Preparing the Next Generation of Clinicians for Practice Using Augmented and Artificial Intelligence
Mina Ghorbanifarajzadeh, DMD; Ahmed M. Mahrous, BDS, MS; Muhammad Ali Shazib, DMD; Sheila Riggs, DDS, MS, DMSc; Jayda Dogan; and Teresa A. Dolan, DDS, MPH
ABSTRACT
Artificial intelligence (AI) and augmented intelligence (AuI) have existed for decades but have only recently been applied to dentistry and incorporated into higher education for dental professionals. Early examples of the incorporation of AI into dental education suggest that it can enhance students' learning and be applied in preclinical and clinical instruction. AI can be used to support clinical decision-making for dental professionals, making radiographic interpretation, for example, more precise and consistent. This article provides a brief overview of AI, highlights opportunities to improve higher education, and presents examples of individuals and organizations working to advance the quality of dental education using AI. Opportunities for the application of AI in dental education include the adoption of clinical decision support that can improve patient outcomes and overall quality of patient care; development of courses that assist students in learning enhanced radiographic interpretation, diagnosis, and treatment planning; research collaborations with industry for product evaluation and future product developments; and practice administration in understanding the quality of the care being delivered at the school.
Artificial intelligence (AI) and augmented intelligence (AuI) have existed for decades but have only recently been incorporated into higher education and applied to dentistry. These technologies can enhance students' learning experiences and be applied in preclinical and clinical instruction.1 Higher education students are increasingly aware of the presence of AI in their daily lives, suggesting that students will come to expect and quickly adapt to the integration of AI into their professional education.2 While AI and AuI are in the early stages of use in higher education, academic leaders believe their usage can support the creation of real-time, integrated, learning healthcare systems.3 AI can also support "on the go" education by using mobile learning and AI-tailored content based on the interests, weak points, or other needs of the learner. Additionally, AI can support mentoring and use real-time data to track students' progress, clinical experiences, and professional development.1 Thus, it is reasonable to expect the continued development and testing of how AI and mobile learning can be used to advance the education of health professionals.
This article provides a concise overview of AI, highlights opportunities to improve higher education, and presents brief case studies of individuals and organizations working to advance the quality of dental education using AI.
Artificial intelligence is defined as "the ability of a machine to perform cognitive functions that we associate with human minds, such as perceiving, reasoning, learning, interacting with the environment, problem-solving, decision-making, and even demonstrating creativity."4 It is important to note that AI cannot replace human intelligence but rather supports human interpretation and decision-making.5 Therefore, the argument has been made that it is more appropriate to discuss augmented intelligence when describing applications of these technologies to dental education and practice.3 In this article, artificial intelligence will be referred to in its various forms simply as AI. The advantages of using AI and its various applications include its ability to reduce or eliminate potential bias and human error, which typically occurs during repetitive work.5 Dental professionals can use AI to support clinical decision-making, such as making radiographic interpretation more precise and consistent, for example.5
The most common forms of AI include machine learning, deep learning, cognitive computing, computer vision, and natural language processing.3,4 They involve training computing systems to look for patterns to build analytical models and use algorithms to predict outcomes based on a dataset.5 Machine learning can occur in a supervised or unsupervised environment. Supervised machine learning uses labeled inputs and outputs to train algorithms to classify data or predict outcomes accurately. Unsupervised machine learning analyzes unlabeled datasets to discover patterns.6 Deep learning is a subset of machine learning and uses a complex neural network of computing systems to discover and analyze complicated patterns in very large datasets.3 This type of AI helps significantly with clinical decision support, such as aiding in the diagnosis, prognosis, and treatment planning of certain diseases.5
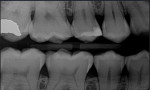
AI applied in healthcare has the potential to assist clinicians in reaching a diagnosis and predicting an accurate prognosis by quickly cross-referencing large amounts of patient data.5 The data from radiologic examinations can be analyzed using algorithms, which have the ability to assist with the identification of pathologies and diseases.5 Current applications of AI technology in dentistry include the detection of common oral findings, such as caries, calculus, and periapical lesions, as well as salivary gland, bony, and other pathologies, and alveolar bone measurements.5 Figure 1 compares a conventional bitewing radiograph to an AI annotated bitewing, on which the radiolucencies, restorations, and periodontal bone levels are labeled.
