Retrospective Study to Determine Patient Satisfaction of Immediately Placed and Provisionalized Implants in the Esthetic Zone From a US Private-Practice Research Network
E. Todd Scheyer, DDS, MS; Christopher Richardson, DMD, MS; George Mandelaris, DDS, MS; Stephen Pickering, DDS, MSD; Marc Nevins, DMD, MMSc; Bryan Pope, DMD, MSD; Jim Janakievski, DDS; Gregory Toback, DMD, MS; and Rick H. Heard, DDS, MS
ABSTRACT:
Background: Immediately placed/immediately restored dental implants in the esthetic zone are judged by not only their functional success but also the appearance and acceptance of the restorative outcome. The purpose of this study was to retrospectively evaluate in a private-practice setting the satisfaction of both patients and doctors regarding immediately placed/immediately restored implants in the esthetic zone. Methods: The author group consists of nine board-certified periodontists. Each private practice contributed to the patient population of this study through a primarily referral-based source. In a 6-month period, practices evaluated patients who were candidates for dental implant replacement with teeth Nos. 5 through 12 scheduled for extraction. All patients received informed consent and were asked if their data could be used with a visual analog scale (VAS) they graded. Pretreatment and 6-month post-final restoration loading was compared for statistically significant changes in reference to crestal bone changes, papilla index score (PIS), facial gingival margin stability (FGMS), and investigator/patient esthetic evaluations using a VAS. Results: Thirty-five patients were included in the study with a total of 35 implants placed and 32 restored with a final restoration. Implants were followed for an average of 15.4 months prior to reporting. A total of three failures were encountered. The PIS resulted in an average score of 2.7. VAS resulted in an average score of 9.3 by the surgeons and 9.5 by the patients. The FGMS accounted for 76% of the implants with no change, 15% demonstrating recession, and 9% demonstrating coronal migration. Conclusions: Immediately placed and immediately temporized implants in the esthetic zone demonstrated a successful outcome that was highly acceptable to patients in private-practice settings from a diverse group of private periodontal practices.
The success of implants placed and restored using an immediate approach has been studied extensively.1-13 This treatment modality is especially demanding in the esthetic zone, with success measured by the appearance and acceptance of the restorative outcome in addition to proper functionality.1,14-24 Multiple quantifiable factors have been evaluated for judging success and include: soft-tissue stability,25 buccal bone stability,26 crestal bone maintenance,27 and overall survival rate.25-37 The ultimate determinant of a successful implant-supported restoration in the esthetic zone, however, is patient satisfaction. A search of the literature yielded a paucity of data reporting patient satisfaction in a quantifiable manner.38
Controlled clinical trials provide an effective method of assessing techniques and gathering data that are measureable. Transitioning techniques from clinical research to private practice, however, is oftentimes slow, and they can be difficult to apply to the everyday delivery of patient care. Private practice does not afford the implant surgeon or restorative dentist the opportunity to subject their patient populations to procedures that have not first demonstrated success through sound clinical research completed in a practice-based research network (PBRN). Rather than resorting to an unproven technique that might have only a better chance of success, clinicians need to provide their patients the optimal treatment with the highest potential for success. Immediately placed/immediately restored implants have shown success rates comparable to other implant modalities such as delayed placement or delayed restoration.25,32,33 However, the relative lack of data regarding patient satisfaction should be noted. In fact, the US Food and Drug Administration has elevated patient-reported outcomes to a primary outcome variable,34 so a patient’s assessment of outcomes will become more important with future research.
The purpose of this study was to retrospectively evaluate from within a private-practice setting patient satisfaction of immediately placed/immediately restored dental implants in the esthetic zone. This study is a retrospective nonsponsored analysis of implants that were immediately placed in the esthetic zone and received immediate provisional crowns. The outcomes appear to be favorable with regard to patient and doctor satisfaction and validate the efficiency of a PBRN model of research.
Materials and Methods
The author group consists of nine board-certified periodontists, with an average of 14 years’ experience as private practitioners. Each private practice contributed to the patient population of this study through a primarily referral-based source from a diverse demographic area.
