A Predictable Approach to Exquisite Anterior Direct Restorations—the Additive Solution
Mehrdad Razaghy, DDS
Abstract: A rapidly increasing knowledge of and value in minimally invasive dentistry has shed more light on additive bonding as an ideal solution for esthetic improvement in anterior teeth. Understanding the essentials to performing predictable composite bondings, when indicated and possible, can transform everyday treatment planning to offer enduring, functional, and visually appealing results achieved, most importantly, through additive means. By preserving natural tooth structure and seamlessly blending restorations, additive bonding represents a revolutionary approach to achieving esthetic enhancements while optimizing patient satisfaction. Improvements in the composition of new composite materials have significantly enriched the quality of end-results achievable through layered bonding in the anterior region. This article summarizes a predictable workflow for layered composite bonding as an approach to achieving enhanced esthetics.
Understanding precise selection and application of composite materials helps dentists artfully mimic the natural characteristics of teeth and seamlessly blend restorations with the surrounding dentition. This newly emerging level of finesse has unlocked unparalleled possibilities for cosmetic and restorative procedures, drastically improving patients' smiles while preserving their tooth structure. In many cases, performing layered anterior bondings can be challenging and time-consuming. However, with proper case selection and use of the correct steps, ideal and esthetic results can be predictably achieved with direct composites.
Initial Design
Today, dentists can consider anterior composite restorations as a viable long-term solution in many cases.1 Once clinicians incorporate this mindset into their daily practice, they, in turn, naturally dedicate more time to the preparation and design of such cases.
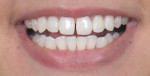
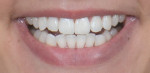
An effective approach to prepare for these additive cases is to initially comprehend and agree upon the patient's expectations by digitally designing a prototype, which helps ensure that both the patient and practitioner are "on the same page."2 Such designs can be created using high-quality photographs and basic presentation tools like Adobe® Photoshop® and Apple® Keynote®. An example of a digital design using Photoshop is shown in Figure 1 and Figure 2.
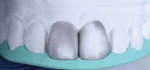
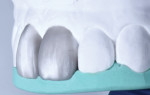
This realistic digital simulation can eventually inspire a diagnostic wax-up, which is a crucial and necessary step in the initial design phase. This wax-up provides clinicians their first understanding of the material thickness that will be needed to achieve the proposed result.3 Hence, using a different colored wax than the model is suggested for additive cases (Figure 3 and Figure 4). It is also important to plan to complete any type of bleaching, resin infiltration, or esthetic crown lengthening procedure prior to direct anterior bonding.4 The initial design phase often serves as an opportunity to identify the need for such procedures.
Shade Selection
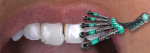
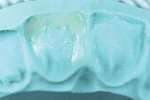
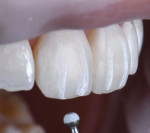
Shade selection should be one of the initial steps during the bonding appointment, as tooth rehydration can significantly affect the choice of composite shades.5 Once the target shade is chosen, a combination of different shades should be selected for what is referred to as a "wet mock-up." The wet mock-up involves quickly stacking the chosen layers using prefabricated putties based on the wax-up, with the intended thickness in mind.6 One might think of this as a fast composite restoration with no isolation. This step should be performed without etching or the use of any bonding agent (Figure 5). It has been suggested that the wet mock-up be allowed to stay in the mouth for full hydration to take place. A complementary step clinicians can take to confirm their choices of layers is to take a cross-polarized photograph with the mock-up on the tooth. Handheld polarized flashlights can also be helpful when evaluating the selection of shades.7 Such mock-ups are encouraged to be repeated until the desired shade is achieved.
