Simultaneous Crestal Sinus Elevation and Implant Placement Using a Ribose Cross-Linked, Collagen Bone Graft Material: Case Series of 28 Consecutive Patients
Barry P. Levin, DMD; and Sergio Rubinstein, DDS
Abstract: The anatomic proximity of the maxillary sinus to the apices of molar and premolar teeth is a significant factor when considering implant therapy to replace maxillary posterior teeth. An emerging field within tissue engineering is the application of xenografts capable of stimulating de novo bone regeneration. This article presents a technique using a crestal approach to sinus grafting utilizing a novel bone graft material composed of porcine, ribose cross-linked collagen seeded with a nanocrystalline hydroxyapatite mineral. This highly cohesive biomaterial is able to minimize graft migration, which is particularly important in case of undetected Schneiderian membrane perforations. The material also has been demonstrated in animal studies to be capable of osteoconduction, resulting in increased bone volume in ridge augmentation procedures.
Implant therapy aimed at replacing posterior maxillary teeth presents clinicians the challenge of contending with the maxillary sinus. The anatomic proximity of the antral floor to the apices of molar and premolar teeth in most adults is a significant consideration.1 Even if implants are placed simultaneous with extraction, there may be limited bone volume between the base of an extraction socket and the sinus. In cases where posterior teeth are already missing, the height of bone available for implant placement is often suboptimal, and this is fairly typical when the width of bone is deficient as well. It has been demonstrated that the need for sub-antral bone grafting to facilitate implant therapy is common.2
This circumstance has led to many proposed procedural variations by surgeons to elevate the antral floor to regenerate bone and accommodate implant placement. Originally, Boyne and James presented the open or lateral window technique, a procedure that included autogenous bone grafting and had significant morbidity.3 Summers introduced a crestal approach utilizing specially designed osteotomes as a more conservative alternative to a lateral window osteotomy and modified Caldwel-Luc procedure.4 This method is often selected when at least 4 mm to 6 mm of bone height remains.
The application of graft materials beneath the elevated sinus lining and osseous walls is frequently performed. The osteogenic, osteoconductive, or osteoinductive properties of the graft depend on its physical and chemical composition. While autogenous bone for sinus grafts was once considered to be the "gold standard," studies have shown effectiveness of allografts,5,6 xenografts,7 and recombinant growth factors.8 An animal study demonstrated increased bone-to-implant contact in sinus grafts when autogenous bone or autogenous bone mixed with xenograft was compared to xenograft alone.9 Conversely, Lee et al demonstrated predictable bone formation with xenograft alone for sinus elevations in a human, histomorphometric trial.10 Another valuable property of these grafts is the physical space created for chemotaxis of osteoprogenitor cells necessary for de novo bone formation. Sinus elevations are predictable procedures, although infections have been reported in the literature.11
An emerging field within tissue engineering is the application of xenografts capable of stimulating de novo bone regeneration. In animal studies and human case reports, collagen-based grafts cross-linked with ribose have demonstrated the ability to serve as a nidus for direct bone formation.12-14 These studies and reports demonstrate direct bone formation or "ossification" of collagen membranes placed over particulate bone grafts in the application of guided bone regeneration (GBR). In addition to acting as a cell-exclusionary membrane, this collagen material can be manipulated in terms of the level of cross-linking and density to serve other purposes. One such material is a scaffold seeded with nanosized particles of synthetic, crystalline, non-sintered hydroxyapatite (HA). The embedded HA particles do not sterically influence the "honeycomb" structure of the material. The ratio (by weight) of HA to cross-linked collagen is 80:20. This mineral adds an osteoconductive element to the cross-linked collagen. The porosity of the material allows for vascularization of the implanted material and "seeding" of the graft by osteoprogenitor cells.
