Long-term Stability of a Camouflage Retreatment of an Asymmetric Class III/Posterior Open Bite Using Sliding Jigs
Dauro Douglas Oliveira, DDS, MS, DScD; Bruno Franco de Oliveira, DDS, MS; Daniel Santos Fonseca Figueiredo, DDS, MS; Alberto Nogueira da Gama Antunes, PhD; and Paulo Isaías Seraidarian, DDS, MS, PhD
Abstract
This article reports the camouflage retreatment of an adult patient presenting an asymmetric Class III malocclusion and posterior open bite. Sliding jigs (SJs) associated with intermaxillary elastics were used. The long-term stability of the excellent results suggests that the use of SJs to correct asymmetric posterior occlusions may be effective.
Treatment of adult patients can be challenging for an orthodontist, especially when skeletal discrepancies, such as Class III malocclusion, are present that compromise facial esthetics and functional occlusion. The ideal treatment plan for such individuals often involves an orthodontic-surgical approach. However, the clinical challenge may become even greater when the patient refuses the surgical option, either for economic reasons or because he or she does not wish to be exposed to the inherent risks of an orthognathic surgery.1 This is why orthodontists must carefully consider the viability of an alternative treatment plan to overcome a malocclusion issue when the patient has mild or moderate skeletal disharmony and acceptable facial esthetics.2
The use of temporary anchorage devices (TADs) has been considered a relevant accessory for the treatment of moderate skeletal malocclusion, facilitating the orthodontic mechanics.3,4 However, TADs may not be an option in a limited number of patients because of anatomical limitations.5,6 Thus, the aim of this article is to report the treatment of an asymmetrical skeletal Class III malocclusion in a patient who also had a bilateral posterior open bite using sliding jigs (SJs) when neither an orthodontic-surgical approach nor the use of TADs was possible.
Diagnosis and Etiology
A 25-year-old male patient had been seeking orthodontic retreatment with the following chief complaint: During the last year of his initial orthodontic treatment, his lower jaw “grew a lot,” his face became asymmetric, his bite worsened, and since then he had been unable to chew properly. The patient reported that his previous orthodontist was surprised by the amount of jaw growth and the asymmetric direction of his mandibular growth during the last stages of that treatment.
At that point, asymmetric intermaxillary elastics were used to control the problem. However, the therapy was unsuccessful and resulted in temporomandibular dysfunction. The patient, who was a dental student when he sought retreatment, was quite aware of his facial asymmetry. His concern was not with the asymmetry, but rather he wanted to improve his severely compromised occlusion to reestablish better function.
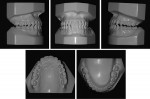
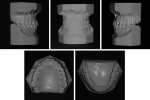
Facial analysis showed moderate asymmetry with a mandibular deviation to the left (Figure 1). He showed good exposure of maxillary incisors when smiling, but there was a mild cant of the maxilla; thus no gingiva was exposed in the left posterior region upon smiling. The face presented good vertical proportions, and the profile was slightly concave with a deficient midface and normal nasolabial angle.
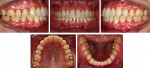
The intraoral examination revealed molar and canine Class III relationship on the right side and Class II on the left side (Figure 2 and Figure 3). There was also a bilateral posterior open bite on both sides and his only posterior contact was between the molars from the right side. The upper midline was coincident to the facial midline, and the lower midline was 3 mm deviated to the left. Both dental arches presented adequate forms. There was no crowding and +1 mm model discrepancy in the lower arch. The Bolton analysis showed 1.5 mm anteroinferior excess, and the periodontal conditions were satisfactory. The temporomandibular disorder previously had been treated with a mandibular splint. At this time there were no more signs or symptoms, and the condyles were positioned in centric relation (Figure 2 and Figure 3). Thus, the patient was already able to begin orthodontic retreatment.
