Middle Superior Alveolar Technique: Efficacy in the Premolar Maxillary Region
Adel Martínez Martínez, DDS, MS; Andres Romero Blanquicett, DDS; and Isabella Manzur Villalobos, DDS
Abstract
Objective: A randomized, single-blind clinical trial was conducted to compare the efficacy of the infraorbital technique with the middle superior alveolar (MSA) technique in achieving pulpal anesthesia of maxillary premolars. Materials and Methods: Thirty voluntary subjects received 1.8 milliliters of 2% lidocaine with 1:80,000 epinephrine. The researchers assessed the degree of pulpal anesthesia with an electronic pulp tester, puncture pain, soft-tissue anesthesia and patient comfort at this anesthesia, and start time and duration of anesthetic effect. The data was analyzed using the Shapiro-Wilk, Mann-Whitney, and McNemar tests. Results: Deep pulpal anesthesia in the MSA technique was significantly higher when compared to the infraorbital technique in first and second premolars, the results being 95.2% and 100% respectively for the former technique and 66.7% and 42.9% respectively for the latter technique. The authors noted statistical significance in the perception of pain associated with the injection, with the infraorbital technique being the more painful technique (P = .003). The onset of the anesthetic effect was shorter after applying the MSA technique, and the duration of anesthetic effect was significantly higher with this technique. The incidence of subjective anesthesia of lips, skin, nasal wing, and gingiva was 100% for the infraorbital technique, with greater discomfort reported for the soft-tissue anesthesia in this technique. Conclusions: The MSA technique proved more effective in achieving pulpal anesthesia of maxillary premolars in comparison to the infraorbital technique.
Among anesthetic methods used in dentistry, the infraorbital technique is perhaps the one that generates the most controversy, especially when considering its effectiveness in dental procedures in maxillary incisors and premolars. Several clinical trials conducted to assess effectiveness of intraoral infraorbital nerve block showed that the rate of anesthetic success in central and lateral incisors was between 15% and 30%.1 In addition, patients catalog anesthesia of soft tissues using this technique as uncomfortable, predisposing the tissues to suffer lacerations or injuries.
Clinicians are forced to consider other alternatives to anesthetic blockade that allow success rates in premolars that exceed 90% without producing the uncomfortable sensation of anesthesia of the facial soft tissues. Among the alternatives that are reported to achieve this task in the premolar region are the use of the intraosseous technique, the middle alveolar technique, the anterior middle superior alveolar (MSA) technique, and the intraligamentary technique.2
In a clinical trial conducted in 28 patients Corbett et al in 2010 reported that the use of the infraorbital technique produced a significantly greater number of non-response episodes in premolars and canines when compared with the anterior MSA technique.3 The authors suggested that the use of the anterior superior and MSA technique be considered to anesthetize maxillary incisors and premolars. Other authors, such as Saxena et al in 2013, reported that MSA nerve block through a palatal approach provides pulpal anesthesia of the upper incisors, canines, and premolars on the anesthetized side, without extraoral anesthesia.4 Acharya et al in 2010 demonstrated that this block can be used as an effective technique in the anesthesia of the dental organs from the first premolar to the first molar in maxillary periodontal surgery.5 Other authors, such as Reed et al in 2012 and Berberich et al in 2009, have evaluated the anesthetic efficacy of the MSA technique and the infraorbital technique and have reported successful pulpal anesthesia in maxillary premolars ranging from 75% to 92%; these authors reported 100% of facial soft-tissue anesthesia, which was rated by the patients as uncomfortable.6,7
The investigators conducted the present study with the aim of comparing the anesthetic efficacy of the infraorbital technique with the MSA technique in maxillary premolars using 2% lidocaine with 1:80,000 epinephrine in a group of healthy voluntary patients. The two techniques were evaluated for: successful pulpal anesthesia using an electronic pulp tester, soft-tissue anesthesia (gingiva, labial semi-mucosa, lip skin), patient's perception of comfort before this anesthesia, the time of onset and the duration of the anesthetic effect.
Materials and Methods
The researchers designed a simple, randomized, blinded clinical trial to compare the effectiveness of the infraorbital technique in upper premolar anesthesia to that of the MSA technique, using 2% lidocaine with epinephrine 1:80,000. This study was carried out on 30 volunteers, 22 women and 8 men between the ages of 18 and 44 years, in whom a total of 120 teeth were evaluated with the use of an electronic pulp tester (Analytic Technology, Redmond, Washington). Also, 600 vitality tests were performed-six tests per tooth every 5, 10, 15, 20, 30, and 40 minutes. The present study was carried out at the University of Cartagena in Cartegena, Colombia.
