Association Between Preventive Dental Care and Healthcare Cost for Enrollees With Diabetes or Coronary Artery Disease: 5-Year Experience
Bijan J. Borah, PhD; Solomon G. Brotman, DDS, MAGD; Ruchita Dholakia, MS, MBA; Stephanie Dvoroznak; Mark T. Jansen, MD; Edward A. Murphy, MBA; and James M. Naessens, ScD
Abstract: Background: Evidence of preventive dental care impacting healthcare costs among diabetes or coronary artery disease (CAD) patients is sparse. Methods: This study examined the association between healthcare costs and adherence with preventive dental care protocols among diabetes and CAD patients in a dental plan affiliated with a large commercial health plan in Arkansas. These patients were auto-enrolled in a program with additional benefits at no cost, and support from medical and dental care management teams was evaluated. All-cause cost was defined as the total amount paid by the health plan. Results: Adherence with preventive dental care was associated with significant average yearly cost savings. The ranges of these savings were progressively higher for patients with only diabetes ($515 to $574), only CAD ($548 to $675), and CAD + diabetes ($866 to $1,718). Most of these savings originated in costs associated with inpatient admissions, which were between 25% and 36% for all disease classifications for all years. Conclusions: Preventive dental care is strongly associated with significant savings for diabetes and CAD patients, and such savings were highest for diabetes + CAD patients, followed by patients with only CAD and only diabetes. Practical Implications: Health plans should include dental coverage in their benefits package and incentivize adherence with preventive dental care to improve health and lower costs for enrollees with diabetes and CAD.
Studies have shown that periodontal disease is associated with some chronic diseases, and its presence can aggravate other conditions. Individuals with type II diabetes are three times as likely to develop periodontal disease.1 A two-way relationship between periodontitis and diabetes has been shown in several longitudinal studies; however, the effects of preventive dental treatments on diabetes control are not clearly defined.1-4 Meanwhile, researchers have found associations between periodontal disease and coronary artery disease (CAD).5,6 Although periodontal interventions reduce systemic inflammation and endothelial dysfunction in short-term studies, there is no evidence that they prevent atherosclerotic vascular disease or modify its outcomes.7
One aspect of medical care that patients cannot control is their need to use inpatient services. Hospital admissions, being emergent in nature or requiring pre-authorization, both are non-elective and must meet standardized pre-authorization requirements for utilization. Further, the selection for hospital admission is blind to a patient's dental condition or past dental experience. In contrast, people may elect to have physician visits or be compliant with medication protocols, including preventive dental care. This bias for or against preventive and active healthcare is often cited as a contributing factor to healthcare costs.
To the best of the authors' knowledge, no prior published studies have quantified the association between healthcare costs and adherence with preventive dental care on healthcare costs of patients with diabetes and/or coronary disease. As such, the authors' objective was to evaluate the impact, if any, of adherence with preventive dental care on healthcare costs. Preventive dental care for the purposes of this study includes all procedures traditionally referred to as prophylaxis, periodontal maintenance, and nonsurgical procedures of scaling and root planing.
Methods
Data Source
Claims data for patients enrolled between 2014 and 2018 in health and dental plans administered by a large commercial health plan in the state of Arkansas was used in this study. The sample included men and women aged ≥18 years with diabetes, CAD, or both (diabetes + CAD cohort) as identified by the relevant Episode Treatment Group (ETG 163000 for diabetes and ETG 386500 for CAD) who were auto-enrolled in the Dental Xtra℠ (DX) program, which is described below.8 All individuals maintained fully insured medical and dental coverage with Arkansas BlueCross BlueShield (ABCBS) as their primary carrier for at least one complete calendar year from 2014 to 2018.
