Use of Soft-Tissue and Bone Grafting to Treat Complex Recession With Root Prominence and Buccal Plate Deficiencies
Bradley S. McAllister, DDS, PhD; V. Thomas Eshraghi, DMD; and Kyle A. Malloy, DMD, MS
Abstract: Beyond the traditional monotherapy of connective tissue grafting, the combination of orthodontic therapy, soft-tissue grafting, and bone grafting with biologics may provide ideal treatment for complex recession defects with root prominence, thin tissues, and buccal plate dehiscences. The authors propose the benefits of performing a preoperative evaluation of complex mucogingival defects with cone-beam computed tomography (CBCT) technology and then considering surgical management with modalities like bone grafting and orthodontics in addition to the classic soft-tissue grafting approach. Regeneration of the complete periodontium may result in better long-term soft-tissue stability and tooth retention following treatment of complex recession cases.
Nearly a decade ago McGuire and colleagues demonstrated human histologic evidence of complete regeneration of the attachment process following their treatment of recession defects with bone graft plus platelet-derived growth factor (PDGF).1 Yet, to date, virtually no shift has occurred in clinical practice away from the routine connective tissue graft (CTG) treatment alone for root coverage, even in complex recession defects that have a deficient buccal plate and root prominence. This article documents several cases presented at the 2017 International Society of Periodontal Plastic Surgeons meeting in which the combination of orthodontic therapy, soft-tissue grafting, and bone grafting with biologics was employed to provide ideal treatment for complex recession defects with root prominence, thin tissues, and buccal plate dehiscences identified on preoperative cone-beam computed tomography (CBCT) scans. To date, no comparative studies have been performed to evaluate the performance differences between routine CTG treatment alone and the proposed combination therapy approach. The authors hypothesize that regeneration of the complete periodontium will result in better long-term soft-tissue stability and tooth retention following treatment of complex recession cases that present with root prominence, thin soft tissues, and a deficient buccal plate. (Authors' note: This article focuses on recession defects rather than on the implant procedures discussed.)
Achieving Root Coverage
The literature is extensive with regard to root coverage, showing excellent overall root coverage outcomes with either autogenous tissue2-4 or allograft-derived dermal tissues.5-7 Meta-analysis reviews have reported consistent results of greater than 90% root coverage with the use of both autogenous and allograft-derived dermal tissues.2,8,9 A trend in the literature has been the reporting of autogenous connective tissue as the "gold standard" with regard to mucogingival root coverage procedures. However, there is evidence that numerous additional materials and techniques may have equivalent results without the need for a second surgical site to harvest the graft. Human histology has been completed comparing autogenous CTGs with acellular dermal matrix grafts.10 The findings demonstrated similar results with no significant differences in root surface connective tissue attachment or tissue thickness. Although the literature offers many outstanding results for a variety of procedures aimed at achieving root coverage, two glaring issues persist: case selection and duration of follow-up.
Most published studies on root coverage outcomes include only patients with either Miller Class I or II gingival recession. These are the least complex and most predictable defects to treat, and, expectedly, a variety of treatment options would result in similar, highly predictable, ideal results. The small amount of data available in the literature related to more complex cases (ie, Miller Class III and IV gingival recession) is not as positive. A small group of studies have reported results for Miller Class III gingival recession in addition to Class I and II.11-18 The mean root coverage ranged greatly, from 51.5% to 98.1%, with complete root coverage being achieved 0 to 90.5% of the time in these studies. Currently, the only available data on the most severe Class IV gingival recession comes from either case reports or case series, and the general consensus is that root coverage results for this classification are inconsistent and predictive results are not possible.19-25
Long-term evaluation of root coverage outcomes is also lacking in the literature. The range of follow-up noted from studies in several systematic and meta-analysis reviews was from 6 to 60 months with 6 to 12 months most common.2,8,9 With limited long-term data on root coverage procedures, especially in the more complex subset of cases (Miller Class III and IV gingival recession and/or those with significant root prominences and buccal plate deficiencies), additional research is clearly needed. The lack of research results in these cases, along with clinical observation, has prompted the authors to consider additional therapies beyond the traditional monotherapy of connective tissue grafting. It is anticipated that the addition of bone grafting and/or orthodontic therapy to the classic connective tissue grafting will optimize the long-term root coverage results in complex cases.