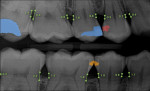
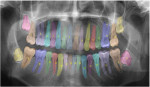
Image segmentation is a key task in computer vision and image processing. In current dental applications, it highlights a specific measurable area on each tooth, as seen in Figure 2. Each tooth is segmented by the AI and labeled with the appropriate tooth number. This then allows the AI to measure the area of each tooth. Segmentation is also used to denote the areas where there are restorations and possible decay. These areas can be measured with respect to the 2-dimensional coronal area of the tooth.
In addition to clinical decision support, AI is increasingly used to support nonclinical functions, such as insurance claims processing, assessing payment integrity, and supporting dental practice administrative functions.3 In recognition of the growing use of AI in dentistry and the need for standards, the American Dental Association Standards Committee on Dental Informatics released a white paper on the use of artificial and augmented intelligence in dentistry for comment.3
AI in Dental Education
Over the years, educators have emphasized the importance of developing students' critical thinking skills, and some have criticized the overuse of slide presentations as the main method of passively transferring information to students.7 Sharma et al went as far as to suggest that "the dental education program needs a ‘reboot' that makes better use of technological advancements," such as artificial intelligence.8 Wolcott et al noted that "dental curricula serve an essential role in preparing learners for the emerging oral healthcare environment," and this preparation can be enriched by incorporating AI into authentic learning experiences, using technologies in preclinical virtual learning experiences and then later in the clinical environment.9 Most dental and dental hygiene students are digital natives and expect the incorporation of technology into their education.7 For example, Yüzbaşıoğlu studied Turkish dental students' awareness and perception of AI.10 Three-fourths of the students agreed AI applications should be part of predoctoral dental education.10 Most dental students in this study agreed that incorporating AI in their dental education could greatly benefit their learning experience and would better prepare them for a future of clinical practice further enabled by technology.8 Dental students should be well versed in "handling and supervising AI tools, along with critically analyzing and interpreting AI data."8
The Commission on Dental Accreditation (CODA) plays a key role in setting standards for dental academic programs in the United States and Canada through reciprocal agreements. The Predoctoral Standards related to the "application of technology" recognize that "technology enables dental education programs to improve patient care, and to revolutionize all aspects of the curriculum, from didactic courses to clinical instruction."11 The two related intent statements regarding technology focus on how graduates should be able to evaluate and utilize new technologies, along with how dental schools should use evidence to assess the use of new technologies. However, AI is not explicitly mentioned in the standards. As AI becomes more commonly used in healthcare practice, CODA should consider revising the predoctoral standards to incorporate specific wording regarding the development of competencies in the use of clinical decision support tools that incorporate AI technology.
High Point University: Using CARE Curriculum Design
The High Point University (HPU) Workman School of Dental Medicine (WSDM) "is a new institution that is developing a novel curriculum and an experiential model that prepares learners for the future of dental medicine."9 The dental school will use a clinician-advocate-researcher-entrepreneur (CARE) curriculum based on an educational philosophy that is learner-centered and focused on supporting individual growth through education.9 The CARE curriculum design aligns with Oral Health In America: Advances and Challenges12 with the commitment that students' education ensures the efficient use of scientific advancements critical for delivering treatment within the changing environment of oral healthcare, which most likely will include the increased use of technology, enhanced capabilities for data exchange, and the opportunity for interprofessional collaboration and practice.9 HPU will incorporate technology, including artificial intelligence, to support students' learning and prepare them for future practice.
The method of learning that the school is embarking on is experiential, according to Muhammad Ali Shazib, DMD, Chief Clinical Officer at WSDM. In the first year, students will be exposed to virtual reality, haptics, simulation, and AI. In addition, students will be presented with concepts in a way that is focused on translation and application to clinical practice, with an emphasis on diagnosis, treatment planning, and practice management. Through the use of cases, students will be exposed to technologies and innovations, as well as key concepts.
