Ten Myths of Guided Implant Surgery
Gary Orentlicher, DMD; Andrew Horowitz, DMD, MD; Batya Goldwaser, DMD, MD; and Marcus Abboud, DMD
Abstract
Since their introduction, guided dental implant planning and surgery procedures, like most new techniques in medicine and dentistry, have undergone many modifications and advances. While some practitioners were early adopters, most dental surgeons have been cautious regarding this methodology. Despite more than a decade of literature, podium presentations, advances in instrumentation and technique, and successful cases, questions remain within the dental surgical community. This article attempts to address some of these by outlining common but erroneous beliefs about this technology and procedure.
Conventional freehand implant surgery has been taught, performed, modified, and refined by dental implant surgeons since the introduction of the first osseointegrated dental implants. Computed tomography (CT)-guided implant surgery was first introduced in the early 2000s. Guided implant surgery involves a reverse engineering workflow, first establishing the ideal position and morphology of the planned restoration, then virtually planning the ideal position of the dental implant(s) according to that restoration.1 Surgical guides are then produced to aid the surgeon in placing the implants accurately, according to the virtual plan. Surgical instrumentation, produced by most major dental implant manufacturers, is available to create osteotomies and place guided implants.
Since their introduction, guided dental implant planning and surgery techniques have undergone many modifications and advances. Some practitioners were early adopters of this technology, but many have been more wary, and some confusion seems to remain within the dental surgical community. This article will address some of the questions and what the authors consider to be “myths” regarding this technology and procedure.
Myth #1:
Guided surgery is an easier way to place a dental implant.
Guided surgery is not an easier way to place a dental implant; it is a more accurate way.2-4 Guided surgery is an advanced implant placement technique and is not recommended for novice implant surgeons. A high level of training, experience, and skill is required to master the techniques and workflows. It is an endeavor for experienced implant surgeons who are willing to invest the time and money necessary to learn the techniques.
Myth #2:
Guided surgery increases clinical time efficiency.
For a clinician who masters guided surgery techniques and instrumentation, chairside time efficiency can increase significantly. This improved efficiency is most obvious in multiple-implant and full-arch reconstructive patient cases. However, overall, guided surgery does not reduce treatment time, as additional time is spent on planning rather than the treatment itself. Taking impressions, wax-ups, and cone-beam computed tomography (CBCT) and optical scans; importing digital imaging and communications in medicine (DICOM) images; and conducting virtual treatment planning are all time-consuming activities.
Myth #3:
Guided surgery is primarily indicated for more challenging cases.
Though many consider guided surgery to be reserved only for difficult cases, in the authors’ experience once clinicians have invested the time and resources into learning the techniques and acquiring the instrumentation, guided surgery alters the way they view a case, whether simple or complex. Although the first guided surgery workflows were developed for implant placement in fully edentulous patients and were given elaborate immediate-load marketing terms that implied teeth could be produced in as little as an hour, many patients who are partially edentulous and/or need only a single implant can benefit from guided surgery. This technique can be used for the replacement of a single tooth or for partially edentulous patients in addition to fully edentulous ones, with or without immediate load. If desired, techniques and armamentarium are available for the fabrication of provisional restorations in all types of cases, before guided implant insertion, for insertion immediately after implant placement.
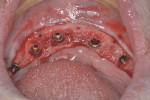
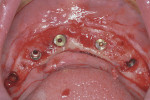
Placement of implants using guided surgery can be performed fully guided or using pilot guides. Fully guided placement involves osteotomies and implant placement, using implant-specific guided surgery instrumentation, to final depth and angulation, through the surgical guide. Use of pilot guides is an option that simplifies case planning and implant placement by establishing the initial osteotomy depth and angulation without requiring fully guided instrumentation. Final implant placement is then done freehand using conventional instrumentation (Figure 1 and Figure 2).
Myth #4:
Guided surgery techniques are similar to conventional implant surgery techniques.
Although placing an implant by using sequential burs to enlarge an osteotomy is common to both conventional and guided surgery implant placement, the surgical instrumentation and techniques are significantly different. An intimate knowledge and understanding of the principles and surgical instrumentation that are unique to guided surgery is necessary before treating patients. Drill guides, implant mounts, drill stops, altered drilling sequencing, different burs, and instrumentation specific for component removal are some of the unfamiliar instrumentation clinicians should understand (Figure 3). Most major implant manufacturers now have guided surgery instrumentation trays specifically designed for their implants (Figure 4 and Figure 5). Some manufacturers have implants packaged specifically for guided surgery placement (Figure 6). Techniques and instrumentation are available for both pilot (2-mm to 2.2-mm burs only) osteotomies and fully guided placement of dental implants.
Before performing guided surgery, implant surgeons must be comfortable with conventional implant placement techniques in the event that a case initially planned for guided surgery must be converted to one using conventional methods. For example, this may occur if surgical guides do not fit properly at surgery or if a patient cannot adequately open his or her mouth to accommodate the guided surgery instrumentation.
Myth #5:
I am smarter than the guided surgery workflows, so I can skip steps.
