Laser Dentistry: Mainstream After 25 Years
Despite the notion that lasers are often considered a new technology, it was almost 25 years ago in 1987 when Dr. Terry Myers received a US Food and Drug Administration (FDA) 510(k) marketing clearance for the use of the Nd:YAG laser in the oral cavity. Soon after, dentistry was changed forever. The promotion, popularity, and successful outcomes of laser treatment in the areas of oral healthcare, particularly in ophthalmology, have made patients and clinicians alike more interested and inquisitive about the use of lasers in dentistry.
Laser use in dentistry today is becoming routine, and over the past 25 years the number of lasers on the market along with the number of indications and applications for laser use in dentistry has grown significantly. These instruments are being used not only for soft-tissue surgery procedures but also in the diagnostic process, laser-assisted root planing and scaling, preparing teeth for restoration, recontouring osseous structures, and promoting enhanced healing. The overall goal of laser therapy is efficient care with improved outcomes.
Identifying Needs
The first and most important step in incorporating laser technology into a dental practice is identifying the true needs of the practice and what benefits laser technology will bring to patient care. Just as the needs of each practice and patient are different, the science, functionality, dependability, and ergonomics of each laser are different. Dental clinicians are responsible for learning and understanding the scientific principles of every procedure they perform, as well as the laser physics of each device they might choose to utilize. The role of the laser device is to provide light energy of a specific wavelength that is absorbed in the intended target to obtain the desired outcomes. When the target is a composite resin the goal of the light energy is to either create or break down a chemical bond. When the light energy is absorbed in the biological tissue the goal is to either vaporize the target or stimulate a tissue response (such as tissue fluorescence or a healing response). Tissue is vaporized and removed when its temperature is instantaneously raised to its vaporization point, and its components become a gas and the cell expands and explodes.
Unfortunately, as the number of laser devices and applications being performed has increased, so has uncertainty over which lasers might be most appropriate for a given dental practice. Contributing to the uncertainty is the fact that the techniques for performing the same procedure may vary from device to device, especially if the lasers emit a different wavelength of light energy.
Not All Lasers the Same
A common misconception is that all laser devices and techniques are the same. This misunderstanding is often further amplified by the terminology that is typically used to describe the various types of lasers. Lasers are commonly referred to by the composition of the their active medium (eg, semiconductor/diode, Nd:YAG, erbium, CO2, etc.) that determines their wavelength.
The wavelength of the light energy emitted is one of the laser’s most important properties and determines how efficiently the light energy will interact to produce the desired response. Lasers and light-based technologies with a semiconductor active medium are often referred to as diode lasers and can have a variety of wavelengths used in dentistry, ranging from 400 to 1,064 nanometers (nm). This range of wavelengths can elicit very different responses and tissue interactions. The difference in the wavelength is determined by the composition and quality of the semiconductor.
Other dental lasers include carbon dioxide (CO2), with a wavelength of 10,600 nm; and neodymium: yttrium aluminum garnet (Nd:YAG), with a wavelength of 1,064 nm. These are designed for soft-tissue procedures. Hard-tissue lasers, often referred to as all-tissue or erbium-class lasers, have wavelengths of 2,940 nm for the erbium: yttrium aluminum garnet (Er:YAG) laser, and 2,780 nm for the erbium, chromium: yttrium, scandium, gallium, garnet (Er,Cr:YSGG) laser. All dental lasers are in the nonionizing range of the electromagnetic spectrum and do not cause any mutagenic changes to the tissue or its DNA.
One of the primary considerations in selecting a laser is matching the laser’s wavelength with the chromophores (the components that absorb the light energy) in the target. Because soft tissue in the oral cavity is approximately 70% water, water is the primary chromophore for absorption. Hemoglobin and melanin are additional chromophores that play a relatively minor role due to their substantially lower concentration within the soft tissue.
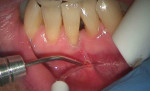
When comparing lasers and the light energy they emit, there is a significant difference in their absorption in water. Studies have demonstrated that the energy from 970-nm to 980-nm wavelengths of light energy is absorbed more than 10 times that of an 810-nm light.1,2 This enhanced absorption of the 970-nm to 980-nm lasers enables the clinician to use water convection cooling to enhance the ablation process and assist in controlling the collateral effects in remaining tissue adjacent to the treatment areas (Figure 1).