This article presents a technique using a crestal approach to sinus grafting, utilizing a novel bone graft material composed of porcine, ribose cross-linked collagen seeded with a nanocrystalline HA mineral. This biomaterial is more cohesive than particulate bone grafts, minimizing graft migration, especially in cases of undetected Schneiderian membrane perforations, which suggests improved safety. Because the human body naturally cross-links collagen with ribose, this mechanism of cross-linking does not elicit a foreign-body response. The graft utilized in this case series, made of porcine tendon, is purified and cross-linked with a proprietary technology (Glymatrix® Technology, Datum Dental, datumdental.com) that allows the graft to resist early enzymatic degradation and support substitution with viable bone. The graft is then seeded with nanoscale particles of HA. The material also has been demonstrated in animal studies to be capable of osteoconduction, resulting in increased bone volume in ridge augmentation procedures.15
In a cadaver study, Reiser demonstrated a 24% incidence of Schneiderian membrane perforation using a crestal approach.16 The study showed that the increase in height of elevation using osteotomes resulted in a higher percentage of membrane perforation. Therefore, incorporation of a bone graft with cohesive properties that is less likely to migrate into the sinus in the event of an undetected perforation of the Schneiderian membrane may be efficacious.
Methods and Materials
Twenty-eight patients were treated in the author's (BPL) private periodontal practice. All of them signed informed consent forms for surgery, and all patients were made aware that they would be receiving a porcine-based xenograft. Each patient required replacement of one or more maxillary posterior teeth. The teeth being replaced either were extracted and the sockets grafted to preserve ridge height and/or width to facilitate delayed implant placement or underwent immediate implant placement at time of extraction, as per Al-Maseeh classification, class 1 through class 4.17 The distribution of sites based on this classification were as follows: class 1, four sites; class 2, two; class 3, three; class 4, 19.
Extraction sites where immediate implant placement was not performed were grafted with a mineralized allograft (freeze-dried bone allograft [FDBA]) (Symbios®, Dentsply Sirona, dentsplysirona.com) and a collagen membrane (either Ossix® Plus, Datum Dental; or Symbios PerioDerm, Dentsply Sirona). Reasons why immediate placement was not performed in these situations included active, purulent infection; anatomic limitations, such as root proximity and lack of septal bone for primary stability; or severely pneumatized maxillary sinuses. These sites were re-entered at approximately 4 to 6 months for implant placement.
Following standard drilling protocols suggested by the manufacturer, but stopping at least 1 mm below the sinus floor, one of two methods was taken: either a rotary approach (Sinus Crestal Approach [SCA] Kit, Hubermed, hubermed.com) with specialized drills and stops was used to reach the Schneiderian membrane, or conventional osteotomes (Astra Tech, Dentsply Sirona) were utilized to perform elevation of the membrane. Zhou et al demonstrated the efficacy of using the rotary drills and stoppers.18 Efforts were made to avoid entry of instrumentation beyond the original floor of the sinus.
A ribose, cross-linked collagen graft seeded with nanocrystalline HA (Ossix® Bone, Datum Dental) was hydrated in either sterile saline or the patient's blood, and then cut into smaller increments with a 15C scalpel blade. The pieces of graft were to be placed into the osteotomy and gently advanced under the sinus membrane manually. Typically, a single implant site required between 0.125 cc and 0.25 cc of graft material. Prior to implant insertion, a large, ball-tipped probe was used to gently confirm a palpable stop, consisting of the graft material. Implants were then placed at the bone crest in the prosthetically determined position.
In immediately implanted sites, multirooted teeth were sectioned and extracted, with the intraradicular septum of bone intentionally preserved. From this point, identical preparation as previously described was performed. No intentional compression or bone spreading to widen this septal bone was done, nor was there any attempt to increase the trabecular density to aid in achieving primary stability. The residual space between the implants and socket walls was grafted with either the same collagenated bone graft or particulate bone and collagen membranes used as described in the socket grafting steps.
In both immediate and delayed sites a transmucosal healing approach was selected. Two sample cases are presented that describe and illustrate the technique.
Clinical Examples
Case 1
The first example is of a 40-year-old, nonsmoking male patient who presented needing extraction of multiple teeth due to endodontic failures. The treatment plan for this patient included comprehensive orthodontic therapy after the extractions. The sites of future implant placement were augmented with FDBA and collagen barriers (Ossix Plus). Tooth No. 14 was extracted and augmented.
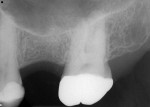
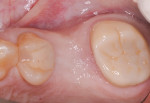
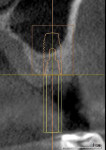
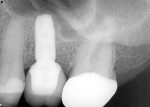
Approximately 26 months after extraction and grafting, orthodontic treatment was completed and the patient returned for implant placement (Figure 1 and Figure 2). A cone-beam computed tomography scan (CBCT) revealed adequate preservation of the buccal-palatal ridge dimensions but inadequate bone height from the crest to the floor of the maxillary sinus (Figure 3).