Dental Xtra℠ Program Overview
ABCBS has offered Dental Xtra, a branded dental service program, to eligible individuals since 2014 with Life and Specialty Ventures (LSV) as its dental affiliate. Patients with diabetes or CAD subscribing to both health and dental insurance from ABCBS were auto-enrolled into the DX program. This medical-dental integrated program provided the additional dental benefits at no cost to the patient. These benefits do not apply to the patient's calendar year maximum. Preventive dental visits refer to cleaning or nonsurgical periodontal treatment (CDT D1110, D4341, D4342, D4355, and D4910). For the general population, CDT codes D1110 and D4910 are covered at 100% for up to two per year under the dental insurance plans. The other codes are covered at 80%, subject to an annual deductible. In the DX program, the deductible and co-insurances are waived, and two additional D1110 or D4910 are paid at 100% and do not apply to the annual maximum allowable benefits. The patient is reminded and prompted of the need for ongoing preventive dental care through various modalities, including but not limited to their medical case management team and direct mail from the DX team.
Dentists are provided with a list of their attributed patients eligible for the benefits for additional contact every quarter in addition to the patient eligibility section of the online provider portal. Eligible enrollees were required to have continuous enrollment in the health plan during the period of study inclusion.
Adherence with the DX program: A patient was considered adherent to the DX program if he or she had at least one preventive dental visit every year of study enrollment ("Adherence Type 1"). Besides this primary adherence definition, the authors also assessed two other adherence types:"Adherence Type 0" = no preventive dental visits in any year of study enrollment. "Adherence Type V" = patients with variable ("V") adherence; for greater statistical sensitivity, the population who had at least 1 year with a preventive dental visit and at least 1 year with no preventive dental visit during enrollment was studied; this population demonstrated inconsistent or variable adherence to the recommended dental protocol. (Results are elaborated in Appendix Table A1 through Table A5.) For the variable adherent group, patients had to be continuously enrolled in the health plan for at least 3 years.
Patient Characteristics
The claims database provides information on the geographic location of the patients within the state of Arkansas, along with age and gender. It should be noted that insurance companies do not capture data on race and income; therefore, that data was not available for this study's sample.
Study Outcomes
The primary outcome was health-plan paid all-cause total yearly healthcare cost. Secondary outcomes were components of total yearly healthcare costs: outpatient, inpatient, and prescription medication costs. Cost was analyzed separately for patients with different lengths of continuous enrollment by compliance type and disease type (diabetes, CAD, and diabetes + CAD). Costs were inflation-adjusted to 2018 using the GDP price index.9
Statistical Analysis
Descriptive statistics for the patient characteristics, including frequencies and percentages for the categorical variables and mean, median, standard deviation (SD), first and third quartile (Q1 and Q3), and range for continuous variables, were provided for the overall cohort and for the specific disease subcohorts (diabetes, CAD, diabetes + CAD) separately. Mean and SD of costs were reported for different continuous enrollment lengths by adherence type and disease type.
Multivariate adjustment for patient characteristics was made through generalized linear modeling (GLM). Given that healthcare cost data is known to be skewed, GLM models with gamma distribution for costs with logarithmic link function is the appropriate multivariate adjustment approach.10 Predicted mean cost from the multivariate adjustment was reported for each compliance type within each disease group, along with their difference, and for patient cohorts with different enrollment lengths.
Given that the study used deidentified healthcare claims data, an institutional review board approval was not required. All the analyses were done using Stata 16.0 (StataCorp LLC, stata.com).
