Multidisciplinary Treatment of Anterior Worn Dentition: A Staged Approach
Abstract:
This case involving a male patient with long-standing wear on his anterior teeth demonstrates the importance of an accurate risk profile and prognosis. It also shows an example of a patient who, as is frequently the case, was aware of his problem but chose not to address it until after many years, being finally motivated by a change in marital status. Upon examination, it was determined that the severe attrition was due to the position of the teeth, and the functional diagnosis was a constricted chewing pattern. Orthodontic therapy was a central aspect of the treatment plan, followed initially by a composite trial restoration of the anterior teeth, and, finally, placement of porcelain crowns. Careful communication among the treating dentist, orthodontist, and the dental laboratory at specific phases of the treatment proved to play a pivotal role in achieving an exceptional esthetic result and stable functional bite.
Determining an accurate risk profile and prognosis is critical in order to properly plan and deliver a treatment that decreases risk, improves prognosis, and achieves a long-term stable result. Additionally, open communication and working together with both the patient and the other dental specialists is essential for clinicians to reach the determined treatment goals and desired results.
In this case, the patient presented with long-standing wear on his anterior teeth. Although he had been aware of this problem over the course of the previous 10 years, he had never been motivated to treat the condition until he married and his new spouse expressed concern about his worn smile. During his comprehensive oral examination, it was determined that the severe anterior attrition was a result of the position of his teeth. The functional diagnosis was a constricted chewing pattern. Since his posterior teeth were primarily unrestored, orthodontics was recommended as part of the treatment option to improve his smile. Careful planning with the orthodontist was required to improve the tooth position and alignment, thereby improving the function and providing sufficient restorative space to replace the lost anterior tooth length.
Clinical Case Overview
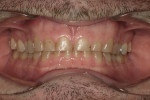
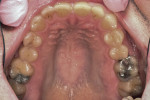
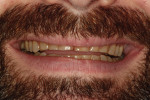
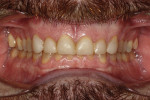
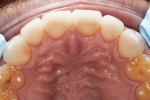
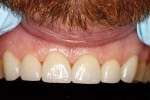
The 42-year-old male patient presented with concerns about the excessive wear of his front teeth and an inability to show his teeth when he smiled (Figure 1 and Figure 2). His maxillary and mandibular anterior teeth showed severe wear for his age. His maxillary central incisors measured only 6 mm vertically. His posterior teeth showed signs of erosion, but had minimal attrition and were primarily unrestored. His medical history was non-contributory.
Diagnostic Findings, Risk Assessment, and Prognosis
Periodontal: The periodontal examination revealed pocketing of 4 mm in the mandibular molars, with readings of 3 mm or less elsewhere. The radiographs revealed generalized minimal horizontal bone loss (< 10%). His oral hygiene was fair. The periodontal diagnosis was AAP type II.
Risk: Low
Prognosis: Good
Biomechanical: The patient had no observable caries, clinically or radiographically. There were several restorations on the posterior teeth; the posterior teeth also had slight areas of erosion. The maxillary and mandibular anterior teeth exhibited erosion, likely due to the exposed dentin from the functional component. Due to the loss of tooth structure anteriorly from attrition, this increased the risk and negatively affected the prognosis.
Risk: Moderate
Prognosis: Fair
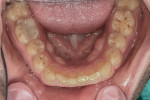
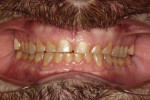
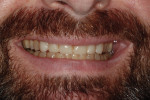
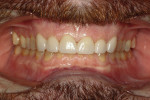
Functional: The patient reported no discomfort in his temporomandibular joints. Both joints had negative load tests and there were no discernable joint sounds. However, the patient did report feeling tightness and discomfort bilaterally in his masseter muscles. Severe wear of 4 mm to 5 mm was observed on all of his maxillary and mandibular anterior teeth from cuspid to cuspid. Minimal wear was noted on the posterior teeth. On the dental history evaluation, he noted that his front teeth had become shorter over the past 5 years. These findings, in particular the severe wear isolated to the front teeth, were consistent with the diagnosis of a constricted chewing pattern1 (Figure 3 and Figure 4).
Risk: Moderate
Prognosis: Poor
Dentofacial: In full smile, or when asked to say “EEEE” with the lips retracted, the patient barely showed the incisal third of his anterior teeth. With the lips in repose, no tooth structure was visible. There was no gingival display in his widest smile. This was consistent with a diagnosis of low lip dynamics and minimal tooth display.
Risk: Low
Prognosis: Hopeless
Treatment Goals
The goals of treatment were threefold:
• The first objective was to improve the worn smile with a conservative, minimally invasive treatment.
• The next goal was to improve the functional risk and prognosis as well as the dentofacial prognosis while minimizing necessary tooth removal and maintaining the periodontal health. This would be accomplished by repositioning the teeth orthodontically to correct the constricted chewing pattern and create restorative space anteriorly to allow restoration of the maxillary and mandibular anterior teeth to a more optimal 10-mm length.
• Finally, the treatment would be staged by restoring the anterior teeth initially with composite as a trial during the first 6 months after orthodontic completion. This would also accommodate the patient’s financial concerns and, at the same time, determine if the tooth length was acceptable and appropriate for him prior to the placement of more definitive porcelain crowns.2
Treatment Plan
The treatment plan consisted of the following steps:
• A detailed referral letter thoroughly describing the diagnosis, treatment goals, and restorative plan was sent to the orthodontist prior to the patient’s consultation appointment. This communication allowed for an efficient and productive consultation for the patient at the orthodontist’s office. Following the patient consultation, a meeting with the orthodontist was arranged to communicate and share a detailed discussion of the restorative goals and realistic results that could be achieved orthodontically.
