Diagnosing Oral Granulomatous Lesions: A Case Report
Trever L. Siu, DMD, MS; Douglas W. Beals, DDS, MS; John R. Francis, DDS, MS; and Vijay P. Parashar, BDS, MDSc, DDS
Abstract: The diagnosis of oral granulomatous lesions raises many challenges for the clinician. This article, which includes a case report, describes a process to formulate differential diagnoses by identifying distinguishing characteristics of an entity and applying that information to attain understanding of the ongoing pathophysiological process. Relevant clinical, radiographic, and histologic findings of common disease entities that can mimic clinical and radiographic presentation of this case are discussed to aid dental clinicians in identifying and diagnosing similar lesions in their practice.
Granulomas are small areas of inflammation,1 and practicing dentists may encounter these on a frequent basis. The causes of granulomas in the oral cavity vary, ranging simply from a root fracture, to extensive decay of a neighboring tooth, or a pending or failed root canal treatment. Of further concern, the reactive inflammation in the presenting area may have been caused by trauma or irritation or could have a more serious form neoplastic in origin, in which case the clinician will need to properly recognize and possibly treat the anomaly. Because many of the granulomatous lesions that can potentially surface in the mouth can be difficult to distinguish, invariably a proper microscopic analysis will be indicated.
The following case report is the basis for a presentation of a process to formulate differential diagnoses by identifying distinguishing characteristics of an entity and applying this information to gain understanding of the ongoing pathophysiological process.
Case Presentation: Diagnosing an Incidental Oral Lesion
A 64-year-old Caucasian woman presented to the Midwestern University Dental Clinic in Arizona for a routine recare dental appointment. Her medical history consisted of postmenopausal hormone therapy, osteoporosis, and a hip arthroplasty. She also had a diagnosis of Parkinsonism and asthma. The patient was currently taking medications that included amantadine, pramipexole, and sinemet for Parkinsonism, estradiol for postmenopausal symptoms, and mometasone and albuterol for asthma as needed.
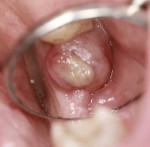
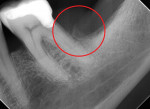
During examination, the patient reported discomfort in the area of site No. 18, which presented intraorally with what seemed to be exposed bone, but was found to be a 6 mm x 6 mm gingival lesion that appeared as a central yellow-like nodule surrounded circumferentially by a 3 mm collar of erythematous gingival tissue (Figure 1). Extraorally, the patient exhibited swelling of her left cheek and generalized pain upon palpation along the left side of her mandible. A diagnostic periapical radiograph was captured, which displayed an area of irregular resorption or new bone formation at the level of the alveolar crest in proximity to the location of the gingival lesion (Figure 2).
Upon review of the patient's dental history, it was noted that tooth No. 18 had been extracted approximately 1 year earlier, at which time future implant therapy had been planned to restore optimal function in the mandibular left posterior sextant. A provisional diagnosis of a periodontal abscess due to food impaction at the distal aspect of tooth No. 19 had been made previously, and the patient had been treated with a 7-day course of systemic antibiotics and chlorhexidine rinse before presenting to the authors' clinic.
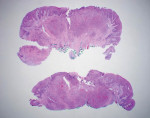
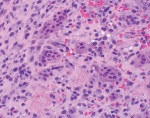
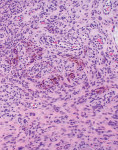
An excisional biopsy of the lesion was performed, and the specimen was submitted to a pathology laboratory. The results of the histologic analysis are shown in Figure 3 and Figure 4.
Diagnosis and Discussion
A number of diagnoses could have been considered in this case, including central giant cell granuloma (CGCG), medication-related osteonecrosis of the jaw (MRONJ), osteosarcoma, peripheral giant cell granuloma (PGCG), and peripheral ossifying fibroma (POF). The authors thought it best to focus their diagnosis on these less frequently observed entities, as the lesion did not present as a more typical bluish pyogenic lesion.
The patient's gender, the duration of the lesion, and the lesion's clinical and histologic appearances strongly aligned with a diagnosis of PGCG. Also known as extraosseous giant cell granuloma or peripheral giant cell lesion, PGCG is a common tumor-like growth found in the oral cavity that often develops as a reactive lesion secondary to local irritation or trauma.1 PGCG is typically described as a reddish-blue colored lesion; however, in this case the clinical presentation of the lesion was whitish-yellow. This case of PCGC could not be diagnosed at the time of its clinical presentation; rather, this lesion was definitively diagnosed as PCGC from the histologic analysis.
