Managing Angulation Challenges With Implant Overdentures
Michael D. Scherer, DMD, MS
ABSTRACT
Proper treatment planning is critical to achieving a successful outcome when treating patients with implant overdenture restorations. Key factors related to success include the number, location, and distribution of implants and choice of abutment. Contemporary design of stud-style abutment systems for overdentures is aimed at accommodating patients who present with challenges such as anatomical limitations or poor dexterity hampering insertion and removal of prostheses. This article describes the effective management of excessive angulation to achieve an enhanced outcome with implant overdenture treatment, even with a less-than-ideal clinical presentation.
Full-arch reconstruction with implant-retained overdentures has long been regarded as a safe and highly effective long-term treatment option for edentulous patients.1-3 Implant overdenture treatment has an extensive history of clinical use, and patient satisfaction has been shown to be favorable.4 When patients are treated with implant overdenture therapy, a complete diagnosis is a critical first step to ensure optimal outcomes.5 Appropriate treatment planning is vital to achieving a proper implant overdenture restoration, while improper treatment planning steps may lead to a poor outcome.
Key factors related to successful treatment with overdentures include the number, location, and distribution of implants and choice of abutment.6,7 While the use of parallel implants that are widely distributed is generally desirable for optimal treatment, patients often present with challenging anatomical features, insufficient bone volume in all dimensions, and/or critical anatomy that precludes ideal placement of dental implants. Some clinicians may consider the ideal placement of implants for overdentures as parallel to each other and perpendicular to the occlusal plane of the denture. With this orientation and design, restorations can reliably and predictably be performed utilizing commercially available stud-style abutments, such as a LOCATOR® (Zest Dental Solutions, zestdent.com). Two to four stud-style abutments may be used to achieve optimal retention, stability, and comfort of the prosthesis with minimal bulk, maintenance, and cost.8 Additionally, overdenture design should emphasize simplicity to ensure clinical outcomes that patients are more inclined to accept.9
Anatomical features associated with mandibular or maxillary edentulous ridges can range from straight or rounded to irregular and sharp ridges, and variability in bone width may limit potential implant sites for overdentures.5 Choosing anatomically challenged anterior and posterior sites for overdenture placement while using 2-dimensional radiography often results in non-ideal implant placement.10 Factors such as narrow bone volume, the inferior alveolar nerve being anteriorly or superiorly positioned, extensive bony undercuts, the inferior portion of the maxillary sinus, proximity to high-risk vascular structures, or a patient's desire to avoid additional surgical procedures may prompt a clinician to angulate a dental implant, which could result in the positioning of implants in non-ideal configurations.
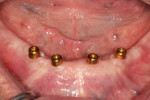
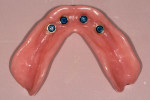
Angulation challenges may be especially evident in overdenture cases in which more than two implants are used, as differences in angulation are more visible in such cases (Figure 1). In the author's experience, challenges with the use of conventional stud-style abutments include excessive angulation, increased maintenance and wear of inserts, and difficulty maintaining hygiene. Increased angulation may result in greater challenges to inserting and removing the prosthesis, which can become difficult for patients who are older and/or have limited dexterity. This challenge also can make it hard for patients to properly clean the inside of the retentive portion of the stud-style abutment and may increase wear of the retentive inserts (Figure 2).
While stud-style abutments offer the ability to correct off-axis, non-ideal implant placement, existing designs have limited angle correction to 40 degrees of total divergence. Contemporary design of stud-style abutment systems for overdentures has been directed toward improving the accommodation of patients with challenging presentations. This article describes how excessive angulation can be managed to enhance outcomes with implant overdenture treatment even in difficult clinical case presentations.
Case Report: Existing Angled Implants
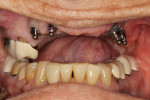
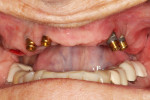
Patients who present with existing implants are often challenging to treat and may not be ideal for overdenture treatment. A 65-year-old female patient with existing maxillary anterior implants presented concerned that she might need a full denture and desired to keep her implants. At presentation, teeth Nos. 2 through 4 were nonrestorable, and there were existing implants at Nos. 5, 6, 11, and 12 with o-ring attachments for an existing removable partial denture (Figure 3). The patient expressed concerns regarding the bulkiness of her current prosthesis and said she had difficulty inserting and removing it. Upon examination, it was evident that existing implants were not in ideal positions nor had ideal angulation, and a moderate amount of bone loss surrounded each implant. The patient indicated that the implants had been placed with the goal of having traditional crown-and-bridge prosthetics fabricated, but a life event occurred that required her to change the treatment plan to a more affordable option.