Lasers with wavelengths in the 800-nm to 940-nm range compensate for this decreased amount of absorption by initiating the fiber tip (blocking the light energy) with a substance such as articulating paper, ink, or cork, etc, to heat the tip. This hot tip is then used in a contact mode to vaporize the tissue. This method of action prohibits the use of convection cooling during the ablation process, limiting the ability to control the amount of heat dissipation into the remaining tissue.
The crystals in enamel, dentin, cementum, and bone, have significantly lower concentration of water than soft tissue. Therefore, a wavelength of light energy is required that is highly absorbed in water, which has peak absorption of light energy at approximately 3,000 nm. In addition, there is a small absorption at around 2,800 nm by carbonated hydroxyapatite mineral of the tissues, but this is far outweighed by the water effects.3 These factors make the erbium-class lasers with a wavelength of 2,780 nm for the Er,Cr:YSGG and 2,940 nm for the Er:YAG an almost ideal device for the laser vaporization of hard tissues.
In Control
Controlling the amount of time that the energy is applied will determine the amount of material that it removes and the amount of heat spread into the remaining tissue. In the pulsing mode, the amount of time between pulses is called the thermal relaxation time (TRT). The longer the TRT the longer the remaining tissue is allowed to cool, thus minimizing the thermal effects and damage to the collateral tissue.
It is extremely important that the clinician has control over the laser duty (emission) cycle, which is the percentage of time that the energy is emitted (on) versus the time off per pulse. The amount of TRT is determined by a combination of the pulse rate expressed in hertz (number of pulses per second) and the duty cycle. Being able to control the TRT gives the clinician an additional modality to assist in attaining the desired outcome for the treatment.
The power that a laser has and how it is controlled is also a key aspect in its efficiency. The peak power of a laser is the maximum amount of energy that is emitted during a single pulse. Some of today’s free-running lasers often have a peak pulse of 1,000 to 2,000 watts. The average power is the amount of energy that is emitted in 1 second and is determined by the peak power and the amount of TRT that occurs during that second. Clinicians are often confused about the different roles and value of peak versus average power. Today’s quality lasers, which are able to manage their high peak power with digital pulsing, give practitioners an even greater ability to use the desired average power to accomplish their goals.
Low-level laser therapy (LLLT), often referred to as photobiomodulation, is a focus of a significant amount of research today and is being utilized more commonly in many healthcare facilities. The goal of photobiomodulation is to promote healing and stimulate the natural reparative process of the body. Ongoing research in this area is showing much promise in improving the quality of bone for more desirable results for procedures such as implant dentistry, as well as reducing postoperative discomfort after many surgical procedures and shortening the healing time after treatment or traumatic injuries.
Keys to Integration
While the upfront cost of a laser device can be significant, another important consideration is the cost per patient along with the ongoing expenses related to maintaining the unit. Besides costs, other considerations include ergonomics, quality of the device and its accessories, and accessibility of consumables (tips, fibers, handpieces, etc). The value of reliability, reputation of the manufacturer, and access to support and maintenance are also key considerations. Before acquiring a laser, clinicians also need to investigate their state regulations and make sure that the necessary training is available through their manufacturer or dealer.
After learning the science and investigating the above-mentioned considerations when selecting and evaluating a laser, the single most valuable aspect should be device-specific training. Each device is different, with specialized programming and features that need to be thoroughly understood for safe and effective use. Device-specific training is essential, and more and more states are starting to require full-day hands-on training before the device can be registered and used in patient care. In addition to education supplied by the manufacturer, the Academy of Laser Dentistry (ALD) (www.LaserDentistry.org) is an excellent resource for additional information and education on the safe, effective, and successful implementation of lasers into practice.
References
1. Cecchetti W, Guazzieri S, Tasca A, et al. 980-nm diode laser and fiber optic resectoscope in endourological surgery. European Biomedical Optics Week, BiOS Europe, 1996.
2. Feldchtein F. Soft Tissue Surgery with Diode Laser: Direct Laser Cutting or Hot Tip? Paper presented at: ALD 18th Annual Conference and Exposition; March 3, 2011; San Diego, CA.
3. Parker SPA, Darbar AA, Featherstone JDB, et al. The Use of Laser Energy for Therapeutic Ablation of Intraoral Hard Tissues. Position Paper: Academy of Laser Dentistry, adopted March 2007. J Laser Dent. 2007;15(2):78-86.
About the Author
Scott D. Benjamin, DDS
Private Practice
Sidney, New York