Use of a Novel ORMOCER as a Universal Direct Restorative Material
Foroud Hakim, DDS, MBA; and Jessie Vallée, DDS
Abstract: Composite resin is considered the material of choice for direct restoration of teeth when esthetic outcome is a high priority. While material science improvements have mitigated many of the traditional liabilities related to composite resin restorations, shrinkage and related shrinkage stress still play a role in outcomes, placement techniques, and overall success. This case report demonstrates two restorative scenarios using an ORMOCER® composite material. The first features a female patient who, upon completion of preliminary orthodontic treatment, determined in consultation with the orthodontist that her central incisors would present more idealistic display and esthetics if they were lengthened by approximately 1.5 mm. The lengthening of the incisors was to precede the phase II refinement with clear aligners, which would aim to extrude the remaining anterior teeth to develop incisal balance and symmetry. The second case is that of a woman who presented with a newly symptomatic upper right second bicuspid with an existing nearly decade old, large MODL composite resin restoration. This article demonstrates the universal nature of the novel direct restorative material used, making it well-suited for both anterior and posterior applications.
Traditional composite resins are composed of an organic methacrylate-based matrix (such as bisphenol A-glycidyl methacrylate [bis-GMA]), inorganic filler particles (such as silicon dioxide, ie, silica), a coupling agent, and a photoinitiator.Early generation composite resins were commonly categorized as “macrofills” and “microfills.” As the terms imply, this nomenclature referenced the relative particle size used as the native glass filler. The glass particles in these early composites were spherical in nature and homogenous. Each of these material classes were developed to be more suitable for particular restorative applications. Parameters like compressive strength, wear resistance, polishability, polish retention, solubility, translucency, and handling are what limited the suitability of either class of composite resin across both posterior and anterior tooth applications.
For example, compressive strength and wear are characteristics that can be sacrificed in an anterior restoration, whereas polishability, polish retention, translucency, and shading are highly desired. These esthetically driven characteristics could only be achieved with the small filler particles contained in a microfill. However, that same material likely could not hold up to the functional requirements of a posterior occlusal restoration, and, therefore, a macrofill composite would be used. These limitations were the impetus behind continuous research and development and material science progression toward a more universally viable composite material that could satisfy both the functional and esthetic requirements unique to posterior and anterior applications.
The chronological development of the ensuing composite material classes, including hybrids, microhybrids, and nanohybrids, has spanned from the 1980s to present day. Of these classes, nanohybrids allowed for the highest filler content while still maintaining high esthetic, physical, and mechanical properties due to the addition of “nanocluster” filler particles. These heterogenous nanoclusters increase compressive and flexural moduli and flexural strength while sustaining high polishability and surface luster. Most recently, the term “universal” has been used in an indiscriminate manner across many dental material classifications ranging from adhesives and bonding materials to substrate-related parameters, delivery techniques, and restorative materials. As it relates to composite resin, the term “universal” seems to imply that a material is equally well-suited for all restorative applications across anterior and posterior teeth.
Novel Direct Restorative
In recent years, a novel ORMOCER® (Fraunhofer Institute for Silicate Research ISC, isc.fraunhofer.de) (ORganically-MOdified-direct-CERamic)-based direct restorativewas introduced to the US market, intended for use across all traditional direct restorative applications. Silicone oxide is the foundational chemistry for an ORMOCER, not only for the nanofiller particles and glass-ceramics, but also the resin matrix. ORMOCERrestorativeis free of the classic monomers such as bis-GMA, triethylene-glycol-dimethacrylate (TEDGMA), or 2-hydroxy-ethyl-methacrylate (HEMA). The release of such substances after polymerization of composite resin has been a topic of recent concern, primarily with regard to neuropsychological development in children.1 Currently one ORMOCER-based direct restorative material is available on the market in the United States (Admira Fusion®, Voco Corp., voco.com).
This article presents two case reports in which the restorative scenarios demonstrate the suitability of the ORMOCER-based, universal direct restorative material for class IV and class II restorations and reviews the clinical steps for delivery.
Case Presentations
Case 1—Anterior
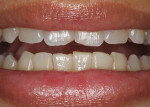
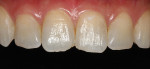
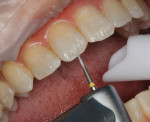
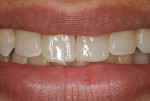
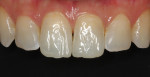
A 29-year-old woman presented with a chief complaint of incisal edge chipping and poor incisal display (Figure 1 and Figure 2). Having recently completed Invisalign® orthodontics (Align Technology, invisalign.com), the patient, in consultation with her treating orthodontist, sought to increase incisal display through a combination of restorative treatment followed by phase II Invisalign refinement.
