Esthetics Built to Last: Treatment of Functional Anomalies May Need to Precede Esthetic Corrections
Joyce L. Bassett, DDS, FAACD
Abstract:
In this case of a 33-year-old male patient seeking a more esthetically pleasing smile, comprehensive restorative treatment planning included recognition of the patient’s incisor position and morphology, dentofacial requirements, and appropriate vertical dimension. The accepted treatment plan consisted of orthodontic correction of the patient’s anterior constriction, followed by placement of eight maxillary veneers and composite augmentation on the mandibular incisors and canines. Keys to achieving a successful outcome included knowledge of smile design, material selection, and preparation techniques. The case demonstrates how functional problems oftentimes must be addressed before esthetic correction can be made.
The relationship between form and function precludes treating anterior teeth as cosmetic challenges alone. Comprehensive restorative treatment planning must include recognition of patients’ incisor position and morphology along with their dentofacial requirements, and determining an appropriate vertical dimension. Additionally, to ensure restoration longevity, functional assessments of bite force management, envelope development, occlusal guidance, and parafunctional forces must be understood and identified so the final restoration design will predictably accommodate the intraoral forces. In order to achieve esthetically exquisite anterior restorations, the clinician should have knowledge of smile design, material selection, and preparation techniques.
Clinical Case Overview
Patient History and Chief Concern
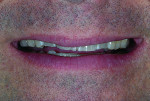
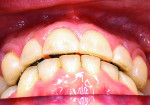
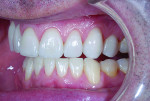
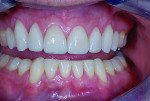
A 33-year-old man presented for assessment of his smile, seeking a cosmetic solution to his condition. He was displeased with the lack of tooth display and stated that in order to see his teeth, he had to open his mouth and pull his lips back, only to expose short, broken, worn, and discolored teeth (Figure 1).
His medical history was noncontributory. He reported orthodontic treatment during childhood, which included the extraction of the four first bicuspids. He was aware of clenching and grinding in his sleep. A nightguard had previously been recommended to him, but he had declined to proceed with that treatment. The patient received a comprehensive examination and complete records, including a full series of radiographs, a panorex, diagnostic models, and photographs.
Diagnostic Findings, Risk Assessment, and Prognosis
An individual risk assessment is critical for determining the most appropriate treatment plan. There can be multiple treatment plans, but only one diagnosis. The goal is to decrease the risk and increase the prognosis.1
Periodontal: Periodontal pocket depths of 3 mm to 4 mm were noted, with no bleeding on probing present. Bone support was within 2 mm of the cementoenamel junction. All four canines presented with localized insufficient zones of attached gingiva and 1 mm of recession. The diagnosis was AAP type II (mild periodontitis).
Risk: Low
Prognosis: Good
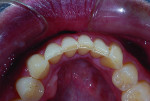
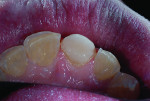
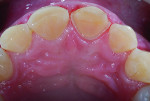
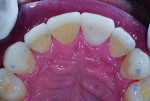
Biomechanical: The patient presented with moderate to severe attrition, erosion, and chipping on the lingual of the maxillary anteriors and bicuspids and on the facial incisal of the mandibular anterior teeth. Areas of erosion on teeth Nos. 23 through 26 revealed cupping, which indicated that the chemical component was outpacing the frictional damage (Figure 2). No carious lesions, defective restorations, or pulpal pathology were present.
Risk: Moderate
Prognosis: Poor
Functional: The patient exhibited a dental Class I malocclusion with a 20% overbite and a 2.5-mm overjet. The first bicuspids were missing and the third molars were present. Group function with balancing interferences on No. 1 with 32 and No. 16 with 17 was noted. There was no tenderness upon palpation of the musculature. Joint noise and late clicking of both the right and left joint were present, and the joints were not painful when loaded. Both clinical findings and the dental history provided evidence of parafunctional activity.
Further diagnostic evaluation with a Kois deprogrammer confirmed the functional occlusal diagnosis. The purpose of a functional analysis is to correlate clinical findings with the mechanics of occlusion and to determine the feasibility of occlusal correction. Mounted casts in centric relation revealed centric occlusion (the first point of tooth contact in centric relation) was located anterior to the canines (teeth Nos. 9, 10, 23, and 24). This analysis confirmed that the chewing envelope constriction was caused by the tooth position of the anterior teeth. During his chewing cycle, the patient’s lower incisors had to push through the upper anterior teeth to gain posterior contact. This condition can cause all or some of the following clinical findings: worn enamel, avoidance patterns during jaw movements, breathing problems, airway concerns, and jaw muscle soreness.
