A Novel Method of Capturing Fluorescence in Clinical Dentistry
Yiannis Brokos, DDS, MSc, Dr. Med. Dent.; Minos Stavridakis, DDS, MSc, Dr. Med. Dent.; and Ivo Krejci, Prof. Dr. Med. Dent.
Abstract
Objectives: A fully integrated esthetic restoration should emit levels of fluorescence similar to that of natural dentition. Also, dental practitioners should be able to monitor this property in their routine clinical setting. The aim of this study was to investigate the efficacy of a removable filter for a macro flash illumination set-up required for the digital photographic recording of the fluorescence emission of human teeth and dental restorations. Methods: The traditional fluorescence capturing method in clinical dentistry, using continuous lighting, was compared with the proposed flash lighting method.A digital single-lens reflex Canon 550D camera with a Canon 100-mm macro lens and a commercially available standard Canon MT-24EX twin light macro flash were used in this study. A custom-fabricated plastic o-ring was fixed with silicone to the original flash framework, which received a removable fluorescence filter composed of two 365-nm ultraviolet (UV) glass filters on both sides, covering the flash lamps. The original protective plastic diffusers in front of the flash lamps were replaced with clear plastic to release the full excitation wavelength range of the xenon flash lamps. No additional filter was placed in front of the lens. Results: The results showed that using the proposed custom-made flash/filter illumination source, f-numbers between 16 through 22, a shutter speed of 1/60, and ISO 800 or 1600 sensitivity settings attained satisfactory fluorescent digital images. Results were comparable to those accomplished using a traditional photographic technique, without the need for a dark room, extended exposure times, and time-consuming set-ups. Conclusion: A contemporary photographic technique was demonstrated using macro flash UV-A 365-nm illumination that allowed fluorescent digital photograph acquisition under standard dental office conditions. Fluorescence documentation using a quick, straightforward procedure can take place during the restorative session to help increase the success rate of dental restorations.
As early as 1845, Sir John Herschel discovered the phenomenon of fluorescence in a solution of equal weights of sulphate of quinine and crystallized tartaric acid, rubbed together with the addition of water. Despite appearing colorless like water, when viewed by transmitted light the solution exhibited a beautiful celestial blue color in certain aspects and under particular incidents of light. The phenomenon was described in two separate papers but was not scientifically documented at that time.1,2 Several years later Irish physicist George Gabriel Stokes, inspired by Herschel's work, observed that the color of the emitted light had a longer wavelength spectrum than the color of the excited light; this difference became known as “Stokes shift.”3
In 1911 Hans Stubel was the first to report that rabbit teeth exhibited an intense blue fluorescence when irradiated with ambient ultraviolet (UV) illumination that was similar to that of the lens of the human eye.4 Benedict in 1928 noted that dentin fluoresces much more brilliantly with a bluish light than enamel, and that the white spot lesions indicative of the initiation of dental caries do not fluoresce, nor does ashed enamel. He also observed that the organic matrix retained its fluorescent power and suggested that fluorescence phenomenon might be useful for studying dental caries.5,6
Based on the these remarkable observations, fluorescence was defined as the optical property of teeth that emits color within visible light at 430 nm to 450 nm when irradiated with UV illumination at 1 nm to 400 nm. Initially, researchers attempting to investigate which tooth elements were responsible for the phenomenon addressed mainly the etiology of dental caries. During almost 50 years of research, some authors assumed that to some extent organic protein compounds were the reason for fluorescence,7-11 while others believed that fluorescence was linked with the mineral phase.12 Tooth enamel consists of approximately 96% mineral and 1% to 2% organic content, while dentin is composed of 30% to 40% organic matrix.13 The greater amount of organic content in dentin may explain the higher fluorescence dentin presents. Clinical tooth fluorometers were constructed14 and artificial UV illumination sources were used within in vitro experiments to observe fluorescence. “Dark bulb” mercury vapor lamps (ie, General Electric AH6, Hanovia Model 11) coupled with glass filters (ie, Corning no. 9863/no. 5860, Wood's filter) producing continuous lighting were among the combinations that enabled UV irradiation of the specimens in the range of 3200 arbitrary units (A.U.) to 3900 A.U., knowing that fluorescence of teeth was excited strongly around 3650 A.U.15-17
Besides the application of the fluorescence phenomenon in caries detection18-20 and other tissue diagnostics,21-25 another important aspect of fluorescence, revealed through the introduction of restorative materials in clinical dentistry, is its correlation with the optical properties of teeth26-30 and the potential of said materials to reproduce it. Ideally, restorative materials should exhibit similar levels of fluorescence to that of natural teeth; however, this is not the case, even with contemporary dental materials presenting variations in fluorescence emission.31-41 Fluorescence is considered a clinically significant optical property in esthetic restorations because it is why teeth appear whiter and brighter, emitting more light than they receive. Ambient UV irradiation emits autofluorescence that is responsible for the “vital” tooth appearance. Under specific artificial lighting, such as black lighting in a nightclub, for example, UV-coated lamps may emit the appropriate excitation light (300 nm to 400 nm) to induce fluorescence in teeth. Because dental restorations ideally should be indistinguishable from natural teeth, clinicians need to be capable of evaluating fluorescence in routine clinical settings.
