Creating Proper Occlusion With OccluSense® to Achieve Sound Function
Isaac Tawil, DDS, MS; and Michael Erdos, DDS
Abstract: Proper occlusion is a foundational element of dentistry that affects various aspects of dental health, including a patient's oral function, structure, and esthetics. Among the tools dentists use to gauge a patient's occlusion are articulating paper and shimstock. A new system that combines both traditional and digital registration of the pressure distribution on occlusal surfaces can aid clinicians in further analyzing a patient's occlusion and more precisely diagnosing anomalies. In this article, three clinical cases are presented in which the OccluSense® system was used to address occlusion issues in restorative dentistry, orthodontics, and prosthodontics.
Occlusion is one of the most important clinical factors in dentistry, as it influences the functional, structural, and esthetic aspects of oral health. From a functional standpoint an improper occlusion can lead to premature tooth wear, mobility, fracture, loss, and dental treatment.1 Occlusion, however, affects more than just teeth; when a patient's occlusal system is not functioning in harmony it can impact eating, speaking, the temporomandibular joint, various muscles of the face and body, and overall quality of life.2 Therefore, it is imperative that dental professionals appreciate occlusion and are able to diagnose occlusal issues properly.
Determining Occlusion
Most dentists today use articulating paper to begin to understand a patient's occlusion. A critical characteristic of articulating paper is its thickness, which is usually measured in microns (µm). Thin articulating paper (<40 µm) is an effective tool to measure precise occlusal points of contact, as it is thin enough to avoid marking teeth that are almost, but not, in occlusion. Thick articulating paper (40 µm to 200 µm) usually captures more occlusal points of contact and, due to its thickness, can create marks that are darker and more distinct.
Besides thin or thick articulating paper, dentists often use shimstock, a super thin foil, in conjunction with articulating paper. This foil is usually around 12 µm in thickness and does not leave marks on a patient's teeth, as there is no color on the foil to transfer. Because it is very thin it is often used to check if certain opposing teeth are in contact and to check occlusal holding force. Clinicians can test this holding force by having the patient bite down on the shimstock foil and then try to remove it from the patient's mouth while the patient is still in occlusion. If the foil slides out of the patient's mouth this indicates that the patient is not occluding on the tested teeth; if the foil cannot be removed during occlusion, then it may be assumed that the tested teeth are in contact.
A recently introduced hybrid articulating paper (Arti-Fol®, Bausch, bauschpaper.com) is a 12-µm foil that shares many characteristics with shimstock but offers the added benefit of having two sides of varying color coatings that will leave markings on a patient's teeth. The product is essentially an extremely thin articulating paper with the tear resistance of a foil. It allows the practitioner to mark static and dynamic occlusion in different colors with the use of one durable product.
Generally, when clinicians check occlusion, they have the patient bite up and down (ie, in a tap, tap, tap motion) on a piece of articulating paper. This helps with understanding the patient's static occlusion, the relationship between the upper and lower teeth when the jaws are at rest and closed in a stable, stationary position, such as maximum intercuspation. Static occlusion is basically the manner in which the teeth fit together when the mouth is not in motion or performing any functional activities, such as mastication or speaking. To learn about a patient's dynamic occlusion, or the occlusion when the jaws are in motion during various oral activities, clinicians have their patients perform excursive movements after static occlusion has been established. Usually, static occlusion is measured in one color and dynamic occlusion is measured in another color, which is easily captured with a multi-color articulating paper, such as Arti-Fol. This two-step occlusion testing helps reveal most premature or interfering contacts.
Analyzing Occlusion
Measuring dynamic occlusion advances the clinician's understanding of the patient's occlusion one step further than simple static occlusion; however, there may still be many questions left unanswered. For example, which tooth is the patient biting on the hardest? Are both sides of the mouth biting evenly? Are the teeth moving or sliding around when they shouldn't be?