These lesions are most commonly found on the gingiva or edentulous ridge and usually present as a nodular mass measuring less than 2 cm. They show no age predilection but are observed more commonly in females and are often mistaken as pyogenic granuloma. The most characteristic radiographic finding associated with PGCGs is the "cupping" resorption of the underlying alveolar bone (Figure 2).1
Routine microscopic analysis of PGCG reveals the presence of an abundance of multinucleated giant cells with ulcerated granulation tissue, which is a distinctive feature of PGCG (Figure 4).1 Evidence of fusion of blood monocytes forming osteoclastic multinucleated giant cells is also characteristic of PGCG (Figure 4 and Figure 5), consistent with profuse hemorrhage observed within the mass. Additionally, the presence of brown pigmentation within the histologic specimen correlates with the presence of hemosiderin and is a hallmark feature of PGCG (Figure 5).1
The most appropriate treatment of PGCG is surgical excision of the lesion followed by thorough debridement of the lesion and adjacent areas. PGCGs have a recurrence rate of approximately 15% following excision without curettage, and a recurrence rate of 3% following excision with curettage.2
In the present case, other than extraction of tooth No. 18 a year earlier, there was no evident ongoing local irritation or trauma to the area in question. With the lesion presenting similarly to other pathologic lesions, and the belief from some researchers that POFs and pyogenic granulomas are difficult to distinguish,1 diagnoses from clinical or radiographic findings alone are hindered, and excisional biopsy is necessary for a confirmed diagnosis. Since excisional removal of the lesion, the patient has been seen for routine prophylaxis over the past year, and there have been no signs of recurrence at the lesion site.
Review of Other Differentials
Central Giant Cell Granuloma
Central giant cell granuloma (CGCG) is a non-neoplastic, reactive lesion of the jaw, commonly found intraosseously in the anterior mandible among young women and girls. Clinically, CGCG typically presents as a slow-growing, asymptomatic expansion of the cortical bone.3 Radiographically, CGCG presents as radiolucent lesions, ranging from a single small lesion around a tooth root to large lesions that encompass much of the mandible.1 Histologically, CGCG is characterized by foci of irregular, highly variable, multinucleated giant cells within a background of mesenchymal and hemorrhagic cells.4
While the etiology of CGCG is unknown, lesions can be categorized as either non-aggressive or aggressive. Non-aggressive lesions are treated with conservative surgical management. In rare instances, CGCGs can develop as rapidly growing, painful lesions that measure more than 5 cm; in such cases, treatment would consist of wide en bloc resection followed by extensive reconstruction of the jawbone.5 Recently, the use of corticosteroids has shown promise in the resolution, or at least the reduction in size, of these aggressive lesions. Despite the availability of this treatment, the lesions are associated with a high recurrence rate (35% to 70%).3
Medication-Related Osteonecrosis of the Jaw
Commonly known by the acronym MRONJ, medication-related osteonecrosis of the jaw is a condition of exposed, dead, or dying bone and is most frequently seen in patients who are currently or were previously taking antiresorptive medications. Current understanding of the mechanism of antiresorptive medications on bone metabolism is that it involves decreased local vascular support and a reduction in the action of osteoclasts and vascularization, which leads to poor bone remodeling and bone matrix physiology.6,7 Some of the main triggering mechanisms of MRONJ are peri-implant surgery, exodontia, and buccal mucosa trauma.8
MRONJ usually manifests clinically as exposed jawbone, but it may also present as infection or remain asymptomatic.6 Maciel et al conducted an integrative review of the clinical profiles of bisphosphonate-related osteonecrosis and concluded that the main diagnostic criterion of the malady is exposure of bone, which was found in 100% of the cases.9 They also concluded that the mandible is twice as likely to be affected than the maxilla and that the posterior mandible is mostly involved.
