Minimally Invasive Coronally Advanced Flap Techniques for Correction of Gingival Recession Defects: A Review
Jennifer M. Duffy, DMD; Jessica M. Latimer, DDS; Ronald M. Fried, DMD, MMSc; and Irina F. Dragan, DDS, DMD, MS
Abstract: For treatment of patients with isolated and/or multiple adjacent gingival recession defects, debate exists as to whether minimally invasive coronally advanced flap-based surgical techniques achieve improved root coverage compared with traditional evidence-based techniques. Correction of gingival recession defects requires mucogingival surgery utilizing tissue grafting and/or soft-tissue alternatives. Traditional mucogingival techniques for root coverage using autogenous tissue are associated with patient morbidity and discomfort. Considering the philosophical shift in daily practice from "patient-centered" to "person-centered," minimally invasive surgical procedures are warranted that provide esthetic results with reduced morbidity. This review article evaluates five minimally invasive mucogingival techniques: semilunar, tunneling, modified tunneling, vestibular incision subperiosteal tunnel access, and pinhole. These surgical procedures and their clinical application are compared and contrasted.
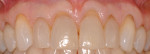
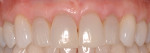
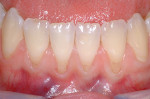
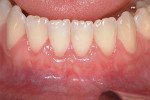
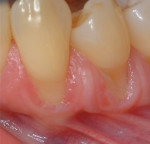
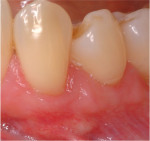
Gingival recession is the displacement of marginal gingival tissue apical to the cementoenamel junction (CEJ) of teeth. The purpose of mucogingival or periodontal plastic surgery is to increase the amount of attached gingiva and/or obtain root coverage in areas of gingival recession (Figure 1 through Figure 3).1 The causes of gingival recession are multifactorial and can include overzealous oral hygiene practices, prior orthodontic therapy, and/or a history of periodontal disease.2 Further, anatomical conditions such as thin gingival phenotype, lack of adequate keratinized tissue, tooth malposition in the dental arch, prominent buccal tooth roots, and thin bony cortices with fenestration/dehiscence defects can predispose individuals to gingival recession.3-6
Surgical correction of recession is indicated for esthetic purposes, root hypersensitivity, and root caries prevention.4 With age, mucogingival recessions increase in prevalence, with one study reporting 99.7% of subjects aged >35 years presenting with a recession defect.7 Traditional corrective techniques, including the use of envelope flaps, pedicle flaps, and coronally advanced flaps (CAFs), all with or without the addition of a subepithelial connective tissue graft (SCTG), have a vast existing evidence base.8 Currently, there is growing interest in minimally invasive surgical techniques that can yield acceptable esthetic outcomes with reduced patient morbidity. This article is intended to make practitioners aware of and critically evaluate newer techniques described in the literature for the treatment of mucogingival deformities.
Methods
With the support of an expert librarian, the authors conducted an electronic, focused search of the PubMed database to identify all relevant English, human-study, free-access articles published prior to August 16, 2021. The comprehensive literature query was conducted from August 2020 through August 2021 by the principal investigator (JMD) with the following search strategy: ("semilunar" [All Fields] OR "tunnel" [All Fields] OR "tunneled" [All Fields] OR "tunneling" [All Fields] OR "tunnelings" [All Fields] OR "tunnelization" [All Fields] OR "tunnelized" [All Fields] OR "tunnelled" [All Fields] OR "tunnelling" [All Fields] OR "tunnels" [All Fields]) OR (("modifiable" [All Fields] OR "modified" [All Fields] OR "modifier" [All Fields] OR "modifiers" [All Fields] OR "modifies" [All Fields] OR "modify" [All Fields] OR "modifying" [All Fields]) AND ("tunnel" [All Fields] OR "tunneled" [All Fields] OR "tunneling" [All Fields] OR "tunnelings" [All Fields] OR "tunnelization" [All Fields] OR "tunnelized" [All Fields] OR "tunnelled" [All Fields] OR "tunnelling" [All Fields] OR "tunnels" [All Fields])) OR "MCAT" [All Fields] OR ("vista" [All Fields] OR "vistas" [All Fields]) OR ("pinhole" [All Fields] OR "pinholes" [All Fields])) AND ("gingiva" [MeSH Terms] OR "gingiva" [All Fields] OR "gingivae" [All Fields] OR ("periodontal" [All Fields] OR "periodontally" [All Fields] OR "periodontically" [All Fields] OR "periodontics" [MeSH Terms] OR "periodontics" [All Fields] OR "periodontic" [All Fields] OR "periodontitis" [MeSH Terms] OR "periodontitis" [All Fields] OR "periodontitides" [All Fields]) OR ("recessed" [All Fields] OR "recessing" [All Fields] OR "recession" [All Fields] OR "recessions" [All Fields])).