Results
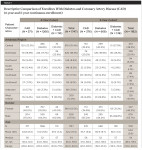
The number of unique patients with 5-, 4-, 3-, 2-, and 1-year continuous enrollment in the insurance plan were 1,182, 1,747, 1,959, 2,652, and 4,194, respectively (Figure 1). Each cohort was treated as an independent sample, with enrollees counted in only one cohort. Primary focus was on the 5- and 4-year cohorts (Table 1), while the relevant results for the other three cohorts (3-, 2-, and 1-year cohorts) are presented in Appendix Table A1, compendiumlive.com/go/cced1999. For the 5-year cohort, of the 1,182 eligible patients, 668 (57%) had diabetes, 376 (32%) had CAD, and 138 (12%) had both diabetes and CAD. For the 4-year cohort, which had 1,747 patients in total, the corresponding sizes for diabetes, CAD, and diabetes + CAD subcohorts were 1,266, 371, and 110, respectively. The mean age was 53 for the 5-year cohort and 52 for the 4-year cohort. Diabetes patients were relatively younger than those with CAD alone (51 vs 56 in 5-year cohort; 51 vs 55 in 4-year cohort) and those with both diabetes and CAD (51 vs 56 in 5-year cohort; 51 vs 57 in 4-year cohort). The proportion of females was 46% and 53%, respectively, in the 5- and 4-year cohorts. As indicated in Table 1, patients in the sample were geographically diverse within the state of Arkansas, with enrollees from the Central and Northeast regions of the state comprising 58% and 54% of the study population in the 5- and 4-year cohorts.
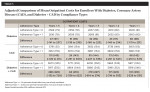
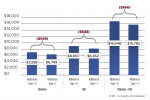
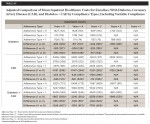
Figure 2 presents the adjusted costs for the three disease categories by Adherence Type 1 (adherent vs non-adherent) and the estimated cost savings for the 5-year cohort. Table 2 provides the same for all five cohorts, adjusting for differences in patient characteristics described above. The corresponding sample sizes for each of the subcohorts defined by disease category, adherence type, and years of continuous enrollment are presented in Appendix Table A2. For Adherence Type 1, adherent patients incurred significantly less all-cause costs across the three disease cohorts and for all of the five continuous enrollment length categories (Table 2). These cost savings for adherent patients ranged from $515 to $574 for diabetes patients, $548 to $675 for CAD patients, and $866 to $1,718 for diabetes + CAD patients depending on their enrollment lengths.
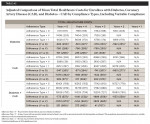
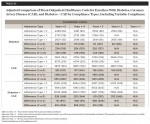
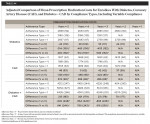
Secondary outcomes or the components of total costs, including outpatient cost, prescription medication cost, and inpatient cost, are presented in Table 3, Table 4, and Table 5. In general, outpatient costs did not differ by adherence type.
Adherent and non-adherent patients did not differ in terms of their prescription medication costs across the three disease cohorts and across different follow-up durations. Another contrasting trend from the total cost that the prescription medication cost exhibited was that the difference in prescription medication costs between adherent and non-adherent patients was not statistically significant.
As seen from Table 5, inpatient costs appear to closely mirror total costs (Table 2) in that adherent patients overall had significantly lower costs compared to their non-adherent peers according to adherent definitions. Nevertheless, it is clear from Table 2 and Table 5 that most of the healthcare cost savings came from savings in inpatient admission costs.
Appendix Table A2 through Table A5 also display adjusted mean cost between different adherence types. Overall, patients that were adherent as per the primary adherence definition in this study (Adherence Type 1) saved significantly more in total healthcare costs than patients with zero or variable adherences (Adherence Types 0 or V).
Discussion
The results suggest that adherence with preventive dental care is strongly associated with significantly lower healthcare costs. Average healthcare cost savings were progressively higher for patients with diabetes, CAD, and diabetes + CAD. The annual cost to the dental insurance affiliate for the procedures required for adherence, which includes the treatment covered at 100%, was $105 per adherent person per year (from proprietary Life and Specialty Ventures data). Auto-enrollment was key to this study, as it eliminated potential biases of participation, and in the implementation of the program, as it reduced barriers to patients who might not be able to navigate entry to DX. Further, patient adherence increased each year of the study period. Thus, a key takeaway is that health plans can generate significant healthcare cost reduction by providing dental coverage for their patients with diabetes and CAD; moreover, such benefits can be amplified if health plans institute programs to improve adherence to preventive dental care.