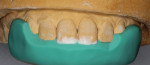
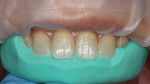
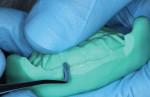
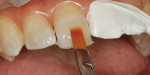
A silicone matrix was fabricated upon completion of a waxed proposal of the desired length increase for the central incisors (Figure 3 and Figure 4).2 The central incisors were prepared for the bonding procedure by irregular bevel placement with diamond instrumentation to aid in marginal blend (Figure 5).3 To maximize adhesive values, the prepared surfaces were air abraded with 50-µm aluminum oxide.4 Total etch with 37% phosphoric acid preceded application and light-curing of a universal adhesive (Futurabond U®, Voco Corp.).
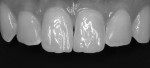
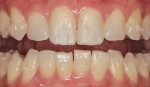
The ORMOCER restorative (Admira Fusion) was placed via a systematic lingual-to-buccal layering technique of the relevant universal (A1) and translucent (incisal and bleach) shades for optimal blending and optical characterization (Figure 6 and Figure 7).5-7 The restorations were shaped, finished, and polished using a conventional sequencing of instruments, including fluted carbides, finishing discs, silicone polishers, and abrasive brushes (Figure 8). Restoration of the right central incisor was completed first, and the steps were repeated for restoration of the left central incisor, and desired length increase was achieved (Figure 9 through Figure 11).
At the 1-year recall, the restoration showed excellent marginal integrity, high polish, and shade retention (Figure 12).
Case 2—Posterior
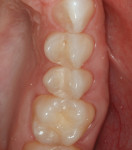
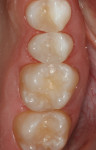
A 37-year-old woman presented with recent symptoms of pain upon chewing on the upper right second bicuspid. The tooth history included a moderately large MODL composite restoration that was placed more than 9 years prior. Clinical and radiographic examination showed evidence of possible delamination and fracture of the adhesive/restorative complex in the distal box form. The existing restoration (Figure 13) was removed with conventional rotary instrumentation and the tooth was prepared to restore.
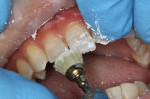
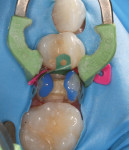
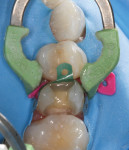
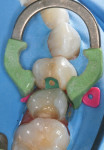
A decision was made to restore mesial and distal segments of the tooth separately due to sectional matrix band and ring placement limitations related to the local architecture. Selective-etch protocol was employed, followed by placement and cure of adhesive (Futurabond U) (Figure 14). Roughly 50% of the box depth was restored with a bulk-fill flowable resin (x-tra base®, Voco Corp.) to reduce the chance of void formation or marginal gapping due to instrument tug back (Figure 15).8 The occlusal portion of the preparation was systematically restored with the ORMOCERrestorative (shades A1 and incisal), which was layered for desired contour and 3-dimensional esthetics (Figure 16). Upon completion of filling, minimal contour and occlusal adjustments were made with rotary instrumentation, and final finish and polish was completed (Figure 17).
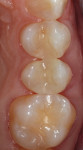
At the 8-month recall, the restoration showed no marginal breakdown, no signs of wear, and excellent polish and shade retention (Figure 18).
Discussion
Placement techniques for composite resin restorations have evolved over time. These protocols have been closely aligned with traditional material limitations. For example, traditional incremental layering and curing of composite restorations is recommended for a multitude of reasons. The primary reason to use an incremental layering technique is to reduce the impact of volumetric shrinkage and the resulting shrinkage stress.9 Placement of resin in increments of 2 mm or smaller has been the operating guideline for many years. Such shrinkage has been cited in the literature to be a causative factor in gap formation,10,11 marginal leakage,12 bond failure,13 and recurrent decay.14 The resulting shrinkage stress is said to result in sensitivity15 and cuspal deflection.16
These unwanted outcomes can be correlated to the volumetric shrinkage values attached to a given material. Early composite materials with lower filler volumes reported shrinkage values approaching 5%. Such values proved problematic, spurring material science improvements that led to progressively lower shrinkage values. These improvements have gradually become more subtle and incremental. Many contemporary composite resins now have values approaching or just below 2%. Material limitations related to resin seem to point toward the diminishing possibility of lowering these values any further.
While values near 2% seem to have mitigated some of the issues related to shrinkage and shrinkage stress, achieving a still lower shrinkage value would seem to be a desirable and logical objective, especially with the significant trend toward bulk-filling, whereby layering is expanded to the 4-mm to 5-mm level. The manufacturer of the ORMOCER-based restorative used in the cases presented reports a volumetric shrinkage value of 1.25% and a correlating shrinkage stress value of 3.7 MPa, representing a meaningful reduction in this adverse clinical characteristic encountered during light polymerization in both traditional and bulk-fill versions.17
Another key rationale for layering is cure depth limitations. When layers of greater than 2 mm are placed, curing-light output and material opacity contribute to unpredictable outcomes for bottom increment hardness and total conversion.18
Finally, layering is important when the esthetic outcome is deemed to be at a premium. The placement of incremental specialty shades of resin of varying opacities and optical characteristics allow practitioners to develop 3-dimensional shading and depth of color most resembling tooth structure.19
Conclusion
Incorporation of ORMOCER-based technology and silicon oxide into resin-based composites shows promise in enabling dentistry to make the next paradigm leap in the evolution of direct restorative material. The case studies presented herein demonstrate that an ORMOCER-based universal direct restorative, offering such characteristics as low shrinkage, low wear, high polishability, and optical esthetics, is an effective material to restore both anterior and posterior teeth to favorable function and appearance.