The strategic vision and goals for HPU are to ensure that technologies, such as AI, are not just taught in theory, but are taught in authentic clinical learning environments and are fully considered from all perspectives, including healthcare systems, economics, practice, and education. According to Dr. Shazib, WSDM and its Oral Health Network believes that AI can deliver the school promising opportunities by way of its ability to objectify, analyze, and assess patterns in education, practice, and management and that AI can be an essential tool that will redefine the role of oral healthcare educators and practitioners.
University of Minnesota: Analyzing "Big Data"
At the University of Minnesota (UMN), it is believed there are opportunities to better understand dentistry and oral health using "big data," with the recognition that "stories exist in insurance claim data," according to Sheila Riggs,DDS, MS, DMSc, an oral epidemiologist and Chair of the Department of Primary Dental Care. She adds that AI can be used to analyze data from millions of insurance claims to better understand and predict clinical outcomes.
UMN recognizes the emerging importance of AI in healthcare as well as the availability of AI-driven and FDA-cleared clinical decision support tools. This helped drive the decision to include AI in UMN's strategic plan. A potential barrier to incorporating AI in the curriculum, according to Dr. Riggs, is ensuring that faculty feel competent and confident in the use of the technology, especially since the faculty will need to design the learning experiences and have them approved by the curriculum committee. At UMN, the belief is that the practice of dentistry will continue to evolve and marry new technologies that have been created to add value to patients and the care delivered.
UCSF Sees "Endless Applications of AI"
When the University of California San Francisco (UCSF) School of Dentistry evaluates new technologies prior to their adoption, the guiding principles always involve consideration of the most modern techniques for patient care and outcomes while creating a top-notch student educational program, according to Joel White, DDS, MS, who serves as the school's Chair of the Division of Preclinical Education, Biomaterials & Engineering and Vice Chair of the Department of Preventive and Restorative Dental Sciences. The dental school is currently evaluating AI products from the patient care, teaching, research, and clinical administration perspectives. UCSF believes there are endless applications of AI within dentistry, from general dentistry to every dental specialty, as well as supporting non-clinical aspects of dentistry, such as administration, productivity, and billing.
At UCSF, key opportunities for the application of AI in dental education include: provider augmentation and clinical decision support that improves patient outcomes and overall quality of patient care; assisting students in learning enhanced radiographic interpretation; research opportunities for validation and collaboratively participating with industry leaders for future product developments; and practice administration in understanding the quality of the care being delivered at the school.
UCSF School of Dentistry has successfully implemented other technologies, including digital scanning, CAD/CAM, 3D intraoral scanning, CBCT, and lasers. The faculty encourages hands-on learning experiences across the curriculum, from preclinical to clinical instruction. For technology to be incorporated into the curriculum, Dr. White says it must be better, quicker, higher quality, and easier to learn and understand than current methods and that technologies like AI can be implemented even more quickly, even within the next 5 years, rather than the 10 or so years that it typically takes to implement new technology. He expects the adoption period to be shorter because the industry better understands the needs of the institutions and provides support and other resources. He also notes that the interoperability of the technology remains a challenge, and as with any technology adoption, the school must consider compatibility and ease of use. In general, UCSF proposes that providers and students who are supported with AI will be enabled to provide their patients better care, better health, and lower costs.
ASDOH: Incorporating AI into Courses, Clinical Decision-Making Learning
Noticing a deficiency in standardization of removable partial denture (RPD) design and a lack of calibration among dentists and faculty in RPD design, Ahmed M. Mahrous, BDS, MS, Director of CAD/CAM Dentistry at the Arizona School of Dentistry and Oral Health (ASDOH), with the assistance of David L. Botsko, DMD, a practicing dentist in Iowa, recently created an AI-assisted RPD design software. The web-based software, along with a game and course, is aimed at taking advantage of the use of AI in education.13 The software uses AI algorithms to automatically generate RPD designs for any possible missing tooth configuration and clinical scenario. The algorithm was developed to support evidence-based RPD design philosophies as well as select institution-specific RPD designs, such as McCracken's, Stewart's, Stratton, University of Iowa, University of Connecticut, and ASDOH.14-16 The software also has a game component that provides AI-generated clinical scenarios to the students and offers instant, consistent feedback (Figure 3). The software and associated course provide numerous clinical scenarios for student practice (Figure 4) as well as automated evaluation and feedback.