Material selection is extremely important when direct composite is used in the anterior region. Resin composite systems for anterior restorations should have a wide range of shade selection options to achieve precise color matching with the patient's natural teeth. The author uses G-ænial™ A'CHORD (GC America, gc.dental/america), which is an ideal composite for anterior cases because of its simplified unishade system that enables the attainment of up to 16 classic VITA shades (VITA, vitanorthamerica.com) effortlessly with only five core shades.8
Composite resins should exhibit excellent handling characteristics to facilitate easy manipulation and sculpting to achieve the desired shape and contour of the restoration. Often, meticulously reshaping the composite into smaller, round increments, while wearing clean and uncontaminated gloves, or using instruments in conjunction with modeling resin can markedly enhance both the material's viscosity and ease of handling.9
The composite resin should be capable of being highly polished to achieve a smooth and glossy surface, enhancing the overall esthetic result.10 Also, good stain resistance helps maintain the restoration's appearance and prevent discoloration over time.11
Because anterior teeth are exposed to multiple forces during biting and chewing, composite resins used in anterior restorations need to possess adequate wear resistance to withstand such challenges. The G-ænial A'CHORD composite system achieves an ideal balance between fillers and complementary components, retaining excellent polishability given its composition.12
Finally, adequate radiopacity is essential for proper detection of the composite restoration on dental radiographs.13
Isolation and Bonding Protocol
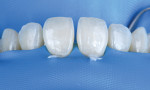
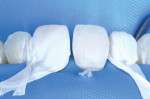
Proper rubber dam isolation in direct anterior composite cases goes beyond avoiding saliva contamination. Isolation, of course, makes a significant difference in the quality of bonding.14,15 However, specifically in anterior direct bondings, it provides access to subgingival areas, which is extremely useful for achieving a smooth transition from the most facial enamel layer to the tooth structure (Figure 6 and Figure 7). This access is gained by using floss ligation techniques on top of the rubber dam on the teeth being treated. Floss ligation allows up to 1 mm of access more gingival than where the rubber dam would normally stay. This becomes particularly valuable in cases involving diastema closure or treatment of black triangles with direct composite.16
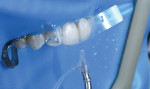
In the bonding protocol, an essential step that is often missed is cleaning the tooth structure before performing the bonding steps. When evaluating bonding areas under high magnification, film and plaque that is not completely removed during etching may be visible.17 This becomes more of a concern if self-etch primer systems are used without selective etching. To eliminate this obstacle, the author always begins the anterior bonding process by simple air-abrasion using 27-micron aluminum oxide. This is shown in Figure 8 and Figure 9, where an air-abrasion unit (AquaCare, Velopex, velopex.com) was used to perform the cleaning step. Doing this provides additional microscopic micromechanical retention and improves bonding strength by cleaning and creating a rough surface. Using rubber dam isolation significantly simplifies this process, as it prevents excessive bleeding that may occur due to tissue damage during this step.18
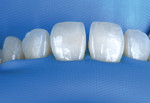
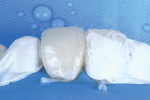
In the clinical case being presented, the clinician chose to close the diastema and improve the shape of both central incisors by bonding them one at a time. Lingual matrix systems serve as optimal guides during these procedures.19 In this case, the primary focus was on completing the facial and interproximal shape of tooth No. 8 initially. After polishing the contact point, the clinician proceeded to add composite to bring tooth No. 9 into contact. This approach enabled the final facial shape of tooth No. 8 to be used as a reference to achieve similar line angles for tooth No. 9 (Figure 10 through Figure 12).
It is crucial to note that colors and translucencies may be misrepresented under rubber dam isolation due to dehydration. This dehydration, resulting from the rubber dam isolation, plays a significant role. It is probable that if the composite restorations appear to match perfectly during the procedure, the final result after rehydration may not achieve the ideal color.20
Finishing and Polishing
A key aspect of dental treatments involving anterior teeth is their shape. The shape of teeth, especially anterior ones, holds considerable influence on how they are perceived. If the tooth's shape is correctly formed, adhering to characteristics that mimic natural tooth structure, discrepancies in shade become more forgiving.21 While the matrices, created based on the diagnostic wax-up, offer essential guidance in completing anterior restorations, having a profound knowledge of shape helps steer the final finishing steps-the most critical aspect.
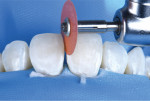
Chairside dental photography is necessary during these finishing steps, as different flash set-ups provide various representations of the teeth. With the right dental photography set-up, clinicians can better assess the shape of their restorations.22 The finishing protocol involves a back-and-forth cycle of photographs and the use of a combination of fine diamond burs, finishing and polishing discs, and composite polishers to improve the shape of the restorations. What is used to shape and polish is not so critical; any tools that allow the clinician to reshape restorations toward the desired final result should be utilized. The keys are having a system to evaluate shape and understanding what needs to be changed to resemble as close as possible the diagnostic wax-up.
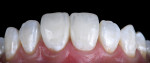
It should be noted that the final finishing and polishing do not have to occur during the same appointment. Practitioners may achieve better results by finishing the final shape and performing the final polish at another appointment when they can take a fresh look at the case (Figure 13 and Figure 14). For this reason, it is highly recommended to present anterior bonding treatment to patients as a two-part treatment.
Discussion
Maximizing the longevity of direct anterior composites extends beyond merely following the steps outlined in this article. Several crucial factors should be taken into account when selecting cases for anterior composite restorations. Initiation of case selection should involve a meticulous evaluation of the patient's bite. In direct anterior cases, particularly when teeth are lengthened, there is risk of incisal fractures if optimal guidances are not established.
Patient education plays a pivotal role in the success of such restorations. Thorough explanations should be provided to the patient regarding post-treatment considerations associated with direct restorations. The need for maintenance and re-polishing should be discussed. Additionally, patients should be informed about the importance of asking their hygienist to avoid using abrasive polishing paste during cleaning sessions. Finally, individuals with a history of grinding and clenching should consider using nightguards after receiving their restorations.