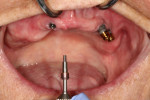
After extensive discussion regarding the existing condition and treatment options, the patient decided to proceed with a complete denture prosthesis. Impressions were made for an immediate denture with the goal of attachment to existing implants at the time of extractions of teeth Nos. 2 through 4. The existing o-ring abutments were removed, the implants were sized, and tissue height measurements were determined. The patient returned, local anesthesia was administered, and teeth Nos. 2 through 4 were extracted. The o-ring abutments were removed from each of the implants, and traditional, low-profile, stud-style abutments (LOCATOR) were placed and torqued to the manufacturer's recommendations (Figure 4).
After placement of the abutments, a recess was prepared within the patient's denture, housings were attached to the abutments, and composite resin (CHAIRSIDE® Attachment Processing Material, Zest Dental Solutions) was used to pick up the housings within the denture (Figure 5). Extended-range nylon inserts were utilized within the denture housings to accommodate the excessive angulation of the implants. The patient demonstrated insertion and removal of the prosthesis and was satisfied with the esthetics, fit, and form of the restoration.
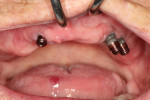
Approximately 3 months after the teeth were removed the patient returned with the concern that she was having difficulty inserting and removing the prosthesis. Upon detailed examination of the prosthesis, the extended-range nylon inserts were found to be bent at the edges and had started to wear prematurely. Additionally, the patient indicated that she had a problem with an implant on her right side. Clinical examination revealed the implant in the No. 5 position had fractured slightly below the gingiva (Figure 6). After explaining to the patient why the excessive angulation of her implants was compounding the problem, the author recommended changing the traditional stud-style abutments to a more contemporary stud-style abutment (LOCATOR R-Tx®, Zest Dental Solutions) that could accommodate extended angulation discrepancies between implants.
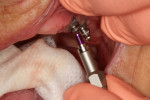
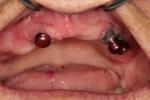
The traditional stud-style abutments were removed and contemporary study-style abutments were placed on top of each implant (Figure 7). Complete adaptation of each abutment to the respective implant was verified, and each abutment was torqued to the manufacturer's recommended settings (Figure 8). Housings were attached to the top of each of abutment (Figure 9), and composite resin was used to attach each one to the denture. The processing inserts were removed and medium-strength nylon inserts were placed into the housings within the denture. The patient was given instructions on inserting and removing the prosthesis and was satisfied with the esthetics, fit, and form of the restoration (Figure 10).
The patient returned approximately 3 months after the abutments were changed and reported enhanced comfort, easy insertion and removal, and satisfaction with the stability of the prosthesis for chewing and speaking. Additionally, the nylon inserts appeared to have no damage or wear, and retention levels for the patient seemed appropriate. The patient expressed satisfaction and indicated that she felt like the change was beneficial to ensuring a long-term result with her teeth and implants.
Discussion
While proper diagnosis and treatment planning may prevent many cases of excessive implant angulation, as dental implant treatment becomes increasingly more prevalent patients will certainly require treatment alterations over the course of their lifetime. In the case of the aforementioned maxillary overdenture treatment, the patient had implants placed that were intended for a crown-and-bridge prosthesis; however, due a major change in her personal life and financial situation, she requested a less expensive removable partial denture option. Although at the time of presentation to the author's office she was accustomed to wearing the removable partial denture, she was never content with that restorative therapy. Ultimately, the design of the removable partial prosthesis impacted her ability to be comfortable with the treatment, because the implants were placed in non-ideal positions for such treatment. Eventually, as the remaining teeth began to fail, a full denture was indicated.
The first option presented to the patient was to prepare the implants to the gingiva on her left side, construct a bar superstructure, and fabricate an overdenture with clips within the bar. The patient, however, declined this option because she was concerned that the implants would "fall out" and did not want to commit to a large financial expense. A bar overdenture likely would have permitted the patient to be able to have the implants splinted together to minimize parafunctional forces and provide enhanced stability. In addition to these benefits, a splinted bar design can incorporate stud-style abutments to achieve prosthetic simplicity and the splinting effect of the bar. While splinted bar treatment may have been the primary indication for this patient's treatment, the higher cost was prohibitive and a simpler, less expensive design was chosen. Contemporary stud-style abutments can allow for more divergence between implants and enhance flexibility while maintaining reasonable costs for patients. Therefore, the patient ultimately accepted this treatment option for the definitive therapy.
Overdenture Abutment Design
Because of enhanced simplicity and ease of use, individual stud-style abutments are often preferred for implant-retained overdentures versus bar, telescopic, and fixed options. Traditional stud-style abutments, such as the LOCATOR system, have low prosthetic height requirements and enhanced physical properties of retention and stability and allow for simple clinical procedures. In some patients, such as the patient described in this case presentation, the use of stud-style abutments may make the insertion and removal of the prosthesis challenging, resulting in increased wear and possible prosthetic complications.