The initial search, excluding repeats, yielded 392 citations. After screening and review, publications that did not report on the desired surgical techniques for correction of gingival recession, root coverage, or phenotypic defects were excluded. A total of 183 relevant articles were identified (Figure 4), 61 of which described a modified tunneling technique. This review provides an evidence-based summary of minimally invasive techniques for mucogingival surgery, providing support for clinicians interested in differentiating these techniques and integrating them into their daily practice. Primary differences among these CAF techniques are shown in the Fig. 5 illustrations.
Results
Semilunar Technique
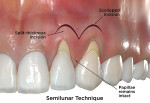
Initially described by Tarnow in 1986,9 the semilunar technique begins with a scalloped incision in the attached gingiva and/or alveolar mucosa that parallels the gingival margin of adjacent teeth with recession defects (Fig 5 a, Semilunar Technique). Coronally, the incision ends interproximally; however, 2 mm of the papillae adjacent to the defect is left undisturbed to provide adequate flap vascularization. A sulcular split-thickness incision is then made for all involved teeth, and the original semilunar incision is connected to the sulcular incision via a split-thickness flap. The mobilized flap is positioned coronally to cover the unwanted recessions, with the apical portion of the flap resting on bone, not root surface. The flap is held down with firm pressure for 5 to 10 minutes using a moist gauze to provide clot formation and flap stability. No sutures are used to secure this flap, and healing of the semilunar incision occurs via secondary intention.9
Indications for the semilunar technique are Miller class I recession defects,10 maxillary recession defects (where gravity reinforces coronal flap positioning),9,11 cases where adequate keratinized tissue is present,9 and cases where a thick gingival phenotype is present.9,11
Advantages of the semilunar technique include papillae preservation, the lack of flap tension after coronal repositioning, no need for sutures, no vestibule shortening, increased width of keratinized tissue, and minimal patient morbidity due to there being no donor tissue site.9,12
Among the disadvantages of the semilunar technique are the likelihood of scar formation and the fact that the procedure produces less predictable long-term complete root coverage when compared with other mucogingival techniques.13 This latter shortcoming may be due to flap instability causing wound contraction.
Tunneling Technique
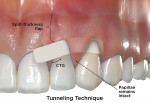
The tunneling technique was originally introduced by Allen in 1994 and later adapted by Zabalegui et al in 1999.14,15 The technique consists of initial intrasulcular incisions around teeth with gingival recession, and these incisions are then extended to the mucogingival junction by partial-thickness flap dissection (Fig 5 b, Tunneling Technique). Continuity is established between these partial-thickness dissections without the releasing of interdental papillae, creating a multi-envelope recipient bed or "tunnel" involving all recession-affected teeth. A graft material is slid through the intrasulcular incision into the tunnel and sutured to its desired position to obtain recession coverage. The mobilized tunnel flap is then coronally repositioned and sutured into place over the graft material. If a soft-tissue alternative is utilized, the coronally repositioned flap must fully cover the graft for adequate results. If a SCTG is used, a limited portion of the graft may be left slightly exposed in relationship to the coronally repositioned flap.14,15
Indications for the tunneling technique include Miller class I, class II, and class III recession defects,14,15 multiple adjacent gingival recession defects,14 and esthetic-zone defects.16 Advantages of this technique are papillae preservation, minimal scarring, quick healing, and minimal postoperative morbidity.14
The tunneling technique, however, is technique sensitive, as care must be taken to avoid gingival flap detachment from interdental papillae, prevent flap perforation, and establish a single plane of dissection.15 Additionally, graft introduction through gingival sulci can be difficult and time-consuming.15,17
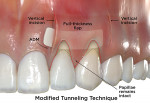
Modified Tunneling Technique
Introduced to overcome limitations of the original tunneling technique, the modified tunneling technique was first described by Mahn in 2001.17 The technique is similar to the tunneling technique, however it incorporates the addition of two vertical releasing incisions (VRIs) at the ends of the tunnel flap to facilitate graft placement and coronal flap advancement (Fig 5 c, Modified Tunneling Technique). These VRIs begin in the middle, or apical to the center, of appropriate interdental papillae and continue into the buccal mucosa, creating a wider trapezoidal mucosal base. A soft-tissue alternative is then sutured into position within the modified tunnel bed, and the flap is coronally repositioned and sutured into place over the respective graft using a vertical mattress suture technique.17
Since its introduction, the modified tunneling technique has been adapted in a wide variety of ways. Variations have involved the number and placement of VRIs, recommended site of correction, nature of flap preparation, graft/membrane material utilization, biomodification agent incorporation, and coronally advanced suturing technique.
