CAD/CAM Beyond Intraoral Restorations: Maxillofacial Implant Guide
Vinicus Machado, DDS, MSc; Filipe Jaeger, DDS, MSc, PhD; Carlos Bettoni Cruz de Castro, MSc; Elizabeth Rodrigues Alfenas, MSc, PhD; and Nelson R.F.A. Silva, DDS, MSc, PhD
Abstract: With a digital revolution impacting nearly all industries and disciplines, the incorporation of digital technologies into dental offices and laboratories appears to be inevitable. Highlighting the use of computer-aided design/computer-aided manufacturing (CAD/CAM) technology, this case report demonstrates the development of a maxillofacial prosthesis after creation of a 3-dimensional printed surgical guide to enable accurate and predictable implant positioning to enhance overall facial prosthetic retention and comfort for the patient. The management of lost craniofacial hard and soft tissues due to congenital abnormalities, trauma, or, in this case, cancer treatment poses a multifaceted challenge to not only oral and maxillofacial surgeons but also general dentists, prosthodontists, dental laboratory technicians, and other dental and medical professionals. CAD/CAM technology may be viewed beyond its use for teeth reconstructions and intraoral implants and become an important tool for success when implant-supported maxillofacial prosthetic components are needed.
As the digital revolution continues to permeate industry and medical disciplines, it seems certain that digital technologies will be increasingly adopted into dental offices and laboratories. Computer-aided design/computer-aided manufacturing (CAD/CAM) in dentistry, however, has thus far been linked to the production of intraoral components/restorations, along with 3-dimensional (3D)-printed surgical and endodontic guides. CAD/CAM's primary use has been constrained to the intraoral environment, mostly involving the treatment planning and design and manufacture of dental prosthetics, including both hard/soft-tissue-supported prostheses and dental implants.
3D-printed surgical guides, in particular, have been used successfully among both general practitioners and implant specialists. Nonetheless, very little attention has been given to implant-supported facial prosthetic rehabilitations after facial tumor removal.
The mutilation of a portion of a person's face has a major impact on his or her self-image and personality. When an eye has to be removed surgically the sensation of loss is psychologically very heavy, as this is an incredibly important organ used to function in everyday life. Therefore, depending on the size and scope of the loss, it may be necessary to create an ocular prosthesis or orbital prosthesis (eye and eyelid) for the rehabilitation of such a patient.1-5
Among dental professionals there is consensus that surgical guided processes using accurate cone-beam computed tomography (CBCT) imaging combined with 3D scanning technology has enabled general clinicians to capably perform intraoral implant therapies.6 With this in mind, it would seem that surgical guidance should be used for most dental implant treatments. Furthermore, CAD/CAM should be considered for use beyond teeth/intraoral implant reconstructions when, for instance, a maxillofacial prosthesis supported by implants is needed.
To operate in the craniomaxillofacial zone, a surgeon needs detailed information about the anatomy of the surrounding area. Use of digital imaging and software allows a computer to process a series of consecutive sectional images to generate multiplanar reconstruction views that provide surgeons insight into the anatomic structure. This allows for predictable and accurate implant positioning at selected locations on the face, following principles that are similarly employed for intraoral implant therapies in which the virtual planning is directly transferred to the drilling guide without loss of accuracy.7
This article discusses the innovative use of CAD/CAM technology beyond implant-supported or implant-retained dental prostheses through a case report in which a maxillofacial prosthesis was developed after a 3D-printed surgical guide was created. This approach allowed accurate and predictable implant positioning and placement aimed at improving the maxillofacial prosthetic retention.
Case Description
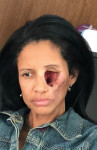
A 44-year-old female patient who had been diagnosed with squamous cell carcinoma had the tumor completely removed, which left her with a large facial deformity (Figure 1). A maxillofacial prosthesis retained by implants was treatment planned. Implant therapy was intended to enhance retention, comfort, and stability of the facial prosthesis.
