Combined Periodontal and Orthodontic Treatment With Clear Aligner Therapy: A Hybrid Model
Payam C. Ataii, DMD, MBA
Abstract: Along with a strong consumer demand for clear aligner therapy, research supports the benefits of combining it with periodontal and restorative treatments for comprehensive treatment planning. This article discusses how the new classification system of periodontal disease adopted by the periodontal community impacts case selection for dental providers who are considering clear aligner therapy and showcases case examples of combination therapy.
Periodontal disease used to be recognized as "chronic" or "aggressive," but recently these two categories became grouped as one ("periodontitis") and further characterized based on a multidimensional staging and grading system espoused by the American Academy of Periodontology and the European Federation of Periodontology.1 Adopted in 2017, the new periodontal disease classification is divided into four stages of progress: stage 1 = gingivitis; stage 2 = slight periodontal disease; stage 3 = moderate periodontal disease; stage 4 = advanced periodontal disease.1 Even minimal to moderate dental crowding or spacing can lead to unnatural tooth positions that may impact the long-term periodontal health of the patient.2 Clear aligner treatment in these mild to moderate cases may alleviate further periodontal disease.
For patients with an intra-arch malpositioned anterior segment of teeth, clear aligner therapy can have a positive effect on the overall health of the surrounding periodontium,particularly for patients diagnosed with stage 2 periodontal disease or who present with early stage 3 periodontal disease.3 The main objective in any orthodontic treatment is to gain better overall tooth alignment within the surrounding bone and arch structure. Occlusal trauma is also linked to local damage such as bone loss, gum disease, and halitosis and may lead to problems in the temporomandibular joints, facial muscles, head and neck posture, and breathing. Clear aligners are most effective in treating mild to moderate malocclusions in adults and teenage patients, emerging as one of the least aggressive orthodontic approaches for betterment of gingival health.4 During clear aligner therapy, the periodontium is not compromised, and the aligners can become a supportive attribute for periodontal health. For instance, aligners aid in attaining better tooth position within the bone, are removable to allow enhanced oral hygiene, and help improve keratinized gingival tissue.5
Clear aligner treatments are increasingly becoming part of the comprehensive treatment planning approach within general practices to help facilitate better periodontal health. Recently, with the growing demand for telehealth in the dental space, the American Dental Association has updated its teledentistry policy, which is expected to help expand the reach of dental care throughout the United States.6 Combined with the steadily improving efficacy of clear aligners, clinicians are now positioned to offer clear aligner treatment as a viable option to patients utilizing a hybrid teledentistry model for aligner therapy for mild to moderate malocclusions between 2 mm and 6 mm. For patients who present with malocclusions that are more than 6 mm, specifically in the anterior arch, traditional clear aligner methodologies may be chosen by the clinician.
Teledentistry is the ability to render consultations, care, and education to dental patients utilizing information technology and telecommunications.7 This medium has been recognized in the literature as an effective means to address low-acuity dental patients.8,9 For instance, equivalent results were found when patients were inspected for tooth decay using photographs compared to visual inspection.10 Similarly, teledentistry has been found to be an effective tool to identify new orthodontic patient referrals11 and for ongoing clear aligner treatment progress.12,13
Hybrid Model
A hybrid model involves a clear aligner treatment process that leverages teledentistry along with in-person office visits to offer a convenient way to straighten mild to moderate misalignments. Unlike the traditional aligner model, some aligner companies have introduced a novel hybrid business model by connecting with dental practices to form partner networks. Through the partnership, dentists are able to offer convenient and affordable clear aligner options to their patients with no financial overhead. Additionally, companies that have pioneered this model are able to drive consumers to the dental practice to aid in effectively growing the practice.