Whether or not a "drug holiday" of antiresorptive medication offers any benefit in preventing MRONJ is debatable. A recent study showed that discontinuing the use of bisphosphonate before dental extraction offered little benefit in the prevention of MRONJ.10 Yet, a position paper by the American Association of Oral and Maxillofacial Surgeons states that for patients receiving oral bisphosphonates, a 2-month drug holiday may be helpful in preventing bone necrosis.11 Although no defined algorithm exists for the treatment of MRONJ, the focus should include pain management, infection control, and prevention of further bone destruction.12
Osteosarcoma
Osteosarcoma is the most common bone malignancy, most often affecting the metaphysis area of lower long bones.13 In the oral cavity, however, these neoplasms are less common and tend to appear in patients younger than age 30 years.14 While the occurrence of these tumors is rare, they are quite deadly and represent the seventh most common cancer in children.15
Osteosarcoma in the jaw usually presents clinically as swelling, accompanied by pain. Ulcerations or paresthesia are less-common presentations.16 Radiographically, the osteosarcoma lesion will appear as a poorly defined lytic, sclerotic, or mixed-density lesion,17 or it may have a spiculated periosteal reaction. This radiographic reaction of the periosteum has been described as a sunburst pattern caused by the radiating mineralized tumor spicules.17 Because of the limited information available from conventional radiographs, it has been suggested that the use of contrast-enhanced multidetector computed tomography may show an enhanced image of the solid component of the neoplasm.18
Once the diagnosis of osteosarcoma is confirmed through an incisional biopsy, management may consist of a combination of wide surgical resection and chemotherapy.17
Peripheral Ossifying Fibroma
Peripheral ossifying fibroma (POF) is a non-neoplastic, reactive gingival condition commonly found within the oral cavity.19 Despite an unknown etiology and pathogenesis, its formation has been known to be precipitated by trauma or local irritation, occlusal overload, and/or poor-quality restorations. Historically, POF was considered synonymous with peripheral odontogenic fibroma, but today it is deemed a distinct entity and is believed to have derived from a pyogenic granuloma that undergoes fibrous maturation and calcification.1
POF typically presents in adolescents and young adults as a pedunculated or sessile, ulcerated nodule exclusively on the gingiva.20 It is usually found around maxillary incisors and canines, emanating from the interproximal papillary tissues.
Histologic analysis is often characterized by a proliferation of fibrous tissue with random traces of mineralized products, such as bone, cementum-like material, or dystrophic calcification.21
Treatment of choice is complete surgical removal of the lesion, including the periosteum, to minimize the chance of recurrence, followed by thorough debridement of the affected and adjacent areas. The specimen should be sent for histopathologic evaluation to confirm its diagnosis.
Conclusion
The patient in this case report presented with a gingival lesion accompanied by generalized pain and localized swelling along the left mandible. In addition to peripheral giant cell granuloma, the differential diagnoses included central giant cell granuloma, medication-related osteonecrosis of the jaw, osteosarcoma, and peripheral ossifying fibroma, as the lesion had characteristics consistent with these entities. Clinically, the patient appeared to present with white, exposed bone, which upon closer examination was found to be an ulcerated, granulomatous mass. The bone resorption or new bone formation and sunburst pattern on the periapical radiograph were also concerning, being more indicative of an aggressive bony lesion or neoplasm.13,14 Per the biopsy report, the diagnosis of PCGC was confirmed histologically by the identification of blood monocytes fused to form osteoclastic multinucleated giant cells.
When formulating a differential diagnosis for a patient who presents with a granulomatous lesion in the oral cavity, the dental practitioner should keep in mind the "three P's": peripheral ossifying fibroma, peripheral giant cell granuloma, and pyogenic granuloma, and the importance of biopsy and histological examination.
Acknowledgment
The authors thank Lee J. Slater, DDS, MS, of Scripps Oral Pathology Service for supplying the histologic images used in this article.
About the Authors
Trever L. Siu, DMD, MS
Associate Professor, Midwestern University College of Dental Medicine, Glendale, Arizona
Douglas W. Beals, DDS, MS
Associate Professor, Midwestern University College of Dental Medicine, Glendale, Arizona
John R. Francis, DDS, MS
Associate Professor, Midwestern University College of Dental Medicine, Glendale, Arizona
Vijay P. Parashar, BDS, MDSc, DDS
Professor and Associate Dean, Midwestern University College of Dental Medicine, Glendale, Arizona
References
1. Neville B, Damm DD, Allen CM, Bouquot JE. Oral & Maxillofacial Pathology. Philadelphia, PA: W.B. Saunders; 2002:188-190.