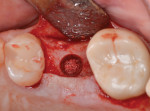
Following full-thickness flap reflection, the osteotomy preparation included use of rotary drills with stops to prevent sinus preparation and specialized drills to protect the membrane from trauma (SCA Hubermed). The collagenated bone graft was hydrated in sterile saline (Figure 4), sectioned as described above, and placed into the osteotomy incrementally. The material could be gently palpated to confirm it had not been displaced into the maxillary sinus (Figure 5).
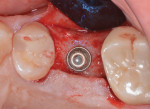
A 4.8 mm x 11 mm implant (Astra Tech EV, Dentsply Sirona) was placed with primary stability at the level of the crestal bone (Figure 6). A healing abutment was placed, and transmucosal healing was selected. The space beneath the Schneiderian membrane, which was filled with the bone graft, could be easily discerned radiographically (Figure 7).
At the 6-week follow-up appointment, the site appeared clinically healthy. A periapical radiograph demonstrated bone stability at the crest and increased radiopacity in the grafted sub-antral region (Figure 8).
The patient was referred back to his restorative dentist to begin abutment and crown fabrication at approximately 10 weeks post-surgery. He then returned for routine periodontal maintenance approximately 5 months after implant surgery. The site was healthy, presenting no probing depths greater than 3 mm and no inflammation (Figure 9). An x-ray demonstrated further remodeling of the grafted region, with less visible differentiation between the native bone and grafted bone (Figure 10). As of the time of this writing, which is more than 2 years since surgery was performed, the patient has not experienced any complications.
Case 2
The second example depicts a 71-year-old male patient who required rehabilitation of his maxillary right quadrant. Because of a severe root fracture, tooth No. 5 was extracted and the site was augmented as described previously. Due to unforeseen medical issues involving oncologic therapy, further treatment was delayed for about 3 years. Once medical clearance was obtained, the patient returned for extraction of teeth Nos. 2 and 3 and implant placement in the positions of teeth Nos. 3 and 5.
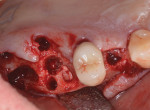
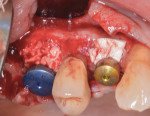
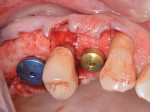
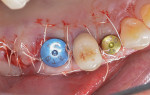
Following reflection of a full-thickness flap, teeth Nos. 2 and 3 were extracted. Osteotomy preparation was performed without modification in the No. 5 position. The intraradicular septal bone in the No. 3 area was prepared to about 1 mm apical to the antral floor. The same rotary preparation described previously was used in conjunction with the aforementioned cross-linked collagen bone graft to elevate the maxillary sinus (Figure 11). The same bone graft was utilized to obturate voids associated with the extraction socket of No. 3 and also over the thin (<1 mm) but intact bone crestally at the No. 5 implant site (Figure 12). A tissue punch was used to pierce a dermal allograft (Symbios PerioDerm) to allow it to be "draped over" two healing abutments and adapted over the socket walls and bone grafts (Figure 13). This material served as a collagen membrane for bone augmentation and as a means to increase peri-implant soft-tissue thickness.
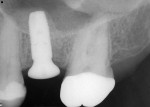
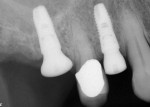
Next, the flaps were readapted for one-stage healing (Figure 14). The postoperative radiograph demonstrated the portion of the posterior implant stabilized by native, septal bone and the area occupied by the bone graft in the region of sinus elevation (Figure 15).
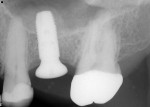
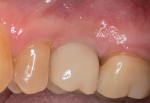
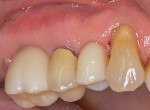
After approximately 12 weeks of healing, restorative treatment commenced. This consisted of fabrication of two screw-retained crowns on the implants in the Nos. 3 and 5 positions (Figure 16). As of the time of this writing, which is 2 years since surgery was performed and more than 18 months after the implants were restored, the patient has had no tenderness, peri-implant inflammation, or bone loss.