• After completion of the orthodontic treatment, a diagnostic wax-up of the anterior teeth was planned to be done on mounted models utilizing the Kois Dento-Facial Analyzer™.
• A putty stent of the diagnostic wax-up would be fabricated to allow direct composite “test teeth” to be created.
• At the completion of the test period, a Kois deprogrammer would be utilized to confirm a healthy, stable, and acceptable occlusion, or allow for a controlled occlusal adjustment if needed.
• Preparation and fabrication of e.max™ (Ivoclar Vivadent, www.ivoclarvivadent.com) porcelain crowns on the anterior teeth would be the final step in the treatment.
Treatment Phases
Phase 1: Orthodontic Treatment
The patient was in full fixed orthodontic brackets and wires for 13 months. The maxillary and mandibular incisors were intruded about 1 mm, the upper incisors were proclined about 2 mm, and the lower incisors were maintained horizontally back as much as possible. During the orthodontic treatment, as his constriction was being relieved and the frictional wear was removed from his anterior teeth, the patient reported an improvement in his masseter muscle discomfort. At the conclusion of the orthodontic treatment, the patient had an anterior open bite in the incisor area and a Class I occlusion from the cuspids posteriorly. The orthodontist was concerned about stabilization of the incisor positions prior to completion of the anterior restorations, so a bonded lingual mandibular retainer and a full-coverage maxillary retainer were provided (Figure 5 and Figure 6).
Phase 2: Preliminary Restorative Treatment
Post-orthodontic models were mounted using the Kois Dento-Facial Analyzer for the maxillary cast. A diagnostic wax-up was fabricated by the dental laboratory with the goal of creating a normal maxillary anterior tooth length that would be esthetically pleasing in his face. A putty stent was made on the wax-up and sectioned to expose the facial surfaces of the maxillary teeth. The palatal portion of the stent with the incisal edge attached was used to build direct composite (TPH3™, DENTSPLY, www.dentsply.com) restorations on the maxillary teeth.3 The restorative space achieved by the orthodontic movement did not allow for both the maxillary and mandibular anterior teeth to be restored. In order to lengthen and properly contour the maxillary anterior teeth, these teeth required all of the space made available by the orthodontic treatment. Because of the patient’s low lip dynamics this resulted in a very acceptable esthetic result. The composite test teeth were adjusted so that when the patient sat up and chewed on 200-micron articulating paper they did not hold shimstock and showed no blue streaks, thus confirming that the new restorations did not introduce interferences in the patient’s envelope of function4 (Figure 7 and Figure 8).
Phase 3: Deprogramming
Six months following the placement of the direct composite transitional bonding, a Kois deprogrammer was utilized to test and confirm that the patient was in acceptable function.5 The 6-month time period was chosen to allow sufficient time for the new alignment and occlusion to settle and stabilize. This step involving the Kois deprogrammer may have been unnecessary as there was no chipping or wear on the composite test teeth, indicating an acceptable function; additionally, when the patient reviewed his dental history form (Kois Center, www.koiscenter.com) all questions relating to bite, jaw, and function were answered negative once the orthodontics were completed.
Phase 4: Restoration
Once the new tooth position was confirmed to be stable and the patient expressed approval and was happy with his new smile, the decision was made to definitively restore his maxillary anterior teeth with e.max crowns. The composite build-ups were used as a shape and contour guide for the definitive crowns, and a very acceptable esthetic result was achieved (Figure 9 through Figure 12).
Discussion and Conclusions
As a clinician, it is interesting to discover the motivating factor(s) for a patient to seek treatment. Years may pass that negatively affect both a patient’s risk and prognosis even though the patient has been well informed of the potential impact of their decisions to forego treatment. In the present case, it wasn’t until the patient married that he became more self-conscious of his worn teeth and unappealing smile.
Comprehensive dental treatment often becomes multidisciplinary, involving teamwork and requiring the treating dentist to work together with perhaps medical professionals, dental specialists, and dental laboratories as needed. In this case, careful communication with the orthodontist and the dental laboratory at specific phases of the treatment resulted in an exceptional esthetic result and a stable and low-risk acceptable functional bite.
Acknowledgments
The author wishes to acknowledge the excellent orthodontic treatment performed by Dr. J.D. Wilcox of Kamloops, British Columbia, Canada, and the exceptional lab work of Jaimie and Jonathan Schell and team at Schell Dental Ceramics in Kelowna, British Columbia, Canada.
About the Author
Chris Wilson, DMD
Private Practice
Kamloops, British Columbia, Canada
References
1. Kois JC. Functional Occlusion: Science Driven Management Manual. Seattle, WA: Kois Center; 2008.
2. Bynum JH. Clinical case report: Testing occlusal management, previewing anterior esthetics, and staging rehabilitation with direct composite and Kois deprogrammer. Compend Contin Educ Dent. 2010;31(4):298-306.
3. Hulac S. “Training Teeth”: transitional resin bonding for diagnostic purposes. Compend Contin Educ Dent. 2013;34(9):686-690.
4. Kois JC. Anterior wear: orthodontic and restorative management. Compend Contin Educ Dent. 2009;30(7):420-429.
5. Jayne D. A deprogrammer for occlusal analysis and simplified accurate case mounting. J Cosmet Dent. 2006;21(4):96-102.