DISCLOSURE
Dr. Hakim occasionally receives honorarium support from Voco Corp. for ADA CERP lectures, and Voco also provides sample materials to his office for evaluation and testing, though he has no financial interest in the company. Dr. Vallée has no disclosures to report.
About the Authors
Foroud Hakim, DDS, MBA
Vice Chair, Department of Reconstructive Dental Sciences, University of the Pacific, Arthur A. Dugoni School of Dentistry, San Francisco, California
Jessie Vallée, DDS
Director of Preclinical Education, Department of Reconstructive Dental Sciences, University of the Pacific, Arthur A. Dugoni School of Dentistry, San Francisco, California
References
1. Maserejian N, Trachtenberg F, Hauser R, et al. Dental composite restorations and neuropsychological development in children: treatment level analysis from a randomized clinical trial. Neurotoxicology. 2012;33(5):1291-1297.
2. Sakai VT, Anzai A, Silva SM, et al. Predictable esthetic treatment of fractured anterior teeth: a clinical report. Dent Traumatol. 2007;23(6):371-375.
3. Aida A, Nakajima M, Seki N, et al. Effect of enamel margin configuration on color change of resin composite restoration. Dent Mater J. 2016;35(4):675-683.
4. Abdelaziz M, Rizzini AL, Bortolotto T, et al. Comparing different enamel pretreatment options for resin-infiltration of natural non-cavitated carious lesions. Am J Dent. 2016;29(1):3-9.
5. Fahl N Jr. Step by step approaches for anterior direct restorative challenges. J Cosmetic Dentistry. 2011;26(4):42-55.
6. Fahl N Jr. A polychromatic composite layering approach for solving a complex class IV/direct veneer-diastema combination: part I. Pract Proced Aesthet Dent. 2006;18(10):641-645.
7. Fahl N Jr. A polychromatic composite layering approach for solving a complex class IV/direct veneer/diastema combination: part II. Pract Proced Aesthet Dent. 2007;19(1):17-22.
8. Roggendorf M, Krämer N, Appelt A, et al. Marginal quality of flowable 4-mm base vs. conventionally layered resin composite. J Dent. 2011;39(10)3:643-647.
9. Relhan N, Ponnappa KC, Relhan A, et al. An in-vitro comparison of micro leakage between two posterior composites restored with different layering techniques using two different LED modes. J Clin Diagn Res. 2015;9(5):ZC78-ZC81.
10. Hilton TJ. Can modern restorative procedures and materials reliably seal cavities? In vitro investigations. Part 2. Am J Dent. 2002;15(4)279-289.
11. Hilton TJ. Can modern restorative procedures and materials reliably seal cavities? In vitro investigations. Part 1. Am J Dent. 2002;15(3):198-210.
12. He Z, Shimada Y, Tagami J. The effects of cavity size and incremental technique on micro-tensile bond strength of resin composite in Class I cavities. Dent Mater. 2007;23(5):533-538.
13. Kim RJ, Kim YJ, Choi NS, Lee IB. Polymerization shrinkage, modulus, and shrinkage stress related to tooth-restoration interfacial debonding in bulk-fill composites. J Dent. 2015;43(4):430-439.
14. Terry DA. Restoring the interproximal zone using the proximal adaptation technique—Part 2. Compend Contin Educ Dent. 2005;26(1):11-18.
15. Ivanović V, Savić-Stanković T, Karadzić B, et al. Postoperative sensitivity associated with low shrinkage versus conventional composites. Srp Arh Celok Lek. 2013;141(7-8):447-453.
16. Kwon Y, Ferracane J, Lee IB. Effect of layering methods, composite type, and flowable liner on the polymerization shrinkage stress of light cured composites. Dent Mater. 2012;28(7):801-809.
17. Admira Fusion ScientificCompendium. Cuxhaven, Germany: VOCO GmbH. https://www.voco.com/en/product/Admira-Fusion/SC_EN_Admira-Fusion.pdf. Accessed November 9, 2017.
18. Frauscher KE, Ilie N. Depth of cure and mechanical properties of nano-hybrid resin-based composites with novel and conventional matrix formulation. Clin Oral Investig. 2012;16(5):1425-1434.
19. Terry DA, Geller W. Selection defines design. J Esthet Restor Dent. 2004;16(4):213-225.