New overdenture abutment designs that accommodate greater implant angulation are intended to overcome some of the limitations associated with conventional stud-style abutments while maintaining many important, desirable features, such as retention, stability, and other physical properties. Contemporary stud-style abutments (eg, LOCATOR R-Tx) permit implant angulation up to 30 degrees per implant or 60 degrees of total divergence between implants (data on file, Zest Dental Solutions). The dual retention features are on the outer part of the abutment, which eases hygiene maintenance and simplifies denture insertion and removal.
Overdenture abutments designed to permit greater flexibility also allow some slight movement of the denture on the soft tissues, minimizing the forces dispersed upon the dental implant. When these occlusal or lateral functional and nonfunctional forces are kept to a minimum, stress reduction on the implant, abutment, and nylon inserts can be expected.11 Additionally, as forces are kept off the dental implant, occlusal and non-occlusal overloading forces are minimized and nylon insert wear is reduced.
Prosthetic flexibility and simplicity are two extremely important factors in overdenture therapy. Designs like those associated with stud-style abutments offer simple form, ease of cleaning, and relatively low cost.9 Research shows that stud-style overdenture abutments can actually increase in retention and stability when angulation between implants is increased by 10 degrees.12 While this style of abutment can accommodate some angulation and even result in greater physical properties, excessive angulation can lead to a dramatic reduction in retention and stability of the prosthesis.13 Furthermore, evaluation of the effects of the long-term retention level of off-angled implants has shown a significant consequence of excessive angulation and increased wear/maintenance of the overdenture inserts.14
Conclusion
Full-arch reconstruction with implant overdenture therapy is a predictable, long-term treatment for patients who are comfortable with removable prostheses. While clinicians generally prefer implants placed as parallel as possible, patients often present with compromised situations that require restoration. Additionally, traditional stud-style overdenture systems only permit a moderate amount of angle correction. Contemporary systems enable greater angulation differences between implants. As a result, challenging cases that usually would require expensive or complex approaches can be treated with simple, affordable, and yet effective techniques.
Disclosure
The author is a clinical consultant to Zest Dental Solutions.
About the Author
Michael D. Scherer, DMD, MS
Assistant Clinical Professor, School of Dentistry, Loma Linda University, Loma Linda, California; Private Practice, Sonora, California
References
1. Naert I, Alsaadi G, Quirynen M. Prosthetic aspects and patient satisfaction with two implant-retained mandibular overdentures: a 10-year randomized clinical study. Int J Prosthodont. 2004;17(4):401-410.
2. Sadowsky SJ. Mandibular implant-retained overdentures: a literature review. J Prosthet Dent. 2001;86(5):468-473.
3. Scherer MD. Overdenture implants. A simplified and contemporary approach to planning and placement. Dent Today. 2015;34(8):54-60.
4. Reissmann DR, Enkling N, Moazzin R, et al. Long-term changes in oral health-related quality of life over a period of 5 years in patients treated with narrow diameter implants: a prospective clinical study. J Dent. 2018;75:84-90.
5. Scherer MD. Presurgical implant-site assessment and restoratively driven digital planning. Dent Clin North Am. 2014;58(3):561-595.
6. Scherer MD, McGlumphy EA, Seghi RR, Campagni WV. Comparison of retention and stability of implant-retained overdentures based upon implant number and distribution. Int J Oral Maxillofac Implants. 2013;28(6):1619-1628.
7. Scherer MD, McGlumphy EA, Seghi RR, Campagni WV. Comparison of retention and stability of two implant-retained overdentures based on implant location. J Prosthet Dent. 2014;112(3):515-521.
8. Roccuzzo M, Bonino F, Gaudioso L, et al. What is the optimal number of implants for removable reconstructions? A systematic review on implant-supported overdentures. Clin Oral Implants Res. 2012;23 suppl 6:229-237.
9. Burns DR, Unger JW, Coffey JP, et al. Randomized, prospective, clinical evaluation of prosthodontic modalities for mandibular implant overdenture treatment. J Prosthet Dent. 2011;106(1):12-22.
10. Ahmad R, Abu-Hassan MI, Chen J, et al. The relationship of mandibular morphology with residual ridge resorption associated with implant-retained overdentures. Int J Prosthodont. 2016;29(6):573-580.
11. Elsyad MA, Eltowery SM, Gebreel AA. Peri-implant strain around mesially inclined two-implant-retained mandibular overdentures with Locator attachments. J Oral Sci. 2017;59(4):483-490.
12. Stephens GJ, di Vitale N, O'Sullivan E, McDonald A. The influence of interimplant divergence on the retention characteristics of locator attachments, a laboratory study. J Prosthodont. 2014;23(6):467-475.
13. Sultana N, Bartlett DW, Suleiman M. Retention of implant-supported overdentures at different implant angulations: comparing Locator and ball attachments. Clin Oral Implants Res. 2017;28(11):1406-1410.
14. Aroso C, Silva AS, Ustrell R, et al. Effect of abutment angulation in the retention and durability of three overdenture attachment systems: an in vitro study. J Adv Prosthodont. 2016;8(1):21-29.