3-Dimensional Information
The recent Best Evidence Consensus (BEC) published by the American Academy of Periodontology describes the benefits of CBCT use for risk assessment of the dentoalveolar changes influenced by tooth movement.25-28 It is well known that CBCT technology is the only means to evaluate the buccal plate around teeth and implants.29 The BEC reviews discuss the importance of having the appropriate 2-dimensional (2D) and 3-dimensional (3D) radiographs for proper treatment planning and surgical management when complex mucogingival defects are present. In cases with significant root prominence, it is ideal to orthodontically move the teeth into a better position within the bony envelope to optimize long-term treatment outcomes.
One recently developed orthodontic treatment planning program (SureSmile®, suresmile.com) combines CBCT data (DICOM file) with optical intraoral scan data (STL file), which allows the clinician to perform virtual orthodontic treatment plans taking into account root position and bone relationships. Historically, this was not possible, and orthodontists typically focused only on the crown position because they did not have information regarding the 3D root position and buccal plate dimensions to assist in treatment planning the case with a healthy mucogingival complex in mind.
Bone Graft Materials
A variety of bone grafting approaches are available to treat recession cases with significant root prominence and a deficient buccal plate. The selection of graft materials and case type may impact the ability to achieve complete regeneration of the periodontium. The extensiveness of the root prominence and recession and degree of buccal plate deficiency will impact graft material selection and clinical outcomes. A variety of materials have histologic evidence of complete regeneration with either recession or intrabony defect treatment, including PDGF-bb,1 enamel matrix derivatives (EMDs),30 freeze-dried bone allograft,31-33 and anorganic bovine-derived hydroxyapatite matrix.34,35
Stem cell therapy does not have human histology, but some animal studies have demonstrated complete regeneration of the periodontium where the labeled stem cells were shown to form cementoblasts, periodontal ligament fibroblasts, and osteoblasts.36 Several publications with stem cell-containing allografts have shown successful use in periodontal defects.37-39
Case Examples
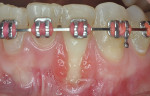
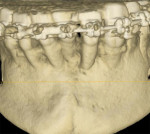
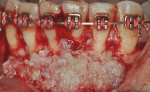
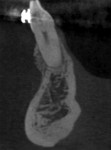
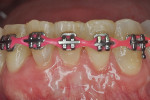
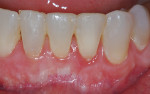
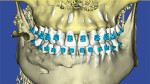
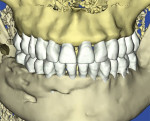
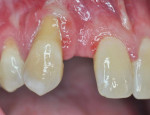
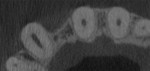
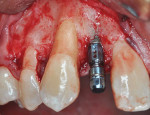
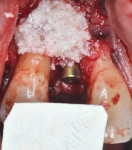
Three cases are presented where bone grafting and biologics were employed in the treatment of complex recession defects. Figure 1 through Figure 6 demonstrate the treatment of tooth No. 23, which presented with significant recession, a buccal plate deficiency, root prominence, and a thin periodontium. In this 44-year-old healthy female patient the recommended orthodontic therapy was initiated to address the root prominence of tooth No. 23 and other tooth positioning issues (Figure 1). A CBCT (Carestream CS 9300, Carestream Dental, carestreamdental.com) was taken at the start of orthodontic treatment for risk assessment; it showed no buccal plate for most of tooth No. 23 (Figure 2). Shortly after initiation of orthodontic tooth movement, combination therapy consisting of soft-tissue grafting along with bone grafting with stem cell therapy (Osteocel® Plus, ACE Surgical Supply Co., Inc., acesurgical.com) and EMD (Emdogain®, Straumann, straumann.com) was started (Figure 3). The outcome of complete root coverage and a significant improvement in the buccal plate (Figure 4 and Figure 5) should improve the long-term prognosis of tooth No. 23 and the adjacent teeth (Figure 6).
