Hypoglossal Nerve Stimulation Therapy for Obstructive Sleep Apnea
Thomas M. Kaffenberger, MD; and Ryan J. Soose, MD
Abstract: Obstructive sleep apnea (OSA) is characterized by repetitive episodes of disrupted breathing during sleep. The most effective treatment for OSA is positive pressure ventilation; however, this treatment can be complicated by adherence difficulties. An array of alternative OSA therapies have emerged, including positional therapy, nasal exhalation devices, oral appliances, and various nasal, pharyngeal, and skeletal surgical treatments. One of the newest options, hypoglossal nerve stimulation (HNS) therapy, represents a hybrid medical and surgical treatment. This therapy involves an FDA-approved surgically implanted neuromodulation system that is activated by the patient each night to augment upper airway dilator muscle activity and improve airflow. The implanted components comprise a pulse generator, an electrode on the distal portion of the hypoglossal nerve, and a respiratory sensing lead that allows for synchronization of electrical impulses with the patient's respiratory cycle. Using a representative patient case, the authors describe HNS therapy, including its indications, patient selection, surgical procedure, long-term outpatient management, and outcomes data.
Obstructive sleep apnea (OSA) is a common condition with a global prevalence estimate approaching 1 billion people and which has substantial implications on public healthcare costs with regard to safety, quality of life, and neurocognitive and cardiovascular health.1 OSA is characterized by transient collapses of the upper airway resulting in reduced airflow and chronic intermittent hypoxia. Severity of the disease can be stratified based on the number of these respiratory events per hour, also called the apnea-hypopnea index (AHI). First-line therapy for moderate to severe OSA is the use of continuous positive airway pressure (CPAP), which creates a pneumatic splint preventing airway collapse and allowing for unimpeded respiration. Despite advances in comfort and refinement in CPAP machines over the past 40 years, patient adherence to this therapy remains a challenge with only 30% to 60% of patients tolerating CPAP.2
For CPAP-intolerant patients, an array of alternative treatments are available. One of the most common alternatives is the use of a custom oral appliance, which is a low-morbidity and effective therapy.3,4 These oral appliances improve airway patency by advancing the mandible and its soft-tissue attachments, thereby providing multilevel opening of the airway. Although an effective treatment for a large portion of the OSA population, oral appliance therapy also has limitations. For patients with limited dentition, appliance therapy discomfort, inadequate adherence, occlusal changes,5 and/or inadequate OSA control, additional alternatives often need to be considered.
Multiple airway reconstructive surgical procedures have been introduced and refined over the past four decades to treat OSA; these range from nasal and pharyngeal procedures to skeletal reconstruction and tracheostomy.6-9 Patient acceptance and implementation of upper airway surgical procedures, however, are limited by the available literature, variability in technique and outcomes, potential perioperative morbidity, and long-term side effects, such as velopharyngeal insufficiency, globus sensation, scar tissue, dysphagia, and need for future surgery, among others.10,11
Particularly for patients in whom traditional first-line treatments have failed, hypoglossal nerve stimulation (HNS) therapy has at least in part filled an unmet need. In recent years, HNS has become a widely accepted and available treatment for CPAP-intolerant patients. The therapy has demonstrated sustained treatment efficacy in both multicenter clinical trials and long-term post-market studies.12-15 Representing the first hybrid surgical procedure and adjustable medical device, the current HNS therapy is the culmination of decades of basic science research and clinical trials investigating electrical stimulation of the hypoglossal nerve as a method of improving upper airway patency and stability during sleep.16,17 With the publication of the Stimulation Therapy for Apnea Reduction (STAR) trial in 2014,13 neurostimulation therapy gained US Food and Drug Administration (FDA) approval using this medical device (Inspire®, Inspire Medical Systems, Inc., inspiresleep.com). As of early 2022, the company reported that more than 20,000 patients had been implanted,18 with this number currently estimated to be 40,000, and the device is now also approved for use in Europe and Asia.
FDA-recommended inclusion criteria, or eligibility guidelines, for HNS therapy include the following19: The patient is at least 22 years old, has moderate to severe OSA (AHI of 15 to 65 events per hour), has central or mixed apneas comprising less than 25% of the total AHI, has a body mass index (BMI) of ≤35 kg/m2, is unable to tolerate CPAP therapy, and has a sleep endoscopy demonstrating an absence of complete concentric collapse (CCC) at the soft palate.
The following case example describes the use of HNS therapy. The case encompasses the patient presentation, work-up, indications for therapy, surgical procedure, and clinical follow-up.