Diagnosis was both parafunction and constricted chewing pattern.
Risk: High
Prognosis: Poor
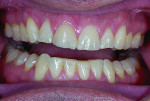
Dentofacial: On a full smile, the patient exhibited low lip dynamics with minimal tooth exposure, poor lip support, and a lack of fullness in the buccal corridors.
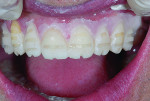
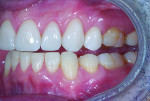
The incisors were yellow, retruded, and retroclined, and they exhibited mild mandibular anterior crowding. The posterior dentition was lingually inclined with an uneven mandibular occlusal plane. The gingival architecture was symmetrical, and the canines presented with recession (Figure 3). The dental midline corresponded with the facial midline.
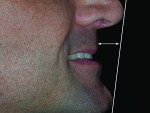
The patient exhibited a deep bite skeletal pattern (lower anterior face height of 38 degrees), with a brachifacial growth pattern (horizontal facial axis of 94 degrees and a flat mandibular plane angle of 16 degrees). Although the patient presented with a Class I dental pattern, he exhibited a tendency towards a Class III skeletal pattern due to maxillary retrognathia (Frankfurt of 86 degrees) (Figure 4).
Risk: Low
Prognosis: Fair
Treatment Goals
The patient’s esthetic desires could not be achieved unless the functional problems were also treated, because the anterior teeth could not be restored in their current position without excessive removal of tooth structure. The anterior teeth needed to be moved out of the path of the chewing cycle. This could be accomplished by orthodontically intruding and proclining the maxillary anterior teeth while intruding and lingually inclining the mandibular incisal edges. A non-orthodontic option would be to increase the vertical dimension of occlusion with restorative dentistry on at least one full arch of the patient’s dentition (in this case, the upper arch). The patient accepted the orthodontic solution; thus, the final treatment goals were to:
• Restore function and esthetics at a minimal biologic cost.
• Use centric relation joint position as the orthopedic position of the mandible, then orthodontically relocate the teeth to free up the constriction of the envelope of function to eliminate premature loading of the anterior teeth.
• Create room for restorative materials to allow placement of minimally invasive restorations.
• Prevent damage from the parafunctional activity by fabricating a nightguard for nightly wear and closely monitor function and wear patterns at recall.
Treatment Plan
The patient rejected a periodontal referral for evaluation of the cuspids, which displayed areas with minimal attached gingiva. The patient accepted the treatment plan of an orthodontic correction of the anterior constriction, followed by placement of eight maxillary veneers on Teeth Nos. 4 through 13 and composite augmentation on the mandibular incisors and canines. Essex retainers would be worn indefinitely, and a maxillary stabilization splint would be fabricated.
Treatment Phases
Phase 1: Orthodontics
Full multi-bracketed lingual Incognito™ Braces (3M™ Unitek, https://solutions.3M.com) were placed and worn for a treatment time of 5 months. Prior to debanding, the general dentist assessed the tooth position and determined that the restorative space requirements had not yet been fulfilled (Figure 5). Additional intrusion and retroclining of teeth Nos. 23 through 26 was completed, and 2 months later, an assessment revealed that the correct tooth position with adequate occlusal space had been achieved. After debanding, Essex retainers were fabricated. The patient was ready to proceed with restorative treatment 14 months after debanding.