Inclusion Criteria
In a 6-month period, practices evaluated patients who were candidates for dental implant replacement with teeth Nos. 5 through 12 scheduled for extraction. All patients received informed consent and were asked if their data could be used with a visual analog scale (VAS) they graded.39
Surgical and Prosthetic Treatment
The study followed a protocol similar to what has been previously published on immediately placed and immediately provisionalized implants.8 The implant system and design was determined by the surgeon. All dental implants had biologically active surfaces and were placed into immediate extraction sites. (Author’s note: Four implant systems were used: Straumann® SLA Bone Level, Straumann USA, straumann.us; Astra Tech™, DENTSPLY Implants, dentsplyimplants.com; NobelReplace®, Nobel Biocare USA, nobelbiocare.com; 3i, Biomet, Inc., biomet3i.com.) Bone grafting was allowed, if needed. The practitioners, in this retrospective study, made individual decisions regarding the use of graft materials based on the presentation of the case they were treating at that specific time. The decision to include bone grafting could be based on the following: the bone-to-implant distance being 2 mm or greater as indicated in the historical literature as being a critical distance, patients with thin-tissue biotypes, the presence of bone dehiscence or perforation, or simply in circumstances in which the practitioner was concerned about maintaining the horizontal alveolar bone width.40 Cases could be performed closed or open. The utilization of one approach verses the other was strictly an individual surgical decision and based on the need for access to facilitate extraction of the tooth, access to an underlying defect for visualization or debridement, or better visualization of the underlying bone to facilitate implant placement. Cases that required connective tissue grafting or other forms of soft-tissue modification were excluded from the retrospective study as they added an additional layer of surgical complexity and soft-tissue management that was not intended to be the focus of analyzing patient satisfaction with immediate implant placement. Presurgical imaging was performed at the discretion of the surgeon. Surgery could be carried out using computed tomography guidance or be non-computed tomography guided. Informed consent was obtained, including consent for the clinician to use the patient’s data and photographs for publication.
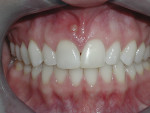
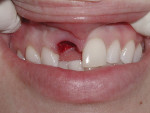
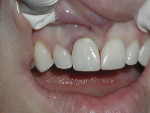
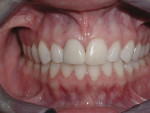
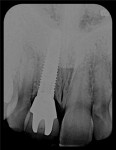
Based on intuitive assessment of implant primary stability, strictly based on insertion torque, implants were subjected to immediate non-occlusal loading. The surgeon and restorative team determined the style of the provisional. Temporary abutments were used to fabricate a composite-resin or acrylic provisional restoration, while UCLA-type or stock abutments were used in most cases to retain the final restoration. An example of the surgical and restorative protocol is depicted in Figure 1 through Figure 6.
Data-Gathering Indices
In private practice, the success of an anterior implant is judged on both objective and subjective factors by the surgeon, restorative dentist, and, most importantly, the patient. The authors analyzed the success of the implants in the following quantifiable manner:
Subjective indices, described as follows, were used to measure the functional and esthetic outcomes. A papilla index score (PIS)41 on the mesial and distal of the restoration was obtained no less than 6 months after the delivery of the final restoration. The PIS designates five different levels of the amount of papillary presence, which is measured from a reference line that passes through the highest gingival curvature of the implant restoration on the facial side and the adjacent permanent tooth. Index score 0 was assigned when papilla was absent. Index score 1 was assessed when less than half of the papillary height was present. Index score 2 indicated that at least half of the height of the papilla was present but did not reach the contact point. Index score 3 was designated when the papilla filled the entire proximal space. Finally, index score 4 was given if the papillae were hyperplastic and overfilled the restoration.
The functional success of the restored implant was recorded as either osseointegrated or failure (+/-). All lost implants were expressed as a percentage.
The doctor and patient esthetic satisfaction was graded using a VAS. This scale was graded from 1 to 10, with 1 representing the worst outcome and 10 representing an excellent esthetic result. The VAS score was recorded on day 0 and again no less than 6 months after the delivery of the final restoration.
The facial gingival margin stability (FGMS) was assessed based on pretreatment comparison to adjacent cementoenamel junction levels on natural teeth verified with nonstandardized digital photographs. The FGMS was recorded as coronal migration (+), no change (=), or recession (-).
Radiographic interproximal crestal bone height was measured as either increased (+), no change (=), or decreased (-) compared to baseline at day of surgery.
Statistical Methods
Pretreatment and 6-month post-final restoration loading was compared for statistically significant changes in reference to crestal bone changes, PIS, FGMS, and investigator/patient esthetic evaluations.
Results
Objective Results
In addition to the nine periodontists, 31 restorative dentists were involved in patient care. Thirty-five patients were included in the study with a total of 35 implants placed and 32 restored with a final restoration. Please note not all patients receiving implants proceed with a final restoration according to the intended time frame if they are satisfied with the esthetic result of the provisional, which was why three were not included here. Implants were followed for an average of 15.4 months prior to reporting. A total of three failures were encountered.