Dentists generally try to develop treatment methods to minimize steps and maximize efficiency while treating patients. When using guided surgery, skipping steps should be avoided during the workup and treatment of patients. Errors made in guided surgery are both additive and cumulative. Workflows from most manufacturers are well established for all types of cases. Attention to detail from all team members (eg, laboratory, restorative, and surgical) is necessary in each step of the workflow to minimize error and maximize accuracy and patient outcomes.
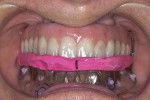
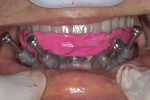
One step that is sometimes skipped is the use of bite registrations to accurately position scanning appliances during scans and to position surgical guides to be used for implant insertion. Neglecting to use bite registrations can lead to inaccuracy in both the placement of a scanning appliance and in the positioning of the surgical guide at surgery, leading to potential errors in planning and implant placement. The use of bite registrations must be included in the protocol, especially in cases involving fully edentulous patients (Figure 7 and Figure 8).
Myth #6:
In guided surgery, CBCT scans are of equal accuracy and quality to medical CT scans.
Sir Godfrey Hounsfield developed medical multi-slice CT (MSCT) in 1967.5 CBCT was introduced in the European market in 1996 and in the US market in 2001.6 MSCT has long been relied upon for one-to-one accuracy in 3-dimensional (3D) radiography; however, MSCT radiation exposure, as compared with CBCT, has been measured to be 10 to 20 times greater.7 The question is whether the benefit of increased accuracy outweighs the risk for increased radiation exposure.
Abboud and colleagues8 scanned objects of a known diameter with one MSCT scanner and five CBCT scanners. They concluded that MSCT devices provided the most accurate images in the study, but the amount of the differences may not have been of clinical significance for most diagnostic purposes. They did note that fiducial marker localization error caused by some CBCT scanners could be a problem for some guided surgery systems. Liang and coworkers9 compared the geometric accuracy of 3D surface model reconstructions created by images produced by five CBCT scanners and one MSCT system. They concluded that the accuracy of the CBCT 3D surface model reconstruction was somewhat lower as compared with MSCT, but acceptable.
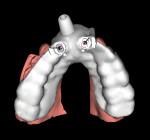
Bone density in MSCT is measured in Hounsfield units (HU). Bone density in CBCT is measured in voxels, a visual gray scale measurement (a 3D pixel). There is no correlation between HUs and voxels. Most dental implant treatment planning software was developed for MSCT, not CBCT. This is why, when using CBCT and importing DICOM image data into proprietary implant planning software, 3D reformation images of less radio-dense areas of bone, such as the maxilla, appear with radiolucent openings, or “holes,” in the bony surfaces (Figure 9 and Figure 10). One could conclude that, when weighing the slight amount of additional inaccuracy along with the potential 3D reformation issues of CBCT against the considerably increased radiation dosage of MSCT, CBCT is an excellent option for dental implant evaluation and placement and guided surgery planning.
Myth #7:
Insertion torque measurements are accurate when using guided surgery.
When using guided surgery for implant insertion, the clinician experiences less tactile sense of the bone density. The surgical guide directs the bur and implant insertion componentry to the planned depth and angulation without consideration of the bone density or tactile resistance. In addition, friction occurs from contact between componentry used in drilling osteotomies (eg, guide sleeves/drill guides and burs) and placing implants (eg, guide sleeves and implant mounts). This all leads to inaccuracy in insertion torque measurements when measuring torque while the surgical guide is in place. Insertion torque of an individual implant can be measured only after the implant has been placed into its final position through the surgical guide, after the guide is removed.
Myth #8:
Bone overheating is of more concern in guided surgery than conventional implant surgery.
Bone overheating is contraindicated in all cases of dental implant surgery. Because of the presence of an intimately fitting surgical guide and insertion instrumentation, questions have arisen about whether cooling irrigation is able to reach the osteotomy site when using guided surgery; if it is not, overheating the bone becomes a concern. Migliorati and colleagues10 studied the internal bone temperature changes registered during guided surgery preparations. They concluded that when using surgical stents, osteotomy preparation generated higher bone temperatures than did conventional drilling. The heat generation, however, did not reach temperature levels that were dangerous to the bone.
Myth #9:
Guided surgery cannot be used in tilted implant/hybrid restoration cases.
The goal of guided surgery is to allow the clinician to avoid vital anatomic structures while placing implants in proper positions, angulations, and depths according to the planned restoration. These two concepts are important considerations in planning and performing “tilted” implant/hybrid restoration cases.
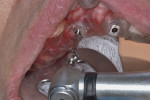
Combining guided surgery and tilted/hybrid cases appears as if it should be a natural marriage of techniques. The questions that arise about the use of guided surgery in these cases are regarding the bone reduction frequently necessary to place implants appropriately, both surgically and restoratively. Some manufacturers have developed bone reduction guides based on virtual treatment plans. Other methods for establishing bone reduction involve using guide pins to mark levels of bone to be removed or the use of the intentional deep placement of the implant to the level of the bone to be reduced (Figure 11 and Figure 12). With proper planning and forethought, guided surgery can be performed relatively easily on tilted implant/hybrid cases.11
Myth #10:
The success rate of guided-placed implants is lower than those placed conventionally.