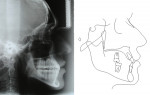
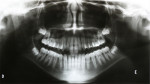
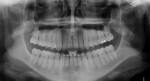
Lateral cephalometric evaluation (Figure 3) confirmed the clinical findings of a moderate skeletal Class III (ANB = -1 degree) and normal vertical dimension (SN-GoGn = 36 degree, FMA = 27 degrees). Maxillary incisors were not proclined (U1-SN = 106 degrees), but were protruded (U1-NA = 8 mm). The mandibular incisors were moderately retroclined (IMPA = 83 degree). Both lips were well positioned in reference to the E-plane (U-lip to E-plane = -7 mm, L-lip to E-plane = -3 mm). Panoramic radiograph showed overall adequate alveolar bone levels and presence of all teeth, including the third molars (Figure 4). However, at the beginning of the present authors’ orthodontic retreatment, the germ of the third molar was no longer present; its extraction was indicated by the previous dentist. The ABO discrepancy index of this case was 35.
Treatment Objectives
The ideal treatment objectives were: correct the facial asymmetry and the cant of the upper occlusal plane, obtain skeletal and dental Class I relationships, close the bilateral posterior open bite to adequately restore the occlusion contacts, and correct the lower midline deviation. Meeting these objectives would make it possible to improve both the facial esthetics and masticatory function.
Treatment Alternatives
The first treatment plan presented to the patient comprised all ideal goals. The only treatment option that would correct his skeletal asymmetry was an orthodontic-surgical approach. The surgical procedure would include an asymmetrical maxillary impaction to correct the cant of the upper occlusal plane and an asymmetrical mandibular setback to correct the facial asymmetry. However, the patient rejected this alternative because of the high costs, risks, and possible complications involved with an orthognathic surgery. Most importantly, though, was the fact that the facial asymmetry was not part of his chief complaint and, accordingly to him, did not negatively influence his self-esteem or social life.
The second treatment alternative was the use of upper and lower fixed appliances associated with SJs on the lower arch to move tooth-by-tooth the right teeth distally and the left teeth mesially, camouflaging the skeletal problems, removing the premature contacts, and providing the correct cusp-to-fossa intercuspation. Consequently, posterior bite closure and improvement of occlusal function would be obtained. The SJs would be anchored in TADs because orthodontic camouflage would require significant amounts of tooth movement. Additionally, the use of TADs would reduce the need for patient cooperation. However, the patient contended that he would like to explore the least expensive treatment alternative.
Therefore, a third treatment option that would be economically realistic was considered. It would involve the use of SJs with intermaxillary elastics and no TADs. The patient was informed that this option would require impeccable cooperation with the use of the elastics and that no improvement in his facial asymmetry would be achieved. Conversely, it would be the least expensive and invasive of the treatment plans. The patient understood the limitations of this treatment alternative, assumed the responsibility for adequate elastic wear, and selected this last treatment option before signing an informed consent authorizing the treatment.
Treatment Progress
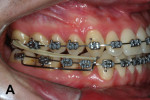
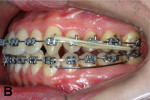
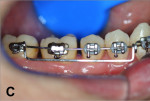
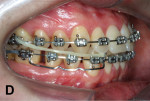
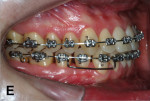
Upper and lower metallic brackets were bonded from R7 to L7 on both arches (0.022-in x 0.028-in, Mini-Master Series, American Orthodontics, americanortho.com). The incisors’ brackets presented MBT prescription, and from 3s to 7s the brackets were standard edgewise. Leveling and alignment progressed up to a 0.019-in x 0.025-in stainless steel (SS) wire on the maxillary arch and to a 0.018-in SS in the mandibular. The purpose was to use a heavier wire for anchorage on the maxilla and a thinner lower wire to provide less friction on the mandible. A 0.019-in x 0.025-in SS SJ was bent and inserted on the right side to apply a distal force directly to the LR7 (Figure 5). On the left side a similar SJ was inserted, but to obtain a mesial movement of LL3 (Figure 6).
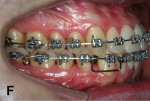
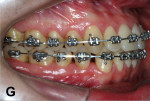
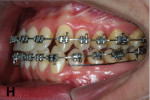
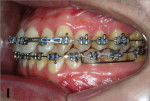
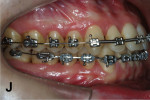
Two months later, LR7 reached a Class I relationship and there was a spontaneous distal drifting of LR6, creating a total of 2 mm of space between LR6 and LR5 (Figure 7). Thus, a new 0.018-in SS with an omega loop bent flush to the mesial surface of the LR7 tube was inserted. The SJ was moved forward to apply a distal force to LR6. After 2 more months, LR6 reached a Class I relationship (Figure 8). A steel ligature was used to tie together LR7 to LR6 to prevent relapse, and the SJ was moved forward to LR5 (Figure 9) and posteriorly to LR4 (Figure 10) after another 1 and 2 months, respectively. Shortly after, LR3 was moved distally with an elastic chain (Figure 11).