Discussion
The crestal approach for elevating the maxillary sinus at the time of implant placement has been used for more than 20 years with numerous methods of elevation being utilized. Although the procedure is considered safe, the potential for Schneiderian membrane perforation exists.19 Should a membrane perforation occur, it may not be detected as easily as with a buccal approach, due to limited visibility. Clinical signs such as fogging of intraoral mirrors may indicate violation of the sinus lining; however, once graft material is placed within the osteotomy, this fogging may not occur even though a perforation has happened. A perforation of the lining mucosa will increase the likelihood of graft migration and subsequent sinus infection. This is most concerning with a particulate bone graft, where small particles can be forced through minute perforations.
The use of a cohesive, collagen-based bone graft that is less likely to migrate in the event of a communication may be beneficial. Compared to a similar form of collagen/HA, the graft used in this case series demonstrated significantly less tendency for graft migration in animal ridge augmentation procedures. Also, the addition of collagen would be advantageous in terms of controlling hemorrhage into the sinus caused by surgical trauma. The graft used in this case series is comprised of a porcine, cross-linked collagen that is resistant to fragmentation and migration. This ribose cross-linking of collagen has demonstrated ossification.12,15 Radiographically, this case series demonstrated increased radiodensity and gradual trabecular pattern, suggestive of osseous substitution of the graft with de novo bone formation.
The replacement of maxillary posterior teeth may occur at different stages of therapy. When amenable to immediate placement, teeth can be extracted and simultaneous sinus elevation and implant placement performed in type 2 and type 3 scenarios.17 In clinical situations where teeth have been extracted and the natural healing processed has occurred, but at least 4 mm to 5 mm of residual bone height exists, type 1 placement can be performed. Often posterior extraction sockets are in close proximity to the floor of the maxillary sinus. When the surgeon determines that crestal elevation risks perforation of the lining membrane, the socket may be grafted to preserve bone height and width, and a type 4 sinus graft executed. Standard osteotomy drills are used in this situation, stopping 1 mm to 2 mm short of the inferior border of the sinus. At this point, a crestal elevation is performed as would be done with type 1 sinus grafts.
All four of these situations require some degree of crestal sinus elevation, utilizing a bone graft material for space maintenance and osteoconductivity functions. With the ribose cross-linked collagen bone graft demonstrated in this case series, safe, predictable sinus floor elevation can be performed to aid in simultaneous implant placement.
The use of bone grafting materials simultaneous with crestal sinus elevations is not universal. Researchers such as Taschieri et al found that crestal sinus lifts performed in conjunction with implant placement can be successful without the use of bone graft materials.20 However, they advocated the use of a platelet-derived growth factor clot, which served as what they referred to as a "cushion" to aid in Schneiderian membrane detachment with osteotomes. Others such as Nedir et al also have demonstrated the efficacy of implant placement simultaneous with crestal sinus elevation while omitting the use of a bone graft.21
The bone graft utilized in this case series served several purposes. First, it provided physical space for the regeneration of bone at the apical portion of implants placed simultaneous with crestal sinus elevation. Second, it provided the "cushion" Taschieri discussed,20 thereby adding an element of safety when detaching the Schneiderian membrane. Third, the presence of collagen may assist in controlling intraoperative hemorrhage caused by surgical trauma and aid in the cohesiveness of the graft, minimizing migration should an undetected membrane perforation occur.
Conclusion
Replacing maxillary posterior teeth in proximity of the sinus should be safe and predictable when augmentation is required. Although the ideal graft material has yet to be developed, bone grafts should be easy to manipulate, hemostatic, and capable of substitution with de novo bone. The collagen-based graft used in this case series possesses these qualities. Cross-linking with ribose is non-cytotoxic and facilitates osseous regeneration. The graft's cohesive nature prevents migration into the maxillary sinus, which is beneficial in case undetected violations of the Schneiderian membrane occur during surgery. Long-term studies are necessary to further validate its use in routine clinical practice.
Disclosure
The authors had no conflicts of interest to report.
About the Authors
Barry P. Levin, DMD
Clinical Associate Professor, University of Pennsylvania School of Dental Medicine; Private Periodontal Practice, Jenkintown, Pennsylvania
Sergio Rubinstein, DDS
Private Practice, Skokie, Illinois
References
1. Kopecka D, Simunek A, Brazda T, et al. Relationship between subsinus bone height and bone volume requirements for dental implants: a human radiographic study. Int J Oral Maxillofac Implants. 2012;27(1):48-54.
2. Nunes LS, Bornstein M, Sendi P, Buser D. Anatomical characteristics and dimensions of edentulous sites in the posterior maxillae of patients referred for implant therapy. Int J Periodontics Restorative Dent. 2013;33
(3):337-345.