The researchers evaluated the degree of successful pulpal anesthesia, pain at the puncture, soft-tissue anesthesia, perception of the patient's comfort before this anesthesia, the time of onset, and the duration of the anesthetic effect. Participants were excluded based on the following criteria: patients with premolars without pulpal vitality or with root canal treatment previously performed, women in pregnancy status, patients undergoing orthodontic treatment, patients with neurological disorders or blood dyscrasias, patients with infectious processes that compromise the maxillary premolar region, patients with ingestion of medications that alter consciousness and the perception of pain, or patients who have undergone extractions of premolars.
Each patient was subjected to two sessions. In the first session the details of the study were explained, a complete clinical history was made to verify the patient's background, a pulp vitality test was performed on the maxillary premolars, and a panoramic radiograph was taken to determine if the patient met the selection criteria. All the patients completed an informed written consent to participate in the study.
In the second session the application of the techniques was carried out. The subjects were operated on in two sessions with an interval of 8 days between each session. For each technique evaluated, 0.9 ml of the solution indicated in the randomization table was applied. The clinician who administered the anesthesia was not responsible for the annotation and evaluation of the results of the intervention. The anesthetic cartridges were masked and coded by a third person who did not belong to the group of investigators and were delivered to the investigator at the time of surgery, according to the randomization table. The operator, the patient, and the researchers in charge of collecting and tabulating the information were unaware of the content of the cartridges. This was revealed after the tabulation of the information.
For the placement of the techniques, the one described by Reed et al was referred to,6 using a dental anesthesia syringe and 24 x 0.30-mm needle, with 0.9 ml of 2% lidocaine with 1:80,000 epinephrine deposited. Immediately after the placement of the anesthetic technique, the subjects were questioned about the perception of the pain associated with the injection in each technique using the visual analog scale (VAS), which evaluates pain ranging from absence of pain (0) to the highest degree of pain (10).8 Pulp sensitivity was determined using the electronic pulp tester, which was adjusted to offer a digital reading from 0 to 80µA, which corresponds to a nonlinear voltage increase from 0 µA to the maximum in an average of 30 seconds. To validate the pulp test reading, the non-anesthetized lower mandibular canine was evaluated to ensure that the electronic pulp tester was operating correctly and that the subject was responding adequately during the experiment. At 4 minutes after anesthesia placement, soft-tissue anesthesia was evaluated by the subjective sensation of anesthesia at the time of performing a sensitivity test, which was performed through stimulation of the skin of the infraorbital region, external nasal wing, upper lip, and gingiva.
The pulp test was performed in its order; first premolar and second premolar on one side and then first and second premolar on the opposite side. Five minutes after the injection of the anesthetic the first test was performed on the evaluated teeth and then at intervals of 5 minutes until 20 minutes, and then every 10 minutes until completing 40 minutes after injection. The criterion used to determine if anesthesia was effective was that there was no response to maximum stimulation (ie, at least two consecutive readings of 80 µA). The number of episodes of no response to maximum stimulation was tabulated in a matrix table. The initiation of pulpal anesthesia (latency period) was evaluated as the first episode of no response to maximum stimulation (two consecutive readings of 80 µA). The duration of the anesthetic effect was evaluated as the time from the first reading of no response to maximum stimulation until the start of two or more responses to less than the maximum stimulation or at the end of the 40 minutes of the trial.
The statistical analysis of the data was developed using frequency measurements (%), as well as averages and standard deviation according to the nature of the variables. The difference between the groups, for quantitative variables, was evaluated depending on the normality of the data using the Shapiro-Wilk statistic. Thus, parametric statistics tests (unpaired Student's T test) or nonparametric (Wilcoxon signed-rank signs) were used. The chi-square test was used to compare proportions. All results were considered statistically significant when the P value was < .05. The analysis was performed using Stata statistical software v.13.2 for Windows (StataCorp, stata.com). This study was classified as a risk investigation greater than the minimum according to Article 11 of Resolution 8430 of 1993 of the Ministry of Health and Social Protection of Colombia, in which the confidentiality of information was reserved for not requesting the name of the patient who signed the informed consent, respecting the decision not to fill it out when he or she did not want to participate in the study.9
Results
Thirty patients (22 women [73.3%] and eight men [26.6%]) with an average age of 24 years (mean ± standard deviation [SD]: 24 ± 6.6; range: 18-44 years) participated in the study. Patients with successful pulpal anesthesia (SPA), determined by two consecutive maximum stimulation readings (80 µA) of the electronic pulp tester, did not present statistically significant differences in either technique. The SPA observed with the application of the middle superior alveolar (MSA) technique was 96.7% and 100% for the first and second premolars, respectively. With the infraorbital technique a SPA of 76.7% and 53.3% was observed, respectively, for the first and second premolars (Figure 1).