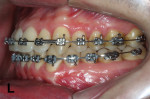
On the left side, after 7 months of using the SJ to move LL3 mesially, the canine was almost in Class I (Figure 12). After positioning the LL3 in Class I, the SJ was moved backward to also bring LL4 mesially. After that, the SJ was maintained to reinforce anchorage while LL5 and LL6 were moved mesially with an elastic chain (Figure 13).
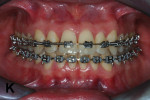
After a Class I relationship was obtained on both sides, the SJs were removed and the midline deviation was corrected. The patient was oriented to wear bilateral triangular ¼ M” elastics to maintain the occlusion achieved. The spaces in the anterosuperior region were properly redistributed and preserved with closed springs. The maxillary lateral incisors received composite build-ups to increase their width, thus eliminating the Bolton discrepancy and consolidating the achievement of a correct overjet (Figure 14 through Figure 16).
Six months prior to the end of treatment, a panoramic radiograph was obtained to check for root parallelism and the brackets of those teeth that needed to correct their axial inclination were rebonded. The total duration of the entire treatment was 32 months.
Treatment Results
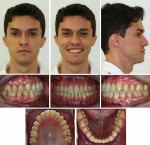
The realistic treatment objectives established with the third option presented to the patient were achieved, including improvement mainly in the occlusion and also in dental esthetics (Figure 17), fulfilling the patient’s expectations. The facial features were maintained because of the inherent treatment limitations without the benefits of an orthognathic surgery.
The final occlusal result achieved was excellent (Figure 18) as confirmed with the patient’s total ABO cast-radiograph evaluation score of 11.7 Class I relationship for both the canines and molars was obtained on both sides and appropriate overbite and overjet were achieved. Adequate arch coordination and intercuspation were obtained, with improvement of midline deviation and closure of the bilateral posterior open bite. The patient reported significant improvement in masticatory function, increased muscular comfort post-treatment, and absence of any symptoms in the temporomandibular joints.
Cephalometric analysis and superimpositions (Figure 19) showed a small mandibular rotation in a counter-clockwise direction and a decrease in lower facial height (SN-GoGn from 36 degrees to 33 degrees, FMA from 27 degrees to 26 degrees). The ANB decreased due the mandible rotation (-1 degrees to -2 degrees). The retro-inclination of the mandibular incisors was slightly improved (IMPA from 83 degrees to 86 degrees). The maxillary incisors were moderately proclined (U1-SN from 106 degrees to 112 degrees). Panoramic radiograph evaluation showed adequate root parallelism (Figure 20).
The retention protocol consisted of a bonded lower 3x3 and a wrap-around Hawley retainer. The patient was orientated to wear the upper retainer full-time for the first 6 months and at night after the first semester without fixed appliances. The results remained stable 4 years post-treatment (Figure 21).
Discussion
Orthodontists often must perform realistic rather than idealistic treatment plans, especially when dealing with adults.8,9 Based on the significant facial asymmetry and consequent malocclusion, the idealistic and first treatment plan proposed to the patient was the combination of fixed orthodontic appliances and orthognathic surgery. This interdisciplinary approach would provide significant benefits such as improved facial esthetics, better masticatory function, and decreased potential for relapse.10,11 However, it also had disadvantages, such as high financial costs, risk of surgical complications, vascular or nervous damages, infection, osseous necrosis, ophthalmic alterations, dysphagia, and psychological problems.1 For these reasons and because the facial asymmetry did not cause any esthetic discomfort, the patient chose to reject the surgical option.
Therefore, a second, more realistic treatment plan alternative was proposed that utilized SJs associated with TADs. These anchorage devices are often used in cases of orthodontic camouflage.3,4,12,13 However, the patient needed to minimize costs and asked if yet another alternative was available. Thus, a third option was proposed that also involved the use of SJs; however, it was associated with the use of intermaxillary elastics.