In this hybrid model, the simple but effective workflow is designed to reduce practice overhead, expand clear aligner options for the practice, and increase patient flow through the practice. The benefit of this model is twofold: (1) the practice has options to suit most types of patients, and (2) lifetime value is formed as consumers looking to straighten their teeth often become patients of the practice for treatments beyond clear aligners. For instance, if a consumer presents to the hybrid in-office visit but is periodontally compromised, they may be presented with a comprehensive treatment planning approach: aligners through the hybrid model plus periodontal treatment under the auspices of the partner network dentist or specialist equals long-term stabilization.
Consumers interested in receiving clear aligner therapy can connect with the aligner-prescribing doctor via the teledentistry platform or visit a participating partner network dental office to start their aligner treatment. Patient records, chief concern, and oral health evaluation, including periodontal evaluation, are then reviewed via a teledentistry platform by a state licensed dental practitioner prescribing the patient's custom tooth movements, for aligners to be manufactured and shipped to the patient. The aligner-prescribing doctor may request additional information and/or clearances if necessary, including but not limited to periodontal clearance, which the patient can provide from their current dental provider. Should the patient not have a dental provider, an option of sending the patient to a partner network dental office is provided. The aligner-treating doctor will use the information collected to evaluate if the consumer is a candidate for mild to moderate malocclusion to be treated with clear aligners utilizing remote teledentistry directed by the treating doctor. The patient then maintains virtual aligner check-ins throughout the term of the aligner treatment via teledentistry to evaluate tracking and progress of prescribed tooth movements. The patient can also have a collaborative option by having their existing dental provider follow-up for hygiene and routine dental visits as the patient continues their aligner therapy and check-ins online with the aligner-prescribing doctor via teledentistry. In essence, through teledentistry the patient is continually monitored to check aligner tracking with similar efficacy to that of a face-to-face in-office visit.
To reiterate, when necessary, periodontal aspects are managed by a specialist. Hesitancy to move teeth that might be periodontally compromised without close office supervision would be a concern if raised by said specialist. In the two cases described in this article, the specialists felt that clear aligner therapy would address the periodontal condition of the patients, which indeed occurred. Periodontal condition must be considered and factored into any long-term treatment. As stated earlier, clear aligner therapy may be utilized to address mild to moderate, not moderate to severe, periodontally compromised patients.
Clinical Case Reports
Early In-Office Approach
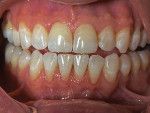
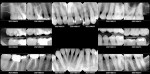
A 47-year-old female patient who experienced bone loss caused by traumatic occlusion was first seen in 2006 (Figure 1). She presented class I posterior occlusion with mandibular anterior mobility of grade 2+ from teeth Nos. 23 through 26 with accompanying generalized horizontal bone loss of greater than 50%. The patient further presented an anterior deep bite greater than 4 mm and an interproximal anterior arch spacing of more than 4 mm with noted mobility of the anterior arch. Radiographically, the patient showed moderate to severe bone loss, specifically in the mandibular anterior arch, with a soft-tissue probe of only 2 mm to 3 mm. The patient at the time was classified as a class II transitioning into class III periodontal condition. She also had been seen by several other general dental clinicians and specialists who offered her multiple treatment options ranging from periodontal tissue treatments to the removal of lower anterior teeth followed by a fixed or removable restorative option. Her chief concern was that she did not want to "lose" her teeth.
For the initial treatment plan, the patient was given clear aligners as an orthodontic option to intrude the upper anterior arch by 2 mm and intrude the lower anterior arch 2 mm within the bone. The treatment goal was to reduce the anterior deep bite and minimize the constant traumatic anterior load, which could lead to healthier bone and initiate better osteoblastic (cellular) activity.14 The treatment plan also included endodontic and restorative treatment on the posterior arch and a cosmetic option of reducing the residual interproximal open gingival embrasures in the upper and lower anterior arches. Given that clear aligner treatment can also help close all anterior interproximal spacing, the patient's profile and anterior overjet were used to dictate the amount of interproximal closure. This protocol leaves a small residual interproximal space to avoid over-lingual tipping of the anterior teeth.