Subjective Results
The average PIS was taken from 32 mesial and distal papillae, resulting in an average score of 2.7. The esthetic satisfaction score taken via a VAS resulted in an average of 9.3 by the surgeons and 9.5 by the patients (Table 1).
The FGMS accounted for 76% of the implants with no change in free gingival margin location, 15% demonstrating recession, and 9% demonstrating coronal migration.
Lastly, the radiographic interproximal crestal bone level height assessment calculated no change in 71% of the implants, increased height in 25%, and decreased height in 4%.
Discussion
One intention of this study was to examine the clinical relevance of immediately placed and restored implants in the esthetic zone to a private practitioner. In other words, can the immediately placed and restored implant in the esthetic zone be predictably successful in a private-practice setting? The diversity of this study with regards to implant systems, methods of surgical placement, and final restorations fabricated by the referring restorative dentists must be taken into account. In fact, this diversity should be viewed as an inherent strength when considering the results and impact of the investigation on the everyday practice of implant dentistry.
This study simply included each patient from a private-practice setting who was an implant candidate for teeth Nos. 5 through 12. The candidacy for implant placement was based on each periodontist’s clinical and educational experience, resulting in a diagnosis and treatment plan for each patient. The candidacy and rationale for immediate implant placement is based on multiple factors that are too extensive to cover within the context of this manuscript.
The patient and doctor satisfaction with the esthetic outcome were each high as indicated by respective VAS scores of 9.5 and 9.3. Other studies have reported patient satisfaction via a categorical description of excellent, very good, good, fair, or poor, but these methods of assessing patient satisfaction were not quantifiable compared to a VAS. Though the majority of patients indicated that the outcome was excellent,32 the use of the VAS provided a less restrictive measureable outcome compared to a list of subjective categories that patients were asked to choose from.
Clinical parameters measuring esthetics included soft-tissue stability of the free gingival margin (FGM) and PIS. Most cases, 85%, demonstrated either no change or coronal migration of the FGM. The PIS score averaged 2.7, which indicates that the majority of cases either had a papilla fill more than half of the proximal space but not completely, or the papilla was completely filling the proximal space. These scores confirmed, via a measureable index, a favorable outcome regarding implants in the esthetic zone.
The average follow-up time in this study was 15.4 months. Studies of longer duration have found that most soft-tissue parameters either remained the same or improved slightly.33,41 Therefore, the authors anticipate that future follow-up of the patients in this study beyond 15 months may find that the initial high degree of satisfaction by both the patients and doctors is maintained or possibly even increased. Due to the PBRN model, long-term follow-up can currently be carried out with an institutional review board submission. It should be noted that the efficiency in recruitment, retention, study completion, and publication is elite.
The recognition of potential risks of this treatment method must be illustrated. The reported success rate from controlled clinical studies is 95% to 97%.1,5,18,22,42 In contrast, the present study revealed a 93% implant survival rate. The differences could be due to the relatively small sample of patients in this study, resulting in an insufficient number to adequately assess the success rate. In addition, the private-practice nature of the patient population introduced the possibility of reduced cooperation by patients with postoperative protocols. The private-practice setting precluded the selection of a large sample size of appropriate cases to offer this particular treatment modality due to a multitude of factors, most notably financial restrictions. In this relatively difficult economic era, patient selection for “elective treatment” may have influenced the authors’ ability to analyze patients for participation within a short enrollment time.
Conclusion
In summary, immediately placed/immediately restored dental implants in the esthetic zone demonstrated a successful outcome that was highly acceptable to patients in a private-practice setting. Furthermore, the clinicians found great value in developing and conducting this research network and feel this method of research has great potential to answer clinical questions that might otherwise go unanswered by traditional academic research.
ABOUT THE AUTHORS
E. Todd Scheyer, DDS, MS
Private Practice, Houston, Texas
Christopher Richardson, DMD, MS
Private Practice, Richmond, Virginia
George Mandelaris, DDS, MS
Private Practice, Park Ridge and Oakbrook Terrace, Illinois
Stephen Pickering, DDS, MSD
Private Practice, San Mateo, California
Marc Nevins, DMD, MMSc
Private Practice, Boston, Massachusetts
Bryan Pope, DMD, MSD
Private Practice, San Mateo, California
Jim Janakievski, DDS
Private Practice, Tacoma, Washington
Gregory Toback, DMD, MS
Private Practice, New London, Connecticut
Rick H. Heard, DDS, MS
Private Practice, Victoria, Texas*All authors are members of the McGuire Institute for Practice based Research (iMc), a not for profit organization.