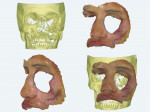
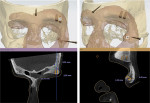
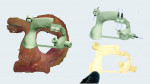
The postoperative treatment planning process started with a full-head CBCT (Figure 2, upper left) together with a 3D color facial scan using an intraoral scanner (TRIOS® 3, 3Shape A/S, 3shape.com) (Figure 2, upper right and lower left). CBCT and 3D facial scans were manually aligned (Figure 2, lower right). Subsequently, virtual implant positioning along with a surgical guide were created using CAD software (Implant Studio®, 3Shape).
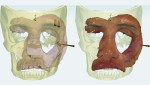
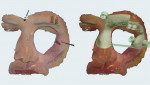
Three implants (NobelReplace Select, Nobel Biocare, nobelbiocare.com) were virtually planned. One was positioned at the upper aspect of the left zygoma, and two were positioned at the temporal bone in the supraorbital area (Figure 3). Anchor pins were located at the nasion and posterior aspect of the zygoma (Figure 4). A surgical guide (surgical mask) was designed to allow a fully guided process during implant placement (Figure 5). After the surgical guide design was completed, a standard tessellation language (STL) file was generated and sent to a 3D printer (SLA Form 2, Formlabs, formlabs.com) to manufacture the surgical guide. The final printed surgical guide is shown in Figure 6.
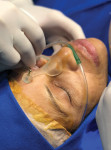
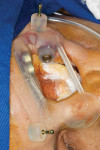
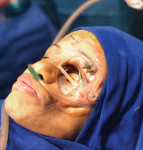
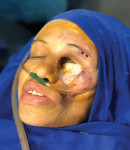
Implant surgical therapy using a guided surgical kit (Nobel Biocare) was performed with the patient under complete sedation (Figure 7 and Figure 8). A flapless approach was used (Figure 9 and Figure 10). After a 6-month healing process a maxillofacial prosthetic mask was developed and customized for the patient (Figure 11 and Figure 12).
For the fabrication of the facial prosthesis, the following treatment sequence was employed: facial record, decision on the mode of retention of the prosthesis, fabrication of the ocular component, location of the eyecup for sculpture, sculpture of the prosthesis, test drive onto the face, intrinsic painting of prosthetic material, pressing, polymerization, finishing, and extrinsic painting. Final outcome of the facial prosthesis is shown in Figure 13.
(To view a short video that shows the process of creating the surgical mask and demonstrates the precision of the implant planning and guided surgical approach, along with additional images of this case, scan the QR code below or go to https://compendiumlive.com/go/cced1883.)
Clinical Significance
Digital dentistry is an integral part of modern clinical practice given its numerous perceived advantages and improvements in efficiency and patient outcome predictability. Patients have also benefitted from shorter surgical times, less postoperative pain, enhanced clinical outcomes, and improved comfort. Moreover, novel and diverse dental technologies continue to improve aspects of diagnosis, treatment planning, and communication across the entire medical/dental team. Digital dentistry uses CAD/CAM production in many ways. The technology produces dental restorations that are hard- and soft-tissue supported as well as implant supported. The technology's impact via intraoral scanners, CAD software, and milling/printing units has already become an important part of routine clinical workflow in a global context. However, contemporary digital dentistry has now surpassed the initial concept of using CAD/CAM technology for only dental crowns and fixed partial dentures. As demonstrated in this report, the incorporation of face scanning using intraoral scanners combined with CBCT can result in a precise surgical mask that fits onto the patient's face before surgery, improving implant positioning predictability.
Digital scanners for dental applications record information by capturing images via a scanning device and camera. The camera component has been used mainly to record details of the intraoral condition or analog objects (eg, elastomeric impressions, stone models, etc).8 However, the use of intraoral scanners for recording facial details is not commonly recommended; instead, face scans can be utilized. In the present article, the authors used the intraoral scanner as a face scanner with proper stitchings between scans to subsequently align to the CBCT scans and develop the surgical guide mask. Considering, though, that the face scan process via intraoral scanning could be somewhat lengthy, technically sensitive, and complicated, the face scan presented here demonstrated that it is possible to scan face details via an intraoral scanner. Although the treatment plan for the implants was performed mostly digitally, the maxillofacial prosthesis was created using analog approaches, suggesting that this mechanism of prosthetic fabrication needs to be revisited and developed to attain a more digitally driven outcome to enhance reproducibility.