A new system, the OccluSense® (Bausch), is designed to answer many of these questions and has been extremely useful to the authors in analyzing their patients' occlusions. The system comprises a full-arch, 60-µm articulating paper that records a patient's occlusion both physically in the patient's mouth and digitally on an iPad® (Apple Inc.). As with a traditional articulating paper, the patient's teeth are marked, with a red color; however, the digital component is what gives this technology additional value. While the patient is articulating, the OccluSense records his or her mastication in 256 different pressure levels, which can be displayed on the accompanying iPad in diagrams showing up to 150 images per second. In simple terms, the technology shows occlusion over time, from the initial contact, sliding into intercuspation, and then into the maximal intercuspal position. The clinician and patient can see which teeth or quadrants of teeth are receiving the most force, where all the contact points are, whether the contacts are broad or sharp, and how these change over time.
This tool can be used for various purposes. A record of the patient's occlusion can be taken prior to performing any dental work to serve as a diagnostic tool and, more importantly, as a reference point. A post-treatment recording can be taken to ensure that the patient's occlusion was, in fact, improved or maintained. Within the scope of restorative dentistry this can include evaluating occlusion upon completing a quadrant of composites; within orthodontics, it may include equilibrating occlusion after completing treatment; and in prosthodontics, occlusion can be balanced when fabricating fixed or removable prostheses. The indications for the use of OccluSense are numerous.
The following three case examples help demonstrate some of the benefits of incorporating this technology into practice.
Case 1
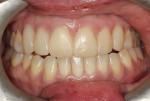
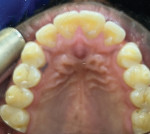
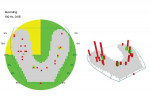
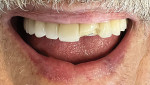
Patient No. 1 presented to the authors' office while she was in the midst of having prosthodontic work done that had been started in another country. She had completed orthodontic therapy and was now in the process of improving her occlusion and dental cosmetics by having crowns fabricated for her upper teeth. Her chief complaint when she arrived at the authors' office was that she was unable to find a comfortable occlusion, a problem that would often leave her with muscle pain and headaches. Her occlusion was rather unique, as she was only occluding on her posterior teeth, yet she felt most comfortable in that arrangement (Figure 1).
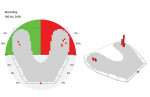
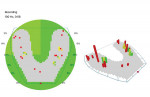
The clinician started by recording a set of diagnostics, which included radiographs, an intraoral scan, photographs, and an OccluSense reading. The initial reading showed that the patient had only a few true points of contact, with much heavier occlusion on the left side of her mouth (Figure 2). Because the patient was in temporary crowns when she presented to the office, a combination of additive dentistry and reduction was used to facilitate a more stable occlusion. An intraoral scan was then taken to record this occlusion, and a new set of temporary crowns were fabricated, with care taken to maintain the occlusion that had just been created.
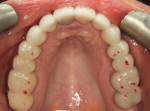
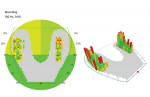
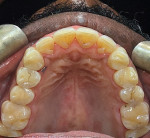
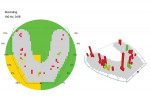
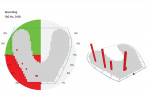
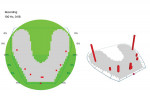
The patient remained in the temporary crowns for a few weeks, during which time she was brought back into the office once to adjust the occlusion, with the OccluSense used as an aid. When the patient was comfortable and happy with her bite, one more intraoral scan was taken so that the final restorations could be made in an occlusion that was acceptable to her (Figure 3 and Figure 4). Using the OccluSense to clearly identify where the occlusion was unbalanced enabled the clinician to take the patient out of discomfort and create a solution for her complex case.