Traditionally, use of a fluorescence capturing set-up was quite complicated. It required a UV light source and a dark room to avoid any other artificial lighting source in the operatory field to make the fluorescence visible, because the intensity of the fluorescence is very low. In addition, the photographic recording necessitated long exposure times of several seconds and increased ISO sensitivity of the sensor of the digital single-lens reflex (DSLR) camera resulting in increased picture noise, the need to stabilize the camera on a tripod, and significant irradiation of the patient with UV light.
The purpose of this study was to investigate the efficacy of a contemporary fluorescence capturing set-up consisting of a removable filter for UV flash illumination, along with a DSLR camera, macro lens, and twin light macro flash (Figure 1).
Materials and Method
Support system.An adjustable support system (Manfrotto Autopole, Manfrotto, manfrotto.us) was used to stabilize the photographic equipment when long exposures were needed. The product has a single-action cantilever locking system to assure a secure and balanced fit of the camera.
Camera. A DSLR camera body (Rebel T2i or EOS 550D, Canon, canon.com) was used for digital imaging in this study. The camera was equipped with an 18MP APS-C CMOS sensor coupled with DIGIC 4 image processor, having available ISO numbers ranging from 100 to 6400.
Memory storage.A SanDisk memory card (SanDisk, sandisk.com) with 8 GB capacity, C4 video speed, and SDCH form factor was used to temporarily store and transfer intraoral photographs to a personal computer.
Remote control.A wireless remote control (Canon RC-06, Canon) was used to avoid any camera movement while shooting.
Lens. An EF 100-mm f/2.8 Macro USM lens (Canon) was used for the camera set-up. F-numbers between f/2.8 and f/32 could be selected, and magnifications from 1:1 to 1:5 were used.
Continuous illumination source.Two black light halogen lamps (Supratec L18W/73, Osram, osram.com) 590 mm in length and 26 mm in diameter with long-wave radiation between 300 nm and 400 nm were attached on a metallic tray. The black light tubes were the only lighting source within the operatory field while digital imaging.
Flash illumination source.A MT-24EX Macro Twin Lite (Canon) flash unit was used for bilateral flash lighting. The flash weighs 585 g with 4 AA batteries. A custom-fabricated plastic o-ring with four metallic screws at 0o-90o-180o-270o was fixed with silicone to the original flash framework to support the UV-A filter (CNC machine).
UV-A 365-nm filter. A plastic framework that contained four magnets able to attach to the o-ring with the metallic screws was custom fabricated. On the plastic removable framework, two UV-A 365-nm glass filters (UG1 Schott optical filters, Schott AG, schott.com) were adapted on both sides to cover both flash lamps when attached to the o-ring. The protective plastic diffusers originally used to cover both flash lamps were carefully removed and replaced with clear plastic to protect and release the full excitation wavelength range of the xenon flash lamps from the initial visible spectrum of 400 nm to 700 nm to that of 300 nm to 800 nm. This procedure ensured the excitation range of the UV-A 365-nm glass filters. The flash combined with the attached filter controlled the UV irradiation source for both natural teeth and dental restorations.
Intraoral fluorescent images. A single-piece, self-retained lip retractor (KleerView™, Ultradent Products Inc., ultradent.com) was used to obtain a full view of the dentition in 1:2 magnification, including upper first molars.
Personal computer and software.A 27-inch iMac (Apple, apple.com) with 2.8-GHz Intel Core i5 processor and 4-GB 1333 MHz DDR3 memory was used to import and preview the captured intraoral images. Adobe Photoshop® software was used to analyze the images. No external card reader was required because the computer was equipped with the appropriate SDCH card slot.
Traditional set-up. The traditional set-up consisted of the camera DSLR body, macro lens, supporting system, remote control, and continuous illumination source. The patient was positioned horizontally. No other lighting source was switched on while shooting (Figure 2). The time consumed for the described set-up was approximately 10 minutes.