As stated earlier, many practitioners consider the use of guided surgery only for more difficult implant cases, such as full-arch or multiple-implant cases, or those involving limited bone volume, anatomic issues, difficult prosthetic considerations, trauma, extensive grafting, or cases that encompass medical, orthopedic, or psychological issues with the patient. Given the inherent problems with these types of cases, combined with some of the aforementioned issues associated with guided implant placement, such as the overheating and cooling questions, the inability to accurately measure insertion torque, the diminished clinician tactile sense, and fully guided implant placement with or without a flap being essentially a blind procedure, one might think that the cumulative survival rate (CSR) of implants placed with this technique would be lower than those placed conventionally. This has not been found to be the case, however. In a 7-year retrospective study of 798 implants placed fully guided using different software and implant systems, the authors reported a CSR of 96.98%. Compared with the well-established CSR of 95% to 98% for conventional freehand placement of implants, the CSR of implants placed using fully guided protocol is not lower.12
Conclusion
Guided surgery techniques have been researched and refined for many years and can be used in most clinical scenarios. Attention to detail is necessary in all steps to minimize potential errors, as consistent success requires a solid knowledge and understanding of treatment workflows and armamentarium. The successful integration of guided surgery into practice can lead to improved patient outcomes, which is the ultimate goal of treatment.
About the Authors
Gary Orentlicher, DMD
Section Chief
Division of Oral and Maxillofacial Surgery
White Plains Hospital
White Plains, New York
Private Practice
New York Oral, Maxillofacial, and Implant Surgery
Scarsdale, New York
Andrew Horowitz, DMD, MD
Associate Attending
White Plains Hospital
White Plains, New York
Private Practice
New York Oral
Maxillofacial, and Implant Surgery
Scarsdale, New York
Batya Goldwaser, DMD, MD Attending Oral and Maxillofacial Surgeon,
White Plains Hospital
White Plains, New York
Private Practice
New York Oral
Maxillofacial, and Implant Surgery
Scarsdale, New York
Marcus Abboud, DMD
Associate Dean of Digital Dentistry
University of Kentucky College of Dentistry
Lexington, Kentucky
References
1. Orentlicher G, Horowitz A, Abboud M. Minimally invasive implant surgery using computer-guided technology. In: Minimally Invasive Dental Implant Surgery. Cullum D, Deporter D, eds. Hoboken, NJ: Wiley Publications; 1, 2016:169-189.
2. van Steenberghe D, Glauser R, Blombäck U, et al. A computed tomographic scan-derived customized surgical template and fixed prosthesis for flapless surgery and immediate loading of implants in fully edentulous maxillae: a prospective multicenter study. Clin Implant Dent Relat Res. 2005;7(suppl 1):S111-S120.
3. Sarment DP, Sukovic P, Clinthorne N. Accuracy of implant placement with a stereolithographic surgical guide. Int J Oral Maxillofac Implants. 2003;18(4):571-577.
4. Ozan O, Turkyilmaz I, Ersoy AE, et al. Clinical accuracy of 3 different types of computed tomography-derived stereolithographic surgical guides in implant placement. J Oral Maxillofac Surg. 2009;67(2):394-401.
5. Beckmann EC. CT scanning the early days. Br J Radiol. 2006;79(937):5-8.
6. Hatcher DC. Operational principles for cone-beam computed tomography. J Am Dent Assoc. 2010;141(suppl 3):3S-6S.
7. Carter JB, Stone JD, Clark RS, Mercer JE. Applications of cone-beam computed tomography in oral and maxillofacial surgery: an overview of published indications and clinical usage in United States academic centers and oral and maxillofacial surgery practices. J Oral Maxillofac Surg. 2016;74(4):668-679.
8. Abboud M, Guirado JL, Orentlicher G, Wahl G. Comparison of the accuracy of cone beam computed tomography and medical computed tomography: implications for clinical diagnostics with guided surgery. Int J Oral Maxillofac Implants. 2013;28(2):536-542.
9. Liang X, Lambrichts I, Sun Y, et al. A comparative evaluation of cone beam computed tomography (CBCT) and multi-slice CT (MSCT). Part II: on 3D model accuracy. Eur J Radiol. 2010;75(2):270-274.
10. Migliorati M, Amorfini L, Signori A, et al. Internal bone temperature change during guided surgery preparations for dental implants: an in vitro study. Int J Oral Maxillofac Implants. 2013;28(6):1464-1469.
11. Orentlicher G, Jensen O, Horowitz A, et al. Combining All-on-4 treatment with CT-guided technology: technique and report of three cases. Compend Contin Educ Dent. 2013;34(7):534-542.
12. Orentlicher G, Horowitz A, Goldsmith D, et al. Cumulative survival rate of implants placed “fully guided” using CT-guided surgery: a 7-year retrospective study. Compend Contin Educ Dent. 2014;35(8):590-598,600.