Case 2
Patient No. 2 presented to the authors' office with a chief complaint of disliking the spacing between his upper anterior teeth (Figure 5). This seemed like an ideal case for clear aligner orthodontic therapy, so the clinician took diagnostic records, including a pretreatment OccluSense measurement (Figure 6). The patient then proceeded to undergo about 3 months of orthodontic treatment.
At the conclusion of the orthodontic treatment the patient was extremely satisfied with the results, as the gaps in his smile were fully closed (Figure 7). However, he mentioned that his "bite felt off" but was unsure why. The clinician suspected that this was due to a premature anterior contact caused by retrusion of the patient's upper anterior teeth that had been done in order to close his gaps. Using the OccluSense, the clinician pinpointed the exact areas of occlusal interferences and equilibrated the patient's occlusion to get him into an occlusion that was similar to his pretreatment occlusion (Figure 8 and Figure 9). This was made possible by having the pretreatment OccluSense measurement that had been taken at the beginning of treatment and which served as a reference when adjusting the post-treatment occlusion.
In most orthodontic cases some level of equilibration is usually needed at the end of treatment to ensure a comfortable and fully functional occlusion.3 Use of the OccluSense makes these equilibrations more predictable and efficient, and thus it is beneficial to take a pretreatment and post-treatment reading in all orthodontic cases.
Case 3
In the case of Patient No. 3, the patient presented to the authors' practice having recently completed a maxillary full arch of implants at a different practice and was now looking for a fixed prosthesis. Several appointments were spent determining the proper esthetics and function for the prosthesis, until both the patient and clinician were satisfied. The clinician then delivered the final restoration and told the patient to return in 1 week for a post-treatment check-up. One day later, however, the patient returned with fractured porcelain on his front tooth, No. 9 (Figure 10).
This was an astonishing and highly unexpected development, and the clinician proceeded to try to determine a cause for the problem in order to correct it. After several diagnostic tests were conducted, an OccluSense measurement was taken, which revealed that the patient's occlusion was completely unbalanced (Figure 11) and unprotected. While the OccluSense had not been used at the initial delivery appointment, the clinician did check the occlusion before dismissing the patient. However, because the patient had a complete mandibular denture, the occlusion that he demonstrated at his prosthesis delivery must have been different from the occlusion shown at this emergency appointment.
Utilizing the OccluSense for guidance, the clinician equilibrated the patient's occlusion and was able to create a balanced and protected occlusion (Figure 12). After the patient was in the temporary prosthesis for several weeks, he confirmed that the occlusion functioned well. At that point, a new final full-arch prosthesis was delivered to the patient. This new prosthesis is currently functioning very well and the patient's occlusion has been corrected. The OccluSense provides invaluable information, especially when it relates to fixed or removable full-arch prostheses, turning long and frustrating occlusal equilibrations into predictable appointments.
Conclusion
While there are many tools to aid clinicians in determining and analyzing occlusion, two products in particular can be instrumental in doing so. The first and most essential product is a thin, durable, two-colored articulating paper, like Arti-Fol. The second, more advanced tool is a digital occlusal analyzer, such as the OccluSense. With the correct usage of complementing products, dental practitioners can ensure that their patients' oral health is examined and treated properly.
Disclosure
This article was commercially supported by Bausch.
About the Authors
Isaac Tawil, DDS, MS
Founder and Director, Advanced Implant Education; Private Practice, Brooklyn, New York
Michael Erdos, DDS
Private Practice, Brooklyn, New York
References
1. Lobbezoo F, Ahlberg J, Manfredini D, Winocur E. Are bruxism and the bite causally related? J Oral Rehabil. 2012;39(7):489-501.
2. de Kanter RJ, Battistuzzi PG, Truin GJ. Temporomandibular disorders: "occlusion" matters! Pain Res Manag. 2018;2018:8746858. doi: 10.1155/2018/8746858.
3. Jones PE. Innovative techniques with clear aligners: the thermoplastic pontic appliance. J American Academy of Cosmetic Orthodontics. Winter 2015;14-20.