REFERENCES
1. Avvanzo P, Ciavarella D, Avvanzo A, et al. Immediate placement and temporization of implants: three- to five-year retrospective results. J Oral Implantol. 2009;35(3):136-142.
2. Lee CY, Hasegawa H. Immediate load and esthetic zone considerations to replace maxillary incisor teeth using a new zirconia implant abutment in the bone grafted anterior maxilla. J Oral Implantol. 2008;34(5):259-267.
3. Hall JA, Payne AG, Purton DG, et al. Immediately restored, single-tapered implants in the anterior maxilla: prosthodontic and aesthetic outcomes after 1 year. Clin Implant Dent Relat Res. 2007;9(1):34-45.
4. Solakoglu O, Cooper LF. Immediate implant placement and restoration in the anterior maxilla: a tissue-related approach. Observations at 12 months after loading. Int J Periodontics Restorative Dent. 2006;26(6):571-579.
5. Barone A, Rispoli L, Vozza I, et al. Immediate restoration of single implants placed immediately after tooth extraction. J Periodontol. 2006;77(11):1914-1920.
6. Saadoun AP, Sebbag P. Immediate implant placement and temporization: literature review and case studies. Compend Contin Educ Dent. 2004;25(4):277-286.
7. Locante WM. Single-tooth replacements in the esthetic zone with an immediate function implant: a preliminary report. J Oral Implantol. 2004;30(6):369-375.
8. Kan JY, Rungcharassaeng K, Lozada J. Immediate placement and provisionalization of maxillary anterior single implants: 1-year prospective study. Int J Oral Maxillofac Implants. 2003;18(1):31-39.
9. Saadoun AP. Immediate implant placement and temporization in extraction and healing sites. Compend Contin Educ Dent. 2002;23(4):309-318.
10. Petrungaro PS. Immediate restoration of dental implants in the aesthetic zone. Dent Implantol Update. 2001;12(12):89-95.
11. el Charkawi H. Immediate implant in fresh extraction socket of resected mandibular first molar: a preliminary clinical report. Implant Dent. 2001;10(4):272-279.
12. Kan JY, Rungcharassaeng K. Immediate placement and provisionalization of maxillary anterior single implants: a surgical and prosthodontic rationale. Pract Periodontics Aesthet Dent. 2000;12(9):817-824.
13. Dietz JB Jr. The dental facade: a replacement for teeth removed at the time of insertion of endosseous dental implants. Compend Contin Educ Dent. 1993;14(9):1116-1120.
14. De Rouck T, Collys K, Wyn I, Cosyn J. Instant provisionalization of immediate single-tooth implants is essential to optimize esthetic treatment outcome. Clin Oral Implants Res. 2009;20(6):566-570.
15. Mankoo T. Maintenance of interdental papillae in the esthetic zone using multiple immediate adjacent implants to restore failing teeth—a report of ten cases at 2 to 7 years follow-up. Eur J Esthet Dent. 2008;3(4):304-322.
16. Lops D, Chiapasco M, Rossi A, et al. Incidence of inter-proximal papilla between a tooth and an adjacent immediate implant placed into a fresh extraction socket: 1-year prospective study. Clin Oral Implants Res. 2008;19(11):1135-1140.
17. den Hartog L, Slater JJ, Vissink A, et al. Treatment outcome of immediate, early and conventional single-tooth implants in the aesthetic zone: a systematic review to survival, bone level, soft-tissue, aesthetics and patient satisfaction. J Clin Periodontol. 2008;35(12):1073-1086.
18. De Rouck T, Collys K, Cosyn J. Immediate single-tooth implants in the anterior maxilla: a 1-year case cohort study on hard and soft tissue response. J Clin Periodontol. 2008;35(7):649-657.
19. McArdle B. Aesthetic restoration of an immediate implant. Dent Today. 2007;26(4):112,114.
20. Harvey BV. Optimizing the esthetic potential of implant restorations through the use of immediate implants with immediate provisionals. J Periodontol. 2007;78(4):770-776.
21. Zeren KJ. Minimally invasive extraction and immediate implant placement: the preservation of esthetics. Int J Periodontics Restorative Dent. 2006;26(2):171-181.
22. Lindeboom JA, Frenken JW, Dubois L, et al. Immediate loading versus immediate provisionalization of maxillary single-tooth replacements: a prospective randomized study with BioComp implants. J Oral Maxillofac Surg. 2006;64(6):936-942.