Figure 2 and Figure 3 show the pain at puncture during the injection. Twenty-five patients (83.33%) to whom the infraorbital technique was applied and 20 patients (66.67%) in the MSA technique classified the perception of pain associated with the injection as moderate according to VAS. There were statistically significant differences when evaluating the pain puncture during the injection (P = .003), with the infraorbital technique being more painful than the MSA technique.
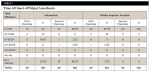
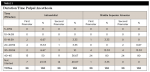
Table 1 and Table 2 show the time of onset and the duration of the anesthetic effect. With the MSA technique 83.33% of first premolars and 100% of second premolars were in the range between 5:00 to 9:59 minutes for the time of onset of pulpal anesthesia. With the infraorbital technique the percentage of the beginning of anesthesia for the first and second premolars was 50% and 46.67%, respectively. Similarly, the duration of pulpal anesthesia in the range of 40 to 45 minutes was evaluated during the application of each technique. With the MSA technique, 80% of both first and second premolars were found to be in this duration range, while with the infraorbital technique the percentage of duration of anesthesia in this range was 50% for first premolars and 36.67% for second premolars. There were no statistical differences between any these variables (P ˃ .05).
Regarding subjective evaluation of soft-tissue anesthesia, in the infraorbital technique 100% of the patients reported loss of sensitivity of the nasal wing, upper lip, cheeks, and vestibular gingiva in proximity to the puncture area, with the patients saying that anesthesia sensation was discomfort. Conversely, in the application of the MSA technique patients reported only anesthesia of the gingiva and cheeks, referring to this sensation as comfortable.
Discussion
In this study, the MSA anesthetic technique was more effective in achieving deep pulpal anesthesia of the maxillary premolars than the infraorbital technique. Anesthesia of soft facial tissues in the infraorbital technique was reported in 100% of the subjects evaluated, who classified this sensation as uncomfortable. These findings agree with the results found by Corbett et al, who in 2010 conducted a study in which they used the same criteria to define successful pulpal anesthesia (two consecutive maximum stimulation readings [80 µA] of the electronic pulp tester).3 As in the present study, they compared the effectiveness of the MSA blockade and the infraorbital block in obtaining deep pulpal anesthesia in anterior maxillary teeth, using lidocaine 2% with epinephrine 1:80,000. Those authors reported that the infraorbital technique has better rates of pulp anesthetic success in canines and premolars, although with the anterior MSA technique a greater number of episodes of pulpal nonresponse was achieved in the central (P = .012) and lateral (P < .001) incisors. They also observed that the incidence of anesthesia on the lips was 100%, with a sensation of numbness twice as high using the infraorbital technique; nevertheless, they concluded that both techniques produce similar levels of discomfort in the patient.
Berberich et al compared the anesthetic efficacy of 2% lidocaine with 1:100,000 epinephrine, 2% lidocaine with 1:50,000 epinephrine, and 3% mepivacaine in the intraoral, infraorbital nerve block.7 They concluded that the intraoral infraorbital nerve block was ineffective in providing profound pulpal anesthesia of the maxillary central incisor, lateral incisor, and first molar. Successful pulpal anesthesia of the canine and first and second premolars ranged from 75% to 92% by using 2% lidocaine with 1:100,000 and 1:50,000 epinephrine. However, pulpal anesthesia did not last for 60 minutes. The use of 3% mepivacaine provided a shorter duration of anesthesia than the lidocaine formulations with epinephrine in the canines and premolars. These results are similar to the present study, which was conducted with the same criteria to define successful pulpal anesthesia, soft-tissue anesthesia, and discomfort as reported by the patients.