Case Report
The authors' patient was a 71-year-old woman who presented to the otolaryngology clinic for OSA treatment options, specifically CPAP alternatives. She had a several-year history of snoring and gasping at night, witnessed by her bed partner, along with daytime sleepiness and unrestful sleep. An in-laboratory sleep study revealed severe OSA with an AHI of 35 events per hour and associated hypoxemia and sleep fragmentation. The study report demonstrated a rapid eye movement (REM) stage AHI of 71 events per hour, a supine AHI of 58 events per hour, and a central apnea index of 0.2 events per hour. She had tried CPAP but could not tolerate therapy due to mask discomfort and removing the device unconsciously during sleep. She also had tried using an oral appliance but developed jaw discomfort and discontinued therapy.
The patient had a history of hypertension and depression, both of which were controlled. Upon examination, she had a BMI of 27 kg/m2 and her oral cavity had intact dentition with a Friedman tongue position III and no palatine tonsils. The authors discussed alternative strategies to manage her severe OSA, including revisiting CPAP, performing upper airway reconstructive surgery, and undergoing HNS therapy.
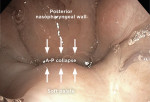
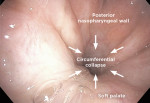
For HNS therapy, patients who meet the aforementioned clinical and polysomnographic screening criteria must then undergo a drug-induced sleep endoscopy (DISE) to evaluate their anatomic candidacy. DISE is a brief outpatient procedure using intravenous sedation to establish pharyngeal collapse conditions that mimic sleep-disordered breathing. Once in the steady state of sleep-disordered breathing, a small endoscope is passed into the nose and pharynx to examine the upper airway structure and patterns of collapse. Early HNS feasibility studies demonstrated poor response to therapy in patients who had a CCC pattern at the velum or soft palate instead of an anterior-posterior (A-P) collapse pattern (Figure 1 and Figure 2).20 In the present case, the patient underwent DISE and had complete A-P collapse at the velum (Figure 1), making her a candidate for HNS therapy. After discussing the potential risks, benefits, and limitations of the various treatment options, she elected to proceed with HNS implantation.
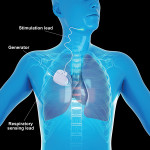
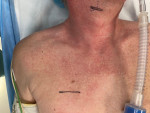
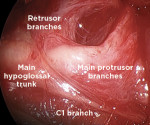
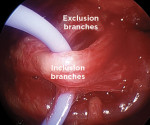
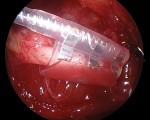
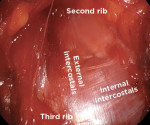
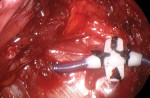
The currently available HNS system (Inspire Medical Systems, Inc.) is implanted under a general anesthetic with two incisions: one on the neck and one on the chest. There are three components to the device: an electrode cuff that is placed on the hypoglossal nerve, a respiratory sensing lead that is placed in the intercostal space, and an implantable pulse generator (IPG), which is placed in a subcutaneous pocket overlying the pectoralis major muscle (Figure 3).19 The neck incision sits in the submandibular triangle, which allows for exposure of the distal branches of the hypoglossal nerve (Figure 4 and Figure 5). Dissecting out the distal branches of the hypoglossal nerve allows for cuff placement on only the nerve branches that selectively innervate the protruding muscles of the tongue (genioglossus and geniohyoid) while excluding the retractor muscles (styloglossus and hyoglossus) (Figure 6 and Figure 7). The electrode is connected to the IPG by tunneling the stimulation lead into the chest. The respiratory sensing lead is placed between the external and internal intercostal muscles of the second intercostal space (Figure 8 and Figure 9).21 The respiratory sensor allows the IPG to synchronize stimulation with inspiration when the upper airway is susceptible to collapse.
After the HNS implantation, the patient was discharged home the same day of surgery with a normal diet and no prescription pain medications-a post-treatment protocol that differs substantially from the typical postoperative recovery after traditional pharyngeal or skeletal surgery. The device was activated in the office setting 4 weeks after surgery, according to the standard protocol, which allows the patient time to heal from surgery and the electrode to make appropriate contact with the hypoglossal nerve. At the activation visit, a device check confirmed comfortable uninhibited anterior tongue motion, an adequate respiratory sensing waveform, and appropriate system function. The patient received therapy education and a remote-control unit that turns therapy on/off and can be used to adjust the stimulation as needed to optimize comfort and symptom response (analogous to oral appliance adjustments). The remote-control unit can also be used to pause therapy if desired.