New set-up. The new set-up consisted of the camera DSLR body, macro lens, flash illumination source, and UV 365-nm filter. Neither patients' position nor the operatory lighting conditions were modified for the shooting (Figure 3). The time consumed for the described set-up was approximately less than 30 seconds.
Results
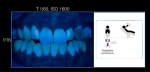
Results obtained with the traditional set-up are shown in Figure 4. The DSLR camera and the macro lens were stabilized on the supporting system. Using continuous illumination source, intraoral 1:2 pictures were captured under f-numbers varying from 8 to 16 and ISO numbers varying from 800 to 1600. The shutter speed was kept at 1/8 sec.
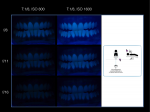
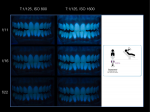
Results obtained with the new set-up are shown in Figure 5. The DSLR camera, macro lens, and the twin flash light were used to capture intraoral 1:2 pictures under f-numbers varying from 11 to 22 and ISO numbers varying from 800 to 1600. The shutter speed was kept at 1/125 sec. The best images were those with the following acquisition parameters: continuous illumination source, t 1/8-ISO 1600-f/11, t 1/8-ISO 800-f/8; and flash illumination source, t 1/125-ISO 1600-f/16, t 1/125-ISO 800-f/11. Other settings produced unacceptable images that were either underexposed, overexposed, or blurry.
Discussion
The purpose of this study was to examine the possibility of producing UV illumination using a custom-fabricated UV glass filter coupled with a commercial twin light flash device. The proposed set-up can be applied using virtually any commercially available flashing system. Considering that restorative materials emit varying fluorescence intensities compared to natural teeth, clinicians should strive to control fluorescence, both prior to and during the restorative session, to increase the success rate of the final restorations.
Unfortunately, the literature lacks documentation regarding technical aspects of a rapid and simple photographic application on fluorescence. The traditional fluorescence capturing set-up is highly detailed, requiring long exposure times (1/8, 1/15), low aperture numbers (f/8, f/11, f/16), and increased ISO sensor sensitivity (1600, 3200), and has the potential for producing intraoral images that are underexposed with increased noise. A determinant camera feature for quality intraoral image acquisition is the ISO index related to sensor sensitivity, with the necessary higher ISO settings resulting in increased grain of the captured image. An insurmountable shortcoming of the traditional technique is the amount of exposure time of both clinicians and patients to the continuous and harmful UV illumination; because of this it is highly recommended that during the exposure protective glasses and appropriate clothing for skin protection are used. UV flash light illumination is considered less harmful compared to continuous lighting sources due to the fact that the flash time is very limited.
The novel set-up used in this study offers greater convenience than the traditional set-up, as it utilizes camera settings similar to those applied in dental macro photography. Shorter exposure times (1/60, 1/125) negate the need for a tripod, while aperture numbers (f/11, f/16, f/22) coupled with decreased ISO sensor sensitivity (800, 1600) relative to the traditional technique result in highly satisfactory images with increased depth of field. The reduced amount of time needed for set-up, combined with the fact that there is no need for complete darkness, allows for usage of the proposed custom-made flash/filter illumination source during the restorative session. This enables the fluorescence level between natural tissues and dental restorations to be compared and adjustments made as needed.
With this novel technique, the custom-made flash modification and loss of warranty after replacing the plastic diffusers with clear plastic are factors to consider. However, the authors judge both issues as secondary in light of their advantages for both the practitioner and patient. The main objectives of this study were to explore the level of fluorescence utilizing a straightforward and quick procedure, while at the same time reviewing the technical aspects of the proposed low-cost photographic application.
Usage of a commercially available flash system with limited application in fluorescence emission has been recently proposed.41,42 Clinical studies have emphasized the importance of fluorescence as a fundamental aspect in the success of shade matching43 without discussing the capturing protocol applied and the impact on the daily practice workflow. This is why the present authors have focused on a multiple application concept using one single flash system, thereby minimizing overall equipment cost.44
Fluorescence is a form of luminescence. Ambient UV irradiation components, which are present in the sunlight spectrum (1 nm to 400 nm), are responsible for any fluorescent reaction of both natural tissues and dental restorations.45 This process that occurs during the day is apparent in fluorescent substances, showing vitality and brightness as part of living tissue. Any variation in emission levels is undesirable in the smile frame. Additionally, artificial lighting (eg, black light, nightclub settings) will produce the same fluorescence phenomenon and reveal possible shade mismatches. As previously discussed, natural dentin is much more fluorescent than enamel, and fluorescence is related with time and a patient's age. Dental restorative materials should, therefore, mimic natural structures in terms of shade and optical properties.Finally, practitioners should be able to control fluorescence, as well as other important optical properties such as metamerism, translucency, and opalescence, in a straightforward procedure without having to engage numerous devices.