Ideally in these types of orthodontic cases, which are at risk for recession, pretreatment planning with a CBCT and intraoral scan is performed to allow the dental team to determine if grafting is required and what orthodontic movement is achievable. Figure 7 and Figure 8 show a second periodontal-orthodontic case where SureSmile computer-generated treatment planning was utilized. The CBCT (Carestream CS 9300) and intraoral optical scan (Carestream CS 3600) were used to optimize both the clinical crown position and the roots within the grafted bone. The treatment planning program then uses a series of robotically bent orthodontic wires to accomplish the desired orthodontic movement.40
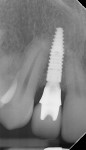
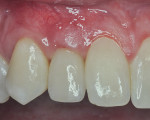
In the authors' third case (Figure 9 through Figure 15), treatment of a complex recession defect on tooth No. 6 is illustrated. The tooth presented with root prominence, thin tissues, and a deficient buccal plate (Figure 9 and Figure 10). The healthy 28-year-old male patient had no systemic issues and had declined orthodontic therapy, which was recommended for the significant root prominence on No. 6 and other tooth positioning issues.
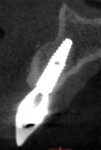
After placement of a Roxolid® 3.3-mm diameter implant (Straumann) in position No. 7 (Figure 11), Emdogain was placed on the root of No. 6 (Figure 12). Because the root prominence was substantial and no orthodontic treatment was planned, the bone graft material chosen was anorganic bovine bone, which has excellent long-term dimensional stability.41 The final result shows complete root coverage with an improvement in the buccal bone (Figure 13 and Figure 14). The CBCT (Figure 15) also shows at least 2 mm of buccal bone on implant No. 7, a factor that has been reported to be critical to long-term soft-tissue stability.42 Soft-tissue thickness also has been shown to be important in long-term soft-tissue stability around implants.43,44
Conclusions
The goal of this article was to demonstrate through case presentation the benefit of performing a preoperative evaluation of complex mucogingival defects with CBCT technology and then considering surgical management with modalities such as bone grafting and orthodontics in addition to the classic soft-tissue grafting approach. Ideally, potential regeneration of the complete periodontium along with elimination of possible patient-controlled etiologies may lead to long-term stability of the soft tissues and minimize the potential for recurrent recession, root sensitivity, root damage, esthetic issues, and tooth loss.
Disclosure
Dr. McAllister occasionally receives honoraria from Straumann and ACE Surgical Supply, and Dr. Eshraghi occasionally receives honoraria from Straumann.
About the Authors
Bradley S. McAllister, DDS, PhD
Part-time Faculty, Department of Periodontology, Oregon Health & Sciences University, Portland, Oregon; Private Practice, Tualatin, Oregon
V. Thomas Eshraghi, DMD
Assistant Professor, Graduate Periodontics, Oregon Health & Sciences University, Portland, Oregon; Private Practice, Tualatin, Oregon
Kyle A. Malloy, DMD, MS
Private Practice, Portland, Oregon
References
1. McGuire MK, Scheyer T, Nevins M, Schupbach P. Evaluation of human recession defects treated with coronally advanced flaps and either purified recombinant human platelet-derived growth factor-BB with beta tricalcium phosphate or connective tissue: a histologic and microcomputed tomographic examination. Int J Periodontics Restorative Dent. 2009;29(1):7-21.
2. Clauser C, Nieri M, Franceschi D, et al. Evidence-based mucogingival therapy. Part 2: Ordinary and individual patient data meta-analyses of surgical treatment of recession using complete root coverage as the outcome variable. J Periodontol. 2003;74(5):741-756.
3. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
4. Raetzke PB. Covering localized areas of root exposure employing the "envelope" technique. J Periodontol. 1985;56(7):397-402.
5. Aichelmann-Reidy ME, Yukna RA, Evans GH, et al. Clinical evaluation of acellular allograft dermis for the treatment of human gingival recession. J Periodontol. 2001;72(8):998-1005.