The AI-assisted RPD design software and the course have since been implemented at the Spear online dental education platform as well as at multiple universities, including ASDOH, University of Iowa, University of Connecticut, and University of Illinois. The software is used at both the preclinical and clinical dental education levels and also as a reference for patient treatment in clinical practice. The biggest advantage of the AI-assisted RPD design software in education, according to Dr. Mahrous, is that it provides almost endless, standardized virtual practice exercises for dental students, while in clinics it provides a standardized design reference for patient care. He adds that his AI RPD course helps him teach better, enables students to learn more effectively, and gives clinical practitioners a standardized clinical reference.
Future Opportunities
Digitally-native dental students expect to use contemporary technology in their education, and schools are thus challenged to evaluate, select, and adopt technologies that advance student education and improve the quality of care delivered to patients. The aforementioned examples describe how dental schools and educators are incorporating AI into their educational philosophies, courses, and clinical workflows. Faculty members are finding new ways to enhance student learning and prepare them for future clinical practice that will undoubtedly incorporate more technology in the future. The goal, of course, is to prepare clinicians with strong critical-thinking skills who are committed to providing the best care to their patients. The recent availability of clinical decision support tools using AI cleared by the Food and Drug Administration provides opportunities for dental educators to use new approaches to teaching clinical topics such as caries detection and radiographic interpretation.
Clinical decision support tools such as radiographic annotations supported by AI have demonstrated key benefits, including provider consistency and standardization, efficient diagnostic workflows, increased case acceptance rates, and enhanced patient communication.17 In the educational environment, such a tool can be integrated into the dental curriculum to also assist in calibrating both faculty and students in radiographic interpretation and diagnosis.18
Implementing AI into dental education has potential barriers, including the cost of incorporating the software and integrating it into existing workflows and systems at the school. As with most technologies, clinical champions who invest the time to learn about the technology and thoughtfully evaluate its application in the dental school's educational and clinical environment are essential to successful adoption.17 The school's faculty must feel ready to embrace the technology and introduce it into the curriculum, and the school should be committed to systematically evaluating the impact of new technology on student learning and patient care.
Conclusion
Dental schools are responsible for preparing the next generation of clinicians who will practice in a world that increasingly utilizes advanced technology, including artificial intelligence, as a routine part of care delivery and management. Dental students expect to be engaged in authentic and active learning experiences using contemporary technologies so that they are well prepared for clinical practice. This article has highlighted examples of leading organizations and educators who have incorporated AI into their teaching or are thoughtfully considering how to best incorporate AI and new technologies into their organizations. Opportunities for the application of AI in dental education include the adoption of clinical decision support tools that can improve patient outcomes and overall quality of patient care and care delivery; development of courses that assist students in learning enhanced radiographic interpretation, diagnosis, and treatment planning; and research collaborations with industry for product evaluation and future product development.
ACKNOWLEDGMENT
The authors thank Joel White, DDS, MS, for his interview and perspectives.
DISCLOSURES
Drs. Dolan and Ghorbanifarajzadeh are full-time employees of Overjet, Inc., and Jayda Dogan was a student intern at Overjet, Inc. in 2022. Dr. Mahrous is owner of Dental Atlas LLC, the co-founder of AiDental systems with DB-connect LLC of David L. Botsko, DMD. Dr. Riggs is a member of the Board of Directors of Benco Dental.