This study involved dental procedures that were provided to patients at no cost by a network of dentists that provided utmost convenience for the patient population. In the state of Arkansas, 87.4% of actively practicing dentists participated in the ABCBS Paycheck Protection Program (PPP) (range 83.9% to 92%) during this period.11 While there is no absolute method to eliminate barriers to care or socioeconomic factors, patients had a wide selection of dentists and locations to provide geographic and scheduling convenience.
These findings indicate a reduction in healthcare costs in the last 2 years of the study period. This can be ascribed to reductions in hospital payments that occurred after the Affordable Care Act.12 The health plan from which the data for this study was used reported these payment adjustments in 2017 and 2018, which is reflected in lower trending costs for all adherence groups, when compared to the first 3 years of the study. Irrespective of the change in payment per procedure and admission, the medical cost and inpatient savings remained constant on a percentage basis.
These results are consistent with the few studies previously reported. Jeffcoat and colleagues reported significant savings for people with follow-up dental care among both those with type 2 diabetes and those with CAD who also had periodontal disease.13 They found annual savings of $2,890 and $1,040 for the two groups, respectively. A recent study that assessed the relationship between periodontal interventions (any visit with CPT-4 codes D4000-D4999 in 2 years) and healthcare costs and utilization among patients with type 2 diabetes in an integrated dental, medical, and pharmacy commercial claims database found similar cost savings as the present study: $1,799 for 2-year follow-up versus approximately $750 per year for this study.14,15 Lamster et al recently reported similar inpatient cost savings in an 18-month study of New York state Medicaid data using different inclusion criteria.14
When the commercial insurance company in Arkansas from which data for this study was derived entered the Medicare Advantage (MA) programs in 2021, it was revealed that 29% of the MA patients could be eligible for DX benefits that would result in healthcare cost reductions (Life and Specialty Ventures proprietary data).Other state plans report that up to 48% of their Medicare insured patients have CAD or diabetes.If Medicare participants experience similar adherence savings to those observed in this study, similar adherence rates among Medicare patients could result in program savings sufficient to cover the preventive dental treatment costs.
The finding that the cost savings from preventive dental care come primarily from inpatient costs was supported indirectly by earlier findings that the receipt of dental care is associated with reduced diabetes-related healthcare utilization, including hospitalization and emergency department visits.16 At the same time, regular tooth scaling was found to be associated with a significant reduction in cardiac events that are often treated in inpatient settings.17
This study also underscores the importance of promoting medical-dental integration, particularly in the context of caring for patients with chronic conditions, such as diabetes and CAD, that have been shown to be associated with periodontal care.18-20 Furthermore, the benefits of preventive dental care likely are not restricted to just diabetes and coronary artery disease. Studies have shown associations between periodontitis and cerebrovascular disease or pregnancy, which are some of the other conditions eligible for Dental Xtra enrollment.13,21,22 The findings have clearly demonstrated that access to dental benefits and adherence with preventive dental care results in lower healthcare utilization leading to significantly lower healthcare costs that may be applicable to the general population. Of course, this study also brought to the fore the issue of non-adherence in the freely available dental care, which needs to be reviewed separately in follow-up research.
Adherence definitions that are easy to understand, clinically valid, and easy to implement by health plans were adopted. The evidence of overall cost savings is borne out by similar findings within the adherence definitions. Although not statistically significant, an interesting finding was that the inconsistently adherent group was costlier than the non-adherent group. Because many hypotheses could explain this difference, this finding needs further evaluation, including potentially patient interviews in a future study.
Study Strengths and Limitations
To the authors' knowledge, this is one of very few studies that have quantified the financial impact of preventive dental care on overall healthcare costs among patients with diabetes and/or CAD. More specifically, the cost savings for up to 5 years for two of the disease cohorts, diabetes and CAD, were quantified, where there is extant evidence documenting associations between these conditions and preventive dental treatments.1-6 The findings have broad generalizability as the commercial insurance company from which this study's data was derived is the largest commercial health plan in Arkansas, with approximately 42% market share in the state.23 This patient population is probably not very different from other commercially insured populations in the country, and therefore these findings can be expected to be valid for other commercially insured populations in the United States as well. The study isolated cost savings to non-elective activities, eliminating patient biases and tendencies from the potential healthcare cost savings. Further, hospital admissions are emergent in nature, require pre-authorization based on specific criteria in which the patient's dental adherence status is unknown, or both.