All the effort invested in anterior direct restorations, from both the patient and operator perspectives, culminates in the value that additive density provides. The impetus behind putting in this effort in daily practice should stem primarily from the clinician's profound appreciation for nature, which is simply irreplaceable.
Acknowledgment
The author thanks Sam Alawie, MDT, and his team at Beverly Hills Dental Laboratory; his hard-working dental assistants and entire staff at Mehrdad Razaghy, DDS Inc.; his mentor, Pascal Magne, DMD, MSc, PhD; Michel Magen, MDT, and Abdi Sameni, DDS, who inspire him every day; and his loving wife, Sara Mokhtari.
Disclosure
This article was commercially supported by GC America.
About the Author
Mehrdad Razaghy, DDS
Private Practice, Beverly Hills, California
REFERENCES
1. Dietschi D, Shahidi C, Krejci I. Clinical performance of direct anterior composite restorations: a systematic literature review and critical appraisal. Int J Esthet Dent. 2019;14(3):252-270.
2. Coachman C, Calamita MA, Sesma N. Dynamic documentation of the smile and the 2D/3D digital smile design process. Int J Periodontics Restorative Dent. 2017;37(2):183-193.
3. Magne P, Belser UC. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J Esthet Restor Dent. 2004;16(1):7-16.
4. Ng F, Manton DJ. Aesthetic management of severely fluorosed incisors in an adolescent female. Aust Dent J. 2007;52(3):243-248.
5. Ahmed YT, Almutairi FA, Alomran SA, et al. Dehydration time effect on tooth color measurement: an in vitro study. Eur J Dent. 2022;16(4):895-900.
6. de Araujo Júnior EM, Baratieri LN, Monteiro Júnior S, et al. Direct adhesive restoration of anterior teeth: Part 3. Procedural considerations. Pract Proced Aesthet Dent. 2003;15(6):433-437.
7. Kelkar KC, Dogra ES, Bhat V, Hegde C. OSC36: A comparison between conventional V/S digital photography V/S polarizing filter photography for shade selection. J Indian Prosthodont Soc. 2018;18(suppl 1):S23.
8. Huang W, Ren L, Cheng Y, et al. Evaluation of the color stability, water sorption, and solubility of current resin composites. Materials (Basel). 2022;15(19):6710.
9. Takamizawa T, Ishii R, Tamura T, et al. Handling properties and surface characteristics of universal resin composites. Dent Mater. 2021;37(9):1390-1401.
10. Molina GF, Cabral RJ, Mazzola I, Burrow M. Surface gloss, gloss retention, and color stability of 2 nano-filled universal resin composites. Restor Dent Endod. 2022;47(4):e43.
11. Ersöz B, Karaoğlanoğlu S, Oktay EA, Aydin N. Resistance of single-shade composites to discoloration. Oper Dent. 2022;47(6):686-692.
12. Gurgan S, Koc Vural U, Miletic I. Comparison of mechanical and optical properties of a newly marketed universal composite resin with contemporary universal composite resins: an in vitro study. Microsc Res Tech. 2022;85(3):1171-1179.
13. Dukic W, Delija B, Derossi D, Dadic I. Radiopacity of composite dental materials using a digital X-ray system. Dent Mater J. 2012;31(1):47-53.
14. Wang Y, Li C, Yuan H, et al. Rubber dam isolation for restorative treatment in dental patients [update in Cochrane Database Syst Rev. 2021;5:CD009858]. Cochrane Database Syst Rev. 2016;9(9):CD009858.
15. Zou H, Wang Y, Zhang H, et al. An overview on rubber dam application in dental treatments [in Chinese]. Zhonghua Kou Qiang Yi Xue Za Zhi. 2016;51(2):119-123.
16. Alkhatib OA, Bissasu S, Daud A. Dental floss ties for rubber dam isolation: a proposed classification and a new technique. J Prosthodont. 2023;32(1):83-89.
17. Huang CT, Kim J, Arce C, Lawson NC. Intraoral air abrasion: a review of devices, materials, evidence, and clinical applications in restorative dentistry. Compend Contin Educ Dent. 2019;40(8):508-513.
18. Olsen ME, Bishara SE, Damon P, Jakobsen JR. Comparison of shear bond strength and surface structure between conventional acid etching and air-abrasion of human enamel. Am J Orthod Dentofacial Orthop. 1997;112(5):502-506.
19. Koczarski M. Smile makeover utilizing direct composite resin veneers. Dent Today. 2008;27(12):76,78-9.
20. Notarantonio AE, McClintock D. The effect of isolation and dehydration on shade matching. Compend Contin Educ Dent. 2022;43(5):e9-eE12.
21. Bazos P, Magne P. Bio-emulation: biomimetically emulating nature utilizing a histo-anatomic approach; structural analysis. Eur J Esthet Dent. 2011;6(1):8-19.
22. McLaren EA, Terry DA. Photography in dentistry. J Calif Dent Assoc. 2001;29(10):735-742.