6. Papageorgakopoulos G, Greenwell H, Hill M, et al. Root coverage using acellular dermal matrix and comparing a coronally positioned tunnel to a coronally positioned flap approach. J Periondontol.2008;79(8):1022-1030.
7. Woodyard JG, Greenwell H, Hill M, et al. The clinical effect of acellular dermal matrix on gingival thickness and root coverage compared to coronally positioned flap alone. J Periodontol.2004;75(2):44-56.
8. Roccuzzo M, Bunino M, Needleman I, Sanz M. Periodontal plastic surgery for treatment of localized gingival recessions: a systematic review. J Clin Periodontol. 2002;29 suppl 3:178-194.
9. Gapski R, Parks CA, Wang HL. Acellular dermal matrix for mucogingival surgery: a meta-analysis. J Periodontol. 2005;76(11):1814-1822.
10. Cummings, LC, Kaldahl WB, Allen EP. Histologic evaluation of autogenous connective tissue and acellular dermal matrix grafts in humans. J Periodontol. 2005;76(2):178-186.
11. Zucchelli G, Marzadori M, Mele M, et al. Root coverage in molar teeth: a comparative controlled randomized clinical trial. J Clin Periodontol. 2012;
39(11):1082-1088.
12. Miller PD Jr. Root coverage using the free soft tissue autograft following citric acid application. II. Treatment of the carious root. Int J Periodontics Restorative Dent. 1983;3(5):38-51.
13. Barker TS, Cueva M, Rivera-Hidalgo F, et al. A comparative study of root coverage using two different acellular dermal matrix products. J Periodontol. 2010;81(11):1596-1603.
14. Boltchi FE, Allen EP, Hallmon WW. The use of a bioabsorbable barrier for regenerative management of marginal tissue recession. I. Report of 100 consecutively treated teeth. J Periodontol.2000;71(10):1641-1653.
15. Carney CM, Rossmann JA, Kerns DG, et al. A comparative study of root defect coverage using an acellular dermal matrix with and without a recombinant human platelet-derived growth factor. J Periodontol.2012;83(7):893-901.
16. Cueva MA, Boltchi FE, Hallmon WW, et al. A comparative study of coronally advanced flaps with and without the addition of enamel matrix derivative in the treatment of marginal tissue recession. J Periodontol.2004;75(7):949-956.
17. Jepsen S, Heinz B, Kermanie MA, Jepsen K. Evaluation of a new bioabsorbable barrier for recession therapy: a feasibility study. J Periodontol.2000;71(9):1433-1440.
18. Nart J, Valles C, Mareque S, et al. Subepithelial connective tissue graft in combination with a coronally advanced flap for the treatment of Miller Class II and III gingival recessions in mandibular incisors: a case series. Int J Periodontics Restorative Dent.2012;32(6):647-654.
19. Miller PD Jr, Binkley LH Jr. Root coverage and ridge augmentation in Class IV recession using a coronally positioned free gingival graft. J Periodontol. 1986;57(6):360-363.
20. Azzi R, Takei HH, Etienne D, Carranza FA. Root coverage and papilla reconstruction using autogenous osseous and connective tissue grafts. Int J Periodontics Restorative Dent. 2001;21(2):141-147.
21. Azzi R, Etienne D, Sauvan JL, Miller PD. Root coverage and papilla reconstruction in Class IV recession: a case report. Int J Periodontics Restorative Dent.1999;19(5):449-455.
22. De Castro Pinto RC, Colombini BL, Ishikiriama SK, et al. The subepithelial connective tissue pedicle graft combined with the coronally advanced flap for restoring missing papilla: a report of two cases. Quintessence Int. 2010;41(3):213-220.
23. Chambrone LA, Chambrone L. Root coverage in a class IV recession defect achieved by creeping attachment: a case report. J Int Acad Periodontol. 2006;8(2):47-52.
24. Vergara JA, Caffesse RG. Localized gingival recessions treated with the original envelope technique: a report of 50 consecutive patients. J Periodontol. 2004;75(10):1397-1403.
25. Mandelaris GA, Scheyer ET, Evans M, et al. American Academy of Periodontology Best Evidence Consensus statement on selected oral applications for cone-beam computed tomography. J Periodontol. 2017;
88(10):939-945.