One key limitation of the study is that it is based on retrospective claims data that is primarily used for health plan administration purposes, including reimbursement, and such data lacks clinical detail. However, this is a typical and well-recognized limitation of any claims-based study; at the same time, as already noted above, this claims-based study brings forth real-world evidence. Additionally, the study evaluated only all-cause cost but not disease-related cost and addresses the important policy question as to whether preventive dental care is associated with all-cause healthcare cost savings or not. Defining costs related to specific diseases in claims data can be non-trivial, and the authors hope to pursue this, as well as the impact of comorbidities, in a future study.
A study based on the effects of adherence rather than the provision of dental benefits could be another potential limitation of this study. Although the assessment of the effect of offering free dental benefits to enrollees with diabetes, CAD, or other chronic diseases, or the effects of the integrated DX program, would be informative, the authors felt that practical and ethical issues would prevent a successful clinical trial where additional dental benefits were offered only to the enrollees in the intervention arm. The conclusions are strengthened by consistent effects across multi-year cohorts and the two disease cohorts, as well as the cost-savings impact resulting primarily from unanticipated hospital costs.
Disclosure
This study was partially funded by Life and Specialty Ventures through a research grant to Mayo Clinic. The study sponsor, however, did not play a role in the design and conduct of the study, analysis, interpretation of the data, and preparation of the manuscript. The data for the study was provided to the authors by Arkansas BlueCross BlueShield. Institutional review board approval was not required since the data used was deidentified.
About the Authors
Bijan J. Borah, PhD
Professor of Health Services Research, Mayo Clinic College of Medicine and Science;Robert D. and Patricia E. Kern Endowed Scientific Director, Health Services and OutcomesResearch Program, Center for the Science of Health Care Delivery, Rochester, Minnesota
Solomon G. Brotman, DDS, MAGD
Clinical Instructor, Department of Neural and Pain Sciences, University of Maryland School of Dentistry, Baltimore, Maryland; Vice President, National Clinical Operations, Life and Specialty Ventures, Jacksonville, Florida; Private Practice, Jacksonville, Florida
Ruchita Dholakia, MS, MBA
Principal Health Services Analyst, Mayo Clinic, Center for the Science of Health Care Delivery, Rochester, Minnesota
Stephanie Dvoroznak
Program Director, Dental4Health, Life and Specialty Ventures, Jacksonville, Florida
Mark T. Jansen, MD
Chief Medical Officer, Arkansas BlueCross BlueShield, Little Rock, Arkansas
Edward A. Murphy, MBA
President, Life and Specialty Ventures DM, LLC, Little Rock, Arkansas
James M. Naessens, ScD
Consultant, Mayo Clinic, Center for the Science of Health Care Delivery,
Rochester, Minnesota
References
1. Llambes F, Arias-Herrera S, Caffesse R. Relationship between diabetes and periodontal infection. World J Diabetes. 2015;6(7):927-935.
2. Bascones-Martinez A, Gonzalez-Febles J, Sanz-Esporrin J. Diabetes and periodontal disease. Review of the literature. Am J Dent. 2014;27(2):63-67.
3. Preshaw PM, Alba AL, Herrera D, et al. Periodontitis and diabetes: a two-way relationship. Diabetologia. 2012;55(1):21-31.
4. Teeuw WJ, Gerdes VE, Loos BG. Effect of periodontal treatment on glycemic control of diabetic patients: a systematic review and meta-analysis. Diabetes Care. 2010;33(2):421-427.
5. DeStefano F, Anda RF, Kahn HS, et al. Dental disease and risk of coronary heart disease and mortality. BMJ. 1993;306(6879):688-691.