After a year of clear aligner treatment and an additional 6 months of bite stabilization, the patient's mandibular tooth mobility was reduced to grade +0, and she could then eat foods without the fear of losing her teeth. Residual spacing was addressed via restorative bondings (Figure 2 through Figure 4), and final retention was completed with a fixed lower wire and an upper centric relation splint. Retainers were provided at the conclusion of aligner treatment.
Although this proposed treatment option was considered unconventional at the time, the patient was willing and eager to undergo the treatment given the poor prognosis in the near future had she not received the treatment. Continued hygiene and recall visits were scheduled. The patient's teeth were retained, and her oral condition was thriving nearly a decade after her initial aligner treatment (Figure 5 through Figure 7).
Hybrid Aligner Model
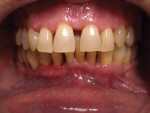
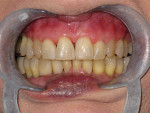
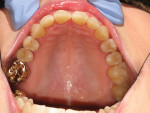
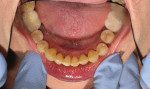
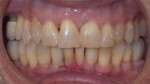
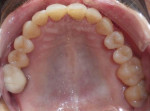
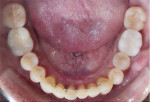
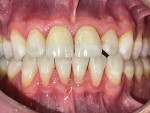
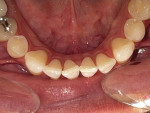
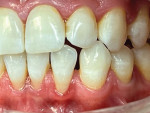
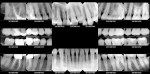
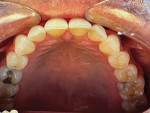
A 43-year-old male patient with good oral hygiene desired to have residual spacing closed and to stop further shifting of his teeth. The patient was a classic relapse case as a result of losing his retainers following previous orthodontic treatment. He searched online for a convenient clear aligner solution and considered SmileDirectClub (SDC) as an option. During his visit to an SDC partner office, initial photographs were taken that showed mild malocclusion and mild gingival recession in the anterior region (Figure 8). The patient complained of mandibular anterior arch rotations and interproximal spacing that was leading to continued food entrapment, specifically at the distal aspect of tooth No. 23 (Figure 9 and Figure 10). The lower anterior soft tissue presented with slight gingival dehiscence, specifically teeth Nos. 23 through 26 (Figure 10). Radiographs of the patient that had been recorded previously, which the office now had, showed stable hard-tissue condition (Figure 11). The maxillary anterior arch showed lateral incisor rotations of less than 5 degrees and limited interproximal spacing (Figure 12). The patient was periodontally classified as class II.
Left untreated, the patient's condition could lead to a poor prognosis with the possible need for soft-tissue grafting, mobility of teeth, and the potential for traumatic occlusion leading to the loss of the alveolar process. With less than 3 mm of interproximal mandibular anterior arch spacing and tooth rotations less than 15 degrees, this case was considered a mild clear aligner case with the patient being an ideal candidate for the hybrid aligner model to correct the malocclusions-specifically, the anterior malocclusions, followed by retention. During the hybrid aligner treatment process, the patient maintained his check-ups with the partner office for overall oral health and also maintained telehealth check-ins with SDC's aligner-treating doctor to ensure aligner tracking and evaluate tooth movement progress, to ensure a favorable aligner outcome.
Six months into the aligner treatmentthe patient stated he was no longer dealing with food trapped between his teeth, specifically on the lower anterior arch (Figure 13). During the teledentistry check-ins the patient also reported that he felt his teeth were shifting back to a better bite and noticed a full bite during mastication compared to the previous bite before aligner treatment.
The partner network practice placed the patient on a recall hygiene regimen as he concluded his aligner treatment via the hybrid model, as well as a final retention program. The final retention program consisted of upper and lower clear aligners to be worn for 22 hours a day for the initial 6 months, followed by a lifetime of nighttime wear through the SDC's retention program. Postoperative treatment radiographs taken at the completion of the aligner treatment (Figure 14) showed no signs of active periodontal disease or additional bone loss, as the patient continued to wear his retention aligners. Presently, the patient is considering addressing his overall gingival health as well.