After an initial 3-month accommodation period, the patient returned to the clinic to assess therapy comfort/usage, symptom response, and objective adherence data, which is monitored similar to CPAP data downloads. At this time, she had resolution of her sleep symptoms and excellent adherence without significant discomfort. A sleep study was ordered at this visit to assess control of objective metrics of OSA. The post-treatment sleep study may consist of a titration study completed in a sleep laboratory or a home portable study depending on the clinical circumstances. In the authors' experience, titration sleep studies overestimate the effect of HNS because patients may not be able to tolerate the therapeutic level that is identified in the sleep laboratory. Regardless of whether a titration study is included, the authors recommend a multi-night home portable study at the current settings to better assess efficacy in the patient's sleep environment.
For long-term therapy management, HNS data download software (Inspire SleepSync™) provides an objective patient adherence report, which details the percentage of nights used, percentage of nights used 4 hours or more, number of hours per night used, average number of therapy pauses per night, and nightly therapy on/off times. The patient in the present case reported symptomatic improvement in measures of sleep quality and daytime sleepiness as measured by the Epworth Sleepiness Scale (12 preoperatively to 4 postoperatively). The post-treatment home study was completed 5 months postoperatively and demonstrated an AHI of 7.2 events per hour. Nightly adherence was 8.5 hours per night.
Discussion
Electrical neurostimulation of the upper airway is a novel therapy for OSA that augments the patient's own neuromuscular physiology to improve upper airway patency and airflow. Five-year outcomes study of the initial STAR trial demonstrated significant improvements in patient-reported and polysomnographic metrics of sleep apnea, with minimal serious adverse events.12,14 A large HNS registry with 1,017 patients assessed at 12 months postoperatively noted a median usage of 5.7 hours per night and a significant drop in median AHI from 32.8 to 9.5 events per hour.14 A survey of these registry patients on the HNS registry showed that 95% preferred HNS over CPAP and 93% reported overall satisfaction with HNS treatment.
The implantation procedure is commonly well-tolerated with limited downtime and minimal to no opioid requirement. Procedure-related risks include mild incision discomfort and temporary nerve weakness. Serious surgical complications, such as hematoma, pneumothorax, device infection, and IPG migration, have been reported but are rare. The most common therapy-related adverse event was discomfort due to the electrical stimulation, often modifiable with office-based programming adjustments.12-14
Despite favorable efficacy and usage and relatively low levels of perioperative risk, both patients and practitioners should be cognizant of several device-related factors. For one, the current device (Inspire Medical Systems, Inc.) has a battery life of 10 to 12 years,19 and an additional surgery is required to replace the battery. Battery replacement may need to occur earlier in the case of device malfunction or iatrogenic injury, such as during cardioversion.22 Some patients may have cosmetic concerns related to the external incisions and/or the potential for the hardware components to be visible or palpable through the skin. Another important consideration for these devices is magnetic resonance imaging (MRI) compatibility. Inspire devices implanted in 2018 or later are approved by the FDA for full-body MRIs in ≤1.5 Tesla magnets.23 Patients with devices implanted before 2018 should consult their surgeon and the company prior to undergoing an MRI. Lastly, patient counseling is imperative to set expectations. HNS therapy requires long-term compliance similar to CPAP and oral appliances, and patients need to be aware that therapy success demands regular nightly use and long-term monitoring. The authors recommend that once a patient's treatment is optimized, they return yearly for a check of the system and to monitor adherence and effectiveness.
Conclusion
In appropriately selected moderate to severe OSA patients who have failed CPAP and other conservative measures, hypoglossal nerve stimulation therapy can provide an effective and safe treatment alternative. Current and future research directions include cardiovascular outcomes studies, clinical trials in Down syndrome and other special patient populations, new technology development, and improving patient selection and outcomes by studying the demographic, clinical, and physiologic predictors of therapy response.
Disclosure
Dr. Soose is a consultant for Cryosa, Inc., Inspire Medical Systems, Inc., and XII Medical, Inc. and also receives research support from Inspire Medical Systems, Inc. Dr. Kaffenberger had no disclosures to report.
About the Authors
Thomas M. Kaffenberger, MD
Sleep Medicine and Sleep Surgery Fellow Physician, Department of Otolaryngology, Thomas Jefferson University, Philadelphia, Pennsylvania
Ryan J. Soose, MD
Director, Sleep Division, Associate Professor, Department of Otolaryngology, University of Pittsburgh, Pittsburgh, Pennsylvania
References
1. Benjafield AV, Ayas NT, Eastwood PR, et al. Estimation of the global prevalence and burden of obstructive sleep apnoea: a literature-based analysis. Lancet Respir Med. 2019;7(8):687-698.
2. Rotenberg BW, Murariu D, Pang KP. Trends in CPAP adherence over twenty years of data collection: a flattened curve. J Otolaryngol Head Neck Surg. 2016;45(1):43.