6. Lockhart PB, Bolger AF, Papapanou PN, et al. Periodontal disease and atherosclerotic vascular disease: does the evidence support an independent association?: a scientific statement from the American Heart Association. Circulation. 2012;125(20):2520-2544.
7. Sanz M, Del Castillo AM, Jepsen S, et al. Periodontitis and cardiovascular diseases. Consensus report. Glob Heart. 2020;15(1):1.
8. Symmetry® Episode Treatment Groups®. Measuring health care with meaningful episodes of care. Eden Prairie, MN: Optum; 2020. https://www.optum.com/content/dam/optum3/optum/en/resources/white-papers/Symmetry_ETG_White_Paper_Analytics_815.pdf. Accessed January 24, 2022.
9. Bureau of Economic Analysis. GDP Price Index. BEA website. 2021. https://www.bea.gov/data/prices-inflation/gdp-price-index. Accessed March 17, 2021.
10. Manning WG, Basu A, Mullahy J. Generalized modeling approaches to risk adjustment of skewed outcomes data. J Health Econ. 2005;24(3):465-488.
11. Kaiser Family Foundation. State Health Facts: Professionally Active Dentists. KFF website. 2021. https://www.kff.org/other/state-indicator/total-dentists/?currentTimeframe=0&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D. Accessed October 10, 2021.
12. Dobson A, DaVanzo J, Haught R, Luu PH, American Hospital Associaton. Estimate of Federal Payment Reductions to Hospitals Following the ACA 2010-2028: Estimates and Methodology. Dobson DaVAnzo & Associates, LLC: Vienna, VA; 2018. https://www.aha.org/system/files/2018-06/estimate-of-fed-payment-reductions-to-hospitals-following-aca-2010-2018-report.pdf. Accessed January 24, 2022.
13. Jeffcoat MK, Jeffcoat RL, Gladowski PA, et al. Impact of periodontal therapy on general health: evidence from insurance data for five systemic conditions. Am J Prev Med. 2014;47(2):166-174.
14. Lamster IB, Malloy KP, DiMura PM, et al. Dental services and health outcomes in the New York State Medicaid program. J Dent Res. 2021;100
(9):928-934.
15. Nasseh K, Vujicic M, Glick M. The relationship between periodontal interventions and healthcare costs and utilization. Evidence from an integrated dental, medical, and pharmacy commercial claims database. Health Econ. 2017;26(4):519-527.
16. Mosen DM, Pihlstrom DJ, Snyder JJ, Shuster E. Assessing the association between receipt of dental care, diabetes control measures and health care utilization. J Am Dent Assoc. 2012;143(1):20-30.
17. Chen ZY, Chiang CH, Huang CC, et al. The association of tooth scaling and decreased cardiovascular disease: a nationwide population-based study. Am J Med. 2012;125(6):568-575.
18. Atchison KA, Weintraub JA, Rozier RG. Bridging the dental-medical divide: case studies integrating oral health care and primary health care. J Am Dent Assoc. 2018;149(10):850-858.
19. Mosen DM, Banegas MP, Dickerson JF, et al. Examining the association of medical-dental integration with closure of medical care gaps among the elderly population. J Am Dent Assoc. 2021;152(4):302-308.
20. Nasseh K, Greenberg B, Vujicic M, Glick M. The effect of chairside chronic disease screenings by oral health professionals on health care costs. Am J Public Health. 2014;104(4):744-750.
21. Munoz Aguilera E, Suvan J, Orlandi M, et al. Association between periodontitis and blood pressure highlighted in systemically healthy individuals: results from a nested case-control study. Hypertension. 2021;77(5):1765-1774.
22. Seitz MW, Listl S, Bartols A, et al. Current knowledge on correlations between highly prevalent dental conditions and chronic diseases: an umbrella review. Prev Chronic Dis. 2019;16:E132.
23. 2018 Market Share Reports: For the Top 125 Accident and Health Insurance Groups and Companies by State and Countrywide.Washington, DC: National Association of Insurance Commissioners; 2019.