The modified tunneling technique is indicated for coverage of multiple adjacent gingival recession defects in the esthetic zone,18 and evidence points toward its success in the correction of Miller class I, class II, and class III recession defects.17,19 Its advantages include papillae preservation,17 and the vertical incisions provide improved access to the tunnel for graft introduction and direct visual inspection of the tissue bed for tissue tags.17,20 Because of its somewhat less technique-sensitive nature, with increased flap mobility and decreased flap/papilla tearing,17,20 its usage has been expanded to include clinical conditions traditionally considered challenging for the tunneling technique; for example, it might be used in areas with inadequate keratinized gingival tissue.21 Nevertheless, the modified tunneling technique is still a fairly demanding procedure.20
Vestibular Incision Subperiosteal Tunnel Access
(VISTA) Technique
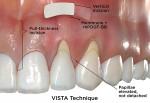
The VISTA technique was originally described by Zadeh in 2011.22 The technique begins with a vestibular full-thickness vertical access incision in nonkeratinized tissue (Fig 5 d, VISTA Technique). A subperiosteal tunnel is created through this incision using specialized instruments and is extended from beyond the mucogingival margin through the gingival sulci of affected teeth. The interdental papillae are undermined but not detached to facilitate coronal advancement of the flap. As per Zadeh, a resorbable collagen membrane saturated with recombinant human platelet-derived growth factor-BB (rhPDGF-BB) is positioned into the tunnel to cover adjacent recessions, and then the membrane and overlying mucogingival complex is advanced at least 2 mm coronal to the CEJ and secured with a coronally anchored suturing technique. Next, a beta-tricalcium phosphate (ß-TCP) matrix is placed between the secured membrane and the alveolar bone to aid wound healing and site vascularization. Lastly, the vertical access incision is closed with interrupted sutures.22
As with the modified tunneling technique, a number of variations of the VISTA technique have been utilized. These variations involve primarily the following aspects of the technique: recommended correction site, flap preparation, access incision location, graft choice, and coronally anchored suturing technique.
Indications for the VISTA technique include Miller class I, class II, and class III recession defects,22-24 multiple adjacent gingival recession defects,22,23 esthetic-zone defects,22 and soft-tissue augmentations/enhancements around dental implants in the esthetic zone.25
Along with papillae preservation, advantages of the VISTA technique include reduced surgical trauma to gingiva, reduced flap tension, and the allowance of broader surgical access. Also, vertical incision is less likely to disrupt blood supply to the surgical site. Additionally, reduced micromotion of gingival margins results in less scar-tissue formation, enhanced esthetic outcomes, and good long-term results.22
A limitation of this technique is the need for sufficient vestibular depth to perform the procedure.26
Pinhole Technique
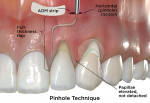
Developed by Chao in 2012, the pinhole technique is the newest of the minimally invasive CAF techniques described for recession coverage.27 The technique involves a 2 mm to 3 mm mucosal horizontal incision (termed a "pinhole" incision) near the base of the vestibule, apical to the teeth that are planned for recession coverage (Fig 5 e, Pinhole Technique). Specialized instruments are inserted through the incision to mobilize a full-thickness flap, which is extended to undermine interdental papillae two teeth mesial and distal to the recession area. Next, small graft strips are inserted through the pinhole incision and packed into place within the subgingival spaces and underneath papillae and marginal soft tissue. No sutures are required, but firm digital pressure is recommended for 5 minutes following material placement. Lastly, the pinhole incision is left to heal by first intention without suturing.