Phase II: First Restorative Appointment
Complete records were taken at the first restorative appointment, and a diagnostic wax-up was fabricated along with incisal, facial, and provisional siltech stints (Flexitime® putty, Heraeus Kulzer, www.heraeus-kulzer-us.com). The patient wanted lighter teeth and desired a quick and significant result; therefore, power bleaching (Philips Zoom!, Philips Oral Healthcare, www.philipsoralhealthcare.com) was performed on the mandibular teeth.2 No bonding was done for 14 days after the bleaching to minimize the risk of a decreased bond strength due to the bleaching product.3
Phase III: Restorative
The patient returned for direct composite placement on the incisal edges of teeth Nos. 22 through 27 as well as the preparation of teeth Nos. 4 through 13 for porcelain veneers. Shade selection for teeth Nos. 22 through 27 was accomplished by evaluating the opacity and shade of the remaining tooth structure at the mandibular incisal edge. Shade A1B (Filtek™ Supreme Ultra, 3M ESPE, www.3MESPE.com) was chosen, and a small increment was placed on the missing portion of each tooth as a test sample, which was then light-cured to verify that this shade would provide a seamless, undetectable transition from tooth to restoration. The incisal edges of teeth Nos. 22 through 27 were lightly abraded with a fine diamond (Brasseler 850.31.016, Brassler USA, www.brasselerusa.com) to remove the aprismatic enamel and then microetched (MicroEtcher IIA, Danville Materials, www.danvillematerials.com).4 The particles used in the etcher were 27-micron white aluminum oxide. The total-etch technique was used: 37% phosphoric etch was placed first on the enamel circumference, then on the dentin, followed by agitation with a microbrush. Rinsing occurred 15 seconds later, followed by light air-drying, with the intention of leaving a moist dentin surface. A single-bottle light-cured adhesive (Adper™ Single Bond Plus, 3M ESPE) was applied and agitated for 20 seconds, air-dried for 5 seconds, and light-cured for 10 seconds. A gold waxing instrument (Titanium 8A Instrument, Cosmedent, www.cosmedent.com) was used to sculpt the composite. Verification of proper shape and form from a frontal perspective was accomplished, and when the 3-dimensional (3-D) form was morphologically correct, the resin was cured.
Local anesthesia was administered on the maxillary arch. The provisional matrix was loaded with bis-acrylic composite (Venus® Temp C&B, Shade B1, Heraeus Kulzer) and seated on the maxillary arch. This provided a preparation guide to ensure appropriate but minimal reduction. The resulting composite prototypes were then used for patient approval of the final tooth contours before any tooth structure was removed.5-8 After the patient previewed and approved the esthetics of the prototype, the color and the opacity of the material was evaluated for shade matching to the opposing dentition. It is at this time that the brand of composite to be used in the final prototypes be selected. The composite used for the final prototypes must exhibit the appropriate translucency to mask the stump of the prepared tooth and blend with the surrounding dentition; brands vary considerably in their opacity.
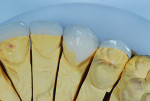
Depth cuts were made with 0.7-mm depth diamonds (Brasseler 828.31.030, Brassler USA) across the upper middle third and lower middle third to establish the amount of facial reduction. Next, 2 mm was removed from the previously approved incisal edge length (Figure 6). A lingual chamfer design was chosen to enhance the resistance form of the preparation, as well as to provide increased enamel surface for increased bond strength. This was necessary in this case due to the amount and anatomy of the wear present on the edges9 (Figure 7 and Figure 8).
Records consisting of a facebow (Kois Dento-Facial Analyzer System, Panadent, www.panadent.com), maximum intercuspal position (MIP) bites, polyvinyl siloxane (PVS) impressions, provisional models, and photo documentation were taken and sent to the lab. Provisionals were fabricated using the provisional matrix, which was loaded with a more opaque bis-acrylic composite (Protemp™ Plus B1, 3M ESPE) due to the darker hue of the preparation stumps. The temporaries were luted with a combination of spot-etching and bonding with veneer cement (RelyX™ Veneer, 3M ESPE) in the center of the preparation and TempBond® Clear (Kerr Dental, www.kerrdental.com) at the periphery.
One week later, the patient returned for an evaluation of the shape, form, color, and function of the provisionals. Looseness was noted on both cuspids. This finding was significant in planning for the final functional contours, overjet, and steepness of the guidance. In order to achieve high-strength esthetic restorations, IPS e.max® Press (Ivoclar Vivadent Inc., www.ivoclarvivadent.com) was selected; since the incisal edges of the mandibular anterior teeth were created in composite, the ceramist was instructed to cover the lingual enamel past the margin of the lingual chamfer on teeth Nos. 6 and 11 (Figure 9 and Figure 10). This was possible with IPS e.max Press material because of its high flexural strength (400 MPa), even at the minimum thickness of 0.3 mm.10,11 Also at the time of placement, fine-tuning of this feather-edge can be accomplished due to the material strength.
At the delivery appointment, the porcelain restorations were placed intraorally for esthetic evaluation and approval by the patient. All eight maxillary restorations were then cemented with OptiBond® FL (Kerr Dental) and RelyX Veneer. After cement removal, an occlusal equilibration was performed in MIP until all posterior teeth displayed bilateral, simultaneous forces. The creation of precise, correct occlusion at delivery is critical to decrease the risk of any future porcelain failure or debonding.