3. Boyne PJ, James RA. Grafting of the maxillary sinus floor with auto-genous marrow and bone. J Oral Surg. 1980;38(8):613-616.
4. Summers RB. A new concept in maxillary implant surgery: the osteotome technique. Compendium. 1994;15(2):152-158.
5. Soardi CM, Spinato S, Zaffe D, Wang HL. Atrophic maxillary floor augmentation by mineralized human bone allograft in sinuses of different size: an histologic and histomorphometric analysis. Clin Oral Implants Res. 2011;22(5):560-566.
6. Gapski R, Neiva R, Oh TJ, Wang HL. Histologic analyses of human mineralized bone grafting material in sinus elevation procedures: a case series. Int J Periodontics Restorative Dent. 2006;26(1):59-69.
7. Froum SJ, Wallace S, Cho SC, et al. A histomorphometric comparison of Bio-Oss alone versus Bio-Oss and platelet-derived growth factor for sinus augmentation: a postsurgical assessment. Int J Periodontics Restorative Dent. 2013;33(3):269-279.
8. Nevins M, Kirker-Head C, Nevins M, et al. Bone formation in the goat maxillary sinus induced by absorbable collagen sponge implants impregnated with recombinant human bone morphogenetic protein-2. Int J Periodontics Restorative Dent. 1996;16(1):8-19.
9. Jensen T, Schou S, Gundersen HJ, et al. Bone-to-implant contact after maxillary sinus floor augmentation with Bio-Oss and autogenous bone in different ratios in mini pigs. Clin Oral Implants Res. 2013;24(6):635-644.
10. Lee DZ, Chen ST, Darby IB. Maxillary sinus floor elevation and grafting with deproteinized bovine bone mineral: a clinical and histomorphometric study. Clin Oral Implants Res. 2012;23(8):918-924.
11. Urban IA, Nagursky H, Church C, Lozada JL. Incidence, diagnosis, and treatment of sinus graft infection after sinus floor elevation: a clinical study. Int J Oral Maxillofac Implants. 2012;27(2):449-457.
12. Zubery Y, Goldlust A, Alves A, Nir E. Ossification of a novel cross-linked porcine collagen barrier in guided bone regeneration in dogs. J Periodontol. 2007;78(1):112-121.
13. Zubery Y, Nir E, Goldlust A. Ossification of a collagen membrane cross-linked by sugar: a human case series. J Periodontol. 2008;79(6):
1101-1107.
14. Levin BP, Zubery Y. Use of a sugar cross-linked collagen membrane offers cell exclusion and ossification. Compend Contin Educ Dent. 2018;
39(1):44-48.
15. Zubery Y, Goldlust A, Bayer T, et al. Alveolar ridge restoration using a new sugar cross-linked collagen-hydroxyapatite matrix in canine L-shaped defects. Orlando, FL: 2017 E-Poster Session. Academy of Osseointegration Annual Meeting. March 15-18, 2017.
16. Reiser GM, Rabinovitz Z, Bruno J, et al. Evaluation of maxillary sinus membrane response following elevation with the crestal osteotome technique in human cadavers. Int J Oral Maxillofac Implants. 2001;16(6):
833-840.
17. Al-Maseeh J, Levin B, Symeonides E. The osteotome technique: a classification for technique approach and clinical Case Seriess. Compend Contin Educ Dent. 2005;26(8):551-556.
18. Zhou X, Hu XL, Li JH, Lin Y. Minimally invasive crestal sinus lift technique and simultaneous implant placement. Chin J Dent Res. 2017;20(4):211-218.
19. Reiser GM, Rabinovitz Z, Bruno J, et al. Evaluation of maxillary sinus membrane response following elevation with the crestal osteotome technique in human cadavers. Int J Oral Maxillofac Implants. 2001;16(6):833-840.
20. Taschieri S, Corbella S, Saita M, et al. Osteotome-mediated sinus lift without grafting material: a review of literature and a technique proposal. Int J Dent. 2012. doi: 10.1155/2012/849093.
21. Nedir R, Nurdin N, Szmukler-Moncler S, Bischof M. Placement of tapered implants using an osteotome sinus floor elevation technique without bone grafting: 1-year results. Int J Oral Maxillofac Implants. 2009;24(4):727-733.