23. Testori T, Bianchi F, Del Fabbro M, et al. Implant aesthetic score for evaluating the outcome: immediate loading in the aesthetic zone. Pract Proced Aesthet Dent. 2005;17(2):123-130.
24. Palti A. Immediate placement and loading of implants in extraction sites: procedures in the aesthetic zone. Dent Implantol Update. 2004;15(6):41-47.
25. Canullo L, Iurlaro G, Iannello G. Double-blind randomized controlled trial study on post-extraction immediately restored implants using the switching platform concept: soft tissue response. Preliminary report. Clin Oral Implants Res. 2009;20(4):414-420.
26. Degidi M, Nardi D, Daprile G, Piattelli A. Buccal bone plate in the immediately placed and restored maxillary single implant: a 7-year retrospective study using computed tomography. Implant Dent. 2012;21(1):62-66.
27. Pieri F, Aldini NN, Marchetti C, Corinaldesi G. Influence of implant-abutment interface design on bone and soft tissue levels around immediately placed and restored single-tooth implants: a randomized controlled clinical trial. Int J Oral Maxillofac Implants. 2011;26(1):169-178.
28. Zembic A, Johannesen LH, Schou S, et al. Immediately restored one-piece single-tooth implants with reduced diameter: one-year results of a multi-center study. Clin Oral Implants Res. 2012;23(1):49-54.
29. Grandi T, Guazzi P, Samarani R, Garuti G. Immediate positioning of definitive abutments versus repeated abutment replacements in immediately loaded implants: effects on bone healing at the 1-year follow-up of a multicentre randomised controlled trial. Eur J Oral Implantol. 2012;5(1):9-16.
30. Turkyilmaz I. Immediate provisional restoration of implant placed using flapless surgery and ridge mapping. Case report. NY State Dent J. 2011;77(3):21-23.
31. Traini T, Pettinicchio M, Murmura G, et al. Esthetic outcome of an immediately placed maxillary anterior single-tooth implant restored with a custom-made zirconia-ceramic abutment and crown: a staged treatment. Quintessence Int. 2011;42(2):103-108.
32. Vidal R, Greenwell H, Hill M, et al. Success rate of immediate implants placed and restored by novice operators. Implant Dent. 2010;19(1):81-90.
33. Tortamano P, Camargo LO, Bello-Silva MS, Kanashiro LH. Immediate implant placement and restoration in the esthetic zone: a prospective study with 18 months of follow-up. Int J Oral Maxillofac Implants. 2010;25(2):345-350.
34. US Dept of Health and Human Services. Guidance for Industry. Patient-Reported Outcome Measures: Use in Medical Product Development to Support Labeling Claims. Silver Spring, Md: Food and Drug Administration, Center for Drug Evaluation and Research, Center for Biologics Evaluation and Research, Center for Devices and Radiological Health; 2009.
35. den Hartog L, Raghoebar GM, Stellingsma K, Meijer HJ. Immediate loading and customized restoration of a single implant in the maxillary esthetic zone: a clinical report. J Prosthet Dent. 2009;102(4):211-215.
36. Degidi M, Novaes AB Jr, Nardi D, Piattelli A. Outcome analysis of immediately placed, immediately restored implants in the esthetic area: the clinical relevance of different interimplant distances. J Periodontol. 2008;79(6):1056-1061.
37. Schwartz-Arad D, Laviv A, Levin L. Survival of immediately provisionalized dental implants placed immediately into fresh extraction sockets. J Periodontol. 2007;78(2):219-223.
38. Grütter L, Belser UC. Implant loading protocols for the partially edentulous esthetic zone. Int J Oral Maxillofac Implants. 2009;24 suppl:169-179.
39. Miller MD, Ferris DG. Measurement of subjective phenomena in primary care research: the Visual Analogue Scale. Fam Pract Res J. 1993;13(1):15-24.
40. Weigl P, Strangio A. The impact of immediately placed and restored implants single-tooth implants on hard and soft tissues in the anterior maxilla. Eur J Oral Implantol. 2016;9(Suppl 1):S89–S106.
41. Jemt T. Regeneration of gingival papillae after single-implant treatment. Int J Periodontics Restorative Dent. 1997;17(4):326-333.
42. Maló, P, Friberg B, Polizzi G, et al. Immediate and early function of Brånemark System implants placed in the esthetic zone: a 1-year prospective clinical multicenter study. Clin Implant Dent Relat Res. 2003;5 suppl 1:37-46.