26. Rios HF, Borgnakke WS, Benavides E. The use of cone-beam computed tomography in management of patients requiring dental implants: An American Academy of Periodontology best evidence review. J Periodontol. 2017;88(10):946-959.
27. Mandelaris GA, Neiva R, Chambrone L. Cone-beam computed tomography and interdisciplinary dentofacial therapy: an American Academy of Periodontology best evidence review focusing on risk assessment of the dentoalveolar bone changes influenced by tooth movement. J Periodontol. 2017;88(10):960-977.
28. Kim DM, Bassir SH. When is cone-beam computed tomography imaging appropriate for diagnostic inquiry in the management of inflammatory periodontitis? An American Academy of Periodontology best evidence review. J Periodontol. 2017;88(10):978-998.
29. Eshraghi T, McAllister N, McAllister B. Clinical applications of digital 2-D and 3-D radiology for the periodontist. J Evid Based Dent Pract. 2012;12(3 suppl):36-45.
30. Cochran DL, King GN, Schoolfield J, et al. The effect of enamel matrix proteins on periodontal regeneration as determined by histological analyses. J Periodontol. 2003;74(7):1043-1055.
31. Bowers GM, Chadroff B, Carnevale R, et al. Histologic evaluation of new attachment apparatus formation in humans: Part I. J Periodontol. 1989;60(12):664-674.
32. Bowers GM, Chadroff B, Carnevale R, et al. Histologic evaluation of new attachment apparatus formation in humans: Part II. J Periodontol. 1989;60(12):675-682.
33. Bowers GM, Chadroff B, Carnevale R, et al. Histologic evaluation of new attachment apparatus formation in humans: Part III. J Periodontol. 1989;60
(12):683-693.
34. Mellonig JT. Human histologic evaluation of a bovine-derived bone xenograft in the treatment of periodontal osseous defects. Int J Periodontics Restorative Dent. 2000;20(1):19-29.
35. Nevins ML, Camelo M, Lynch SE, et al. Evaluation of periodontal regeneration following grafting intrabony defects with bio-oss collagen: a human histologic report. Int J Periodontics Restorative Dent. 2003;23(1):9-17.
36. Kawaguchi H, Hirachi A, Hasegawa N, et al. Enhancement of periodontal tissue regeneration by transplantation of bone marrow mesenchymal stem cells. J Periodontol. 2004;75(9):1281-1287.
37. Eshraghi T, McAllister B. Clinical applications of a stem cell-based therapy for oral bone reconstruction. In: Li S, L'Heureux N, Elisseeff J, eds. Stem Cell and Tissue Engineering. 2nd ed. Singapore: World Scientific; 2018:297-324.
38. McAllister BS. Stem cell-containing allograft matrix enhances periodontal regeneration: case presentations. Int J Periodontics Restorative Dent. 2011;31(2):149-155.
39. McAllister BS, Haghighat K, Gonshor A. Histologic evaluation of a stem cell-based sinus-augmentation procedure. J Periodontol. 2009;80(4):679-686.
40. Sachdeva RC, Aranha SL, Egan ME, et al. Treatment time: SureSmile vs conventional. Orthodontics (Chic.). 2012:13(1):72-85.
41. Margolin MD, Cogan AG, Taylor M, et al. Maxillary sinus augmentation in the non-human primate: a comparative radiographic and histologic study between recombinant human osteogenic protein-1 and natural bone mineral. J Periodontol. 1998;69(8):911-919.
42. Miyamoto Y, Obama T. Dental cone beam computed tomography analyses of postoperative labial bone thickness in maxillary anterior implants: comparing immediate and delayed implant placement. Int J Periodontics Restorative Dent. 2011;31(3):215-225.
43. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol. 2003;74(4):557-562.
44. Kan JY, Rungcharassaeng K, Lozada JL, Zimmerman G. Facial gingival tissue stability following immediate placement and provisionalization of maxillary anterior single implants: a 2- to 8-year follow-up. Int J Oral Maxillofac Implants. 2011;26(1):179-187.