sci. 2009;17(4):315-325.
15. Frankenberger R, Tay FR. Self-etch vs etch-and-rinse adhesives: effect of thermo-mechanical fatigue loading on marginal quality of bonded resin composite restorations. Dent Mater. 2005;21(5):397-412.
17. Sundfeld RH, de Oliveira CH, da Silva AM, et al. Resin tag length of one-step and self-etching adhesives bonded to unground enamel. Bull Tokyo Dent Coll. 2005;46(3):43-49.
18. Torii Y, Itou K, Nishitani Y, et al. Effect of phosphoric acid etching prior to self-etching primer application on adhesion of resin composite to enamel and dentin. Am J Dent. 2002;15(5):305-308.
19. Peumans M, De Munck J, Van Landuyt KL, et al. Eight-year clinical evaluation of a 2-step self-etch adhesive with and without selective enamel etching. Dent Mater. 2010;26(12):1176-1184.
20. Bortolotto T, Doudou W, Stavridakis M, et al. Marginal adaptation after aging of a self-etching adhesive containing an antibacterial monomer. J Adhes Dent. 2007;9(3):311-317.
21. Moretto SG, Russo EM, Carvalho RC, et al. 3-year clinical effectiveness of one-step adhesives in non-carious cervical lesions. J Dent. 2013;41(8):675-682.
22. Van Meerbeek B, Peumans M, Poitevin A, et al. Relationship between bond-strength tests and clinical outcomes. Dent Mater. 2010;26(2):e100-e121.
23. Van Meerbeek B, De Munck J, Yoshida Y, et al. Buonocore memorial lecture. Adhesion to enamel and dentin: current status and future challenges. Oper Dent. 2003;28(3):215-235.
24. Hashimoto M. A review—micromorphological evidence of degradation in resin-dentin bonds and potential preventional solutions. J Biomed Mater Res B Appl Biomater. 2010;92(1):268-280.
25. Mazzoni A, Scaffa P, Carrilho M, et al. Effects of etch-and-rinse and self-etch adhesives on dentin MMP-2 and MMP-9. J Dent Res. 2013;92(1):82-86.
26. Pashley DH, Tay FR, Breschi L, et al. State of the art etch-and-rinse adhesives. Dent Mater. 2011;27(1):1-16.
27. Pashley DH, Tay FR, Yiu C, et al. Collagen degradation by host-derived enzymes during aging. J Dent Res. 2004;83(3):216-221.
28. Schulze KA, Oliveira SA, Wilson RS, et al. Effect of hydration variability on hybrid layer properties of a self-etching versus an acid-etching system. Biomaterials. 2005;26(9):1011-1018.
29. Brackett WW, Ito S, Tay FR, et al. Microtensile dentin bond strength of self-etching resins: effect of a hydrophobic layer. Oper Dent. 2005;30(6):733-738.
30. Giannini M, Mettenburg D, Arrais CA, Rueggeberg FA. The effect of filler addition on biaxial flexure strength and modulus of commercial dentin bonding systems. Quintessence Int. 2011;42(2):e39-e43.
31. Mortavazi V, Samimi P, Rafizadeh M, Kazemi S. A randomized clinical trial evaluating the success rate of ethanol wet bonding technique and two adhesives. Dent Res J (Isfahan). 2012;9(5):588-594.
32. Liu Y, Tjäderhane L, Breschi L, et al. Limitations in bonding to dentin and experimental strategies to prevent bond degradation. J Dent Res. 2011;90(8):953-968.
33. Can Say E, Ozel E, Yurdagüven H, Soyman M. Three-year clinical evaluation of a two-step self-etch adhesive with or without selective enamel etching in non-carious cervical sclerotic lesions. Clin Oral Investig. 2014;18(5):1427-1433.
34. Khoroushi M, Mansoori M. Marginal sealing durability of two contemporary self-etch adhesives. ISRN Dent. 2012;2012:204813.
35. Abdalla AI, El Sayed HY. Clinical evaluation of a self-etch adhesive in non-carious cervical lesions. Am J Dent. 2008;21(5):327-330.
36. Ermis RB, Van Landuyt KL, Cardoso MV, et al. Clinical effectiveness of a one-step self-etch adhesive in non-carious cervical lesions at 2 years. Clin Oral Investig. 2012;16(3):889-897.
37. Cardoso MV, De Almeida Neves A, Mine A, et al. Current aspects on bonding effectiveness and stability in adhesive dentistry. Aust Dent J. 2011;56(suppl 1):31-44.
38. Perdigão J, Lopes MM, Gomes G. In vitro bonding performance of self-etch adhesives: II—ultramorphological evaluation. Oper Dent. 2008;33(5):534-549.
39. Yokota H, Kawaguchi M, Ohsawa M, et al. Finite element analysis of cervical resin composite restorations – the effect of enamel bevel on stresses generated by thermal change and occlusal force. Japan J Conserv Dent. 2007;50(5):545-552.
40. Eliguzeloglu Dalkilic E, Omurlu H. Two-year clinical evaluation of three adhesive systems in non-carious cervical lesions. J Appl Oral Sci. 2012;20(2):192-199.
41. Peumans M, de Munck J, Van Landuyt K, et al. Three-year clinical effectiveness of a two-step self-etch adhesive in cervical lesions. Eur J Oral Sci. 2005;113(6):512-518.
42. Carvalho AO, Oliveira MT, Nikaido T, et al. Effect of adhesive system and application strategy on reduction of dentin permeability. Braz Oral Res. 2012;26(5):397-403.
43. Sahin C, Cehreli ZC, Yenigul M, Davangac B. In vitro permeability of etch-and-rinse and self-etch adhesives used for immediate dentin sealing. Dent Mater J. 2012;31(3):401-408.
44. Pashley DH, Pashley EL, Carvalho RM, Tay FR. The effects of dentin permeability on restorative dentistry. Dent Clin North Am. 2002;46(2):211-245.
45. Akpata ES, Sadig W. Post-operative sensitivity in glass-ionomer versus adhesive resin-lined posterior composites. Am J Dent. 2001;14(1):34-38.
46. Imazato S, Tay FR, Kaneshiro AV, et al. An in vivo evaluation of bonding ability of comprehensive antibacterial adhesive system incorporating MDPB. Dent Mater. 2007;23(2):170-176.
47. Imazato S, Kuramoto A, Takahashi Y, et al. In vitro antibacterial effects of the dentin primer of Clearfil Protect Bond. Dent Mater. 2006;22(6):527-532.
48. Zhou SL, Zhou J, Watanabe S, et al. In vitro study of the effects of fluoride-releasing dental materials on remineralization in an enamel erosion model. J Dent. 2012;40(3):255-263.
49. Shinohara MS, Yamauti M, Inoue G, et al. Evaluation of antibacterial and fluoride-releasing adhesive system on dentin—microtensile bond strength and acid-base challenge. Dent Mater J. 2006;25(3):545-552.