Conclusion
A simplified, time-efficient macro flash illumination set-up using a UV-A 365-nm excitation filter allowing fluorescence emission and documentation was demonstrated. Such a filter may be easily attached in front of the flash under normal dental office working conditions in the same manner as standard clinical photography without the need for a dark room, extended exposure times, and time-consuming set-ups. Based on this approach, documentation can take place prior to restoration, during the restorative phase, and postoperatively. In direct adhesive procedures, refining the fluorescence level of the restorative material is necessary for increasing the esthetic success rate of composite restorations.
Disclosure
The authors had no disclosures to report.
About the Authors
Yiannis Brokos, DDS, MSc, Dr. Med. Dent.
Division of Cariology and Endodontology
University Clinics of Dental Medicine (CUMD)
University of Geneva
Geneva, Switzerland
Private Practice
Rhodes, Greece
Minos Stavridakis, DDS, MSc, Dr. Med. Dent.
Division of Cariology and Endodontology
University Clinics of Dental Medicine (CUMD)
University of Geneva
Geneva, Switzerland
Private Practice
Athens, Greece
Ivo Krejci, Prof. Dr. Med. Dent.
Division of Cariology and Endodontology
University Clinics of Dental Medicine (CUMD)
University of Geneva
Geneva, Switzerland
References
1. Herschel JF. On a case of superficial colour presented by a homogeneous liquid internally colourless. Philos Trans R Soc London. 1845;135:143-145.
2. Herschel JF. On the epipolic dispersion of light. Philos Trans R Soc London. 1845;135:147-153.
3. Stokes GG. On the change of refrangibility of light. Philos Trans R Soc London. 1852;142:463-562.
4. Stübel H. Die Fluoreszenz tierischer Gewebe in ultraviolettem Licht [in German]. Arch Ges Physiol. 1911;142:1-14.
5. Benedict HC. A note on the fluorescence of teeth in ultra-violet rays. Science. 1928;67(1739):442.
6. Benedict HC. The fluorescence of teeth as another method of attack on the problem of dental caries. J Dent Res. 1929;9:274-275.
7. Tiede E, Chomse H. Uber die luminescenz der zahne. Berichte der deutschen chemischen Gesellschaft (A and B Series). 1934;67(12):1988-1992.
8. Armstrong WG. Fluorescence characteristics of sound and carious human dentine preparations. Arch Oral Biol. 1963;8(2):79-90.
9. Shore VG, Pardee AB. Fluorescence of some proteins, nucleic acids and related compounds. Arch Biochem Biophys. 1956;60(1):100-107.
10. Armstrong WG. Ultra-violet spectrophotometric estimation of dentine protein in solution. Arch Oral Biol. 1962;7(6):771-772.
11. Armstrong WG. The presence of ultra violet absorbing material and its relation to fluorescence “quenching” effects in carious dentine. Arch Oral Biol. 1963;8(2):223-231.
12. Glasser J, Fonda GR. The fluorescence of double salts of calcium phosphate. J Am Chem Soc. 1938;60(3):722.
13. Mann A, Dickinson M. Nanomechanics, chemistry and structure at the enamel surface. In: Duckworth RM, ed. The Teeth and Their Environment. Monographs in Oral Science. 2006;19:105-131.
14. Hall JB, Hefferren JJ, Olsen NH. Study of fluorescent characteristics of extracted human teeth by use of a clinical fluorometer. J Dent Res. 1970;49(6):1431-1436.
15. Dickson G, Forziati A, Lawson ME Jr, Schoonover IC. Fluorescence of teeth: a means of investigating their structure. J Am Dent Assoc. 1952;45(6):661-667.
16. Hartles RL, Leaver AG. The fluorescence of teeth under ultraviolet irradiation. Biochem J. 1953;54(4):632-638.
17. Foreman PC. The excitation and emission spectra of fluorescent components of human dentine. Arch Oral Biol. 1980;25(10):641-647.
18. Kim HE, Kim BI. An in vitro comparison of quantitative light-induced fluorescence-digital and spectrophotometer on monitoring artificial white spot lesions. Photodiagnosis Photodyn Ther. 2015;12(3):378-384.
19. Lee ES, Kang SM, Ko HY, et al. Association between the cariogenicity of a dental microcosm biofilm and its red fluorescence detected by Quantitative Light-induced Fluorescence-Digital (QLF-D). J Dent. 2013;41(12):1264-1270.
20. Farah RA, Drummond BK, Swain MV, Williams S. Relationship between laser fluorescence and enamel hypomineralisation. J Dent. 2008;36(11):915-921.