The patient was informed that this last option would not improve the facial asymmetry and would require impeccable cooperation with regard to the use of elastics. Despite these disadvantages, the patient accepted this more realistic treatment plan. Throughout treatment, the patient used the elastics precisely as requested, which was indispensable to the success achieved with the treatment. Orthodontic treatment in adults imposes some limitations such as the lack of craniofacial growth, missing or abraded teeth, old restorations, and periodontal sequelae, but adults usually cooperate better than teenagers do.8,9,14
The patient maintained high enthusiasm and excellent cooperation throughout the entire treatment. The use of skeletal anchorage has truly changed the paradigm of orthodontic mechanics,15,16 but well-used classical mechanics and a cooperative patient may be as effective as skeletal anchorage in some situations.
When facing an asymmetric malocclusion, as described in this case report, many orthodontists may use intermaxillary elastics for en-masse movement of the entire arch, usually asking the patients to use Class II elastics on one side, Class III elastics on the other side, and anterior diagonal elastics.17,18 However, this strategy of mechanics may cause the rotation of the entire arch, potentially causing cross-bite and interarch disharmony.17 This unwanted side effect may occur because the entire arch would rotate around its center of resistance.17
Ideally, application of lighter forces and movement of the teeth around the arch like pearls on a chain would be recommended.17 The mechanical strategy the authors employed to move the mandibular teeth around the arch was the use of SJs and intermaxillary elastics. In the early days of orthodontic specialty, Tweed19 was the first to describe the use of this approach. Though it is an older strategy, it presents some noteworthy advantages. It requires lighter forces due to tooth-by-tooth movement, causing potentially fewer side effects than when intermaxillary elastics are used to move many teeth simultaneously.20 A well-trained orthodontist can custom-bend SJs within minutes. However, those who believe that bending accessories is not efficient may consider the use of prefabricated jigs. The main disadvantage of the mechanics presented in this case report is the great need for patient cooperation when using the elastics. If the patient is unwilling to cooperate, the use of SJs should be associated with TADs.21
Another challenge of the treatment reported was the closure of the extensive posterior open bite without surgical assistance. This was the main cause for the patient’s chief complaint, because it was responsible for the masticatory difficulty. The patient had occlusal contact only on the right molars and the incisors. His bite closure was gradually occurring with the movement of the lower teeth. This resulted in the removal of the occlusal interferences, allowing a proper cusp-fossa intercuspation. Combined with this fact, the discrete projection of upper teeth obtained from the alignment and leveling phase also contributed to the elimination of anterior interference, allowing mandibular counter-clockwise rotation, as observed in the superimpositions. Although this type of mandibular rotation is not desirable in the treatment of Class III patients, it was important to obtain the closing of the bite and reestablishment of the occlusal harmony. Furthermore, facial evaluation showed no significant change in profile concavity at the end of treatment.
Because of the initial complexity of the case, a nonsurgical approach could lead to a questioning of its long-term stability.11 However, evaluation 4 years after treatment showed excellent stability of the results obtained. Often, professionals look for new techniques and technologies in an attempt to offer optimal solutions for patients. However, the basic or classical mechanics should not be overlooked, as in some cases they may provide sound solutions to complex problems.
Conclusion
The use of SJs can be an effective approach to camouflage asymmetric malocclusions. This method offers a minimally invasive and low-cost technique. When a patient is willing to cooperate with elastic wear, this simple and somewhat “forgotten” approach to orthodontic mechanics may be a good alternative even for complex cases.
About the Authors
Dauro Douglas Oliveira, DDS, MS, DScD
Associate Professor
Program Director of Orthodontics
Pontifical Catholic University of Minas Gerais
Belo Horizonte, Brazil
Bruno Franco de Oliveira, DDS, MS
Former Prosthodontics resident
Pontifical Catholic University of Minas Gerais
Belo Horizonte, Brazil
Daniel Santos Fonseca Figueiredo, DDS, MS
PhD student, School of Dentistry
Pontifical Catholic University of Minas Gerais
Belo Horizonte, Brazil
Alberto Nogueira da Gama Antunes, PhD
Associate Professor of Prosthodontics
Pontifical Catholic University of Minas Gerais
Belo Horizonte, Brazil
Paulo Isaías Seraidarian, DDS, MS, PhD
Associate Professor of Prosthodontics
Pontifical Catholic University of Minas Gerais
Belo Horizonte, Brazil
References
1. Panula K, Finne K, Oikarinen K. Incidence of complications and problems related to orthognathic surgery: a review of 655 patients. J Oral Maxillofac Surg. 2001;59(10):1128-1136.