Karkut et al compared the effectiveness of the infraorbital technique with extraoral and intraoral approaches.10 They reported that both extraoral and intraoral blockade were ineffective in providing deep pulp anesthesia in central incisors (15%) and lateral incisors (22%). The rate in canines was 92%, and in first and second premolars it was 80% to 90%. In this study, the authors observed how the infraorbital technique showed a lower degree of anesthesia in the premolars, 66.7% for the first premolars and 42.9% for the second premolars. Saxena et al reported that nerve block MSA provides pulpal anesthesia of the premolars, incisors, and maxillary canines with less extraoral anesthesia.4 Velasco and Soto obtained an anesthetic success of 66% in the second premolars and 40% in the first premolars when performing a blockade of the anterior and superior alveolar nerve.11
Corbett et al compared the levels of pain indicated by patients during insertion of the needle for both the conventional infraorbital technique and the anterior MSA (palatal approach) using computer-controlled anesthesia equipment.3 There were no statistically significant differences when evaluating the perception of pain indicated by patients when using the VAS (P = .768). This data differs from the results expressed in the present report, where the infraorbital technique was indicated to be more painful than the middle alveolar vestibular approach.
de Souza et al reported that the anterior MSA technique can be used as an alternative to anesthetize the vestibular area of the maxilla without undesirable effects on the facial structures, such as the upper lip, nasal wing, and lower eyelids, thus providing better comfort for the patient during performance of procedures.12
Conclusions
The results of this study show that the middle superior alveolar technique, using a vestibular approach and with the puncture made in the bottom groove between the two premolars, was more effective in achieving deep pulpal anesthesia in maxillary premolars when compared with the infraorbital technique, which produced greater pain at the puncture than the MSA technique. The use of the MSA technique in the anesthesia of upper premolars was more beneficial in terms of the speed of rapid onset and prolonged working time in comparison to the time offered by the infraorbital technique. The authors conclude that the application of the infraorbital technique in the anesthesia of premolars does not contribute in a positive way to the comfort of the patient, as soft-tissue anesthesia is uncomfortable for the patient and predisposes him or her to risk of injuries or traumas. The results of the present study allow the authors to recommend the use of the MSA technique when performing procedures in the maxillary premolar region.
About the Authors
Adel Martínez Martínez, DDS, MS
Dentist and Oral Surgeon, University of Cartagena, Cartagena, Colombia; Professor, Faculty of Dentistry, University of Cartagena; Member, GITOUC Research Group
Andres Romero Blanquicett, DDS
Dentist, University of Cartagena, Cartagena, Colombia
Isabella Manzur Villalobos, DDS
Dentist, University of Cartagena, Cartagena, Colombia
References
1. Martinez AM, Lujan MP, Portillo D. Anesthetic efficacy of the infraorbital nerve block in maxillary incisors and premolars using 2% lidocaine with epinephrine 1:80,000. Rev Odont Mex. 2017;21(1):e33-e39.
2. Becker DE, Reed KL. Local anesthetics: review of pharmacological considerations. Anesth Prog. 2012;59(2):90-101.
3. Corbett IP, Jaber AA, Whitworth JM, Meechan JG. A comparison of the anterior middle superior alveolar nerve block and infraorbital nerve block for anesthesia of maxillary anterior teeth. J Am Dent Assoc. 2010;141(12):1442-1448.
4. Saxena P, Gupta SK, Newaskar V, Chandra A. Advances in dental local anesthesia techniques and devices: an update. Natl J Maxillofac Surg. 2013;4(1):19-24.
5. Acharya AB, Banakar C, Rodrigues SV, et al. Anterior middle superior alveolar injection is effective in providing anesthesia extending to the last standing molar in maxillary periodontal surgery. J Periodontol. 2010;81(8):1174-1179.
6. Reed KL, Malamed SF, Fonner AM. Local anesthesia part 2: technical considerations. Anesth Prog. 2012;59(3):127-136.
7. Berberich G, Reader A, Drum M, et al. A prospective, randomized, double-blind comparison of the anesthetic efficacy of two percent lidocaine with 1:100,000 and 1:50,000 epinephrine and three percent mepivacaine in the intraoral, infraorbital nerve block. J Endod. 2009,35(11):1498-1504.
8.Kudo M. Initial injection pressure for dental local anesthesia: effects on pain and anxiety. Anesth Prog. 2005;52(3):95-101.
9. Ministry of Health. Resolution Number 8430 of 1993. Republic of Colombia. https://www.animallaw.info/sites/default/files/RESOLUCION-8430-DE-1993.PDF. Accessed April 8, 2019.
10. Karkut B, Reader A, Drum M, et al. A comparison of the local anesthetic efficacy of the extraoral versus the intraoral infraorbital nerve block. J Am Dent Assoc. 2010;141(2):185-192.
11. Velasco I, Soto R. Anterior and middle superior alveolar nerve block for anesthesia of maxillary teeth using conventional syringe. Dent Res J (Isfahan). 2012;9(5):535-540.
12. de Souza Tolentino L, Barbisan Souza A, Girardi AA, et al. The anesthetic effect of anterior middle superior alveolar technique (AMSA). Anesth Prog. 2015;62(4):153-158.