This case report demonstrates an approach that extends beyond teeth/implant reconstructions and into the development of a surgical mask to digitally guide implant positioning for the maxillofacial prosthetic created. It is important to emphasize that the management of lost craniofacial tissues due to congenital abnormalities, trauma, or cancer treatment poses a challenge to oral and maxillofacial surgeons.9 However, the utilization of a guided process can significantly help the post-cancer treatment workflow as shown in this article, thereby greatly reducing surgical time. Moreover, the increased precision attained with the CBCT aligned with the face scan (Figure 4) resulted in a predictable and precise surgical mask that enabled the surgeons to more readily position the implants.10
Conclusion
The use of CAD/CAM technology is advantageous for the production of facial prosthetic components supported by implants. Even if dentists and laboratories choose to continue working with analog methods, digital technology can still offer significant benefits by contributing to accurately produced 3D-guided alternatives.
Acknowledgment
The authors thank MaxilloFacialTips, Nobel Biocare, and SLICE Group - Belo Horizonte, Brazil, for support during treatment planning, surgery, and prosthesis design. Implant design support was given by 3Shape.
About the Authors
Vinicus Machado, DDS, MSc
Co-founder, SLICE Group, Belo Horizonte, Minas Gerais, Brazil
Filipe Jaeger, DDS, MSc, PhD
Oral and Maxillofacial Surgery Service, Hospital da Baleia - CENTRARE, Belo Horizonte, Minas Gerais, Brazil; Oral and Maxillofacial Surgery Service, Hospital Belo Horizonte - Minas Gerais, Brazil
Carlos Bettoni Cruz de Castro, MSc
Oral Pathologist, Implant Dentist, Oral and Maxillofacial Surgery, Hospital MaterDei and Lifecenter, Belo Horizonte, Minas Gerais, Brazil
Elizabeth Rodrigues Alfenas, MSc, PhD
Professor, Federal University of Minas Gerais (UFMG Brazil), Belo Horizonte, Minas Gerais, Brazil
Nelson R.F.A. Silva, DDS, MSc, PhD
Professor, Federal University of Minas Gerais (UFMG Brazil), Belo Horizonte, Minas Gerais, Brazil; Private Practice, Belo Horizonte, Minas Gerais, Brazil
References
1. Kale E, Meşe A, Izgi AD. A technique for fabrication of an interim ocular prosthesis. J Prosthodont. 2008;17(8):654-661.
2. Manvi S, Ghadiali B. Prosthetic rehabilitation of a patient with an orbital defect using a simplified approach. J Indian Prosthodont Soc. 2008;8(2):116-118.
3. Jebreil K. Acceptability of orbital prostheses. J Prosthet Dent. 1980;
43(1):82-85.
4. Guttal SS, Patil NP, Nadiger RK, et al. Use of acrylic resin base as an aid in retaining silicone orbital prosthesis. J Indian Prosthodont Soc.2008;
8(2):112-115.
5. Dholam KP, Pusalkar HA, Yadav P, Bhirangi PP. Implant-retained orbital prosthesis. J Indian Prosthodont Soc. 2008;8(1):55-58.
6. Almog DM, Torrado E, Meitner SW. Fabrication of imaging and surgical guides for dental implants. J Prosthet Dent. 2001;85(5):504-508.
7. Flügge TV, Nelson K, Schmelzeisen R, Metzger MC. Three-dimensional plotting and printing of an implant drilling guide: simplifying guided implant surgery. J Oral Maxillofac Surg. 2013;71(8):1340-1346.
8. Att W, Girard M. Digital workflow in reconstructive dentistry. In: Ferencz JL, Silva NRFA, Navarro JM, eds. High-Strength Ceramics: Interdisciplinary Perspectives. Chicago, IL: Quintessence Publishing; 2014:261-277.
9. Farré-Guasch E, Wolff J, Helder MN, et al. Application of additive manufacturing in oral and maxillofacial surgery. J Oral Maxillofac Surg.2015;
73(12):2408-2418.
10. Kang SH, Kim MK, Kim HJ, et al. Accuracy assessment of image-based surface meshing for volumetric computed tomography images in the craniofacial region. J Craniofac Surg. 2014;25(6):2051-2055.