3. Phillips CL, Grunstein RR, Darendeliler MA, et al. Health outcomes of continuous positive airway pressure versus oral appliance treatment for obstructive sleep apnea: a randomized controlled trial. Am J Respir Crit Care Med. 2013;187(8):879-887.
4. Doff MHJ, Hoekema A, Wijkstra PJ, et al. Oral appliance versus continuous positive airway pressure in obstructive sleep apnea syndrome: a 2-year follow-up. Sleep. 2013;36(9):1289-1296.
5. Pliska BT, Nam H, Chen H, et al. Obstructive sleep apnea and mandibular advancement splints: occlusal effects and progression of changes associated with a decade of treatment. J Clin Sleep Med. 2014;10(12):1285-1291.
6. Awad M, Capasso R. Skeletal surgery for obstructive sleep apnea. Otolaryngol Clin North Am. 2020;53(3):459-468.
7. Puccia R, Woodson BT. Palatopharyngoplasty and palatal anatomy and phenotypes for treatment of sleep apnea in the twenty-first century. Otolaryngol Clin North Am. 2020;53(3):421-429.
8. Shah RR, Thaler ER. Base of tongue surgery for obstructive sleep apnea in the era of neurostimulation. Otolaryngol Clin North Am. 2020;53(3):431-443.
9. Camacho M, Certal V, Brietzke SE, et al. Tracheostomy as treatment for adult obstructive sleep apnea: a systematic review and meta-analysis. Laryngoscope. 2014;124(3):803-811.
10. Kent D, Stanley J, Aurora RN, et al. Referral of adults with obstructive sleep apnea for surgical consultation: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2021;17(12):2499-2505.
11. Tang JA, Salapatas AM, Bonzelaar LB, Friedman M. Long-term incidence of velopharyngeal insufficiency and other sequelae following uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg. 2017;156(4):606-610.
12. Woodson BT, Strohl KP, Soose RJ, et al. Upper airway stimulation for obstructive sleep apnea: 5-year outcomes. Otolaryngol Neck Surg. 2018;159(1):194-202.
13. Strollo PJ Jr, Soose RJ, Maurer JT, et al. Upper-airway stimulation for obstructive sleep apnea. N Engl J Med. 2014;370(2):139-149.
14. Thaler E, Schwab R, Maurer J, et al. Results of the ADHERE upper airway stimulation registry and predictors of therapy efficacy. Laryngoscope. 2020;130(5):1333-1338.
15. Hasselbacher K, Hofauer B, Maurer JT, et al. Patient-reported outcome: results of the multicenter German post-market study. Eur Arch Otorhinolaryngol. 2018;275(7):1913-1919.
16. Strohl KP, Baskin J, Lance C, et al. Origins of and implementation concepts for upper airway stimulation therapy for obstructive sleep apnea. Respir Investig. 2016;54(4):241-249.
17. Doghramji K, Boon MS, Huntley CT, Strohl KP. Upper Airway Stimulation Therapy for Obstructive Sleep Apnea. New York, NY: Oxford University Press; 2021.
18. Inspire surpasses 20,000 patient milestone for its implanted neurostimulator for sleep apnea. Sleep Review website. February 14, 2022. https://sleepreviewmag.com/sleep-treatments/therapy-devices/neurostimulators/inspire-surpasses-20000-patient-milestone/. Accessed April 24, 2023.
19. Inspire Medical Systems, Inc. Patient Manual, Inspire IV Generator Model 3028. Inspire Product Manuals. August 17, 2022. https://manuals.inspiresleep.com/content/widgets/manual.php?NTAxfDF8MQ==. Accessed April 19, 2023.
20. Vanderveken OM, Maurer JT, Hohenhorst W, et al. Evaluation of drug-induced sleep endoscopy as a patient selection tool for implanted upper airway stimulation for obstructive sleep apnea. J Clin Sleep Med. 2013;9(5):433-438.
21. Kent DT, Weiner JS, Chio EG, Weidenbecher M. Hypoglossal nerve stimulator implantation via a 2-incision technique. Oper Tech Otolaryngol-Head Neck Surg. 2020;31(3):e35-e42.
22. Vasconcellos AP, Huntley CT, Schell AE, et al. Dysfunctional hypoglossal nerve stimulator after electrical cardioversion: a case series. Laryngoscope. 2019;129(8):1949-1953.
23. Inspire Medical Systems, Inc. MRI Guidelines for Inspire Therapy, Clinician's Manual. Inspire Product Manuals. October 4, 2022. https://manuals.inspiresleep.com/content/widgets/manual.php?NTAwfDF8MQ==. Accessed April 19, 2023.