This technique can be used for Miller class I, class II, and class III multiple adjacent gingival recession defects, including in the esthetic zone.27,28 Because this technique is relatively newly developed, however, a minimal amount of supporting evidence for it exists in the literature.
To summarize, the pinhole technique's advantages are the lack of a need for sutures, good esthetic results, minimal postoperative morbidity, and quick healing.27,28 On the downside, specialized instruments are required, a learning curve is necessary, and results in the mandible typically are not as good as in the maxilla as certain factors favor the maxillary arch compared with the mandible, such as the width of keratinized tissue and favorable shape of the papillary tissue.27,28
Conclusion
This review has described newer minimally invasive mucogingival surgical techniques-semilunar, tunneling, modified tunneling, VISTA, and pinhole-used in daily practice for the treatment of recession defects. An evaluation of each technique's surgical approach, indications, advantages, and disadvantages was presented to compare and contrast the procedures. The intent of this review is to provide practitioners with an evidence-based foundation for making treatment decisions concerning the surgical correction of gingival recession defects. While these minimally invasive mucogingival techniques are effective for treating such defects, there is sparse evidence regarding their long-term success compared with traditional corrective methodologies.
Acknowledgment
The authors thank expert librarian Amanda Nevius for her support with this work.
About the Authors
Jennifer M. Duffy, DMD
Class of 2025, First-Year Postgraduate Resident, Department of Periodontology, UConn Health, Farmington, Connecticut
Jessica M. Latimer, DDS
DMSc Candidate, Class of 2024, Second-Year Postgraduate Resident, Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts
Ronald M. Fried, DMD, MMSc
Former Clinical Assistant Professor, Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts, Private Practice in Periodontics, Brookline, Massachusetts
Irina F. Dragan, DDS, DMD, MS
Adjunct Associate Professor, Department of Periodontology, Tufts University School of Dental Medicine, Boston, Massachusetts; Lecturer, Department of Oral Medicine, Infection, and Immunity, Harvard School of Dental Medicine, Boston, Massachusetts; Private Practice in Periodontics, Brookline, Massachusetts
References
1. Kasaj A. Gingival Recession Management: A Clinical Manual. Cham, Switzerland: Springer International Publishing AG, part of Springer Nature; 2018.
2. Chambrone L, Sukekava F, Araújo MG, et al. Root-coverage procedures for the treatment of localized recession-type defects: a Cochrane systematic review. J Periodontol. 2010;81(4):452-478.
3. Sculean A, Cosgarea R, Stähli A, et al. The modified coronally advanced tunnel combined with an enamel matrix derivative and subepithelial connective tissue graft for the treatment of isolated mandibular Miller Class I and II gingival recessions: a report of 16 cases. Quintessence Int. 2014;45(10):829-835.
4. Tözüm TF, Dini FM. Treatment of adjacent gingival recessions with subepithelial connective tissue grafts and the modified tunnel technique. Quintessence Int. 2003;34(1):7-13.
5. Kim DM, Bassir SH, Nguyen TT. Effect of gingival phenotype on the maintenance of periodontal health: an American Academy of Periodontology best evidence review. J Periodontol. 2020;91(3):311-338.
6. Cortellini P, Bissada NF. Mucogingival conditions in the natural dentition: narrative review, case definitions, and diagnostic considerations. J Periodontol. 2018;89 suppl 1:S204-S213.
7. Rios FS, Costa RS, Moura MS, et al. Estimates and multivariable risk assessment of gingival recession in the population of adults from Porto Alegre, Brazil. J Clin Periodontol. 2014;41(11):1098-1107.
8. Caton JG, Armitage G, Berglundh T, et al. A new classification scheme for periodontal and peri-implant diseases and conditions - introduction and key changes from the 1999 classification. J Clin Periodontol. 2018;45 suppl 20:S1-S8.