2. Troy BA, Shanker S, Fields HW, et al. Comparison of incisor inclination in patients with Class III malocclusion treated with orthognathic surgery or orthodontic camouflage. Am J Orthod Dentofac Orthop. 2009;135(2):146.e1-e9.
3. Kaku M, Kawai A, Koseki H, et al. Correction of severe open bite using miniscrew anchorage. Aust Dent J. 2009;54(4):374-380.
4. Jing Y, Han X, Guo Y, et al. Nonsurgical correction of a Class III malocclusion in an adult by miniscrew-assisted mandibular dentition distalization. Am J Orthod Dentofac Orthop. 2013;143(6):877-887.
5. Watanabe H, Deguchi T, Hasegawa M, et al. Orthodontic miniscrew failure rate and root proximity, insertion angle, bone contact length, and bone density. Orthod Craniofac Res. 2013;16(1):44-55.
6. Kuroda S, Yamada K, Deguchi T, et al. Root proximity is a major factor for screw failure in orthodontic anchorage. Am J Orthod Dentofac Orthop. 2007;131(suppl 4):S68-S73.
7. Casko JS, Vaden JL, Kokich VG, et al. Objective grading system for dental casts and panoramic radiographs. American Board of Orthodontics. Am J Orthod Dentofacial Orthop. 1998;114(5):589-599.
8. Kokich VG. Create realistic objectives. Am J Orthod Dentofac Orthop. 2011;139(6):713.
9. Kokich VG, Spear FM. Guidelines for managing the orthodontic-restorative patient. Semin Orthod. 1997;3(1):3-20.
10. McCollum AGH, Gardener GJM, Evans WG, Becker PJ. Soft-tissue changes related to mandibular advancement surgery. Semin Orthod. 2009;15(3):161-171.
11. Baik HS. Limitations in orthopedic and camouflage treatment for Class III malocclusion. Semin Orthod. 2007;13(3):158-174.
12. He S, Gao J, Wamalwa P, et al. Camouflage treatment of skeletal Class III malocclusion with multiloop edgewise arch wire and modified Class III elastics by maxillary mini-implant anchorage. Angle Orthod. 2013;83(4):630-640.
13. Qamruddin I, Shahid F, Alam MK, et al. Camouflage of severe skeletal class II gummy smile patient treated nonsurgically with mini implants. Case Rep Dent. 2014;2014:382367.
14. Kokich VG. Adult orthodontics in the 21st century: guidelines for achieving successful results. World J Orthod. 2005;6(suppl):14-23.
15. Leung MT, Lee TC, Rabie AB, Wong RW. Use of miniscrews and miniplates in orthodontics. J Oral Maxillofac Surg. 2008;66(7):1461-1466.
16. Ellouze S. Mini-implants: pushing the limits of traditional orthodontics. Orthod Fr. 2008;79(1):59-66.
17. Burstone CJ. Diagnosis and treatment planning of patients with asymmetries. Semin Orthod. 1998;4(3):153-164.
18. Burstone C, Filleul MP, Pigeot V. Stability of orthodontic treatment of occlusal asymmetry. Orthod Fr. 2000;71(3):197-205.
19. Tweed CH. Clinical Orthodontics. 6th ed. St. Louis, MO: Mosby; 1999.
20. Janson G, Sathler R, Fernandes TMF, et al. Correction of Class II malocclusion with Class II elastics: a systematic review. Am J Orthod Dentofac Orthop. 2013;143(3):383-392.
21. de Oliveira Ruellas AC, Pithon MM, dos Santos RL. Evaluation of the mechanical behaviour of different devices for canine retraction. Dent Press J Orthod. 2012;17(3):83-87.