ABOUT THE AUTHORS
Mina Ghorbanifarajzadeh, DMD
Clinical Manager, Overjet, Inc., Boston, Massachusetts
Ahmed M. Mahrous, BDS, MS
Associate Professor, Director of CAD/CAM Dentistry, Arizona School of Dentistry and Oral Health, Mesa, Arizona
Muhammad Ali Shazib, DMD
Associate Professor, Assistant Dean and Chief Clinical Officer, High Point University Workman School of Dental Medicine, High Point, North Carolina
Sheila Riggs, DDS, MS, DMSc
Associate Professor, Chair of the Department of Primary Dental Care, University of Minnesota School of Dentistry, Minneapolis, Minnesota
Jayda Dogan
Student Intern, Overjet, Inc., Boston, Massachusetts
Teresa A. Dolan, DDS, MPH
Chief Dental Officer, Overjet, Inc., Boston, Massachusetts; Professor and Dean Emeritus, University of Florida College of Dentistry, Gainesville, Florida
REFERENCES
1. Sousa MJ, Dal Mas F, Pesqueira A, et al. The potential of AI in health higher education to increase the students' learning outcomes. TEM Journal. 2021;10(2):488-497.
2. Kuleto V, Ilić M, Dedić V, Raketić K. Application of artificial intelligence and machine learning in higher education, available platforms and examining students' awareness. EdTech Journal. 2021;1(1):24-28.
3. Faiella R, Accurso B, Connelly S, et al. Overview of artificial and augmented intelligence uses in dentistry. ADA Standards Committee on Dental Informatics (SCDI) - Artificial Intelligence in Dentistry. July 2022. https://www.ada.org/resources/practice/dental-standards/standards-committee-on-dental-informatics. Accessed September 5, 2022.
4. Collins C, Dennehy D, Conboy K, Mikalef P. Artificial intelligence in information systems research: a systematic literature review and research agenda. Int J Information Management. 2021;60:102383.
5. Monterubbianesi R, Tosco V, Vitiello F, et al. Augmented, virtual and mixed reality in dentistry: a narrative review on the existing platforms and future challenges. Appl Sci. 2022;12(2):877.
6. Jiang F, Jiang Y, Zhi H, et al. Artificial intelligence in healthcare: past, present and future. Stroke Vasc Neurol. 2017;2(4):230-243.
7. Breitman LS, Ba AK, Van Doren EJ, Lee JE. A call-to-action: addressing the technological gap in predoctoral dental education. Harvard Medical Student Review. May 22, 2020. https://www.hmsreview.org/covid/addressing-the-technological-gap-in-predoctoral-dental-education. Accessed August 3, 2022.
8. Sharma D, Malik G, Koshy G, et al. Artificial intelligence: need to reboot dental education. Univ J Dent Sciences. 2021;7(2):138-142.
9. Wolcott MD, Shazib M, Cromartie J, et al. Responding to emerging oral healthcare needs with CARE: Design of the CARE curriculum model. J Dent Educ. 2022 May 26. doi: 10.1002/jdd.12959.
10. Yüzbaşıoğlu E. Attitudes and perceptions of dental students towards artificial intelligence. J Dent Educ. 2021;85(1):60-68.
11. Commission on Dental Accreditation. Accreditation Standards For Dental Education Programs. Chicago, IL: CODA; August 6, 2021. https://coda.ada.org/~/media/CODA/Files/predoc_standards.pdf?la=en. Accessed September 6, 2022.
12. Oral Health in America: Advances and Challenges. Bethesda, MD: US Dept of Health and Human Services, National Institutes of Health, National Institute of Dental and Craniofacial Research; 2021.
13. AiDENTAL. https://www.aidental.app/. Accessed September 11, 2022.
14. Carr AB, Brown DT. McCracken's Removable Partial Prosthodontics. 13th ed. St. Louis, MO: Elsevier; 2016.
15. Phoenix RD, David DR, DeFreest CF. Stewart's Clinical Removable Partial Prosthodontics. 4th ed. Chicago, IL: Quintessence Publishing; 2008.
16. Stratton RJ, Wiebelt FJ. An Atlas of Removable Partial Denture Design. Quintessence Publishing; 1988.
17. Balaban C, Inam W, Kennedy R, Faiella R. The future of dentistry: how AI is transforming dental practices. Compend Contin Educ Dent. 2021;42(1):14-17.
18. Islam NM, Laughter L, Sadid-Zadeh R, et al. Adopting artificial intelligence in dental education: a model for academic leadership and innovation. J Dent Educ. 2022 July 3. doi: 10.1002/jdd.13010.