Conclusion
The use of clear aligner therapy, regardless of the model (in-office or hybrid through teledentistry), can positively impact a patient's overall health and the long-term effectiveness of the dental treatment. Practices need to identify patients who may be experiencing mild to moderate malocclusion leading to a compromised periodontium while educating them on the benefits of clear aligner treatment. Combined therapies of periodontics and orthodontics with clear aligners can provide partner practices an opportunity to effectively treat a broader patient base using the hybrid approach.
Acknowledgment
The second case presented is courtesy of Kenneth Rubinstein, DMD.
Disclosure
This article was commercially supported by National Academy of Dental Professionals & Staff Members™.
About the Author
Payam C. Ataii, DMD, MBA
Clinical Instructor, Tufts University School of Dental Medicine, Boston, Massachusetts; Private Practice, Laguna Hills, California
References
1. Papapanou PN, Sanz M, Buduneli N, et al. Periodontitis: Consensus report of workgroup 2 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J Periodontol. 2018;89(suppl 1):S173-S182.
2. Staufer K., Landmesser H. Effects of crowding in the lower anterior segment-a risk evaluation depending upon the degree of crowding. J Orofac Orthop. 2004;65(1):13-25.
3. Ngom PI, Diagne F, Benoist HM, Thiam F. Intraarch and interarch relationships of the anterior teeth and periodontal conditions. Angle Orthod. 2006;76(2):236-242.
4. Borda AF, Garfinkle JS, Covell DA, et al. Outcome assessment of orthodontic clear aligner vs fixed appliance treatment in a teenage population with mild malocclusions. Angle Orthod. 2020;90(4):485-490.
5. Miethke RR, Vogt S. A comparison of the periodontal health of patients during treatment with the Invisalign system and with fixed orthodontic appliances. J Orofac Orthop. 2005;66(3):219-229.
6. ADA News. ADA updates teledentistry policy. American Dental Association website. November 5, 2020. https://www.ada.org/en/publications/ada-news/2020-archive/november/ada-updates-teledentistry-policy. Accessed September 10, 2021.
7. Jampani ND, Nutalapati R, Dontula BS, Boyapati R. Applications of teledentistry: a literature review and update. J Int Soc Prev Community Dent. 2011;1(2):37-44.
8. Namakian M, Subar P, Glassman P, et al. In-person versus "virtual" dental examination: congruence between decision-making modalities. J Calif Dent Assoc. 2012;40(7):587-595.
9. Estai M, Kanagasingam Y, Tennant M, Bunt S. A systematic review of the research evidence for the benefits of teledentistry. J Telemed Telecare. 2018;24(3):147-156.
10. Inês Meurer M, Caffery LJ, Bradford NK, Smith AC. Accuracy of dental images for the diagnosis of dental caries and enamel defects in children and adolescents: a systematic review. J Telemed Telecare. 2015;21(8):449-458.
11. Mandall NA, O'Brien KD, Brady J, et al. Teledentistry for screening new patient orthodontic referrals. Part 1: a randomised controlled trial. Br Dent J. 2005;199(10):659-662.
12. Park JH, Kim JH, Rogowski L, et al. Implementation of teledentistry for orthodontic practices. J World Fed Orthod. 2021;10(1):9-13.
13. Morris RS, Hoye LN, Elnagar MH, et al. Accuracy of dental monitoring 3D digital dental models using photograph and video mode. Am J Orthod Dentofac Orthop. 2019;156(3):420-428.
14. Fan J, Caton JG. Occlusal trauma and excessive occlusal forces: narrative review, case definitions, and diagnostic considerations. J Periodontol. 2018;89 suppl 1:S214-S222.