9. Tarnow DP. Semilunar coronally repositioned flap. J Clin Periodontol. 1986;13(3):182-185.
10. Bittencourt S, Del Peloso Ribeiro E, Sallum EA, et al. Semilunar coronally positioned flap or subepithelial connective tissue graft for the treatment of gingival recession: a 30-month follow-up study. J Periodontol. 2009;80(7):1076-1082.
11. Ahad A, Tasneem S, Lamba AK. Semilunar coronally repositioned flap: a minimally invasive technique for predictable management of gingival recession. N Y State Dent J. 2018;84(4):30-33.
12. Moka LR, Boyapati R, M S, et al. Comparison of coronally advanced and semilunar coronally repositioned flap for the treatment of gingival recession. J Clin Diagn Res. 2014;8(6):ZC04-ZC08.
13. Santana RB, Mattos CM, Dibart S. A clinical comparison of two flap designs for coronal advancement of the gingival margin: semilunar versus coronally advanced flap. J Clin Periodontol. 2010;37(7):651-658.
14. Allen AL. Use of the supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodontics Restorative Dent. 1994;14(3):216-227.
15. Zabalegui I, Sicilia A, Cambra J, et al. Treatment of multiple adjacent gingival recessions with the tunnel subepithelial connective tissue graft: a clinical report. Int J Periodontics Restorative Dent. 1999;19(2):199-206.
16. Santarelli GA, Ciancaglini R, Campanari F, et al. Connective tissue grafting employing the tunnel technique: a case report of complete root coverage in the anterior maxilla. Int J Periodontics Restorative Dent. 2001;21(1):77-83.
17. Mahn DH. Treatment of gingival recession with a modified "tunnel" technique and an acellular dermal connective tissue allograft. Pract Proced Aesthet Dent. 2001;13(1):69-74.
18. Sculean A, Cosgarea R, Katsaros C, et al. Treatment of single and multiple Miller Class I and III gingival recessions at crown-restored teeth in maxillary esthetic areas. Quintessence Int. 2017;48(10):777-782.
19. Sculean A, Cosgarea R, Stähli A, et al. Treatment of multiple adjacent maxillary Miller Class I, II, and III gingival recessions with the modified coronally advanced tunnel, enamel matrix derivative, and subepithelial connective tissue graft: a report of 12 cases. Quintessence Int. 2016;47(8):653-659.
20. Mahn DH. Esthetic correction of gingival recession using a modified tunnel technique and an acellular dermal connective tissue allograft. J Esthet Restor Dent. 2002;14(1):18-23.
21. Zuhr O, Fickl S, Wachtel H, et al. Covering of gingival recessions with a modified microsurgical tunnel technique: case report. Int J Periodontics Restorative Dent. 2007;27(5):457-463.
22. Zadeh HH. Minimally invasive treatment of maxillary anterior gingival recession defects by vestibular incision subperiosteal tunnel access and platelet-derived growth factor BB. Int J Periodontics Restorative Dent. 2011;31(6):653-660.
23. Gil A, Bakhshalian N, Min S, Zadeh HH. Treatment of multiple recession defects with vestibular incision subperiosteal tunnel access (VISTA): a retrospective pilot study utilizing digital analysis. J Esthet Restor Dent. 2018;30(6):572-579.
24. Fernández-Jiménez A, Estefanía-Fresco R, García-De-La-Fuente AM, et al. Description of the modified vestibular incision subperiosteal tunnel access (m-VISTA) technique in the treatment of multiple Miller class III gingival recessions: a case series. BMC Oral Health. 2021;21(1):142.
25. Lee CT, Hamalian T, Schulze-Späte U. Minimally invasive treatment of soft tissue deficiency around an implant-supported restoration in the esthetic zone: modified VISTA technique case report. J Oral Implantol. 2015;41(1):71-76.
26. Schulze-Späte U, Lee CT. Modified vestibular incision subperiosteal tunnel access procedure with volume-stable collagen matrix for root coverage: report of three cases. Int J Periodontics Restorative Dent. 2019;39(5):e181-e187.
27. Chao JC. A novel approach to root coverage: the pinhole surgical technique. Int J Periodontics Restorative Dent. 2012;32(5):521-531.
28. Reddy SSP. Pinhole surgical technique for treatment of marginal tissue recession: a case series. J Indian Soc Periodontol. 2017;21(6):507-511.