21. Paolillo FR, Romano RA, de Matos L, et al. Fluorescence spectroscopy of teeth and bones of rats to assess demineralization: in vitro, in vivo and ex vivo studies. J Photochem Photobiol B. 2016;165:291-297.
22. Furuhashi K, Uo M, Kitagawa Y, Watari F. Rapid and non-destructive analysis of metallic dental restorations using x-ray fluorescence spectra and light-element sampling tools. Applied Surface Science. 2012;262:13-18.
23. Rüttermann S, Ritter J, Raab WM, et al. Laser-induced fluorescence to discriminate between a dental composite resin and tooth. Dent Mater. 2007;23(11):1390-1396.
24. Tani K, Watari F, Uo M, Morita M. Discrimination between composite resin and teeth using fluorescence properties. Dent Mater. 2003;22(4):569-580.
25. Bachmann L, Zezeli DM, da Costa Ribeiro A, et al. Fluorescence spectroscopy of biological tissues—a review. Applied Spectroscopy Reviews. 2006;41(6):575-590.
26. da Silva RD, da Silva MA, de Oliveira OB, et al. Dental fluorescence: potential forensic use. Forensic Sci Int. 2013;231(1-3):167-171.
27. Wilson HJ. Restorative materials and ultra-violet radiation. Br Dent J. 1969;126(8):345-346.
28. Kvaal S, Solheim T. Fluorescence from dentin and cementum in human mandibular second premolars and its relation to age. Scand J Dent Res. 1989;97(2):131-138.
29. Hafström-Björkman U, Sundström F, ten Bosch JJ. Fluorescence in dissolved fractions of human enamel. Acta Odontol Scand. 1991;49(3):133-138.
30. Lee YK. Fluorescence properties of human teeth and dental calculus for clinical applications. J Biomed Opt. 2015;20(4):040901.
31. Kim BR, Kang SM, Kim GM, Kim BI. Differences in the intensity of light-induced fluorescence emitted by resin composites. Photodiagnosis Photodyn Ther. 2016;13:114-119.
32. Meller C, Klein C. Fluorescence of composite resins: a comparison among properties of commercial shades. Dent Mater J. 2015;34(6):754-765.
33. Meller C, Klein C. Fluorescence properties of commercial composite resin restorative materials in dentistry. Dent Mater J. 2012;31(6):916-923.
34. Figueiredo C, Silva AM, Figueiredo A, Azenba ME. Fluorescence of dental composite resins. Experimental Pathology and Health Sciences. 2012;6(1):11-14.
35. Yu B, Lee YK. Differences in color, translucency and fluorescence between flowable and universal resin composites. J Dent. 2008;36(10):840-846.
36. Lim YK, Lee YK. Fluorescent emission of varied shades of resin composites. Dent Mater. 2007;23(10):1262-1268.
37. Aquiar Dos Reis RSA, Casemiro LA, Carlino GV, et al. Evaluation of fluorescence of dental composites using contrast ratios to adjacent tooth structure: a pilot study. J Esthet Restor Dent. 2007;19(4):199-207.
38. Lee YK, Lu H, Powers JM. Effect of surface sealant and staining on the fluorescence of resin composites. J Prosthet Dent. 2005;93(3):260-266.
39. Lee YK, Lu H, Powers JM. Changes in opalescence and fluorescence properties of resin composites after accelerated aging. Dent Mater. 2006;22(7):653-660.
40. Queiroz RS, Bandeca MC, Calixto LR, et al. Influence of the light-curing unit, storage time and shade of a dental composite resin on the fluorescence. Laser Physics. 2010;20(7):1647-1653.
41. Bazos P, Magne P. Bio-Emulation: biomimetically emulating nature utilizing a histoanatomic approach; visual synthesis. Int J Esthet Dent. 2014;9(3):330-352.
42. Hein S, Bazos P, Guadix JT, Naves LZ. Beyond visible: exploring shade interpretation. Quintessence of Dental Technology. 2014;37:199-211.
43. Gamborena I, Blatz MB. Fluorescence—mimicking nature for ultimate esthetics in implant dentistry. Quintessence of Dental Technology. 2011;34:1-17.
44. Brokos Y, Stavridakis M, Krejci I. Digital photographic procedure for comprehensive two-dimensional tooth shade analysis. Compend Contin Educ Dent. 2017; 38:8:e1-e4.
45. Matsumoto H, Kitamura S, Araki T. Autofluorescence in human dentine in relation to age, tooth type and temperature measured by nanosecond time-resolved fluorescence microscopy. Arch Oral Biol. 1999;44(4):309-318.