The maxillary lingual contact points were placed in the safe zone, avoiding the margin of the ceramic and tooth interface (Figure 11). The functional occlusion was evaluated with the patient sitting up in the chair and chewing on thick (22-micron) articulating paper, which simulates the chewing envelope, activating the closing muscles. All functional adjustments were made by recontouring the composite on the mandibular dentition. To create cuspid rise, the lateral streaks were left untouched on the canines, but all other streaks present on the posterior dentition were removed. Lack of fremitus on the anterior teeth was confirmed by placing fingers on the roots of the maxillary anterior teeth while the patient closed into MIP. Shimstock was used to confirm clearance between the incisors in maximum intercuspation. All surfaces of ceramic and composite were finished and polished to a high gloss. Postoperative photos and records were taken, and a maxillary flat plane occlusal splint and Essex retainers were fabricated. On subsequent evaluation of the photos it was noted that tooth No. 22 had a deficient cuspal contour, which resulted in a shape and form that did not satisfy functional requirements because there was not clearance of the centrals when the patient shifted into left lateral guidance (Figure 12). When the patient returned for the delivery of the maxillary splint and Essex retainers, further augmentation of composite on the mandibular canine was performed, and steeper guidance was obtained (Figure 13). The patient was aware that he would need to wear the maxillary splint every night and the Essex retainers “diurnal” indefinitely to maintain the results achieved.
The recare protocol for this patient includes monitoring of temporomandibular joint function, assessment of parafunctional habits by reading the surface of the nightguard, and evaluation of occlusal markings and wear on the incisal edge of the mandibular composite and the lingual porcelain of the maxillary uppers in all functional excursions.
Conclusion
Consistent reevaluation at every step in the procedure is paramount to the longevity of the restorations and success of the case. Just because the restorations are esthetically pleasing does not guarantee they are built to last. Most of all, they must be done right (Figure 14 through Figure 16)—in keeping with functional as well as esthetic principles.
Acknowledgment
The author wishes to thank orthodontist Howard Henry and laboratory technician Brad Patrick of Patrick Dental Arts (Bend, Oregon) as well as Dr. Jean Martin for editing. The concepts in this article are based on the teachings of the Kois Center (Seattle, Washington).
About the Author
Joyce L. Bassett, DDS, FAACD
Adjunct Faculty
Senior Dental Student Esthetic Continuum
A.T. Still University
Arizona School of Dentistry
Mesa, Arizona;
Private Practice
Scottsdale, Arizona
References
1. Bassett JL. There is more to front teeth than looks alone: diagnosis and treatment planning. Compend Contin Educ Dent. 2010;31(8):604-606, 608, 610-612.
2. Lee SS, Kwon SR, Arambula M, et al. Assessment of whitening efficacy of two in-office professional bleaching regimens [abstract]. J Dent Res. 2013;92(spec iss A). Abstract 1139.
3. Haywood VB. Bleaching—the facts and the myths. Interview by Aisling O’Mahony. J Ir Dent Assoc. 2004;50(1):30-34.
4. Onisor I, Bouillaguet S, Krejci I. Influence of different surface treatments on marginal adaptation in enamel and dentin. J Adhes Dent. 2007;9(3):297-303.
5. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16.
6. Gürel G. The Science and Art of Porcelain Laminate Veneers. Hanover Park, IL: Quintessence Publishing; 2003:241-251, 261-276.
7. Gürel G. Predictable, precise, and repeatable tooth preparation for porcelain laminate veneers. Pract Proced Aesthet Dent. 2003;15(1):17-24.
8. Bassett J. A trio of techniques for assuring predictable results. Inside Dentistry. 2007;3(10):2-5.
9. Chaiyabutr Y, Phillips KM, Ma PS, Chitswe K. Comparison of load-fatigue testing of ceramic veneers with two different preparation designs. Int J Prosthodont. 2009;22(6):573-575.
10. Anusavice KJ. Standardizing failure, success, and survival decisions in clinical studies of ceramic and metal-ceramic fixed dental prostheses. Dent Mater. 2012;28(1):102-111.
11. Bühler-Zemp P, Völkel T, Fischer K. Scientific Documentation IPS e.max® Press. Schaan, Liechtenstein: Ivoclar Vivadent AG; 2011.