2. Chrcanovic BR, Gomes CC, Gomez RS. Peripheral giant cell granuloma: an updated analysis of 2824 cases reported in the literature. J Oral Pathol Med. 2018;47(5):454-459.
3. Rachmiel A, Emodi O, Sabo E, et al. Combined treatment of aggressive central giant cell granuloma in the lower jaw. J Craniomaxillofac Surg. 2012;40(3):292-297.
4. Gupta M, Gupta M, Singh S, Kaur R. Central giant cell granuloma of the maxilla. BMJ Case Rep. 2013;2013:bcr2013009102.
5. de Lange J, van den Akker HP, van den Berg H. Central giant cell granuloma of the jaw: a review of the literature with emphasis on therapy options. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;104(5):603-615.
6. Marx RE. Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg. 2003;61(9):1115-1117.
7. Ruggiero SL, Mehrotra B, Rosenberg TJ, Engroff SL. Osteonecrosis of the jaws associated with the use of bisphosphonates: a review of 63 cases. J Oral Maxillofac Surg. 2004;62(5):527-534.
8. Lopes RN, Rabelo GD, Rocha AC, et al. Surgical therapy for bisphosphonate-related osteonecroses of the jaw: six-year experience of a single institution. J Oral Maxillofac Surg. 2015;73(7):1288-1295.
9. Maciel AP, Quispe RA, Martins LJO, et al. Clinical profile of individuals with bisphosphonate-related osteonecrosis of the jaw: an integrative review. Sao Paulo Med J. 2020;138(4):326-335.
10. Hasegawa T, Kawakita A, Ueda N, et al. A multicenter retrospective study of the risk factors associated with medication-related osteonecrosis of the jaw after tooth extraction in patients receiving oral bisphosphonate therapy: can primary wound closure and a drug holiday really prevent MRONJ? Osteoporos Int. 2017;28(8):2465-2473.
11. Ruggiero SL, Dodson TB, Fantasia J, et al. American Association of Oral and Maxillofacial Surgeons position paper on medication-related osteonecrosis of the jaw - 2014 update. J Oral Maxillofac Surg. 2014;72(10):1938-1956.
12. Nicolatou-Galitis O, Schiodt M, Mendes RA, et al. Medication-related osteonecrosis of the jaw: definition and best practice for prevention, diagnosis, and treatment. Oral Surg Oral Med Oral Pathol Oral Radiol. 2019;127(2):117-135.
13. Lindsey BA, Markel JE, Kleinerman ES. Osteosarcoma overview. Rheumatol Ther. 2017;4(1):25-43.
14. Baumhoer D, Brunner P, Eppenberger-Castori S, et al. Osteosarcomas of the jaws differ from their peripheral counterparts and require a distinct treatment approach. Experiences from the DOESAK Registry. Oral Oncol. 2014;50(2):147-153.
15. Ward E, DeSantis C, Robbins A, et al. Childhood and adolescent cancer statistics, 2014. CA Cancer J Clin. 2014;64(2):83-103.
16. ElKordy MA, ElBaradie TS, ElSebai HI, et al. Osteosarcoma of the jaw: challenges in the diagnosis and treatment. J Egypt Natl Canc Inst. 2018;30(1):7-11.
17. Tahmasbi-Arashlow M, Barnts KL, Nair MK, et al. Radiographic manifestations of fibroblastic osteosarcoma: a diagnostic challenge. Imaging Sci Dent. 2019;49(3):235-240.
18. Bojan A, Christy W, Chanmougananda S, Ashokan K. Osteosarcoma of mandible: a case report and review of literature. J Clin Diagn Res. 2012;6(4):753-757.
19. Mohiuddin K, Priya NS, Ravindra S, Murthy S. Peripheral ossifying fibroma. J Indian Soc Periodontol. 2013;17(4):507-509.
20. Mishra MB, Bhishen KA, Mishra S. Peripheral ossifying fibroma. J Oral Maxillofac Pathol. 2011;15(1):65-68.
21. Sharma S, Anamika S, Ramachandra SS. Peripheral ossifying fibroma: a clinical report. Compend Contin Educ Dent. 2011;32(5):E86-E90.